Abstract
SUMMARY: The cases presented are rare examples of congenital nystagmus associated with isolated absence of the optic chiasm. MR imaging in both patients demonstrated unremarkable anterior optic pathways and optic tracts. No additional midline central nervous system abnormalities, migrational anomalies, space-occupying lesions, or destructive processes were noted. These cases demonstrate that the achiasmatic syndrome should be included in the differential diagnosis of congenital nystagmus and may be overlooked without careful MR imaging evaluation.
Congenital nystagmus is a condition that is associated with rhythmic involuntary eye movements. It presents in the neonatal period and persists throughout life. It can be of sensory or motor origin and is often transmitted as part of a genetic disorder. Although sometimes idiopathic, congenital nystagmus may herald underlying causes including ocular pathway pathology, pituitary gland dysfunction, and even sudden death.1,2 Neuroimaging is commonly performed during the work-up of congenital nystagmus, evaluating for space-occupying lesions, optic nerve pathology, or other midline central nervous system anomalies. We present 2 nonrelated nonalbino patients with congenital nystagmus who were diagnosed with isolated absence of the optic chiasm, a rare condition in which the nasal-retinal fibers do not decussate to the contralateral hemisphere.
Case Reports
Patient 1 was a 2.5-year old African American boy who was born at term. At birth, he was diagnosed with coarctation of the aorta, supravalvular pulmonic stenosis, and patent foramen ovale. At 2 months of age, the patient was noted to have poor visual responsiveness. Ophthalmologic examination at that time demonstrated horizontal conjugate nystagmus. Pupillary reflex was normal. At approximately 6 months of age, the patient developed strabismus. Findings of an eye examination at that time demonstrated normal pupillary response with mildly hypoplastic optic nerves. He was noted to have constant horizontal conjugate nystagmus with disconjugate vertical nystagmus. He was slightly myopic.
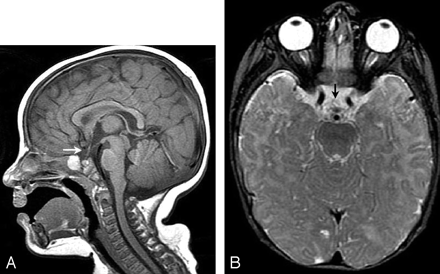
A laboratory work-up was negative for any metabolic disorder. The patient was evaluated by the genetics department and was determined to have no syndromic features. Chromosomal analysis was not performed. Family history was noncontributory. MR imaging demonstrated isolated absence of the optic chiasm (Fig 1A, -B).
A, Midline sagittal T1-weighted image demonstrates absence of the optic chiasm (arrow). The globes, optic nerves, and optic tracts are intact, but the optic chiasm is not present.
B, Axial T2-weighted image at the level of the suprasellar cistern confirms absence of the optic chiasm (arrow).
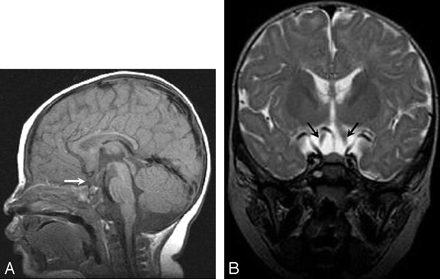
Patient 2 was a 6-month-old white girl who was born at term with multiple congenital abnormalities including unilateral cleft lip and palate and a 2-vessel umbilical cord. Findings of a physical examination revealed dysmorphic facial features and a right preauricular accessory auricle. Ophthalmologic examination at 3.5 months of age demonstrated large-amplitude horizontal nystagmus. The right eye was mildly hyperopic, whereas the left eye was mildly myopic. Findings of a fundal examination were normal. Family history was noncontributory. Results of chromosomal analysis were not available. MR imaging demonstrated isolated absence of the optic chiasm (Fig 2A, -B).
A, Midline sagittal T1-weighted image demonstrates the absent optic chiasm (arrow). The remaining midline structures are unremarkable. B, Coronal T2-weighted image at the expected level of the optic chiasm demonstrates the optic nerves (arrows) lateral to the pituitary infundibulum. The optic nerves enter directly into the optic tracts without crossing at the chiasm.
Discussion
Nystagmus can be defined as involuntary rapid eye oscillations that may be congenital or acquired. Congenital nystagmus is classically divided into 2 categories: sensory and motor. Sensory nystagmus is associated with visual impairment and may be associated with diseases of the afferent visual pathway (globes, optic nerves, optic chiasm, or optic tracts).1–3 Sensory nystagmus typically affects children who lose vision before 6 months of age. Nystagmus will not develop in children who lose vision after this time.2
Motor nystagmus is not associated with visual impairment and is related to abnormalities of the central oculomotor control system.1,2 It is often transmitted as an X-linked autosomal dominant or autosomal recessive disorder.1
Absence or hypoplasia of the optic chiasm has been described in patients with congenital anophthalmos.4,5 Patients with albinism have been reported to have small optic chiasm widths, with wider angles between the optic nerves and optic tracts. This abnormality is attributed to congenital misrouting of the optic fibers.6 Hypoplasia of the optic chiasm can be seen in conjunction with other midline abnormalities such as in septo-optic dysplasia. Isolated absence of the optic chiasm is an unusual condition, with only a few cases reported before this study. The achiasmatic syndrome, also called the nondecussating retinal-fugal fiber syndrome, is a rare inborn isolated achiasmatic condition in which patients present clinically with nystagmus.3,7–11
Decussation of the nasal retinal fibers ensures that each cerebral hemisphere receives binocular information from the contralateral visual field. Functional MR imaging evaluation of 1 patient with absence of the optic chiasm demonstrated that each occipital cortex received a complete but monocular visual field from the ipsilateral retina. Despite this fact, the patient achieved “behaviorally normal vision in most regards.”9 This is in comparison with patients with acquired chiasmatic lesions who classically present with bitemporal hemianopsia.
The pathophysiologic basis for decussation of retinal axons is an area of active research. Pathfinding of retinal axons at the optic chiasm is incompletely understood at this time. A common genetic cause for isolated absence of the optic chiasm is yet to be discovered. Mutation of a midline homeobox gene is a potential consideration.
In this article, we have documented the MR imaging findings in 2 patients with achiasmatic syndrome. Each patient presented with congenital nystagmus and was diagnosed with isolated absence of the optic chiasm on the basis of neuroimaging. The achiasmatic syndrome should be included in the differential diagnosis of congenital nystagmus and could be easily overlooked without careful MR imaging evaluation.
Footnotes
The views expressed in this article are those of the authors and do not reflect the official policy or position of the Department of the Army, Department of Defense, or the US Government.
References
- Received September 18, 2005.
- Accepted after revision January 11, 2006.
- Copyright © American Society of Neuroradiology