Abstract
Objectives
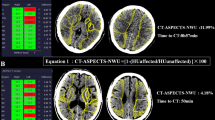
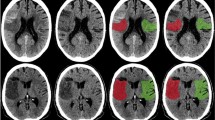
Net water uptake (NWU) has been shown to have a linear relationship with brain edema. Based on an automated-Alberta Stroke Program Early Computed Tomography Score (ASPECTS) technique, we automatically derived NWU from baseline multimodal computed tomography (CT), namely ASPECTS-NWU. We aimed to determine if ASPECTS-NWU can predict the development of malignant cerebral edema (MCE).
Methods
One hundred and forty-six patients with large-vessel occlusion were retrospectively enrolled. Quantitative NWU based on automated-ASPECTS was measured both on nonenhanced CT (NECT) and CT angiography (CTA), namely NECT-ASPECT-NWU and CTA-ASPECTS-NWU. The correlation between ASPECTS-NWU and cerebral edema (CED) grades was calculated using Spearman rank correlation. Univariate logistic regression was used to assess the effect of radiological and clinical features on MCE, and a multivariable model with significant factors from the univariate regression analysis was built. Receiver operating characteristic (ROC) was obtained and area under curve (AUC) was compared.
Results
CTA-ASPECTS-NWU had a moderate positive correlation with CED grades (r = 0.62; 95% confidence interval [CI], 0.51–0.71; p < 0.001). The CTA-ASPECTS-NWU performed better than the NECT-ASPECTS-NWU with AUC: 0.88 vs. 0.71 (p < 0.001). Multivariable logistic regression model integrating CTA-ASPECTS-NWU, collateral score, and age showed the CTA-ASPECTS-NWU was an independent predictor of MCE with an AUC of 0.94 (95% CI: 0.90–0.98; p < 0.001).
Conclusions
This study demonstrates that ASPECTS-NWU is a quantitative predictor of MCE after large-vessel occlusion of the middle cerebral artery territory. The multivariable logistic regression model may enhance the identification of patients with MCE needing anti-edematous treatment.
Key Points
• The automated-ASPECTS technique can automatically detect the affected regions with early ischemic changes and NWU could be manually calculated.
• The CTA-ASPECTS-NWU performs better than the NECT-ASPECTS-NWU on predicting the development of MCE.
• The multivariable logistic regression model may enhance the identification of patients with MCE needing anti-edematous treatment.





Similar content being viewed by others
Abbreviations
- AIS:
-
Acute ischemic stroke
- ASPECTS:
-
Alberta Stroke Program Early CT Score
- ASPECTS-NWU:
-
ASPECTS-Net water uptake
- BBB:
-
Blood-brain barrier
- CED:
-
Cerebral edema
- CS:
-
Collateral score
- CTA-SI:
-
CT angiography source images
- CTP:
-
CT perfusion
- IQR:
-
Interquartile range
- LVO:
-
Large-vessel occlusion
- MCA:
-
Middle cerebral artery
- MCE:
-
Malignant cerebral edema
- MLS:
-
Midline shift
- mRS:
-
Modified RanKin scale
- mTICI:
-
Modified thrombolysis in cerebral infarction
- NECT:
-
Nonenhanced CT
- NIHSS:
-
National Institutes of Health Stroke Scale scores
- NWU:
-
Net water uptake
References
Hacke W, Schwab S, Horn M, Spranger M, De Georgia M, von Kummer R (1996) ‘Malignant’ middle cerebral artery territory infarction: clinical course and prognostic signs. Arch Neurol 53:309–315
Thanvi S, Treadwell S, Robinson T (2008) Early neurological deterioration in acute ischaemic stroke: predictors, mechanisms and management. Postgrad Med J 84:412–417
Huttner HB, Schwab S (2009) Malignant middle cerebral artery infarction: clinical characteristics, treatment strategies, and future perspectives. Lancet Neurol 8:949–958
Jha SK (2003) Cerebral edema and its management. Med J Armed Forces India 59:326–331
Vorasayan P, Bevers MB, Beslow LA et al (2019) Intravenous glibenclamide reduces lesional water uptake in large hemispheric infarction. Stroke 50:3021–3027
Nawabi J, Flottmann F, Kemmling A et al (2019) Elevated early lesion water uptake in acute stroke predicts poor outcome despite successful recanalization - when “tissue clock” and “time clock” are desynchronized. Int J Stroke. https://doi.org/10.1177/1747493019884522
Wardlaw JM, Mielke O (2005) Early signs of brain infarction at CT: observer reliability and outcome after thrombolytic treatment–systematic review. Radiology 235:444–453
Kobkitsuksakul C, Tritanon O, Suraratdecha V (2018) Interobserver agreement between senior radiology resident, neuroradiology fellow, and experienced neuroradiologist in the rating of Alberta Stroke Program Early Computed Tomography Score (ASPECTS). Diagn Interv Radiol 24:104–107
Barber PA, Demchuk AM, Zhang J, Buchan AM (2000) Validity and reliability of a quantitative computed tomography score in predicting outcome of hyperacute stroke before thrombolytic therapy. ASPECTS Study Group. Alberta Stroke Programme Early CT Score [published correction appears in Lancet 2000;355:2170]. Lancet 355:1670–1674
Puetz V, Dzialowski I, Hill MD, Demchuk AM (2009) The Alberta Stroke Program Early CT Score in clinical practice: what have we learned? Int J Stroke 4:354–364
Maegerlein C, Fischer J, Mönch S et al (2019) Automated calculation of the Alberta Stroke Program Early CT Score: feasibility and reliability. Radiology 291:141–148
Bal S, Bhatia R, Menon BK et al (2015) Time dependence of reliability of noncontrast computed tomography in comparison to computed tomography angiography source image in acute ischemic stroke. Int J Stroke 10:55–60
Reidler P, Thierfelder KM, Rotkopf LT et al (2019) Attenuation changes in ASPECTS regions: a surrogate for CT perfusion-based ischemic core in acute ischemic stroke. Radiology 291:451–458
Wolff L, Berkhemer OA, van Es ACGM et al (2021) Validation of automated Alberta Stroke Program Early CT Score (ASPECTS) software for detection of early ischemic changes on non-contrast brain CT scans. Neuroradiology 63:491–498
Broocks G, Flottmann F, Scheibel A et al (2018) Quantitative lesion water uptake in acute stroke computed tomography is a predictor of malignant infarction. Stroke 49:1906–1912
Tan IY, Demchuk AM, Hopyan J et al (2009) CT angiography clot burden score and collateral score: correlation with clinical and radiologic outcomes in acute middle cerebral artery infarct. AJNR Am J Neuroradiol 30:525–531
Strbian D, Meretoja A, Putaala J, Kaste M, Tatlisumak T; Helsinki Stroke Thrombolysis Registry Group (2013) Cerebral edema in acute ischemic stroke patients treated with intravenous thrombolysis. Int J Stroke 8:529–534
Schisterman EF, Perkins NJ, Liu A, Bondell H (2005) Optimal cut-point and its corresponding Youden Index to discriminate individuals using pooled blood samples. Epidemiology 16:73–81
DeLong ER, DeLong DM, Clarke-Pearson DL (1988) Comparing the areas under two or more correlated receiver operating characteristic curves: a nonparametric approach. Biometrics 44:837–845
Simard JM, Kent TA, Chen M, Tarasov KV, Gerzanich V (2007) Brain oedema in focal ischaemia: molecular pathophysiology and theoretical implications. Lancet Neurol 6:258–268
Bhatia R, Bal SS, Shobha N et al (2011) CT angiographic source images predict outcome and final infarct volume better than noncontrast CT in proximal vascular occlusions. Stroke 42:1575–1580
Camargo EC, Furie KL, Singhal AB et al (2007) Acute brain infarct: detection and delineation with CT angiographic source images versus nonenhanced CT scans. Radiology 244:541–548
von Kummer R, Dzialowski I (2017) Imaging of cerebral ischemic edema and neuronal death. Neuroradiology 59:545–553
Aviv RI, Shelef I, Malam S et al (2007) Early stroke detection and extent: impact of experience and the role of computed tomography angiography source images. Clin Radiol 62:447–452
Bektas H, Wu TC, Kasam M et al (2010) Increased blood-brain barrier permeability on perfusion CT might predict malignant middle cerebral artery infarction. Stroke 41:2539–2544
Horsch AD, Dankbaar JW, Stemerdink TA et al (2016) Imaging findings associated with space-occupying edema in patients with large middle cerebral artery infarcts. AJNR Am J Neuroradiol 37:831–837
Sharma M, Fox AJ, Symons S, Jairath A, Aviv RI (2011) CT angiographic source images: flow- or volume-weighted? AJNR Am J Neuroradiol 32:359–364
Cheng Y, Wu S, Wang Y et al (2020) External validation and modification of the EDEMA score for predicting malignant brain edema after acute ischemic stroke. Neurocrit Care 32(1):104–112
Foroushani HM, Hamzehloo A, Kumar A et al (2020) Quantitative serial CT imaging-derived features improve prediction of malignant cerebral edema after ischemic stroke. Neurocrit Care 33:785–792
Battey TW, Karki M, Singhal AB et al (2014) Brain edema predicts outcome after nonlacunar ischemic stroke. Stroke 45:3643–3648
Acknowledgements
We thank MengJie Lu for contributing to the statistical analysis.
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is GuangMing Lu.
Conflict of Interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and Biometry
One of the authors has significant statistical expertise.
Informed Consent
Written informed consent was waived.
Ethical Approval
Institutional Review Board approval was not required because of the retrospective nature of the study.
Methodology
• retrospective
• diagnostic or prognostic study
• performed at one institution
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Shi, J., Wu, H., Dong, Z. et al. Automated quantitative lesion water uptake in acute stroke is a predictor of malignant cerebral edema. Eur Radiol 32, 2771–2780 (2022). https://doi.org/10.1007/s00330-021-08443-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-021-08443-2