Abstract
Purpose
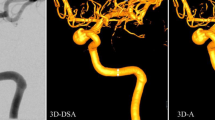
The three-dimensional digital subtraction angiography (3D DSA) technique is the current standard and is based on both mask and fill runs to enable the subtraction technique. Artificial intelligence (AI)-based 3D angiography (3DA) was developed to reduce radiation dosage because only one contrast-enhanced run of the C‑arm system is required for reconstruction of DSA-like 3D volumes. The aim was the evaluation of this algorithm regarding its diagnostic information.
Methods
3D DSA datasets without pathologic findings were reconstructed both with subtraction technique and with the AI-based algorithm. Corresponding reconstructions were evaluated by 2 neuroradiologists with respect to image quality (IQ), visualization of major segments of the circle of Willis (ICA = C4-C7; OphA; ACA = A1-A2, MCA = M1-M2; VA = V4; BA; AICA; SUCA; PCA = P1-P2), identifiability of perforators (lenticulostriate/thalamoperforating arteries) and vessel diameters (ICA = C4; MCA = M1; BA; PCA = P1).
Results
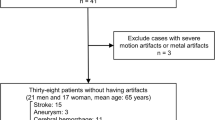
In total 15 datasets were successfully reconstructed as 3D DSA and 3DA with diagnostic image quality. All major segments of the circle of Willis and perforators were comparably visualized with 3DA. Quantitative analysis of vessel diameters in 3D DSA and 3DA datasets was equivalent and did not show relevant differences (rICA = 0.901, p = 0.001; rM1 = 0.951, p = 0.001; rBA = 0.906, p = 0.001; rP1 = 0.991, p = 0.001).
Conclusions
The use of 3DA demonstrated reliable visualization of cerebral vasculature with respect to quantitative and qualitative parameters. Therefore, 3DA is a promising method that might help to reduce patient radiation.



Similar content being viewed by others
References
Wong SC, Nawawi O, Ramli N, Abd Kadir KA. Benefits of 3D rotational DSA compared with 2D DSA in the evaluation of intracranial aneurysm. Acad Radiol. 2012;19:701–7.
van Rooij WJ, Sprengers ME, de Gast AN, Peluso JP, Sluzewski M. 3D rotational angiography: the new gold standard in the detection of additional intracranial aneurysms. AJNR Am J Neuroradiol. 2008;29:976–9.
Mistretta CA, Crummy AB, Strother CM. Digital angiography: A perspective. Radiology. 1981;139:273–6.
Hochmuth A, Spetzger U, Schumacher M. Comparison of three-dimensional rotational angiography with digital subtraction angiography in the assessment of ruptured cerebral aneurysms. AJNR Am J Neuroradiol. 2002;23:1199–205.
Anxionnat R, Bracard S, Ducrocq X, Trousset Y, Launay L, Kerrien E, Braun M, Vaillant R, Scomazzoni F, Lebedinsky A, Picard L. Intracranial aneurysms: clinical value of 3D digital subtraction angiography in the therapeutic decision and endovascular treatment. Radiology. 2001;218:799–808.
Missler U, Hundt C, Wiesmann M, Mayer T, Brückmann H. Threedimensional reconstructed rotational digital subtraction angiography in planning treatment of intracranial aneurysms. Eur Radiol. 2000;10:564–8.
Struffert T, Hauer M, Banckwitz R, Köhler C, Royalty K, Doerfler A. Effective dose to patient measurements in flat-detector and multislice computed tomography: a comparison of applications in neuroradiology. Eur Radiol. 2014;24:1257–65.
Pearl MS, Torok CM, Messina SA, Radvany M, Rao SN, Ehtiati T, Thompson CB, Gailloud P. Reducing radiation dose while maintaining diagnostic image quality of cerebral three-dimensional digital subtraction angiography: an in vivo study in swine. J Neurointerv Surg. 2014;6:672–6.
Pearl MS, Torok C, Katz Z, Messina SA, Blasco J, Tamargo RJ, Huang J, Leigh R, Zeiler S, Radvany M, Ehtiati T, Gailloud P. Diagnostic quality and accuracy of low dose 3D-DSA protocols in the evaluation of intracranial aneurysms. J Neurointerv Surg. 2015;7:386–90.
Grass M, Koppe R, Klotz E, Proksa R, Kuhn MH, Aerts H, Op de Beek J, Kemkers R. Three-dimensional reconstruction of high contrast objects using C‑arm image intensifier projection data. Comput Med Imaging Graph. 1999;23:311–21.
Raabe A, Beck J, Rohde S, Berkefeld J, Seifert V. Three-dimensional rotational angiography guidance for aneurysm surgery. J Neurosurg. 2006;105:406–11.
Gosch D, Kurze W, Deckert F, Schulz T, Patz A, Kahn T. Radiation exposure with 3D rotational angiography of the skull. Rofo. 2006;178:880–5.
Beck J, Rohde S, Berkefeld J, Seifert V, Raabe A. Size and location of ruptured and unruptured intracranial aneurysms measured by 3‑dimensional rotational angiography. Surg Neurol. 2006;65:18–27.
Hirai T, Korogi Y, Suginohara K, Ono K, Nishi T, Uemura S, Yamura M, Yamashita Y. Clinical usefulness of unsubtracted 3D digital angiography compared with rotational digital angiography in the pretreatment evaluation of intracranial aneurysms. AJNR Am J Neuroradiol. 2003;24:1067–74.
Montoya JC, Li Y, Strother C, Chen GH. 3D deep learning Angiography (3D-DLA) from C‑arm Conebeam CT. AJNR Am J Neuroradiol. 2018;39:916–22.
Goodfellow I, Bengio Y, Courville A. Deep learning. Cambridge: MIT Press; 2016.
Van den Oord A, Dieleman S, Zen H, Simonyan K, Vinyals O, Graves A, Kalchbrenner N, Senior A, Kavukcuoglu K. Wavenet: a generative model for raw audio. 2016. arXiv: 1609.03499v2[cs.SD].
Yu F, Koltun V. Multi-scale context aggregation by dilated convolutions. 2016. arXiv: 1511.07122v3[cs.CV].
Chun CW, Kim BS, Lee CH, Ihn YK, Shin YS. Patient radiation dose in diagnostic and interventional procedures for intracranial aneurysms: experience at a single center. Korean J Radiol. 2014;15:844–9.
Kim DJ, Park MK, Jung DE, Kang JH, Kim BM. Radiation dose reduction without compromise to image quality by alterations of filtration and focal spot size in cerebral angiography. Korean J Radiol. 2017;18:722–8.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
S. Lang, P. Hoelter, S. Manuel, F. Eisenhut, C. Kaethner, M. Kowarschik, H. Lücking and A. Doerfler declare that they have no competing interests.
Additional information
Disclaimer
The concepts and results presented in this paper are based on research and are not commercially available.
Rights and permissions
About this article
Cite this article
Lang, S., Hoelter, P., Schmidt, M. et al. Evaluation of an Artificial Intelligence-Based 3D-Angiography for Visualization of Cerebral Vasculature. Clin Neuroradiol 30, 705–712 (2020). https://doi.org/10.1007/s00062-019-00836-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-019-00836-7