Abstract
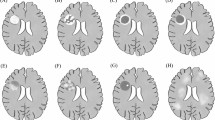
Atypical lesions of a presumably idiopathic inflammatory demyelinating origin present quite variably and may pose diagnostic problems. The subsequent clinical course is also uncertain. We, therefore, wanted to clarify if atypical idiopathic inflammatory demyelinating lesions (AIIDLs) can be classified according to previously suggested radiologic characteristics and how this classification relates to prognosis. Searching the databases of eight tertiary referral centres we identified 90 adult patients (61 women, 29 men; mean age 34 years) with ≥1 AIIDL. We collected their demographic, clinical and magnetic resonance imaging data and obtained follow-up (FU) information on 77 of these patients over a mean duration of 4 years. The AIIDLs presented as a single lesion in 72 (80 %) patients and exhibited an infiltrative (n = 35), megacystic (n = 16), Baló (n = 10) or ring-like (n = 16) lesion appearance in 77 (86 %) patients. Additional multiple sclerosis (MS)-typical lesions existed in 48 (53 %) patients. During FU, a further clinical attack occurred rarely (23–35 % of patients) except for patients with ring-like AIIDLs (62 %). Further attacks were also significantly more often in patients with coexisting MS-typical lesions (41 vs. 10 %, p < 0.005). New AIIDLs developed in six (7 %), and new MS-typical lesions in 29 (42 %) patients. Our findings confirm the previously reported subtypes of AIIDLs. Most types confer a relatively low risk of further clinical attacks, except for ring-like lesions and the combination with MS-typical lesions.

Similar content being viewed by others
References
Polman C, Reingold S, Edan G, Filippi M, Hartung H, Kappos L et al (2005) Diagnostic criteria for multiple sclerosis: 2005 revisions to the “McDonald criteria”. Ann Neurol 58:840–846
Filippi M, Rocca M, Arnold D, Bakshi R, Barkhof F, De Stefano N et al (2006) EFNS guidelines on the use of neuroimaging in the management of multiple sclerosis. Eur J Neurol 13(4):313–325
Rovira Cañellas A, Rovira Gols A, Río Izquierdo J, Tintoré Subirana M, Montalban Gairin X (2007) Idiopathic inflammatory-demyelinating diseases of the central nervous system. Neuroradiology 49(5):393–409
Seewann A, Enzinger C, Filippi M, Barkhof F, Rovira A, Gass A et al (2008) MRI characteristics of atypical idiopathic inflammatory demyelinating lesions of the brain: a review of reported findings. J Neurol 255(1):1–10
Lucchinetti C, Gavrilova R, Metz I, Parisi J, Scheithauer BW, Thomsen K et al (2008) Clinical and radiographic spectrum of pathologically confirmed tumefactive multiple sclerosis. Brain 131(pt 7):1759–1775
Poser C, Brinar V (2004) The nature of multiple sclerosis. Clin Neurol Neurosurg 106(3):159–171
Pichiecchio A, Tavazzi E, Maccabelli G, Precupanu CM, Romani A, Roccatagliata L et al (2009) What insights have new imaging techniques given into aggressive forms of MS—different forms of MS or different from MS? Mult Scler 15(3):285–293
Kurtzke J (1983) Rating neurologic impairment in multiple sclerosis: an expanded disability status scale (EDSS). Neurology 33:1444–1452
Llufriu S, Pujol T, Blanco Y, Hankiewicz K, Squarcia M, Berenguer J et al (2010) T2 hypointense rims and ring-enhancing lesions in MS. Mult Scler 16(11):1317–1325
Montalban X, Tintore M, Swanton J, Barkhof F, Fazekas F, Filippi M et al (2010) MRI criteria for MS in patients with clinically isolated syndromes. Neurology 74(5):427–434
Chaodong W, Zhang KN, Wu XM, Gang H, Xie XF, Qu XH et al (2008) Balo’s disease showing benign clinical course and co-existence with multiple sclerosis-like lesions in Chinese. Mult Scler 14(3):418–424
Altintas A, Petek B, Isik N, Terzi M, Bolukbasi F, Tavsanli M et al (2012) Clinical and radiological characteristics of tumefactive demyelinating lesions: follow-up study. Mult Scler 18(10):1448–1453
Nagappa M, Taly AB, Sinha S, Bharath RD, Mahadevan A, Bindu PS et al. (2012) Tumefactive demyelination: clinical, imaging and follow-up observations in thirty-nine patients. Acta Neurol Scand [Epub ahead of print]
Tenembaum S, Chitnis T, Ness J, Hahn JS (2007) Acute disseminated encephalomyelitis. Neurology 68(16 Suppl 2):S23–S36
Enzinger C, Strasser-Fuchs S, Ropele S, Kapeller P, Kleinert R, Fazekas F (2005) Tumefactive demyelinating lesions: conventional and advanced magnetic resonance imaging. Mult Scler 11(2):135–139
Cha S, Pierce S, Knopp EA, Johnson G, Yang C, Ton A et al (2001) Dynamic contrast-enhanced T2*-weighted MR imaging of tumefactive demyelinating lesions. AJNR Am J Neuroradiol 22(6):1109–1116
Malhotra HS, Jain KK, Agarwal A, Singh MK, Yadav SK, Husain M et al (2009) Characterization of tumefactive demyelinating lesions using MR imaging and in vivo proton MR spectroscopy. Mult Scler 15(2):193–203
Kiriyama T, Kataoka H, Taoka T, Tonomura Y, Terashima M, Morikawa M et al (2011) Characteristic neuroimaging in patients with tumefactive demyelinating lesions exceeding 30 mm. J Neuroimaging 21(2):e69–e77
Saini J, Chatterjee S, Thomas B, Kesavadas C (2011) Conventional and advanced magnetic resonance imaging in tumefactive demyelination. Acta Radiol 52(10):1159–1168
Bolcaen J, Acou M, Mertens K, Hallaert G, Van den Broecke C, Achten E et al. (2012) Structural and metabolic features of two different variants of multiple sclerosis: a PET/MRI study. J Neuroimaging [Epub ahead of print]
Acknowledgments
We want to thank the Steering Committee of MAGNIMS [A. Rovira (co-chair), N. de Stefano (co-chair), F. Barkhof, O. Ciccarelli, C. Enzinger, M. Filippi, J. Frederiksen, L. Kappos, X. Montalban, J. Palace, M. Rocca, T. Yousry, H. Vrenken] for the support of this study.
Conflicts of interest
The authors have no conflicts of interest to declare.
Ethical standard
The study has been performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Author information
Authors and Affiliations
Corresponding author
Additional information
On behalf of the MAGNIMS group.
Rights and permissions
About this article
Cite this article
Wallner-Blazek, M., Rovira, A., Fillipp, M. et al. Atypical idiopathic inflammatory demyelinating lesions: prognostic implications and relation to multiple sclerosis. J Neurol 260, 2016–2022 (2013). https://doi.org/10.1007/s00415-013-6918-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00415-013-6918-y