Abstract
BACKGROUND AND PURPOSE: Thyroid carcinoma arising in a thyroglossal duct cyst may be clinically indistinguishable from a benign thyroglossal duct cyst. The preoperative diagnosis of carcinoma, however, can have important implications for surgical planning and postoperative treatment. Our purpose was to describe the CT appearance of thyroglossal duct carcinoma and identify the features that distinguish thyroglossal duct carcinoma from benign thyroglossal duct cysts.
METHODS: Retrospective review of the medical records from the University of Pittsburgh Medical Center and Geisinger Medical Center (Danville, Pennsylvania) identified six patients with papillary thyroid carcinoma within the thyroglossal duct who had undergone preoperative CT examinations of the neck. There were two women and four men. Their ages ranged from 14 to 59 years. Three patients underwent contrast-enhanced CT of the neck, and three underwent unenhanced CT. All CT examinations consisted of 3- to 5-mm-thick contiguous axial sections.
RESULTS: Each patient had an anterior neck mass with a cystic component. Two of the masses had dense or enhancing mural nodules, two had irregular calcification throughout the mass, and two had dense or enhancing mural nodules with additional foci of calcification. One patient had cervical lymphadenopathy.
CONCLUSION: Carcinoma should be considered in thyroglossal duct cysts that have a mural nodule or calcification or both.
Thyroglossal duct cysts account for 70% of congenital neck masses (1). Thyroid carcinoma arising in a thyroglossal duct cyst is rare, affecting less than 1% of cysts (2). Thyroglossal duct carcinoma, however, may be clinically indistinguishable from a benign thyroglossal duct cyst. A preoperative radiologic diagnosis can change the type of surgery that is performed and provide prognostic information. We evaluated the CT appearance of six cases of thyroglossal duct carcinoma and identified the features that distinguish thyroglossal duct carcinoma from benign thyroglossal duct cysts.
Methods
We reviewed the digital medical records at the University of Pittsburgh Medical Center, Pittsburgh, Pennsylvania, from August 1981 to November 1998. Seventeen patients had a histologic diagnosis of thyroid carcinoma within the thyroglossal duct. (The high incidence of thyroglossal duct carcinoma is presumably the result of a wide referral base.) Three of the seventeen patients had preoperative CT scans of the neck that were available for retrospective review.
We reviewed the Cytopathology Department records from Geisinger Medical Center, Danville, Pennsylvania, from 1965 to 1997. Three patients were identified with histologically proven carcinoma within a thyroglossal duct cyst. All three had preoperative CT examinations available for retrospective review. (These three patients have been previously reported, and their CT findings briefly discussed [3].) No attempt was made to distinguish between primary thyroglossal duct tumors and metastatic disease from tumors in the thyroid gland.
Two of the patients were women and four were men. Their ages ranged from 14 to 59 years at the time of CT examination. All six patients were evaluated for a recently detected neck mass. None of the patients had a medical history pertinent to their neck mass. Three patients underwent contrast-enhanced CT of the neck, and three unenhanced CT. All CT examinations consisted of 3- to 5-mm-thick contiguous axial sections. One of the noncontrast examinations was available only on bone windows and was accompanied by a conventional radiograph of the neck.
Results
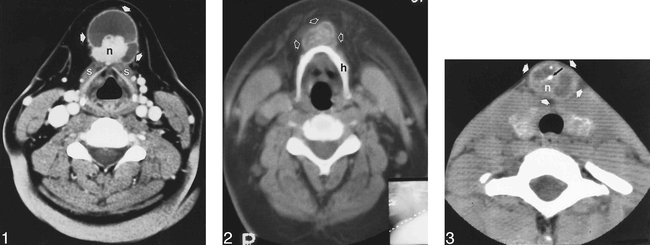
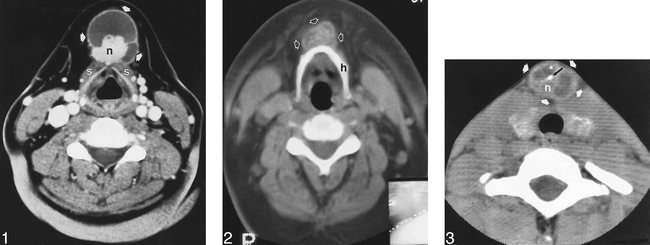
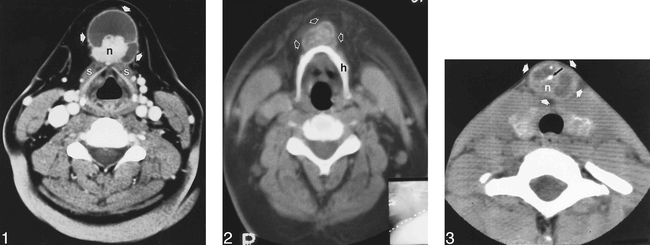
All six patients had anterior neck masses. Five of the masses were below the hyoid bone, and one was at the level of the hyoid. Four were in the midline, and two were slightly off midline. All six masses had a cystic component. Two had dense or enhancing mural nodules (Fig 1), two had irregular calcification throughout the mass (Fig 2), and two had dense or enhancing mural nodules with additional foci of calcification (Fig 3). The thyroid gland was included on four of the six scans. No definite thyroid gland abnormalities were noted, but the gland was partially obscured by artifact from the shoulders in all four cases. One patient had a large, heterogeneously dense or enhancing, partially calcified lymph node in the posterior cervical chain (Fig 4). A neck dissection in this patient revealed metastatic papillary thyroid carcinoma. The other five patients had no CT evidence of cervical lymphadenopathy, and lymph node dissections were not performed.
Papillary thyroid carcinoma of the thyroglossal duct. Contrast-enhanced CT at the level of the thyroid cartilage reveals a cystic mass in the anterior neck (arrows), inseparable from the strap muscles (s), with septation and a lobular mural nodule (n).
Papillary thyroid carcinoma of the thyroglossal duct. Unenhanced CT at the level of the hyoid bone reveals a cystic mass (arrows) anterior to the hyoid bone (h) with irregular calcifications throughout the mass.
Papillary thyroid carcinoma of the thyroglossal duct. Unenhanced CT at the level of the thyroid gland reveals a complex cystic mass (white arrows) with septations, a mural nodule (n), and calcifications (black arrow)
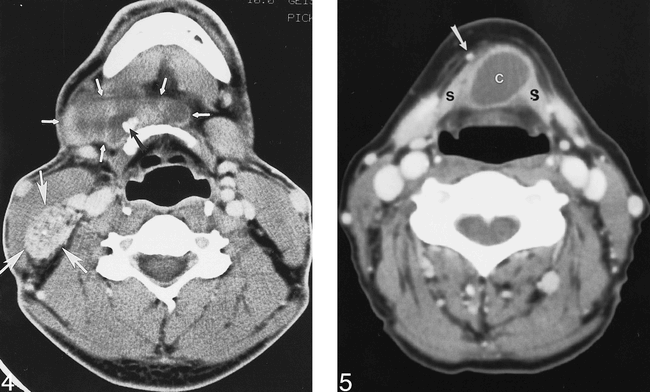
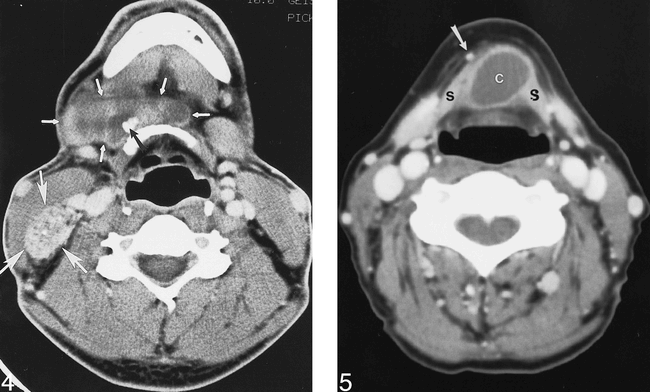
Papillary thyroid carcinoma of the thyroglossal duct. Contrast-enhanced CT at the level of the hyoid bone reveals a cystic and solid mass (small arrows) extending from the anterior hyoid bone to the right lateral neck. Calcifications are identified within the mass (black arrow). A large, heterogeneous mass with calcifications in the posterior right neck (large arrows) represents metastatic disease to a cervical lymph node.
All six patients underwent surgical removal of the neck mass. Histologic evaluation revealed papillary thyroid carcinoma in all six patients. Thyroidectomy was performed in two patients, and in one of these patients, a focus of papillary carcinoma was discovered in the thyroid isthmus despite normal preoperative scintigraphic findings. Long-term clinical follow-up was unavailable for all six patients.
Discussion
During the 3rd week of fetal life, the thyroid gland develops from the floor of the pharynx at the site that will become the foramen cecum. Over the next few weeks, the gland migrates inferiorly, crosses the hyoid bone, and reaches its normal position anterior to the trachea. The epithelial connection between the thyroid gland and the foramen cecum is called the thyroglossal duct. The duct is normally resorbed during the 8th to 10th week of fetal development. If the duct fails to involute completely, the remaining secretory epithelium may create a thyroglossal duct cyst (Fig 5) (4). The average age for presentation of a thyroglossal duct cyst is 6 years, and there is no sex predilection (5).
Benign thyroglossal duct cyst. Contrast-enhanced CT below the level of the hyoid bone reveals a cystic mass (c) inseparable from the strap muscles (s). The mass has a thin, smooth rim, and the contents are of fluid density. No calcifications are identified within the mass. The anterior jugular vein (arrow) is displaced by the mass
Histologic examination reveals carcinoma in less than 1% of thyroglossal duct cysts (2, 6). Patients with thyroglossal duct carcinoma have an average age of 40 years, but carcinoma has been reported in patients as young as 6 years. Thyroglossal duct carcinoma has a slight female predilection. These demographics are similar to those for carcinoma arising in the thyroid gland (7). The histologic findings of thyroglossal duct carcinoma are most commonly papillary carcinoma (75–80%), but other thyroid tumors such as follicular, Hürthle cell, and mixed papillary and follicular carcinomas have been reported (8). Most benign thyroglossal duct cysts contain microscopic foci of thyroid tissue (9), which are presumably the source of thyroglossal duct carcinoma. A metastasis to the thyroglossal duct from a primary thyroid gland tumor is also possible, although it may be difficult to determine which is the primary tumor and which is the metastasis (3). Invasion into surrounding soft tissue is seen in only 17% of thyroglossal duct carcinomas (8). Metastatic disease is present in 1.3%, which is much lower than the rate from carcinoma arising in the thyroid gland (8).
The clinical presentation of thyroglossal duct carcinoma may be indistinguishable from that of benign thyroglossal duct cysts (7, 10). Thyroglossal duct carcinoma may present with a rapidly enlarging neck mass (8), but the same history can be elicited in patients with recent infection in a benign cyst (10).
The surgical treatment for benign thyroglossal duct cysts is the Sistrunk procedure, in which the cyst, the central portion of the hyoid bone, and the entire thyroglossal tract are removed. The surgical treatment of thyroglossal duct carcinoma is controversial. Although some authors consider the Sistrunk procedure alone to be sufficient (7), recent reports recommend total thyroidectomy in addition to the Sistrunk procedure (3). In patients with abnormal cervical lymph nodes by clinical or radiographic criteria, the Sistrunk procedure combined with thyroidectomy and lymphadenectomy is widely accepted (3, 7). The removal of the thyroid gland allows for long-term monitoring of thyroglobulin levels and the use of I131 scintigraphy and I131 ablation therapy. Also, patients with thyroglossal duct carcinoma are at increased risk of carcinoma within the thyroid gland. It is unclear, in such patients, whether the thyroid gland or the thyroglossal duct is the primary tumor site (3).
Benign thyroglossal duct cysts are most often diagnosed clinically. There are two goals for preoperative diagnostic testing: documenting a normal thyroid gland, and determining whether the Sistrunk procedure is sufficient surgical treatment. Documenting a normal thyroid gland is important because an ectopic thyroid gland may mimic a thyroglossal duct cyst clinically. If this tissue is removed, the patient will be rendered hypothyroid (11). Should the preoperative evaluation reveal thyroid abnormalities or cervical lymphadenopathy, the surgical approach may be altered.
Some authors recommend contrast-enhanced CT of the neck for all suspected thyroglossal duct cysts (8), but others reserve CT for older patients, who have an increased risk of carcinoma (2); patients with recent infection, whose clinical presentation may suggest carcinoma (2); patients with a suprahyoid mass, who are at greater risk for ectopic thyroid (12); and patients with laryngeal symptoms, who may have preepiglottic or laryngeal tumor invasion (1).
On a CT scan, a benign thyroglossal duct cyst appears as a midline, fluid-attenuated mass near the level of the hyoid bone, with a thin, smooth wall (2). Infrahyoid thyroglossal duct cysts may be slightly off midline and are intimately associated with the strap muscles (Fig 5).
The thyroglossal duct carcinomas in our series were similar to benign thyroglossal duct cysts in location. The carcinomas, however, had either a dense or enhancing mural nodule, calcification within the cyst, or both. The contrast-enhanced CT studies could not distinguish between inherently dense nodules and enhancing nodules. In one case, a posterior cervical mass with heterogeneous high density indicated metastatic tumor to a cervical lymph node (Fig 4).
Calcifications are present in 60% of papillary carcinomas arising in the thyroid gland (13). These calcifications correspond to the psammoma bodies that are visible histologically. To our knowledge, there are no reports in the English-language literature of calcifications in a benign thyroglossal duct cyst.
Other entities may have CT findings similar to thyroglossal duct carcinoma. Infection in a thyroglossal duct cyst may increase the density of the cyst contents and thicken the cyst wall (Fig 6). Ectopic thyroid tissue anywhere along the thyroglossal duct tract appears as a dense or heterogeneous nodule (Fig 7). In our experience, however, all thyroglossal duct cysts with a mural nodule have proven to be carcinoma, and all thyroglossal duct carcinomas were at least partially cystic. A congenital dermoid tumor may appear as a cystic midline mass, and some dermoid tumors have mural nodules or debris (Fig 8). A dermoid tumor can be differentiated from a thyroglossal duct cyst if fat is detected within the lesion, and unlike a thyroglossal duct remnant, a dermoid tumor usually is not intimately associated with the strap muscles.
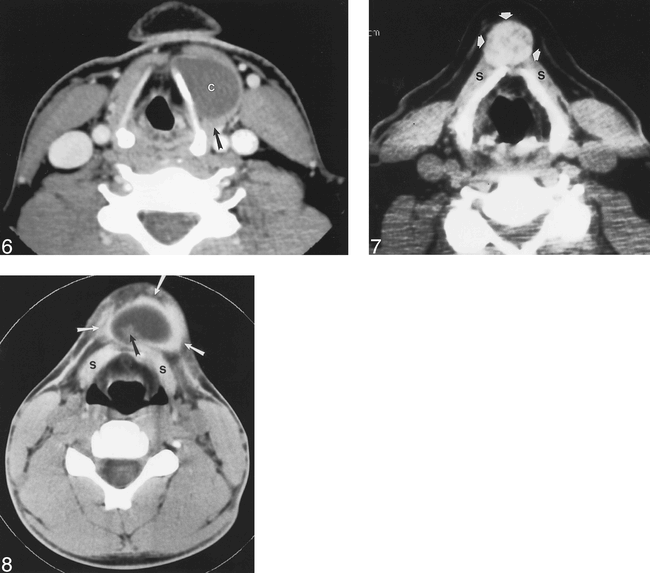
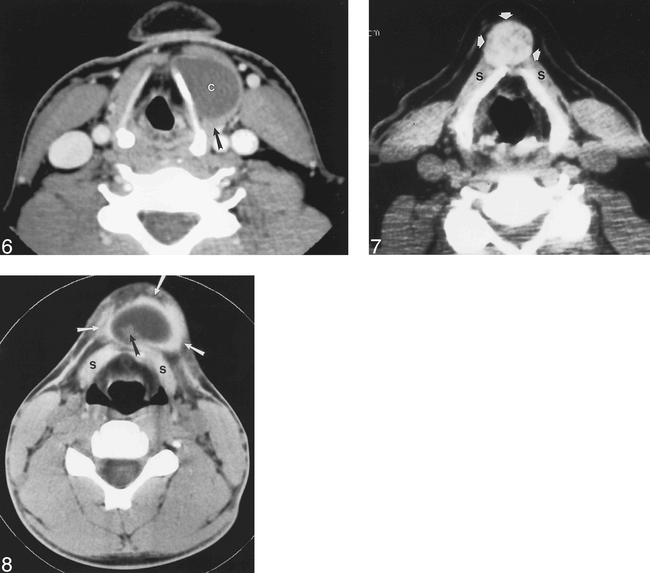
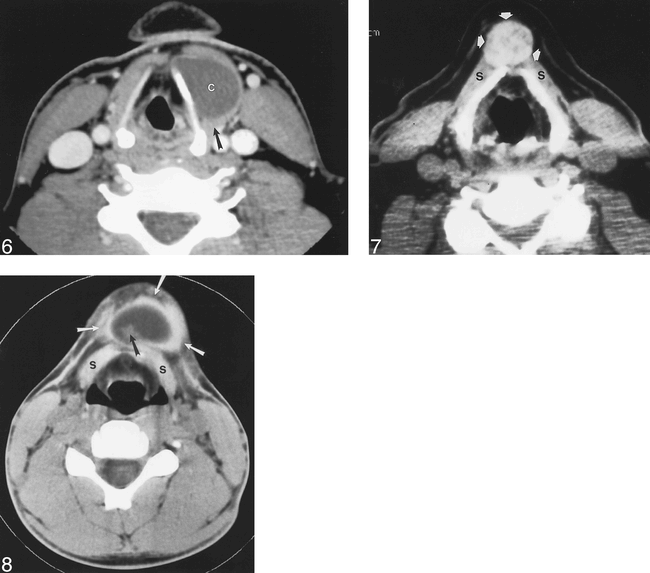
Previously infected thyroglossal duct cyst. Contrast-enhanced CT through the larynx reveals a cyst (c) adjacent to the left thyroid cartilage. The cyst contents are higher than fluid density. The posterior wall of the mass is thick (arrow), but no nodules are noted. The cyst contains no calcifications. The patient had multiple episodes of anterior neck pain prior to this examination.
Ectopic thyroid gland. Unenhanced CT at the level of the thyroid cartilage reveals a heterogeneous, dense, midline mass (arrows) intimately associated with the strap muscles (s). No cystic component is identified.
Dermoid tumor. Unenhanced CT below the level of the hyoid bone reveals a cystic midline mass (white arrows) anterior to the strap muscles (s). A mural nodule (black arrow) is noted within the mass. The center of the mass measured −20 HU, indicating fat content
Conclusion
Thyroglossal duct carcinoma is a rare complication of a thyroglossal duct cyst. Carcinoma should be considered in thyroglossal duct cysts that have a mural nodule or calcification. The preoperative diagnosis of carcinoma can have important implications for surgical planning and postoperative treatment.
Footnotes
1 Presented in part at the 37th annual meeting of the American Society of Neuroradiology, May 1999; San Diego, CA.
2 Address reprint requests to Barton F. Branstetter, M.D., Department of Radiology, University of Pittsburgh Medical Center, 200 Lothrop Street, Pittsburgh, PA 15213.
References
- Received October 22, 1999.
- Accepted after revision March 10, 2000.
- Copyright © American Society of Neuroradiology