Abstract
Purpose
To determine the perfusion-sensitive characteristics of cerebral dural metastases and compare them with the data on meningiomas.
Methods
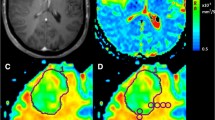
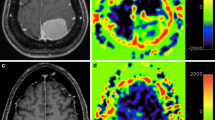
Twenty-two patients presenting with dural tumor underwent conventional and dynamic susceptibility-contrast MR imaging: breast carcinoma metastases, two patients; colorectal carcinoma metastasis, one patient; lung carcinoma metastasis, one patient; Merkel carcinoma metastasis, one patient; lymphoma, one patient; meningiomas, 16 patients. The imaging characteristics were analyzed using conventional MR imaging. The cerebral blood volume (CBV) maps were obtained for each patient and the relative CBV (rCBV) in different areas was calculated using the ratio between the CBV in the pathological area (CBVp) and in the contralateral white matter (CBVn).
Results
The differentiation between a meningioma and a dural metastasis can be difficult using conventional MR imaging. The rCBVs of lung carcinoma metastasis (1 case: 1.26), lymphoma (1 case: 1.29), breast carcinoma metastasis (2 cases: 1.50,1.56) and rectal carcinoma metastasis (1 case: 3.34) were significantly lower than that of meningiomas (16 cases: mean rCBV = 8.97±4.34, range 4–18). Merkel carcinoma metastasis (1 case: 7.56) showed an elevated rCBV, not different from that of meningiomas.
Conclusion
Dural metastases are sometimes indistinguishable from meningiomas using conventional MR imaging. rCBV mapping can provide additional information by demonstrating a low rCBV which may suggest the diagnosis of metastasis.




Similar content being viewed by others
References
Simionescu M. Metastatic tumors of the brain: a follow-up study of 195 patients with neurosurgical considerations. J Neurosurg 1960; 17:361–373.
Johnson MD, Powell S, Boyer P, Weil R, Moots P. Dural lesions mimicking meningiomas. Hum Pathol 2002; 33:1211–1226.
Khalfallah M, Roche P, Figarrela-Branger D, Malca S, Pellet W. Isolated dural metastasis mimicking meningioma. A case report. Neurochirurgie 1999; 45:250–254.
Rumana C, Hess K, Shi W, Sawaya R. Metastatic brain tumors with dural extension. J Neurosurg 1998; 89:552–558.
Tagle P, Villanueva P, Torrealba G, Huete I. Intracranial metastasis or meningioma ? An uncommon clinical diagnostic dilemma. Surg Neurol 2002; 58:241–245.
Cha S, Knopp E, Johnson G, Wetzel S, Litt A, Zagzag D. Intracranial mass lesions: dynamic contrast-enhanced susceptibility-weighted echo-planar perfusion MR imaging. Radiology 2002; 223:11–29.
Griebel J, Mayr N, De Vries, Knopp MV, Gneiting T, Kremser C, et al. Assessment of tumor microcirculation: a new role of dynamic contrast MR imaging. J Magn Reson Imaging 1997; 7:111–119.
Pathak AP, Schmainda K, Ward B, Linderman J, Rebro K, Greene A. MR-derived cerebral blood volume maps: issues regarding histological validation and assessment of tumor angiogenesis. Magn Reson Med 2001; 46:735–747.
Barbier E, Lamalle L, Decorps M. Methodology of brain perfusion imaging. J Magn Reson Imaging 2001; 13:496–520.
Provenzale JM, Wang GR, Brenner T, Petrella JR, Sorensen AG. Comparison of permeability in high-grade and low-grade brain tumors using dynamic susceptibility contrast MR imaging. AJR Am J Roentgenol 2002; 178:711–716.
Hartmann M, Heiland S, Harting I, Tronnier VM, Sommer C, Ludwig R, et al. Distinguishing of primary cerebral lymphoma from high grade glioma with perfusion weighted magnetic resonance imaging. Neuroscience Lett 2003; 338:119–122.
Kremer S, Grand S, Remy C, Esteve F, Lefournier V, Pasquier B, et al. Cerebral blood volume mapping by MR imaging in the initial evaluation of brain tumors. J Neuroradiol 2002; 29:105–113.
Maeda M, Itoh S, Kimura H, Iwasaki T, Hayashi N, Yamamoto K, et al. Vascularity of meningiomas and neurinomas: assessment with dynamic susceptibility contrast MR imaging. AJR Am J Roentgenol 1994; 163:181–186.
Kleihues P, Cavenee W, eds. Pathology and genetics of tumours of the nervous system, 2nd edn. Lyon: International Agency for Research, 2000.
Rosen B, Belliveau J, Vevea J, Brady T. Perfusion imaging with NMR contrast agents. Magn Reson Med 1990; 14:249–265.
Sheporaitis L, Osborn A, Smirniotopoulos J, Clunie D, Howieson J, D’agostino A. Radiologic-pathologic correlation: intracranial meningioma. Am J Neuroradiol 1992; 13:29–37.
Buetow M, Buetow P, Smimiotopoulos J. Typical, atypical, and misleading features in meningioma. Radiographics 1991; 11:1087–1106.
Goldsher D, Litt A, Pinto R, Bannon K, Kricheff I. Dural “tail” associated with meningiomas on Gd-DTPA-enhanced MR images: characteristics, differential diagnostic value, and possible implications for treatment. Radiology 1990; 176:447–450.
Nakau H, Miyazawa T, Tamai S, Tsuchiya K, Shima K, Shirotani T, et al. Pathologic significance of meningeal enhancement (“flare sign”) of meningiomas on MRI. Surg Neurol 1997; 48:584–591.
Tokumaru A, O’uchi T, Eguchi T, Kawamoto S, Kokubo T, Suzuki M, et al.. Prominent meningeal enhancement adjacent to meningioma on Gd-DTPA-enhanced MR images: histopathologic correlation. Radiology 1990; 175:431–433.
Wilms G, Lammens M, Marchal G, Calenbergh FV, Plets C, Van Frayenhoven L, et al.. Thickening of dura surrounding meningiomas: MR features. J Comput Assist Tomogr 1989; 13:763–768.
Quint D, McGillicuddy J. Meningeal metastasis of the cerebellopontine angle demonstrating “dural tail” sign. Can Assoc Radiol J 1994; 45:40–43.
Wilms G, Lammens M, Marchal G, Demaerel P, Verplancke J, Van Calenbergh F, et al. Prominent dural enhancement adjacent to nonmeningiomatous malignant lesions on contrast-enhanced MR images. AJNR Am J Neuroradiol 1991; 12:761–764.
Kremer S, Grand S, Berger F, Hoffmann D, Pasquier B, Remy C, et al. Dynamic contrast-enhanced MRI: differentiating melanoma and renal carcinoma metastases from high-grade astrocytomas and other metastases. Neuroradiology 2003; 45:44–49.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kremer, S., Grand, S., Rémy, C. et al. Contribution of dynamic contrast MR imaging to the differentiation between dural metastasis and meningioma. Neuroradiology 46, 642–648 (2004). https://doi.org/10.1007/s00234-004-1194-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-004-1194-2