Abstract
BACKGROUND AND PURPOSE: The carotid bulb is innervated by the sinus nerve of Hering, a branch of the glossopharyngeal nerve, derived from the third pharyngeal arch. The aim of this study was to determine the frequency, predictors, and outcome of the carotid BR after carotid stent placement according to the location of the plaque lesion.
MATERIALS AND METHODS: Atherosclerotic carotid plaques of apical versus body lesions were prospectively analyzed in 95 consecutive patients who underwent carotid stent placement. Patients with hypertension after stent placement were excluded, and transient (<3 hours) and prolonged (3–24 hours) BR, together with AEs such as strokes and death, were assessed in the 2 lesion locations (apical versus body). Other factors known to affect the carotid baroreceptor were also investigated, and the results were analyzed by χ2 or Mann-Whitney U tests.
RESULTS: Transient BR occurred in 30% of apical lesions in contrast to 70% of body lesions (P = .001). Transient BR showed a significant relationship to lesion location (P = .001), occurring most frequently in body lesions, and to the distance of maximum stenosis from the ICA ostium (P = .001). Hyperperfusion and AE rates (P = .076) in 1 month occurred more frequently in apical lesions.
CONCLUSIONS: The frequency of transient BR after carotid stent placement was lower in the apical region of the carotid bulb. Different cardiovascular disturbances after carotid stent placement can be attributed to anatomically different areas of the carotid bulb.
ABBREVIATIONS:
- AE
- adverse event
- BP
- blood pressure
- BR
- baroreceptor reaction
- CCA
- common carotid artery
- CEA
- carotid endarterectomy
- mRS
- modified Rankin Scale
- NIHSS
- National Institutes of Health Stroke Scale
- NTS
- nucleus tractus solitarii
- SBP
- systolic blood pressure
The carotid bulb, an enlarged vascular structure just distal to the bifurcation of the CCA, is the major site of involvement in atherosclerotic stenosis.1 The carotid bulb is confined to the CCA, which is a remnant of the third aortic arch, and has a different embryologic origin from the cervical ICA, which is derived from the dorsal aorta between the second and third aortic arches.2,3 This difference in embryologic origin could contribute to the size discrepancy between the carotid bulb and the cervical segment of the ICA and also to the distribution of glossopharyngeal nerve endings. The glossopharyngeal nerve is a remnant of the third pharyngeal arch and the third aortic arch and contains afferent fibers that mediate the vasovagal reflex, thus differences in the distribution of glossopharyngeal nerve endings could lead to different hemodynamic patterns after carotid stent placement.
There have been several speculations regarding the embryologic origin of the common and internal carotid arteries4 (ie, the CCA is derived from the third aortic arch5 and both the whole common and the proximal ICAs are derived from the third aortic arch6). The root portion of the ICA is formed by the whole third aortic arch with the gradual disappearance of the carotid duct derived from the dorsal aorta between the third and fourth aortic arches, whereas the CCA develops from the aortic sac.7 A recent study of gene-targeted mice have reported that Hoxa 3 is involved in the patterning and remodeling of the third pharyngeal arch arteries; they have also revealed that the carotid bulb belongs to the third aortic arch, whereas the cervical segment of the ICA belongs to the dorsal aorta between the second and third aortic arch.2
Hemodynamic depression after CEA and stent placement consists of hypotension related to baroreceptor stimulation and bradycardia or asystole.8⇓⇓⇓⇓–13 Although regarded as a BR, hypertension after CEA or stent placement may have different effects on the immediate outcome after the stent placement procedure by resulting in hyperperfusion.11,13⇓–15 Our previous study revealed no difference in hemodynamic depression between apical and body lesion locations, probably because patients showing postprocedural hypertension were included.3 Therefore, hypertension was excluded from the carotid BR, which was separated into transient (<3 hours) and prolonged (3–24 hours) BR, and these were assessed depending on their association with factors known to affect the carotid sinus BR.
Materials and Methods
A prospective analysis was performed of 95 consecutive patients (male/female ratio = 82:13; mean age, 69 years; range, 38–89 years) who underwent carotid stent placement between January 2007 and June 2009. Included in the study were patients diagnosed with symptomatic carotid stenosis (≥50%) or asymptomatic stenosis (≥80%), on the basis of angiography by using North American Symptomatic Carotid Endarterectomy Trial criteria, whereby the diameter at the most stenotic point is compared with the diameter of the normal part of artery beyond the constriction.16 The patients included in the study, according to these criteria, met ≥1 of the high-risk criteria, as defined previously.3,17 Patients with nonatherosclerotic arterial diseases such as Takayasu arteritis or who had undergone dissection and stent placement following intra-arterial thrombolysis and/or angioplasty as a part of their acute stroke management, were excluded from the analysis. Our institutional review board approved this study, and written informed consent was obtained from the patients and their families.
According to previously described anatomic definitions, the carotid bulb with atheromatous plaques can be categorized as having an apical or body lesion (Fig 1). 3 Body lesions are those in which the transitional zones of the CCA and the bulb are affected by a plaque located mainly in the body segment, thus causing the most severe stenosis in the body. Apical lesions are those in which the transitional zone of the bulb and the proximal cervical ICA segment (ie, the apical segment) are affected by plaques, with or without minimal involvement of the body segment. We also differentiated the primarily involved area of plaque and the most severe stenosis. Because plaque enlargement is regarded as an extended form of plaque, we defined an extended apical lesion as one in which apical plaque involves the body of the carotid bulb, and we defined the extended body location of plaque as one in which the body plaque involved the apex.3 The main component of the plaque involvement and the level of the most severe stenosis were considered as part of the extent of the plaque to differentiate the extended lesions.
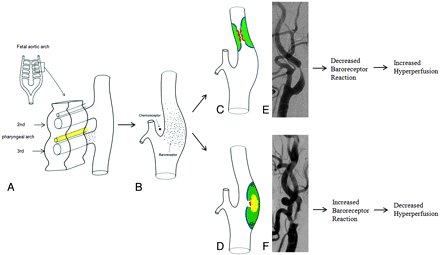
Concept map showing the embryologic origins of the carotid bulb (apical versus body area), respectively. The glossopharyngeal nerve (yellow in A), derived from the third pharyngeal arch, innervates the carotid bulb (a remnant of the third aortic arch) as shown by the dotted areas in A and B. Note the absent or sparse nerve endings in the bulb apex, which contribute to the reduced BR in this region. Note the chemoreceptor in the bifurcation apex and the 2 locations of carotid bulb lesions: apical (C) and body (D). The transient BR was absent in E and present in F after stent placement.  indicates the glossopharyngeal nerve endings for the carotid BR.
indicates the glossopharyngeal nerve endings for the carotid BR.
Angiographs were analyzed for lesion length, distance of maximum stenosis from the ICA ostium, degree of stenosis and procedural results for balloon diameter, balloon pressure, and stent length. Calcification was identified by the presence of attenuated calcification on angiographs and/or by the presence of attenuated calcified shadows in Doppler sonography studies of the carotid bulb.18 The distribution of the calcification was assessed, and the vessels were divided qualitatively into 2 groups: 1) the mild calcification group, a lesion with no or a few small spotty calcium deposits; 2) the severe calcification group, a lesion with intermediate and extensive calcification.19 Patients in the severe calcification group were classified as having a calcified plaque on the basis of the judgment of 2 experienced, independent observers.
Hyperperfusion (n = 8) was diagnosed in 2 categories occurring within 1 month of the procedure.17 The first category is the symptomatologic occurrence of a throbbing headache ipsilateral to the treated artery with or without nausea, vomiting, or ipsilateral focal seizures, or as the presence of a focal neurologic deficit without radiographic evidence of infarction.20 Although such throbbing headaches have often been described in the literature, we observed severe irritability and confusion more frequently than headache along with increased blood pressure; however, these symptoms subsided after the strict control of a patient's high blood pressure by intravenous antihypertensive medication. Therefore, we included those patients (n = 5) in the hyperperfusion category. We performed MR imaging with a perfusion study in 2 patients and identified increased (n = 1) and normalized (n = 1) perfusion in the vascular territory of the brain compared with the decreased perfusion noted before the procedure.
The second category is hemorrhage (n = 3) in the ipsilateral vascular territory following the procedure, which can be explained by reperfusion or hyperperfusion unless there was another cause of the hemorrhage. One patient without any previous infarction developed a massive hemorrhage at home 4 days following the procedure. Another patient developed massive hemorrhage, which occurred in the previous infarction in the basal ganglia. The patient without any previous infarction developed multifocal hemorrhage in the ipsilateral brain territory 1 day following the procedure. Those hemorrhages led to 1 death and 2 major strokes.
Unless there was a contraindication such as known severe flow-limiting stenoses in other vascular beds, BP was maintained at <130/90 mm Hg for postprocedural BP parameters. The carotid stent placement procedure used in this study was the same as that previously described.17,21⇓–23 Wallstents (Boston Scientific, Natick, Massachusetts) were used in 45 patients; Precise stents (Cordis, Miami Lakes, Florida), in 43; and Protégé stents (ev3, Irvine, California), in 7. Protection devices were used in 92 patients (97%).
AEs were minor stroke, major stroke, or death. “Minor stroke” was defined as a new nondisabling neurologic deficit or as an increase of 3 in the NIHSS score that completely resolved within 30 days.24 A “major stroke” was defined as a new neurologic deficit with an increase of 4 in the NIHSS that persisted longer than 30 days. The final outcome at 6 months was determined by the mRS (good outcome, ≤2; poor outcome, ≥3).
Carotid BR
The BR was defined during and after stent placement and included periprocedural hypotension (systolic blood pressure of <90 mm Hg), bradycardia (heart rate of <50 beats/s), or heart rate fluctuation (>20 beats/s).9,10 Patients with periprocedural hypertension (>160 mm Hg), which, in other reports, was included for hemodynamic depression or instability,3,11 were evaluated separately. Postprocedural transient hypertension was noticed in 21 patients, who had 13 apical lesions and 8 body lesions. Prolonged hypertension was noticed in 14 patients who had 8 apical and 6 body lesions.
We divided the BR during 24 hours after stent placement into transient (<3 hours) versus prolonged (3–24 hours) because transient BR is directly affected by the procedure and prolonged BR is a more sustainable change or a later response than transient BR. The management of BR included control of the fluid load and intravenous administration of atropine and/or vasoconstrictors. Throughout the procedure and for at least 24 hours after stent placement, continuous electrocardiograph and continuous intra-arterial blood pressure via the arterial line were monitored.
Statistical Analysis
Transient and prolonged BRs were regarded as dependent variables. Explanatory variables were extracted from angiographic and stent placement results, and these included lesion location, the presence or absence of diabetes mellitus and calcification, lesion length, distance of maximum stenosis from the ICA ostium, degree of stenosis, balloon diameter, balloon pressure, and stent length. Mann-Whitney U tests were performed to determine the association between the BR and continuous explanatory variables. χ2 or Fischer exact tests were used for categoric variables. All P values were calculated by using the 2-tailed test. A P < .05 was considered significant. Calculations were performed by using the Statistical Package for the Social Sciences, Version 14.0 for Windows (SPSS, Chicago, Illinois).
Results
Transient BR showed a significant relationship to the location of the lesion and was present in 30% of apical lesions and 70% of body lesions (P = .001) and a significant relationship to the distance of maximum stenosis from the ICA ostium (P = .001) (Table 1). Prolonged BR was not related to lesion location (Table 2). There were no significant differences for the other variables. The event rate in 1 month showed some relationship to lesion location (P = .076), with 8.9% of patients with apical lesions having an AE within 1 month (Table 3). The link between hyperperfusion and lesion locations was not statistically significant but was more likely to occur in apical lesions (Table 3).
Comparison of significant differences in transient BR
Comparison of significant differences in prolonged BR
Carotid bulb lesion location versus increased systolic BP, ipsilateral event, hyperperfusion, and restenosis
Among our patients with symptomatic (82%) or asymptomatic (18%) stenosis, there was ≥70% (72%) or 50%–70% stenosis (28%). Five AEs in 1 month occurred in the symptomatic patients with ≥70% stenosis. Four of the 5 AEs were related to hyperperfusion (3 hemorrhages and 1 reperfusion injury). An AE at 4 months was a minor stroke caused by a small intracerebral hemorrhage in a stable patient with 67% stenosis.
Systolic BP before stent placement, and during transient (<3 hours) and prolonged (3–24 hours) periods, was 141 ± 19 mm Hg (139 ± 18 versus 144 ± 19 mm Hg in apical versus body lesions), 132 ± 27 mm Hg (134 ± 26 versus 128 ± 27 mm Hg in apical and body lesions), and 120 ± 22 mm Hg (120 ± 21 mm Hg versus 120 ± 24 mm Hg in apical versus body lesions). Atropine (0.25–1 mg) was used in 82% of our patients (80% versus 85% with apical versus body lesions) during stent placement. The percentage of patients in whom intravenous antihypertensives were used during transient or prolonged periods included 22% of patients (25% versus 18% of apical versus body lesions) during the transient period and 52% of patients (59% versus 41% of apical versus body lesions) during the prolonged period.
Discussion
Our study revealed that after stent placement, the transient BR frequency varied according to the location of carotid bulb lesion (apical versus body). As demonstrated in other studies,2,3,25 the distance of maximum stenosis from the ICA ostium was also related to BR. Body lesions were more vulnerable to BR than apical lesions due to the anatomic location of baroreceptors in the carotid sinus (eccentric dilated carotid bulb) compared with chemoreceptors in the carotid glomus (body), which is located at the apex of the carotid bifurcation (Fig 1). Baroreceptors, triggered by the glossopharyngeal nerve, are stretch receptors located at the bifurcation of the external and internal carotid arteries in the carotid bulb. The body of the carotid bulb is a dilated segment of the ICA at its origin from the CCA, which is a remnant of the third aortic arch and the third pharyngeal arch, and is innervated by the nerve of the third arch, the glossopharyngeal nerve.2,25 In contrast, the apex of the carotid bulb is partially confined to the carotid bulb and is less affected by stimulation of the glossopharyngeal nerve. Thus, our results suggest that the embryologic origin of the lesion site affects BR frequency, which was greater in carotid bulb lesions than in apical lesions.
Our study revealed the different frequency of BR after carotid stent placement, according to the location of the atheromatous plaque. We hypothesized such a different response according to lesion location from several aspects. First, there must be variability in the innervation attenuation and distribution of the baroreceptors in the carotid bulb (apex versus body), as seen in other body parts.26 Second, because atherosclerosis is an acquired disease process, distribution of atheromatous plaque does not follow the anatomic disposition. Because growing plaque can straddle the anatomic disposition, there must be an extended plaque lesion that might respond differently from those in the typical lesion location. Third, BR can also be affected by procedure-related factors because atheromatous plaque involving the apex versus body locations might have a different baroreflex sensitivity or responsiveness of the baroreceptor.27
Among patients with hemodynamic instability or depression, which consists of hypertension, hypotension, or bradycardia after CEA or carotid stent placement, acute hypertension is attributed to the transient dysfunction of adventitial baroreceptors in patients who underwent endarterectomy, though metabolic factors such as renin and vasopressin have also been implicated.8,13,14,28⇓⇓⇓–32 Our study revealed an increase in the tendency to present with AEs and hyperperfusion in apical lesions. In some cases, reduced BR frequency in apical lesions may not be detected by measuring blood pressure (>160 mm Hg) because hyperperfusion syndrome, after relief of severe carotid stenosis, can still occur in patients with normal blood pressure but who have a decreased reservoir for cerebral circulation and loss of autoregulation. Therefore, the increased tendency to hyperperfusion and event rate in apical lesions may support the hypothesis that acute hypertension after CEA or stent placement is due to transient baroreceptor dysfunction with decreased baroreflex sensitivity or responsiveness of the baroreceptor.27
The baroreflex or BR originates from stretch-sensitive carotid baroreceptors in the arterial wall of the carotid sinus and the aortic arch and in the large vessels of the thorax and buffers abrupt changes in blood pressure.33 Afferent fibers from carotid baroreceptors of the glossopharyngeal nerve (ninth cranial nerve) project to the NTS in the dorsal medulla, where they inhibit sympathetic neurons and reduce sympathetic tone to peripheral blood vessels, leading to a reduction in systemic blood pressure. In conjunction with the aortic baroreceptors, the carotid sinus baroreceptors play a key role in short-term adjustments of blood pressure due to relatively abrupt changes in blood volume, cardiac output, or peripheral resistance. Impulses from the carotid sinus also initiate excitatory impulses from the NTS to the nucleus ambiguus and dorsal vagal nucleus.34 The subsequent increase in vagal activity results in a decrease in heart rate.
Apical lesions are regarded as high cervical lesions and are a well-known risk factor for CEA because surgical access to the bulb apex can be limited if a plaque lesion is positioned high in the carotid bulb.3,17 In contrast to body lesions with greater BR frequencies, apical lesions with reduced BR are more prone to hypertension or hemorrhage, which is related to hyperperfusion, especially in patients with a loss of autoregulation.8 Therefore, our study suggests that different hemodynamics operate in each of the carotid bulb lesion locations, and we recommend careful consideration of the possible variations in hemodynamic responses after stent placement.3,17,21,35
There are several limitations to our study. First, although we demonstrated carotid BR differences according to carotid body lesion location and a tendency of AE difference, a larger cohort may reveal a significant difference between event rate and the location of carotid bulb lesion. Second, because the atherosclerotic plaque is an acquired lesion related to numerous risk factors, it was not possible to separate the BR response to carotid stent placement, which is also affected by many procedure-related factors. The embryologically related response of the glossopharyngeal nerve to the stent placement procedure observed in this study is only possible when the patient population has 2 distinct locations of carotid bulb lesion, as occurs in the Korean population in which carotid bulb apical lesions are more common than body lesions.3 Third, our consecutive study patients revealed a predominance of male patients; male/female = 82 (86%):13 (14%) compared with male/female = 78:22 in our previous report regarding 100 intracranial stentings36 or male/female = 165 (82.5%):35 (17.5%) in a total of 200 carotid stentings.3 Further studies may clarify the different effects of BR according to sex, though the male predominance in our study might have affected the results.
Conclusions
Lesions in the apex of the carotid bulb had a lower BR and tended to have a higher event rate, which might be associated with periprocedural hypertension, a common finding in patients undergoing a procedure such as stent placement. By contrast, BR was more common in lesions of the carotid body, which is derived from the remnant of the third aortic arch and the third pharyngeal arch (the origin of the glossopharyngeal nerve), and this increased BR may help to reduce high blood pressure, which might otherwise contribute to hyperperfusion syndrome. Thus, our finding that BR varied in the 2 locations of carotid bulb lesions, which are of embryologically diverse origin, suggests that more careful management of blood pressure control in patients with apical lesions would be necessary after carotid stent placement.
Acknowledgments
We acknowledge the assistance of Sun Moon Whang, BS, and Eun Hye Kim, RN, with patient data collection, and of Yun Gyeong Jeong, with the preparation of the manuscript. We thank Bonnie Hami for her English editorial assistance.
Footnotes
-
This study was supported by a grant from the Korea Healthcare Technology R&D Project, Ministry of Health and Welfare, Republic of Korea (A080201).
Indicates open access to non-subscribers at www.ajnr.org
References
- 1.
- 2.
- 3.
- 4.
- 5.
- 6.
- 7.
- 8.
- 9.
- 10.
- 11.
- 12.
- 13.
- 14.
- 15.
- 16.
- 17.
- 18.
- 19.
- 20.
- 21.
- 22.
- 23.
- 24.
- 25.
- 26.
- 27.
- 28.
- 29.
- 30.
- 31.
- 32.
- 33.
- 34.
- 35.
- 36.
- Received April 30, 2011.
- Accepted after revision August 22, 2011.
- © 2012 by American Journal of Neuroradiology