Abstract
BACKGROUND AND PURPOSE: Several studies suggest that VLBW is associated with a reduced CC size later in life. We aimed to clarify this in a prospective, controlled study of 19-year-olds, hypothesizing that those with LBWs had smaller subregions of CC than the age-matched controls, even after correcting for brain volume.
MATERIALS AND METHODS: One hundred thirteen survivors of LBW (BW <2000 grams) without major handicaps and 100 controls underwent a 3T MR examination of the brain. The cross-sectional area of the CC (total callosal area, and the callosal subregions of the genu, truncus, and posterior third) was measured. Callosal areas were adjusted for head size.
RESULTS: The posterior third subregion of the CC was significantly smaller in individuals born with a LBW compared with controls, even after adjusting for size of the forebrain. Individuals who were born with a LBW had a smaller CC (mean area, 553.4 mm2) than the controls (mean area, 584.1 mm2). Differences in total area, however, did not remain statistically significant after adjusting for FBV.
CONCLUSIONS: The uncorrected callosal size in 19-years-olds born with LBW was smaller than that of normal controls. However, after adjusting for FBV, the group difference was restricted to the posterior third. The clinical impact of a smaller posterior part needs further investigation.
Abbreviations
- aFBV
- area measure of forebrain volume
- ANOVA
- analysis of variance
- BW
- birth weight
- CC
- corpus callosum
- DTI
- diffusion tensor imaging
- FBV
- forebrain volume
- GA
- gestational age
- IQ
- intelligence quotient
- LBW
- low birth weight
- MD
- mean diffusivity
- MNI
- Montreal Neurologic Institute
- relCC
- relative corpus callosum
- resCC
- residualized corpus callosum
- TBV
- total brain volume
- VLBW
- very low birth weight
LBW (<2500 g) is a major public health problem found in approximately 20% of all births worldwide, particularly in low-income countries. The prevalence varies substantially, from 3% to 4% in Italy and Scandinavia to 30% in India.1 Numerous long-term follow-up studies indicate that individuals born with a BW <2000 g have an increased risk of learning difficulties, impaired attention functions, and behavioral problems.2,3 The reasons for these associated problems are unclear. However, most children born with a BW <2000 g are also born at a GA of <37 weeks, and several studies suggest that those born prematurely have smaller CCs than those born at term.4–8 A correlation between CC thickness and intelligence (IQ) has been demonstrated in healthy adults,9 whereas studies of very preterm–born individuals have shown that reduced CC size correlates with total IQ,10 verbal IQ,8 and neuropsychologic impairment.11 These studies, however, differ in design, both with regard to inclusion criteria (based on BW versus GA) and image analysis techniques (qualitative versus quantitative studies), thereby making robust conclusions difficult.
Formation of white matter commissures, including the CC, starts at 8–10 gestational weeks,12,13 and maturation continues throughout childhood until adulthood (mid-20s).14 Premature birth and associated perinatal injury may slow down15 this process to some extent or even impair the growth of the CC.16 It is still not clear whether LBW by itself may cause similar injury.
We have followed an unselected cohort of LBW individuals and age-matched controls over a period of 19 years and have previously found that the LBW group had a smaller CC at 19 years than the controls as judged subjectively by using MR imaging.17 Because subjective assessment of CC size is commonly used in clinical practice, our results, supported by those of others predominantly addressing survivors of VLBW (<1500 g),4,8,10 have led to a large proportion of these children being labeled as having a small CC. We therefore set out to examine whether this was true when based on objective measurements and whether adjustments for head size by using different techniques would influence the results. We hypothesized that the LBW group had a smaller CC as well as smaller subregions of CC, irrespective of the method used for adjustment for FBV, than the controls.
Materials and Methods
Subjects
The initial birth cohort consisted of 217 consecutive neonates born with a BW <2000 g (LBW) within the county of Hordaland, Norway, between April 1, 1986, and August 8, 1988.18–20 In total, 44 were excluded (22 died and 22 had major handicaps or cerebral palsy) and of the 173 eligible survivors 134 participated in the clinical follow-up.18,21 The controls were randomly selected from an age-matched population of neonates with a GA of >37 weeks, a BW >3000 g, and without any need for assisted support in the neonatal period. The subjects have been followed closely during childhood and puberty, with 3 major clinical and psychological assessments at age 5, 15, and 19 years.18–20 Because no brain imaging had been performed during the 2 first follow-ups, we found it reasonable to add a head MR imaging at age 19 years, when the brain maturation is nearly completed.
The study participants were invited to undergo an MR imaging and for the present radiologic follow-up at age 19, we included 113 LBW survivors (65% of the initial cohort) and 100 controls. The mean BW for those 113 LBW survivors attending the MR imaging study did not differ from the 60 nonattendees (BW = 1547 g [SD = 344; range, 640–1990] versus BW = 1628 g [SD = 378; range, 570–1990], P = .183). Mean GA in the LBW group was 32.1 weeks (SD = 3.1; range, 24–40 weeks). One hundred and three (91%) of the 113 in the LBW group were born prematurely, ie, before 37 weeks' gestation. The mean (SD) BW for those 103 born preterm within the LBW group was 1520 (347) versus 1808 (188) g for the 10 subjects born at term (P = .001). One hundred of the 170 controls (59%) in the initial study also were included. The mean (SD) height at time of examination at 19 years of age was significantly lower for the LBW group compared with the control group (168.0 [10.6] versus 173.3 [8.3] cm; P < .001).
MR Imaging
The MR imaging examinations were performed at the Department of Radiology, Haukeland University Hospital, Bergen, Norway, during the period January 2006 to May 2007. We used a Signa Excite HD 3T machine (GE Healthcare, Milwaukee, Wisconsin) and an 8-channel head coil to obtain sagittal 3D T1-weighted images (sagittal spoiled gradient-recalled 3D; TR = 5.9 ms, TE = 1.3 ms, section thickness = 1.0 mm, scan time = 8:56 min, FOV = 25 cm, matrix = 256 × 256, NEX = 1.00, and flip angle = 11°).
Estimation of FBV
FBV defined as cerebral volume excluding brain stem and cerebellum was estimated by using a semiautomatic procedure implemented in Matlab (MathWorks, Natick, Massachusetts). First, to perform the volumetric analysis of the forebrain, a template mask of the forebrain (in MNI, standard space), was fitted to each individual brain by applying an inversed normalization procedure. For this purpose, we first estimated the transformation parameters for the normalization of each individual T1-weighted image to the MNI template provided with SPM5 (Wellcome Department of Imaging Neuroscience, London, United Kingdom). Then, we used the inversed transformation parameters to transform the forebrain mask into the native space of each individual (non-normalized) brain image. The final calculation of the FBV was based on gray matter, white matter, and CSF probability maps (obtained in native space), which were obtained by the segmentation procedure as implemented in SPM5. FBV was determined by counting the voxels showing a gray matter or white matter probability of >0.6, located within the fitted forebrain template. In addition, all voxels showing CSF probability >0.3 were excluded. For each individual brain, a map was created showing voxels that had been excluded, to assist in checking whether the masking and segmentation procedures had been successful. The number of forebrain voxels obtained with this procedure was then multiplied by the voxel size to obtain FBV volume estimates in cubic centimeters.
Measurement of CC
The cross-sectional area of the CC was measured on a midsagittal T1-weighted image by using the following procedure. First, the midsagittal image was identified and optimized, ie, rotated and reassessed under visual tracking of the longitudinal fissure with arachnoid, but no white matter showing, by using SPM5. Second, the midsagittal image was oriented horizontally, with respect to an imaginary line connecting the ventral-most points of the callosal genu and splenium. In a third step, the outline of the CC was manually traced by using MRIcro software (www.sph.sc.edu/comd/rorden/mricro), and a binary mask of the obtained region of interest was created and exported.
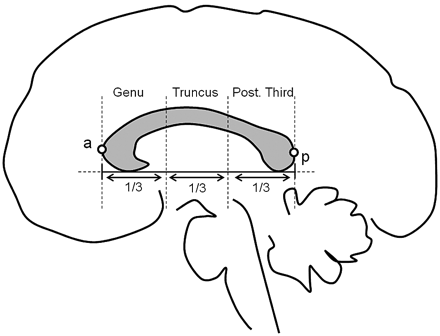
Based on the mask and by using routines written in Matlab, the cross-sectional area of the CC and its 3 subregions (genu, truncus, and splenium) was determined. The subregions were defined following the operational definition as proposed by Witelson22: the total callosal area was subdivided into 3 thirds relative to the genu-splenial line (connecting the anterior- and posterior-most points of the CC), producing the 3 subregions genu (anterior third), truncus (middle third), and the posterior third (Fig 1). Area measures for the 3 subregions of the CC were then stored for further analysis and multiplied by the size of the voxel on a sagittal view to obtain the midsagittal area measure in square centimeters.23
Schematic view of CC subregions; genu (anterior third), truncus (middle third), and posterior third.
Measurements of the CC were adjusted for brain size by using the abovementioned FBV estimates. Callosal and forebrain size estimates, however, pose a different dimensionality (area versus volume) and using FBV to adjust the CC area would overcorrect for brain size (for discussion, see reference 24). Thus, we transformed the FBV into an aFBV by using the equation aFBV = FBV0.667. Callosal measures were then adjusted for forebrain size by using 2 different approaches: 1) calculating relCC by dividing the measures of each callosal subregion with the aFBV value for each subject; or 2) calculating resCC by using a linear regression to estimate the callosal subregion size that would be predicted from each individual forebrain size and then subtracting the predicted from the measured size to obtain the resCC value. Because both adjusted CC measures allow for different interpretations24 and both approaches can be found in the literature, we used both relCC and resCC measures in further statistical analysis.
Descriptive statistics for 113 individuals with LBWa and 100 normal birth weight controlsb followed up at age 19 years
Statistical Analysis
The interobserver variation for measurements of the area of the CC was examined in 10 subjects, 5 LBWs and 5 controls, by using mean differences and 95% limits of agreement.25 The interobserver agreement was acceptable, with a mean difference of 7.5 mm2 (95% limits of agreement; −52.3, 67.4).
For descriptive statistics the mean and SD were used. Pearson correlation coefficient (r) was used to quantify the relationship between brain size as expressed by brain volume in cubic millimeters and brain volume as expressed by area in square millimeters, and between brain volume and body height. The initial group comparisons of brain volume and callosal size were analyzed by using a t test for independent samples.
Three separate 3-way ANOVAs were performed to explore the impact of group and sex on callosal size, by using uncorrected CC size, relCC, and resCC, respectively, as dependent measures. All ANOVAs included 2 between subject factors, namely, group (LBW versus control) and sex as well as a repeated measure factor callosal subregion (with the 3 levels genu, truncus, and posterior third). Significant interaction effects were followed up with paired t tests or t tests for independent samples. The effect size for all main and interaction effects was given as a proportion of explained variance (η2). Effect sizes for comparisons between pairs of subregions were given as Cohen d. A significance level of 5% was used for all statistical tests, and no adjustment for multiple comparisons was performed to retain the statistical power of the performed tests.26
Similar ANOVAs were performed on a subset of subjects fulfilling the criteria for prematurity, ie, those 103 individuals with a gestational age <37 weeks, to test for differences in total as well as subregional CC area between those born prematurely with a BW <2000 g and controls. Statistical analyses were performed by using STATISTICA 8.0 (Statsoft, Tulsa, Oklahoma).
Results
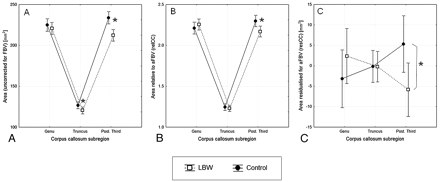
By analyzing the uncorrected CC area, a statistically significant but small main effect of group (F1,208 = 6.57, P = .01, η2 = 0.01) was detected, indicating an overall smaller CC area in the LBW group (mean, 553.4 mm2; SD, 98.3 mm2) compared with controls (mean, 584.1 mm2; SD, 82.7 mm2), equivalent to a standardized mean difference of d = 0.34. Furthermore, the interaction of group and callosal region was statistically significant but small (F2,416 = 12.80, P < .0001, η2 < 0.01; Fig 2 A). Post hoc t tests revealed that the interaction was due to a significantly smaller truncus (t210 = 2.16, P = .03, d = 0.29) and posterior third (t210 = 4.02, P < .001, d = 0.56) in the LBW group, whereas the group difference—although pointing in the same direction—was not significant for the genu area (t210 = 0.88, P = .38, d = 0.12). A significant main effect of sex indicated a larger overall callosal area in males compared with females (F1,208 = 5.15, P = .024, η2 = 0.01). Finally, a statistically significant main effect of callosal region (F2,416 = 1899.18, P < .0001, η2 = 0.69) was detected, indicating a smaller truncus size compared with the 2 other regions. No other effects were significant for the analysis of the uncorrected CC measures.
Size (area) of the CC subregions as measured on a sagittal, midline T1-weighted MR image, in the LBW group (n = 113; black line) versus the control group (n = 100; dotted line). The error bars show mean values, with 95% confidence intervals of the data distribution for 3 different settings. A, No correction made for FBV. B, Corrections made for FBV by using the relCC size measures. C, Corrections made for FBV by using the resCC size measures. The asterisk (*) denotes a statistically significant post hoc t test.
For relCC, there was a statistically significant but small interaction effect between group and callosal region (F2,416 = 11.2, P < .0001, η2 = 0.01). As revealed in post hoc t tests, this interaction was driven by a significantly (t210 = 2.51, P = .012, d = 0.35) and disproportionately smaller posterior subregion in the LBW compared with the control group, whereas the genu (d = −0.11) or truncus (d = 0.08) did not differ significantly in size between the groups (Fig 2 B). A significant main effect of callosal region (F2,416 = 1951.00, P < .0001, η2 = 0.74) indicated a smaller truncus size compared with the 2 other regions. No other main or interaction effects were significant for the relCC analysis.
For resCC, we detected a similar, statistically significant but small interaction effect between group and callosal region (F2,416 = 10.73, P < .0001, η2 = 0.02), which was driven by a smaller posterior third region in the LBW group compared with the control group (t210 = 2.16, P = .03, d = 0.30), in addition to no significant differences in the other 2 regions (see Fig 2C: genu, d = −0.15; truncus, d = 0.01). No other main or interaction effects were statistically significant for the resCC analysis. Similar ANOVAs including only those fulfilling the criteria for prematurity (n = 103) did not change the results (data not shown).
The mean (SD) total forebrain volume was 952 (101) cm3 for the LBW group, compared with 1024 (129) cm3 for the control group (P < .0001). Brain volume in cubic millimeters and brain volume as expressed by area in square millimeters were strongly correlated (r = 0.99, P < .0001), whereas the correlation between brain volume and body height was moderate (r = 0.37, P < .0001). The size of the CC was significantly related to FBV (r = 0.32, P < .0001) and this relation was significant for both the control group (r = 0.35, P < .0001) and LBW group (r = 0.254, P = .007).
Discussion
We have shown that young adults born with a BW <2000 g have an overall smaller (unadjusted) CC compared with their age-matched peers born with normal BW but that this overall difference disappears when adjusting for forebrain size. However, a difference remained for the posterior third of the CC, irrespective of method used to adjust for overall brain size. Our results should be taken into consideration when reporting brain MR imaging results, to avoid overdiagnosing a reduced CC size.
Strengths of our study include the population-based nature of the dataset, the high participation rate, and the different adjustments performed to test the robustness and generality of the outcomes. However, the study included all subjects with a BW <2000 g regardless of GA, inferring that our results may not necessarily apply to a prematurely born population, because 10 subjects out of the LBW group were born with GA of ≥37 weeks and those born prematurely with a BW of >2000 g were not included. In contrast, subanalysis of those fulfilling the criteria for prematurity, ie, the 103 with a GA <37 weeks did not alter the results.
Moreover, the selection of a control group that remained stable for the whole study period of almost 20 years is a strong feature of this dataset. We have thus avoided a supernormal group for comparison, and this more natural control group may support the robustness of our findings in the young adults born with LBW.
We also excluded those with major handicaps, such as cerebral palsy, unlike prior studies.8,27 Both of these studies showed an overall reduced size of the CC in those born prematurely with VLBW (BW <1500 g) at age 15 and 8 years, respectively. Others have performed an MR imaging study during childhood or early adolescence and included those with GA <33 weeks.4,11 This heterogeneity in study design limits the number of quantitative studies with which to compare the present results.8,11,27
Several qualitative studies6,7,28 have used the evaluation of the size of the CC by an expert (radiologist) and have described a thinning of the CC in VLBW adolescents, however, without addressing the different subregions, or taking the overall head size into consideration. These results agree with a previous report from the current cohort17 and also with the preadjusted results from the present study, reflecting difficulties both related to subjective assessment alone and to the justification of adjusting for total forebrain size.
Studies like these are particularly susceptible to biases related to measurements and analysis used, to whether adjustments for FBV have been made, and to the adjustment technique used for CC size. First, although measuring the area of the CC by manual tracing may represent a possible bias, the reproducibility, despite few cases, obtained by 2 independent readers in our study was acceptable. Second, analyzing the size of the CC represents a potential difficulty, because relating callosal area given in square millimeters to brain volume given in cubic millimeters may carry the risk of overadjusting for brain size.24,29 To address this problem, we expressed the volume as an area (volume0.667), as suggested previously.24,30
Because the 2 different volume expressions differ in their mean values, they cannot be used interchangeably when creating relCC areas. Third, most studies have adjusted CC size with some measures for TBV,27,31 though others32 have not covaried for CC size. Finally, the use of slightly different adjustment techniques represents another source of diverging results.29
The finding of a smaller posterior third among the LBW group compared with the control group is noteworthy, because this finding was consistent across the differing techniques used to adjust for overall forebrain size. Others have reported similar findings in younger cohorts of VLBW survivors and by using smaller sample sizes. A controlled study of 25 prematurely born 8-year-olds27 reported a reduced CC size after adjusting for TBV, with an inverse association between the size of the posterior CC and gray matter changes in the cortical projection area. Another study of 72 individuals born very preterm (at age 15 years)8 demonstrated that an overall reduction in callosal size was driven by a reduction of the posterior portion. Thus, there seems to be some support for the finding of a smaller posterior CC in those born with LBW and VLBW. Whether this smaller posterior CC represents a permanent change or merely delayed growth is still unclear, because the CC is believed to reach maturity in young adulthood,33 ie, slightly older than those included in our cohort. A previous study33 reported evidence for a growth spurt of CC between 14–15 years and 23 years in a group of 72 prematurely born subjects.
The smaller posterior segment found in our study may reflect thinning of the interhemispheric fiber bundles, a reduced number of fibers, a reduction of the thickness of the myelin sheet, or a combination of these factors.34 Based on our findings and on extant literature, we postulate that the posterior part of CC is disproportionately reduced in size in those born with a BW <2000 g, consistent with findings in VLBW survivors and those born prematurely (before week 37). This finding suggests that the posterior portion may have an increased susceptibility for injury in LBW children. The splenium forms after the genu and the callosal body, and even though the mature shape of the CC is reached by 17 weeks of gestation, premature birth may interfere with its later stages of development.33
In addition, the reduced size of the posterior CC may reflect important changes within the microstructure. In a quantitative study of VLBW adolescents, including DTI,35 a lower fractional anisotropy was detected in posterior aspects of CC. These findings have, however, been challenged in a recent DTI study36 that demonstrated a higher MD in the genu of the CC and a significant association between the MD and IQ in prematurely-born females at age 18 years. No changes were seen in the splenium in this study nor in any parts of male CCs.
Finally, the reduced size of the posterior CC and the underlying changes in the callosal fiber architecture would consequently be associated with an increased interhemispheric transfer time or a reduced functional connectivity between the hemispheres in the LBW group. However, any such claim awaits testing in future studies. The present findings also have clinical implications. In 8-year-old children born prematurely, an association has been reported between the size reduction of posterior CC and gray matter alterations in the projection area.27 These correlation analyses, however, cannot determine whether injury to the CC produces smaller cortical gray matter volumes or whether injury to gray matter disrupts interhemispheric axons within the CC. In addition, a quantitative study8 of 14–15 year olds born very preterm (< 33 weeks) has documented associations between midposterior CC surface area and verbal skills. Whether this is true for the LBW survivor remains unclear. Neuropsychologic performance data at 5 years of age in our cohort documented that children born with LBW suffered impaired performance on visuospatial and visuomotor tasks.
Prospective studies on the CC at term-equivalent age and later developmental outcome would posit strong documentation for the clinical significance of changes in the CC.37
Conclusions
We have shown that the uncorrected callosal size in LBW 19-year-olds is smaller than that of normal BW controls. However, after adjusting for TBV, the group difference was found to be restricted to the posterior third. Possible clinical impact of a smaller posterior portion requires further investigation.
Acknowledgments
We thank the Department of Radiology, Haukeland University Hospital, lead by Dr. Aslak Aslaksen, for supporting the study and for the use of the 3T MR imaging scanner. We are also very grateful for the efforts of MR radiographers Jan Ankar Monsen and Jarle Seter in this study.
References
- Received August 17, 2010.
- Accepted after revision September 29, 2010.
- Copyright © American Society of Neuroradiology