Abstract
Objectives
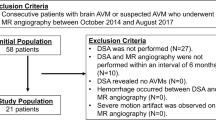
To prospectively evaluate the diagnostic value of 3D fast spin-echo (FSE) T1 black-blood magnetic resonance (MR) imaging (3D CUBE T1WI) in comparison with contrast-enhanced MR venography (CE-MRV) in the detection of sinus invasion by meningiomas.
Methods
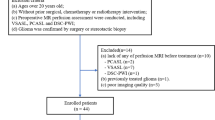
In this study forty consecutive patients with suspected meningiomas adjacent to venous sinus underwent conventional MR imaging, CE-MRV and 3D CUBE T1WI scans. Images obtained by each technique were assessed independently by two neuroradiologists for (1) wall invasion and (2) lumen occlusion of the target venous sinus.
Results
The use of 3D CUBE T1W imaging was found to provide an easy way to detect the venous wall invasion by para-sinus lesions. The interobserver agreement was excellent (κ = 0.843; 95% confidence interval CI 0.757–0.929) and the result was highly consistent with the surgical findings (sensitivity 90.48%, specificity 94.12%). In the analysis of the lumen occlusion, the interobserver agreement obtained by 3D CUBE T1WI sequence was excellent (κ = 0.956; 95% CI, 0.913–0.999) with a diagnostic accuracy of 94.74%, which surpassed CE-MRV not only in interobserver agreement (κ = 0.736; 95% CI, 0.639–0.833) but also in diagnostic value (accuracy = 68.42%). Among 38 patients with meningiomas, the existence and extent of peritumoral edema did not correlate with the invasion of adjacent venous sinus.
Conclusion
Currently, 3D CUBE T1WI sequence is a reliable technique to provide accurate assessment about the venous sinus invasion by meningioma. Meanwhile, CE-MRV is more suitable in the evaluation of the bypass draining veins around the tumor.



Similar content being viewed by others
References
Marosi C, Hassler M, Roessler K, Reni M, Sant M, Mazza E, Vecht C. Meningioma. Crit Rev Oncol Hematol. 2008;67(2):153–71.
Barnholtz-Sloan JS, Kruchko C. Meningiomas: causes and risk factors. Neurosurg Focus. 2007;23(4):E2.
Rogers L, Barani I, Chamberlain M, Kaley TJ, McDermott M, Raizer J, Schiff D, Weber DC, Wen PY, Vogelbaum MA. Meningiomas: knowledge base, treatment outcomes, and uncertainties. A RANO review. J Neurosurg. 2015;122(1):4–23.
Mantovani A, Di Maio S, Ferreira MJ, Sekhar LN. Management of meningiomas invading the major dural venous sinuses: operative technique, results, and potential benefit for higher grade tumors. World Neurosurg. 2014;82(3-4:455–67.
Mathiesen T, Pettersson-Segerlind J, Kihlström L, Ulfarsson E. Meningiomas engaging major venous sinuses. World Neurosurg. 2014;81(1):116–24.
Sindou M. Meningiomas involving major dural sinuses: should we attempt at radical removal and venous repair? World Neurosurg. 2014;81(1):46–7.
Alexiou GA, Gogou P, Markoula S, Kyritsis AP. Management of meningiomas. Clin Neurol Neurosurg. 2010;112(3):177–82.
DiMeco F, Li KW, Casali C, Ciceri E, Giombini S, Filippini G, Broggi G, Solero CL. Meningiomas invading the superior sagittal sinus: surgical experience in 108 cases. Neurosurgery. 2004;55(6):1263–72. discussion 1272-4.
Sindou M. Meningiomas invading the sagittal or transverse sinuses, resection with venous reconstruction. J Clin Neurosci. 2001;8 Suppl 1:8-11.
Brotchi J. Should we pursue superior sagittal sinus grafting in parasagittal meningiomas in 2013? World Neurosurg. 2014;82(3-4):325-6.
Lettau M1, Sartor K, Heiland S, Hähnel S. 3T high-spatial-resolution contrast-enhanced MR angiography of the intracranial venous system with parallel imaging. AJNR Am J Neuroradiol. 2008;30(1):185–7.
Lee JM, Jung S, Moon KS, Seo JJ, Kim IY, Jung TY, Lee JK, Kang SS. Preoperative evaluation of venous systems with 3‑dimensional contrast-enhanced magnetic resonance venography in brain tumors: comparison with time-of-flight magnetic resonance venography and digital subtraction angiography. Surg Neurol. 2005;64(2):128-33; discussion 133-4.
Li ML, Xu YY, Hou B, Sun ZY, Zhou HL, Jin ZY, Feng F, Xu WH. High-resolution intracranial vessel wall imaging using 3D CUBE T1 weighted sequence. Eur J Radiol. 2016;85(4):803–7.
Saam T, Habs M, Pollatos O, Cyran C, Pfefferkorn T, Dichgans M, Dietrich O, Glaser C, Reiser MF, Nikolaou K. High-resolution black-blood contrast-enhanced T1 weighted images for the diagnosis and follow-up of intracranial arteritis. Br J Radiol. 2010;83(993):e182–4.
Ryoo S, Cha J, Kim SJ, Choi JW, Ki CS, Kim KH, Jeon P, Kim JS, Hong SC, Bang OY. High-resolution magnetic resonance wall imaging findings of moyamoya disease. Stroke. 2014;45(8):2457–60.
Edjlali M, Roca P, Rabrait C, Naggara O, Oppenheim C. 3D fast spin-echo T1 black-blood imaging for the diagnosis of cervical artery dissection. AJNR Am J Neuroradiol. 2013;34(9):E103–6.
Mihai G, Winner MW, Raman SV, Rajagopalan S, Simonetti OP, Chung YC. Assessment of carotid stenosis using three-dimensional T2-weighted dark blood imaging: initial experience. J Magn Reson Imaging. 2012;35(2):449–55.
Qiao Y, Steinman DA, Qin Q, Etesami M, Schär M, Astor BC, Wasserman BA. Intracranial arterial wall imaging using three-dimensional high isotropic resolution black blood MRI at 3.0 Tesla. J Magn Reson Imaging. 2011;34(1):22–30.
Yang Q, Duan J, Fan Z, Qu X, Xie Y, Nguyen C, Du X, Bi X, Li K, Ji X, Li D. Early detection and quantification of cerebral venous thrombosis by magnetic resonance black-blood thrombus imaging. Stroke. 2016;47(2):404–9.
Nanda A, Bir SC, Konar S, Maiti TK, Bollam P. World health organization grade I convexity meningiomas: study on outcomes, complications and recurrence rates. World Neurosurg. 2016;89:620–627.e2.
Sindou MP, Alvernia JE. Results of attempted radical tumor removal and venous repair in 100 consecutive meningiomas involving the major dural sinuses. J Neurosurg. 2016;105(4):514–525
Osawa T, Tosaka M, Nagaishi M, Yoshimoto Y. Factors affecting peritumoral brain edema in meningioma: special histological subtypes with prominently extensive edema. J Neurooncol. 2013;111(1):49–57.
Bitzer M, Wöckel L, Morgalla M, Keller C, Friese S, Heiss E, Meyermann R, Grote E, Voigt K. Peritumoural brain oedema in intracranial meningiomas: influence of tumour size, location and histology. Acta Neurochir (Wien). 1997;139(12):1136–42.
Tamiya T, Ono Y, Matsumoto K, Ohmoto T. Peritumoral brain edema in intracranial meningiomas: effects of radiological and histological factors. Neurosurgery. 2001;49(5):1046–51. discussion 1051-2.
Raza SM, Gallia GL, Brem H, Weingart JD, Long DM, Olivi A. Perioperative and long-term outcomes from the management of parasagittal meningiomas invading the superior sagittal sinus. Neurosurgery. 2010;67(4):885–93. discussion 893.
Funding
This project was supported by the National Natural Science Foundation of China (Grant No. 81471627, 81501435).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
D. Wang, Y. Lu, B. Yin, M. Chen, D. Geng, L. Liu, J. Wen, P. Zhong and Y. Li declare that they have no competing interests.
Ethical standards
The present study was approved by the local ethics committee at Fudan University. Informed consents from all patients were obtained before enrolment.
Additional information
D. Wang, Y. Lu, B. Yin and M. Chen contributed equally to the work.
This research Originated from Department of Radiology, Huashan Hospital, Fudan University, 12 Wulumuqi Rd. Middle, Shanghai 200040, China
Rights and permissions
About this article
Cite this article
Wang, D., Lu, Y., Yin, B. et al. 3D Fast Spin-Echo T1 Black-Blood Imaging for the Preoperative Detection of Venous Sinus Invasion by Meningioma. Clin Neuroradiol 29, 65–73 (2019). https://doi.org/10.1007/s00062-017-0637-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-017-0637-1