Abstract
Introduction
Delayed onset of non-ischemic cerebral enhancing (NICE) lesions is a rare complication of intracranial aneurysms’ endovascular therapy (EVT). The purpose of this study is to report this rare complication and its potential pathophysiology in a single-center case series and review the relevant literature.
Methods
After retrospective review of all patients managed by EVT at our institution from January 1, 2012 to December 31, 2014, 2 out of 374 patients (0.5 %) with such a complication were identified. Skin patch testing was performed with all endovascular devices used in the two patients and with the European baseline series, including nickel. All previously published cases in the English literature were reviewed based on exhaustive PubMed and Embase research.
Results
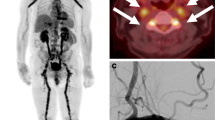
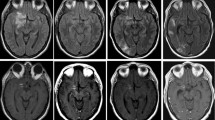
Patient no. 1 developed NICE lesions 1 month after balloon-assisted coiling of a ruptured anterior communicating artery aneurysm. Patient no. 2 developed NICE lesions 12 months (the longest delay reported to date for such a complication) after the treatment of a right carotid-ophthalmic aneurysm by loose coiling and flow diversion. Patient no. 2 demonstrated nickel skin reactivity, but none of the two patients presented allergic reaction to the devices used during interventions.
Conclusions
Based on our observations and review of the literature, we hypothesize that delayed non-ischemic cerebral enhancing lesions after EVT are more likely related to foreign body emboli rather than nickel allergy. The two presented cases demonstrate the potential for recurrence and prolonged fluctuation of NICE lesions, warranting long-term follow-up for all patients presenting this complication.



Similar content being viewed by others
Abbreviations
- ACA:
-
Anterior cerebral artery
- ACom:
-
Anterior communicating artery
- CT:
-
Computed tomography
- DAC:
-
Distal access catheter
- DCI:
-
Delayed cerebral ischemia
- DIPH:
-
Delayed ipsilateral parenchymal hemorrhage
- DSA:
-
Digital subtraction angiography
- DWI:
-
Diffusion-weighted imaging
- EVT:
-
Endovascular therapy
- ICA:
-
Internal carotid artery
- JAK2:
-
Janus kinase 2
- FDS:
-
Flow diverter stent
- FLAIR:
-
Fluid-attenuated inversion recovery
- MCA:
-
Middle cerebral artery
- MRI:
-
Magnetic resonance imaging
- NICE:
-
Non-ischemic cerebral enhancing
- PCA:
-
Posterior cerebral artery
- PCom:
-
Posterior communicating artery
- PVP:
-
Polyvinylpyrrolidone
- SAH:
-
Subarachnoid hemorrhage
References
Molyneux AJ, Birks J, Clarke A et al (2015) The durability of endovascular coiling versus neurosurgical clipping of ruptured cerebral aneurysms: 18 year follow-up of the UK cohort of the International Subarachnoid Aneurysm Trial (ISAT). Lancet Lond Engl 385:691–697. doi:10.1016/S0140-6736(14)60975-2
Pierot L, Wakhloo AK (2013) Endovascular treatment of intracranial aneurysms: current status. Stroke J Cereb Circ 44:2046–2054. doi:10.1161/STROKEAHA.113.000733
Cruz JP, Marotta T, O’Kelly C et al (2014) Enhancing brain lesions after endovascular treatment of aneurysms. AJNR Am J Neuroradiol 35:1954–1958. doi:10.3174/ajnr.A3976
Fealey ME, Edwards WD, Giannini C et al (2008) Complications of endovascular polymers associated with vascular introducer sheaths and metallic coils in 3 patients, with literature review. Am J Surg Pathol 32:1310–1316. doi:10.1097/PAS.0b013e318165582a
Lobotesis K, Mahady K, Ganesalingam J et al (2015) Coiling-associated delayed cerebral hypersensitivity: is nickel the link? Neurology 84:97–99. doi:10.1212/WNL.0000000000001106
Shapiro M, Ollenschleger MD, Baccin C et al (2015) Foreign body emboli following cerebrovascular interventions: clinical, radiographic, and histopathologic features. AJNR Am J Neuroradiol. doi:10.3174/ajnr.A4415
Skolarus LE, Gemmete JJ, Braley T et al (2010) Abnormal white matter changes after cerebral aneurysm treatment with polyglycolic-polylactic acid coils. World Neurosurg 74:640–644. doi:10.1016/j.wneu.2010.03.026
Ulus S, Yakupoğlu A, Kararslan E et al (2012) Reversible intracranial parenchymal changes in MRI after MCA aneurysm treatment with stent-assisted coiling technique; possible nickel allergy. Neuroradiology 54:897–899. doi:10.1007/s00234-012-1048-2
Uter W, Aberer W, Armario-Hita JC et al (2012) Current patch test results with the European baseline series and extensions to it from the “European Surveillance System on Contact Allergy” network, 2007-2008. Contact Dermatitis 67:9–19. doi:10.1111/j.1600-0536.2012.02070.x
Honari G, Ellis SG, Wilkoff BL et al (2008) Hypersensitivity reactions associated with endovascular devices. Contact Dermatitis 59:7–22. doi:10.1111/j.1600-0536.2008.01351.x
Dasika UK, Kanter KR, Vincent R (2003) Nickel allergy to the percutaneous patent foramen ovale occluder and subsequent systemic nickel allergy. J Thorac Cardiovasc Surg 126:2112
Fukahara K, Minami K, Reiss N et al (2003) Systemic allergic reaction to the percutaneous patent foramen ovale occluder. J Thorac Cardiovasc Surg 125:213–214. doi:10.1067/mtc.2003.125
Giménez-Arnau A, Riambau V, Serra-Baldrich E, Camarasa JG (2000) Metal-induced generalized pruriginous dermatitis and endovascular surgery. Contact Dermatitis 43:35–40
Lai DW, Saver JL, Araujo JA et al (2005) Pericarditis associated with nickel hypersensitivity to the Amplatzer occluder device: a case report. Catheter Cardiovasc Interv Off J Soc Card Angiogr Interv 66:424–426. doi:10.1002/ccd.20497
Jeswani S, Alexander MJ (2011) Nickel allergy: a reason for concern? J Neurointerventional Surg 3:2–4. doi:10.1136/jnis.2010.003657
Pratt MD, Belsito DV, DeLeo VA et al (2004) North American Contact Dermatitis Group patch-test results, 2001-2002 study period. Dermat Contact Atopic Occup Drug 15:176–183
Shannon P, Billbao JM, Marotta T, Terbrugge K (2006) Inadvertent foreign body embolization in diagnostic and therapeutic cerebral angiography. AJNR Am J Neuroradiol 27:278–282
Barnwell SL, D’Agostino AN, Shapiro SL et al (1997) Foreign bodies in small arteries after use of an infusion microcatheter. AJNR Am J Neuroradiol 18:1886–1889
Mehta RI, Mehta RI, Fishbein MC et al (2009) Intravascular polymer material after coil embolization of a giant cerebral aneurysm. Hum Pathol 40:1803–1807. doi:10.1016/j.humpath.2009.04.027
Mehta RI, Mehta RI, Solis OE et al (2010) Hydrophilic polymer emboli: an under-recognized iatrogenic cause of ischemia and infarct. Mod Pathol Off J U S Can Acad Pathol Inc 23:921–930. doi:10.1038/modpathol.2010.74
Hu YC, Deshmukh VR, Albuquerque FC et al (2014) Histopathological assessment of fatal ipsilateral intraparenchymal hemorrhages after the treatment of supraclinoid aneurysms with the Pipeline Embolization Device. J Neurosurg 120:365–374. doi:10.3171/2013.11.JNS131599
Gilchrist IC, Kozak M (2010) Hydrophilic-coated radial sheaths: a leap forward, but watch where you land. JACC Cardiovasc Interv 3:484–485. doi:10.1016/j.jcin.2010.03.008
Kozak M, Adams DR, Ioffreda MD et al (2003) Sterile inflammation associated with transradial catheterization and hydrophilic sheaths. Catheter Cardiovasc Interv Off J Soc Card Angiogr Interv 59:207–213. doi:10.1002/ccd.10522
Lim J, Suri A, Chua TP (2009) Steroid-responsive sterile inflammation after transradial cardiac catheterisation using a sheath with hydrophilic coating. Heart Br Card Soc 95:1202. doi:10.1136/hrt.2008.165068
Sado D, Witherow F (2009) Sterile granuloma formation following radial artery facilitated coronary catheterization. Catheter Cardiovasc Interv Off J Soc Card Angiogr Interv 74:606. doi:10.1002/ccd.22048
Subramanian R, White CJ, Sternbergh WC et al (2003) Nonhealing wound resulting from a foreign-body reaction to a radial arterial sheath. Catheter Cardiovasc Interv Off J Soc Card Angiogr Interv 59:205–206. doi:10.1002/ccd.10468
Swaminathan RV, Wong SC (2011) Radial access site inflammatory reaction to a recently available hydrophilic coated sheath. Catheter Cardiovasc Interv Off J Soc Card Angiogr Interv 77:1050–1053. doi:10.1002/ccd.22896
Ziakas A, Karkavelas G, Mochlas S (2005) Sterile inflammation after transradial catheterization using a hydrophilic sheath: a case report. Int J Cardiol 99:495–496. doi:10.1016/j.ijcard.2004.01.047
El-Najjar V, Robinson M (2012) Autopsy demonstration of intramyocardial polymer gel emboli associated with a giant-cell reaction following cardiac catheterization: a case report. Cardiovasc Pathol Off J Soc Cardiovasc Pathol 21:59–61. doi:10.1016/j.carpath.2011.05.005
Rosen LE, Singh RI, Mahon B (2014) Myocardial hydrophilic polymer emboli following cardiac catheterization: a case report and literature review. Cardiovasc Pathol Off J Soc Cardiovasc Pathol 23:175–177. doi:10.1016/j.carpath.2014.01.009
Sequeira A, Parimoo N, Wilson J et al (2013) Polymer embolization from minimally invasive interventions. Am J Kidney Dis Off J Natl Kidney Found 61:984–987. doi:10.1053/j.ajkd.2012.12.021
Allan RW, Alnuaimat H, Edwards WD, Tazelaar HD (2009) Embolization of hydrophilic catheter coating to the lungs: report of a case mimicking granulomatous vasculitis. Am J Clin Pathol 132:794–797. doi:10.1309/AJCPH2PGCCPA0ZJF
Tomas C, Benaissa A, Herbreteau D et al (2014) Delayed ipsilateral parenchymal hemorrhage following treatment of intracranial aneurysms with flow diverter. Neuroradiology 56:155–161. doi:10.1007/s00234-013-1302-2
Rouchaud A, Brinjikji W, Lanzino G et al (2016) Delayed hemorrhagic complications after flow diversion for intracranial aneurysms: a literature overview. Neuroradiology 58:171–177. doi:10.1007/s00234-015-1615-4
Mitha AP, Mynard JP, Storwick JA et al (2015) Can the Windkessel hypothesis explain delayed intraparenchymal haemorrhage after flow diversion? A case report and model-based analysis of possible mechanisms. Heart Lung Circ 24:824–830. doi:10.1016/j.hlc.2015.02.001
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
We declare that our institution does not require ethics committee approval or patient consent for retrospective analyses of patients’ records and imaging data. We declare that the two patients gave informed consent for skin patch tests.
Conflict of interest
We declare that we have no conflict of interest. All tested endovascular devices were provided by the manufacturers free of charge.
Additional information
FDM, NS, and FC contributed equally to this study.
Rights and permissions
About this article
Cite this article
Shotar, E., Law-Ye, B., Baronnet-Chauvet, F. et al. Non-ischemic cerebral enhancing lesions secondary to endovascular aneurysm therapy: nickel allergy or foreign body reaction? Case series and review of the literature. Neuroradiology 58, 877–885 (2016). https://doi.org/10.1007/s00234-016-1699-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-016-1699-5