Abstract
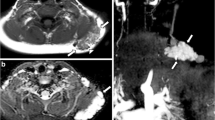
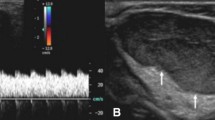
Accurate classification of soft tissue vascular anomalies is critical since treatment options and morbidity differ significantly for the various groups of vascular anomalies (VA). A classification system introduced by Mulliken and Glowacki in 1982 explained the biology of VA, thus resulting in improved management and communication between different disciplines taking care of children with soft tissue vascular anomalies. This classification has been updated by the International Society for the Study of Vascular Anomalies in 1996 and forms the basis for the current nomenclature. Although the majority of vascular anomalies can be accurately classified by their clinical history and a physical exam, imaging is necessary to determine the full anatomical extent of the anomaly, to follow up treatment response, to confirm diagnosis, and to provide correct classification in challenging cases when necessary. This article will review the key magnetic resonance imaging (MRI) features of most common soft tissue vascular anomalies in children. MRI and dynamic contrast-enhanced magnetic resonance angiography are crucial for the evaluation of vascular anomalies in children because of lack of radiation, high soft tissue resolution, and the capability of dynamic contrast-enhanced images to reflect the hemodynamics of the anomalies.









Similar content being viewed by others
References
Adams DM (2001) The nonsurgical management of vascular lesions. Facial Plast Surg Clin North Am 9:601–608
Amir J, Metzker A, Krikler R, Reisner SH (1986) Strawberry hemangioma in preterm infants. Pediatr Dermatol 3:331–332
Babilas P, Shafirstein G, Baumler W, Baier J, Landthaler M, Szeimies RM, Abels C (2005) Selective photothermolysis of blood vessels following flashlamp-pumped pulsed dye laser irradiation: in vivo results and mathematical modelling are in agreement. J Invest Dermatol 125:343–352
Bayrak-Toydemir P, McDonald J, Akarsu N, Toydemir RM, Calderon F, Tuncali T, Tang W, Miller F, Mao R (2006) A fourth locus for hereditary hemorrhagic telangiectasia maps to chromosome 7. Am J Med Genet A 140:2155–2162
Bruder E, Perez-Atayde AR, Jundt G, Alomari AI, Rischewski J, Fishman SJ, Mulliken JB, Kozakewich HP (2009) Vascular lesions of bone in children, adolescents, and young adults. A clinicopathologic reappraisal and application of the ISSVA classification. Virchows Arch 454:161–179
Choi DJ, Alomari AI, Chaudry G, Orbach DB (2009) Neurointerventional management of low-flow vascular malformations of the head and neck. Neuroimaging Clin N Am 19:199–218
Christison-Lagay ER, Fishman SJ (2006) Vascular anomalies. Surg Clin North Am 86:393–425, x
Claudon M, Upton J, Burrows PE (2001) Diffuse venous malformations of the upper limb: morphologic characterization by MRI and venography. Pediatr Radiol 31:507–514
Cole SG, Begbie ME, Wallace GM, Shovlin CL (2005) A new locus for hereditary haemorrhagic telangiectasia (HHT3) maps to chromosome 5. J Med Genet 42:577–582
Dobson MJ, Hartley RW, Ashleigh R, Watson Y, Hawnaur JM (1997) MR angiography and MR imaging of symptomatic vascular malformations. Clin Radiol 52:595–602
Donnelly LF, Adams DM, Bisset GS 3rd (2000) Vascular malformations and hemangiomas: a practical approach in a multidisciplinary clinic. AJR Am J Roentgenol 174:597–608
Dubois J, Alison M (2010) Vascular anomalies: what a radiologist needs to know. Pediatr Radiol 40:895–905
Duffy K (2010) Genetics and syndromes associated with vascular malformations. Pediatr Clin North Am 57:1111–1120
Eerola I, Boon LM, Mulliken JB, Burrows PE, Dompmartin A, Watanabe S, Vanwijck R, Vikkula M (2003) Capillary malformation–arteriovenous malformation, a new clinical and genetic disorder caused by RASA1 mutations. Am J Hum Genet 73:1240–1249
Eifert S, Villavicencio JL, Kao TC, Taute BM, Rich NM (2000) Prevalence of deep venous anomalies in congenital vascular malformations of venous predominance. J Vasc Surg 31:462–471
Enjolras O, Wassef M, Mazoyer E, Frieden IJ, Rieu PN, Drouet L, Taieb A, Stalder JF, Escande JP (1997) Infants with Kasabach–Merritt syndrome do not have “true” hemangiomas. J Pediatr 130:631–640
Fayad LM, Hazirolan T, Bluemke D, Mitchell S (2006) Vascular malformations in the extremities: emphasis on MR imaging features that guide treatment options. Skeletal Radiol 35:127–137
Fayad LM, Hazirolan T, Carrino JA, Bluemke DA, Mitchell S (2008) Venous malformations: MR imaging features that predict skin burns after percutaneous alcohol embolization procedures. Skeletal Radiol 37:895–901
Gorincour G, Kokta V, Rypens F, Garel L, Powell J, Dubois J (2005) Imaging characteristics of two subtypes of congenital hemangiomas: rapidly involuting congenital hemangiomas and non-involuting congenital hemangiomas. Pediatr Radiol 35:1178–1185
Hein KD, Mulliken JB, Kozakewich HP, Upton J, Burrows PE (2002) Venous malformations of skeletal muscle. Plast Reconstr Surg 110:1625–1635
Hochman M, Adams DM, Reeves TD (2011) Current knowledge and management of vascular anomalies: I. Hemangiomas. Arch Facial Plast Surg 13:145–151
Hochman M, Adams DM, Reeves TD (2011) Current knowledge and management of vascular anomalies: II. Malformations. Arch Facial Plast Surg 13:425–433
Konez O, Burrows PE (2002) Magnetic resonance of vascular anomalies. Magn Reson Imaging Clin N Am 10:363–388, vii
Laor T, Burrows PE, Hoffer FA (1996) Magnetic resonance venography of congenital vascular malformations of the extremities. Pediatr Radiol 26:371–380
Legiehn GM, Heran MK (2008) Venous malformations: classification, development, diagnosis, and interventional radiologic management. Radiol Clin North Am 46:545–597, vi
Limaye N, Wouters V, Uebelhoer M, Tuominen M, Wirkkala R, Mulliken JB, Eklund L, Boon LM, Vikkula M (2009) Somatic mutations in angiopoietin receptor gene TEK cause solitary and multiple sporadic venous malformations. Nat Genet 41:118–124
Moukaddam H, Pollak J, Haims AH (2009) MRI characteristics and classification of peripheral vascular malformations and tumors. Skeletal Radiol 38:535–547
Mulliken JB, Glowacki J (1982) Hemangiomas and vascular malformations in infants and children: a classification based on endothelial characteristics. Plast Reconstr Surg 69:412–422
North PE, Waner M, Mizeracki A, Mihm MC Jr (2000) GLUT1: a newly discovered immunohistochemical marker for juvenile hemangiomas. Hum Pathol 31:11–22
North PE, Waner M, Mizeracki A, Mrak RE, Nicholas R, Kincannon J, Suen JY, Mihm MC Jr (2001) A unique microvascular phenotype shared by juvenile hemangiomas and human placenta. Arch Dermatol 137:559–570
Oduber CE, van der Horst CM, Hennekam RC (2008) Klippel–Trenaunay syndrome: diagnostic criteria and hypothesis on etiology. Ann Plast Surg 60:217–223
Orloff MS, Eng C (2008) Genetic and phenotypic heterogeneity in the PTEN hamartoma tumour syndrome. Oncogene 27:5387–5397
Shen W, Cui J, Chen J, Zou J, Ji Y, Chen H (2010) Kasabach–Merritt syndrome with partial resection of tumor, reduction of tumor blood, and vincristine chemotherapy. J Craniofac Surg 21:215–216
Sidbury R (2010) Update on vascular tumors of infancy. Curr Opin Pediatr 22:432–437
Siegel MJ (2001) Magnetic resonance imaging of musculoskeletal soft tissue masses. Radiol Clin North Am 39:701–720
Wu IC, Orbach DB (2009) Neurointerventional management of high-flow vascular malformations of the head and neck. Neuroimaging Clin N Am 19:219–240
Ziyeh S, Strecker R, Berlis A, Weber J, Klisch J, Mader I (2005) Dynamic 3D MR angiography of intra- and extracranial vascular malformations at 3 T: a technical note. AJNR Am J Neuroradiol 26:630–634
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Thawait, S.K., Puttgen, K., Carrino, J.A. et al. MR imaging characteristics of soft tissue vascular anomalies in children. Eur J Pediatr 172, 591–600 (2013). https://doi.org/10.1007/s00431-012-1828-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00431-012-1828-z