Case of the Week
Section Editors: Matylda Machnowska1 and Anvita Pauranik2
1University of Toronto, Toronto, Ontario, Canada
2BC Children's Hospital, University of British Columbia, Vancouver, British Columbia, Canada
Sign up to receive an email alert when a new Case of the Week is posted.
August 6, 2020
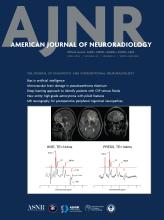
Intracranial Mesenchymal Chondrosarcoma
- Background:
- Intracranial mesenchymal chondrosarcoma (IMCS) is a rare type of extraskeletal chondrosarcoma that has a predilection for the CNS, head, and neck. The most common location in the CNS is the craniospinal meninges, arising from the dura of the supratentorial region.
- Incidence peaks in the second to third decades of life (age range 2 months to 71 years), with a female predilection.
- The pathogenesis of this entity is unclear and various cell origins, such as embryonic cartilaginous remnants in meninges, dural fibroblasts, and meningeal multipotent mesenchymal cells, have been proposed.
-
Its characteristic histologic appearance presenting in the typical form is that of a bimorphic pattern consisting of undifferentiated small round cells mixed with islands of well-differentiated cartilaginous matrix.
- Clinical Presentation:
- Symptoms related to mass effect and increased intracranial pressure, including headache, cognitive decline, visual symptoms, vomiting, gait imbalance, seizures, and hemiparesis
- Key Diagnostic Features:
-
CT shows a mass with heterogeneous density with scattered hyperdensities (chondroid matrix). Additionally, the mass may erode adjacent bone.
-
On MRI, these lesions are hypo- or isointense on T1-weighted images and hyperintense on T2-weighted images, with islands of low signal intensity that are also seen on gradient-echo sequence representing well-differentiated cartilage.
-
On postcontrast CT and MR images, they show vivid heterogeneous enhancement.
-
On DSA/angiography, they sometimes resemble arteriovenous malformations due to high vascularity and large increased flow voids. These lesions may present with intracerebral or subarachnoid hemorrhage.
-
- Differential Diagnoses:
- Meningioma: Avidly enhancing; hyperostosis of underlying calvarium and dural tail
- Primitive neuroectodermal tumor (PNET): Often shows restricted diffusion; leptomeningeal seeding is common.
- Oligodendroglioma: Cortically based tumors; 70–90% show calcification; may have pressure remodeling of the adjacent skull
- Hemangiopericytoma: Avid enhancement; erosion of adjacent bone; on MRS high myoinositol and absent alanine peak
- Treatment:
- The favored treatment is surgical removal. This may be preceded with angiography and presurgical embolization to reduce blood loss and help accomplish a wide tumor resection.
- Adjuvant radiotherapy may be performed (however, this needs further study).
-
Close follow-up monitoring