Abstract
SUMMARY: Cervicogenic headache is a secondary headache syndrome attributable to upper cervical spine pathology. Osteoarthritis of the lateral atlantoaxial joint with resultant C2 dorsal root ganglion irritation is an important and potentially treatable cause of cervicogenic headache. In this case series, we present 11 patients with cervicogenic headache who underwent C2 dorsal root ganglion thermal radiofrequency ablation. Radiologists should be familiar with this efficacious procedure and technical considerations to avoid complications.
ABBREVIATIONS:
- DRG
- dorsal root ganglion
- RF
- radiofrequency
- RFA
- radiofrequency ablation
- VAS
- visual analog scale
Cervicogenic headache is a secondary headache syndrome attributable to upper cervical spine pathology, with an estimated prevalence of up to 4% of the general population and 20% of patients with chronic headache.1 Due to the convergence of upper cervical segment nociceptive afferents with the trigeminal complex, pain from the upper cervical nerves may be referred to the occipital, orbital, frontal, and/or parietal regions.2 Potential culprit nerves include the greater occipital nerve, lesser occipital nerve, and third occipital nerves, with the greater and lesser occipital nerves both receiving contributions from the C2 dorsal root ganglion (DRG).3,4 While cervicogenic headaches may occur from a variety of pathologies (including tumor, fracture, infection, and inflammatory arthritis), osteoarthritis of the lateral atlantoaxial joint with resultant C2 DRG irritation is an important and potentially treatable cause of cervicogenic headache.5 Image-guided pulsed or thermal radiofrequency ablation (RFA) of the C2 DRG has been described with high response rates.6⇓⇓-9 We report clinical outcomes of a series of 11 patients in whom C2 DRG thermal RFA was performed using a CT-guided technique.10
Case Series
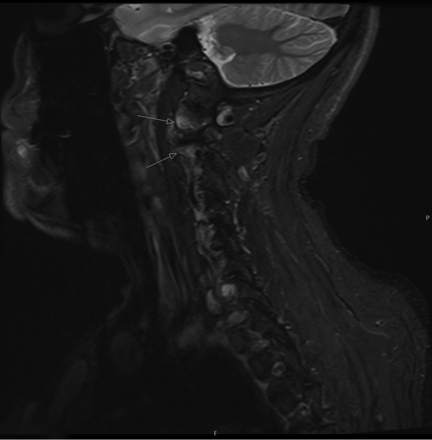
Institutional review board approval was obtained for this retrospective case series from the Hospital for Special Surgery and Weill Cornell Medicine IRBs. Patient characteristics and outcomes are described in the Online Supplemental Data. All 11 patients were diagnosed with cervicogenic headache after clinical evaluation and met the International Classification of Headache Disorders diagnostic criteria for having cervicogenic headache.11 All patients underwent preprocedural cervical MR imaging and demonstrated asymmetric T2 hyperintense edema within the C1–C2 lateral atlantoaxial joint, ipsilateral to the site of neck and occipital distribution pain (Fig 1).
Sagittal STIR image (patient 11) of the cervical spine showing T2 hyperintense bone marrow edema (arrows) in the lateral atlantoaxial (C1–C2) articulation.
From February 2019 through October 2021, eleven C2 DRG RFAs were performed. Cases were performed by a neuroradiologist with a Certificate of Added Qualification and 9 years of postfellowship experience and a musculoskeletal radiologist with 3 years of postfellowship experience. There were 4 men and 7 women in the cohort, with a mean age of 77 (SD, 7.8) years (median, 77 years; range, 62–90 years) (Online Supplemental Data). The C2 DRG RFA procedural technique and contraindications have been described previously.10 In brief, the patient is placed supine on the CT gantry and a noncontrast scan of the craniocervical junction is acquired with a CT grid in place. All patients were offered moderate sedation for the ablation procedure. A suitable entry site to target the C2 DRG is planned at the base of C2; it is critical to place the needle below the C1 ring just above the C2 lateral mass to avoid the traversing the V3 segment of the vertebral artery. By means of intermittent CT guidance, a 22-ga radiofrequency (RF) cannula with a 5-mm active tip (Abbott) is advanced to the C2 DRG (Fig 2). A small amount of nonionic iodinated contrast can be injected to confirm the appropriate position (Fig 3). Following sensory testing at 50 Hz up to 2 V to confirm the appropriate distribution of stimulation, thermal RFA can then be performed for 90 seconds at 80° centigrade (Abbott NeuroTherm; Greyline Medical). A C2 nerve block is then performed using a 1:1 mixture of 1 mL preservative-free dexamethasone, 10 mg/mL, and 0.5% bupivacaine; the needle is removed and sterile dressing applied. Patients are observed for 1 hour and discharged home.
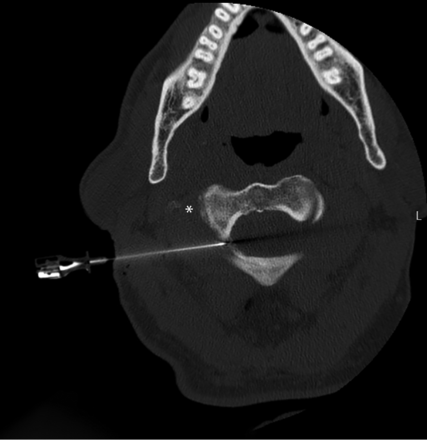
Intraprocedural axial CT image (patient 10) showing placement of a 22-ga RFA cannula at the expected location of the C2 DRG. The needle tip lies just above the C2 pedicle. The vertebral artery is safely located lateral to the C2 vertebral body at this level (asterisk).
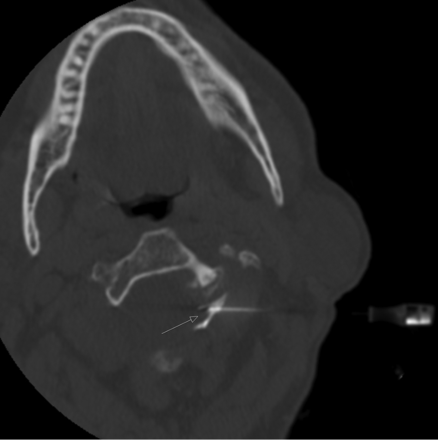
Intraprocedural axial CT image (patient 8) showing contrast injection surrounding the left the C2 DRG (arrow).
The mean preprocedural visual analog scale (VAS) pain score was 8 of 10. The mean postprocedural pain score was 2 of 10. (Table) There was a statistically significant reduction in the mean VAS score as determined by a 2-tailed Wilcoxon signed-rank test (P = .003). There were no major procedural complications. Three of 11 patients reported paresthesia in the occipital distribution with numbness and tingling. The mean follow-up was 10.4 months (range, 1–33 months). Most patients reduced or ceased the use of oral analgesics and reported improvement in lifestyle activities. All patients reported that they would undergo the procedure again if pain symptoms returned.
Patient outcome
DISCUSSION
Cervicogenic headache can have a variety of causes, and an accurate diagnosis is required to guide management.12 Significant overlap exists between cervicogenic headaches and other primary and secondary headache disorders, including migraine headache, tension-type headache, and occipital neuralgia.2 Occipital neuralgia, another secondary headache syndrome with occipital pain as a key feature, differs from cervicogenic headaches in that it is characterized by paroxysmal shooting or stabbing pain over the posterior scalp, typically radiating from the suboccipital region toward the vertex.4 In this cohort, patients were screened using cervical MR imaging and only considered for ablation if C1–C2 lateral mass bone marrow edema was present ipsilateral to the site of occipital distribution pain.
Patients with cervicogenic headaches may respond to local anesthetic blockade of the occipital nerves (greater occipital nerve, third occipital nerve, or both). The C2 DRG is the principal nerve root that contributes to the greater and lesser occipital nerves, providing an ideal target for ablation, because it only provides sensory innervation.13,14
Patients should be considered for C2 DRG RFA if they present with cervicogenic headaches and have failed conservative treatment options, including physical therapy and medication therapy. Diagnostic injections may be performed to exclude a peripheral occipital nerve entrapment. MR imaging of the cervical spine should be performed to evaluate the facet joints and upper cervical nerve roots. In the authors’ experience, a C2 nerve block without RFA does not provide sustained clinical relief, and the authors do not require a C2 block before performing C2 RFA. However, it is not unreasonable to consider a C2 anesthetic block to confirm the pain generator in cases in which it may be unclear.
Pre- or intraprocedural CT angiography may be performed to ensure a safe procedural approach. Vascular injury and vascular variants have been reported.15,16 The authors do not routinely perform vascular imaging before or during C2 ablation. However, preprocedural cervical MR imaging was always reviewed with attention to the vertebral artery and branch vessel flow voids.
Conventional (thermal) RFA generates sustained high temperature surrounding the active tip of an insulated cannula, resulting in neurodestruction. Pulsed RF is an alternative to thermal RF and has advantages, including a decreased potential for local thermal injury and a decreased incidence of postprocedural inflammation. However, pulsed RF is typically less efficacious than thermal ablation, with patients experiencing a shorter duration of pain relief, often necessitating repeat procedures.17
Periprocedural inflammation can cause significant pain and may be distressing for patients. C2 RFA was followed by a C2 DRG nerve block in our cohort using a nonparticulate steroid mixed with a long-acting anesthetic (1 mL of preservative-free dexamethasone, 10 mg/mL, and 0.5% bupivacaine). Clinical improvement of pain may take 2–4 weeks after the ablation but appears to be durable with thermal RFA. None of the patients in this case series had recurrent symptoms during the study period.
No major complications were encountered. No patients in this cohort went on to surgical fusion during the study period. Adverse effects from the procedure include numbness and paresthesia in the occipital distribution. However, all patients indicated they would undergo the procedure again if symptoms returned and numbness did not negatively impact quality of life. Potential risks include intra-arterial or intrathecal puncture and injection of medication, CSF leak, spinal cord puncture, and vertebral artery injury with a risk of stroke.18
Surgical C1–C2 fusion may be considered for patients who fail or have a suboptimal clinical response to C2 RFA. In refractory cases of severe degenerative arthropathy of the C1–C2 articulation, a technique for surgical fusion was described by Goel and Laheri19 and popularized by Harms et al.20 Patients with severe degenerative atlantoaxial arthropathy often have already lost a significant amount of cervical spine rotational motion, making surgical fusion for pain relief a viable option. In addition to the benefit of the elimination of motion around the C2 DRG, direct surgical decompression may be performed; however, nerve root compression is often dynamic. Implantation of cervical interfacet spacers into the C1–C2 joint has been described as a technique for indirect decompression (restoration of C2 foraminal height) with successful results.21
In conclusion, CT-guided C2 RFA appears to be a safe and efficacious procedure for the treatment of cervicogenic headache in patients with C1–C2 lateral mass bone marrow edema and ipsilateral symptomatology. Further prospective study is necessary to fully elucidate the durability of this intervention and compare it with alternative treatment options.
Footnotes
Disclosure forms provided by the authors are available with the full text and PDF of this article at www.ajnr.org.
References
- Received November 26, 2021.
- Accepted after revision January 14, 2022.
- © 2022 by American Journal of Neuroradiology