Abstract
Purpose
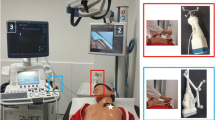
Freehand SPECT is a 3-D tomographic imaging modality based on data acquisition with a hand-held detector that is moved freely, in contrast to conventional, fixed gamma camera systems. In this pilot study, the feasibility of freehand SPECT for 3-D lymphatic mapping in breast cancer was evaluated.
Methods
A total of 85 patients (age: 29–88 years) with an initial diagnosis of invasive breast cancer and no clinical evidence of nodal involvement prospectively underwent sentinel lymph node (SLN) biopsy. Preoperative lymphatic mapping (35–87 MBq 99mTc-Nanocoll) included tomographic imaging with a SPECT/CT device (Siemens Symbia T6) serving as reference. Initially, the freehand SPECT approach was assessed in a pilot study consisting of 50 patients. The quality of each freehand SPECT acquisition was assessed and ranked as good, intermediate or poor. In another series comprising a further 35 patients (validation study), a guidance system for the acquisition was implemented based on the results of the pilot study, ensuring acquisitions with good quality. For 3-D tomographic image reconstruction, ad hoc models and iterative reconstruction algorithms were used in all 85 patients. To allow for adequate comparison, SPECT/CT data and freehand SPECT data were registered within the same coordinate system.
Results
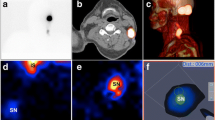
In the pilot study, freehand SPECT enabled mapping of 24 of 83 SLNs in 20 of 44 patients (3 dropouts, 3 patients without SLN either in SPECT/CT or in freehand SPECT). Using SPECT/CT as reference, the accuracy of freehand SPECT was 77.8% (7/9 nodes) in scans with good quality, while for intermediate and poor quality scans, the accuracy was reduced to 34.3 and 12.8%, respectively. In the validation study, quality feedback improved the results significantly and freehand SPECT enabled the mapping of at least one SLN in 87.5% of the patients (28/32 − 3 dropouts). Compared to the reference method, freehand SPECT showed a sensitivity of 83.3% (35/42 nodes). False-negative findings were related to insufficient scanning time, insufficient coverage of the axillary region, close proximity of the SLN to the injection site and low tracer uptake in the SLNs.
Conclusion
In this preliminary study, we could demonstrate that 3-D localization of SLNs is feasible using freehand SPECT technology. Prerequisites for acquisition of a good scan quality, most likely allowing precise SLN mapping, have been defined. This approach has high potential to allow image-guided biopsy and further standardization of SLN dissection, thus bringing 3-D nuclear imaging into the operating room.





Similar content being viewed by others
References
Lyman GH, Giuliano AE, Somerfield MR, Benson AB, Bodurka DC, Burstein HJ, et al. American Society of Clinical Oncology guideline recommendations for sentinel lymph node biopsy in early-stage breast cancer. J Clin Oncol 2005;23:7703–20.
Cserni G, Amendoeira I, Apostolikas N, Bellocq JP, Bianchi S, Bussolati G, et al. Pathological work-up of sentinel lymph nodes in breast cancer. Review of current data to be considered for the formulation of guidelines. Eur J Cancer 2003;39:1654–67.
Kim T, Giuliano AE, Lyman GH. Lymphatic mapping and sentinel lymph node biopsy in early-stage breast carcinoma: a metaanalysis. Cancer 2006;106:4–16.
Husarik DB, Steinert HC. Single-photon emission computed tomography/computed tomography for sentinel node mapping in breast cancer. Semin Nucl Med 2007;37:29–33.
Lerman H, Metser U, Lievshitz G, Sperber F, Shneebaum S, Even-Sapir E. Lymphoscintigraphic sentinel node identification in patients with breast cancer: the role of SPECT-CT. Eur J Nucl Med Mol Imaging 2006;33:329–37.
van der Ploeg IM, Valdés Olmos RA, Nieweg OE, Rutgers EJ, Kroon BB, Hoefnagel CA. The additional value of SPECT/CT in lymphatic mapping in breast cancer and melanoma. J Nucl Med 2007;48:1756–60.
Lerman H, Lievshitz G, Zak O, Metser U, Schneebaum S, Even-Sapir E. Improved sentinel node identification by SPECT/CT in overweight patients with breast cancer. J Nucl Med 2007;48:201–6.
Abe A, Takahashi N, Lee J, Oka T, Shizukuishi K, Kikuchi T, et al. Performance evaluation of a hand-held, semiconductor (CdZnTe)-based gamma camera. Eur J Nucl Med Mol Imaging 2003;30:805–11.
Barranger E, Kerrou K, Pitre S, Duval MA, Charon Y, Uzan S. Place of a hand-held gamma camera (POCI) in the breast cancer sentinel node biopsy. Breast 2007;16:443–4.
Mathelin C, Salvador S, Huss D, Guyonnet JL. Precise localization of sentinel lymph nodes and estimation of their depth using a prototype intraoperative mini gamma-camera in patients with breast cancer. J Nucl Med 2007;48:623–9.
Sánchez F, Benlloch JM, Escat B, Pavón N, Porras E, Kadi-Hanifi D, et al. Design and tests of a portable mini gamma camera. Med Phys 2004;31:1384–97.
Schillaci O, D’Errico G, Scafè R, Soluri A, Burgio N, Santagata A, et al. Sentinel node detection with imaging probe. Tumori 2002;88:S32–5.
Wendler T, Hartl A, Lasser T, Traub J, Daghighian F, Ziegler SI, et al. Towards intra-operative 3D nuclear imaging: reconstruction of 3D radioactive distributions using tracked gamma probes. Med Image Comput Comput Assist Interv 2007;10(Pt 2):909–17.
Kühn T, Bembenek A, Decker T, Munz DL, Sautter-Bihl ML, Untch M, et al. A concept for the clinical implementation of sentinel lymph node biopsy in patients with breast carcinoma with special regard to quality assurance. Cancer 2005;103:451–61.
Schirrmeister H, Kotzerke J, Vogl F, Buck A, Czech N, Koretz K, et al. Prospective evaluation of factors influencing success rates of sentinel node biopsy in 814 breast cancer patients. Cancer Biother Radiopharm 2004;19:784–90.
van Esser S, Hobbelink M, Van Isselt JW, Mali WP, Borel Rinkes IH, van Hillegersberg R. Comparison of a 1-day and a 2-day protocol for lymphatic mapping and sentinel lymph node biopsy in patients with nonpalpable breast cancer. Eur J Nucl Med Mol Imaging 2009;36:1383–7.
Wendler T, Hartl A, Lasser T, Traub J, Ziegler SI, Navab N. Tracking-based statistical correction for radio-guided cancer surgery. World Molecular Imaging Congress, Nice, France; 2008.
Vermeeren L, Valdés Olmos RA, Meinhardt W, Bex A, van der Poel HG, Vogel WV, et al. Intraoperative radioguidance with a portable gamma camera: a novel technique for laparoscopic sentinel node localisation in urological malignancies. Eur J Nucl Med Mol Imaging 2009;36:1029–36.
De Jong M, Valkema R, Jamar F, Kvols LK, Kwekkeboom DJ, Breeman WA, et al. Somatostatin receptor-targeted radionuclide therapy of tumors: preclinical and clinical findings. Semin Nucl Med 2002;32:133–40.
Kwekkeboom DJ, Krenning EP. Somatostatin receptor imaging. Semin Nucl Med 2002;32:84–91.
Nadeem R, Chagla LS, Harris O, Desmond S, Thind R, Flavin A, et al. Tumour localisation with a metal coil before the administration of neo-adjuvant chemotherapy. Breast 2005;14:403–7.
Acknowledgement
This research was partially funded by the SFB 824 of the Deutsche Forschungsgesellschaft (DFG), the Graduate School of Information Science in Health (GSISH) and the TUM Graduate School (TUM-GS).
Author information
Authors and Affiliations
Corresponding author
Additional information
Thomas Wendler and Ken Herrmann contributed equally to the manuscript.
Rights and permissions
About this article
Cite this article
Wendler, T., Herrmann, K., Schnelzer, A. et al. First demonstration of 3-D lymphatic mapping in breast cancer using freehand SPECT. Eur J Nucl Med Mol Imaging 37, 1452–1461 (2010). https://doi.org/10.1007/s00259-010-1430-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-010-1430-4