Abstract
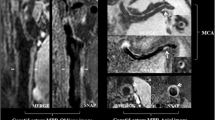
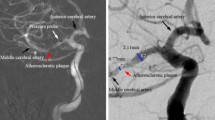
We evaluated associations between cerebral blood flow (CBF) and histopathological features in atherosclerotic lesions of the internal carotid artery. Cerebrovascular reactivity (CVR) and CBF were measured in 72 patients with unilateral carotid artery stenosis who underwent Xe-CT before carotid endarterectomy. Collateral blood flow was estimated as stump pressure. Proportions of fibrous tissue, intraplaque hemorrhage (IPH), and calcification were pathologically compared with the entire plaque body. The Spearman’s rank test and stepwise multiple linear regression analysis revealed that the IPH rate significantly and negatively correlated with CBF, whereas the calcification rate positively correlated with CVR. One-way analysis of variance showed that IPH and the absence of calcification might confer a risk for CBF and CVR reduction. Thus, not only the stenosis rate but also the degree of IPH and calcification in carotid arterial plaque are notable risk factors for ischemic stroke.



Similar content being viewed by others
References
Altaf N, MacSweeney ST, Gladman J, Auer DP (2007) Carotid intraplaque hemorrhage predicts recurrent symptoms in patients with high-grade carotid stenosis. Stroke 38:1633–1635
Charles W (1991) MRC European Carotid Surgery Trial: interim results for symptomatic patients with severe (70–99 %) or with mild (0–29 %) carotid stenosis. Lancet 337:1235–1243
Derdeyn CP, Grubb RL Jr, Powers WJ (1999) Cerebral hemodynamic impairment. methods of measurement and association with stroke risk. Neurology 22(53):251–259
Endo S, Hirashima Y, Kurimoto M, Kuwayama N, Nishijima M, Takaku A (1996) Acute pathologic features with angiographic correlates of the nearly or completely occluded lesions of the cervical internal carotid artery. Surg Neurol 46:222–228
Fuster V, Badimon L, Badimon JJ, Chesebro JH (1992) The pathogenesis of coronary artery disease and the acute coronary syndromes (1). N Engl J Med 326(4):242–250
Hatsukami TS, Ferguson MS, Beach KW, Gordon D, Detmer P, Burns D, Alpers C, Strandness DE Jr (1997) Carotid plaque morphology and clinical events. Stroke 28:95–100
Johnson RC, Leopold JA, Loscalzo J (2006) Vascular calcification: pathobiological mechanisms and clinical implications. Circ Res 99:1044–1059
Kolodgie FD, Gold HK, Burke AP, Fowler DR, Kruth HS, Weber DK, Farb A, Guerrero LJ, Hayase M, Kutys R, Narula J, Finn AV, Virmani R (2003) Intraplaque hemorrhage and progression of coronary atheroma. N Engl J Med 349:2316–2325
Kume S, Hama S, Yamane K, Wada S, Nishida T, Kurisu K (2010) Vulnerable carotid arterial plaque causing repeated ischemic stroke can be detected with B-mode ultrasonography as a mobile component: Jellyfish sign. Neurosurg Rev 33:419–430
Kwee RM (2010) Systematic review on the association between calcification in carotid plaques and clinical ischemic symptoms. J Vasc Surg 51(4):1015–1025
Lammie GA, Sandercock PA, Dennis MS (1999) Recently occluded intracranial and extracranial carotid arteries. Relevance of the unstable atherosclerotic plaque. Stroke 30:1319–1325
Lennihan L, Kupsky WJ, Mohr JP, Hauser WA, Correll JW, Quest DO (1987) Lack of association between carotid plaque hematoma and ischemic cerebral symptoms. Stroke 18:879–881
Lusby RJ, Ferrell LD, Ehrenfeld WK, Stoney RJ, Wylie EJ (1982) Carotid plaque hemorrhage. Arch Surg 117:1479–1488
Markus H, Cullinane M (2001) Severely impaired cerebrovascular reactivity predicts stroke and TIA risk in patients with carotid artery stenosis and occlusion. Brain 124:457–467
Momjian-Mayor I, Baron JC (2005) The pathophysiology of watershed infarction in internal carotid artery disease. Review of cerebral perfusion studies. Stroke 36:567–577
Nandalur KR, Baskurt E, Hagspiel KD, Finch M, Phillips CD, Bollampally SR, Kramer CM (2006) Carotid artery calcification on CT May independently predict stroke risk. AJR Am J Roentgenol 186:547–552
Nandalur KR, Baskurt E, Hagspiel KD, Phillips CD, Kramer CM (2005) Calcified carotid atherosclerotic plaque is associated less with ischemic symptoms than is noncalcified plaque on MDCT. AJR Am J Roentgenol 184:295–298
Nighoghossian N, Derex L, Douek P (2005) The vulnerable carotid artery plaque. Current imaging methods and new perspectives. Stroke 36:2764–2772
North American Symptomatic Carotid Endarterectomy Trial (NASCET) Steering Committee (1991) North American symptomatic carotid endarterectomy trial methods, patient characteristics, and progress. Stroke 22:711–720
Persson AV, Robichaux WT, Silverman M (1983) The natural history of carotid plaque development. Arch Surg 118:1048–1052
Seeger JM, Barratt E, Lawson GA, Klingman N (1995) The relationship between carotid plaque composition, plaque morphology, and neurologic symptoms. J Surg Res 58:330–336
Shaalan WE, Cheng H, Gewertz B, McKinsey JF, Schwartz LB, Katz D, Cao D, Desai T, Glagov S, Bassiouny HS (2004) Degree of carotid plaque calcification in relation to symptomatic outcome and plaque inflammation. J Vasc Surg 40:262–269
Uno M, Hamazaki F, Kohno T, Sebe A, Horiguchi H, Nagahiro S (2001) Combined therapeutic approach of intra-arterial thrombolysis and carotid endarterectomy in selected patients with acute thrombotic carotid occlusion. J Vasc Surg 34:532–540
Virmani R, Kolodgie FD, Burke AP, Finn AV, Gold HK, Tulenko TN, Wrenn SP, Narula J (2005) Atherosclerotic plaque progression and vulnerability to rupture: angiogenesis as a source of intraplaque hemorrhage. Arterioscler Thromb Vasc Biol 25:2054–2061
Yamane K, Shima T, Nishida M, Hatayama T, Yamanaka C (2000) Changes in cerebral blood flow after carotid endarterectomy. Keio J Med 49(Suppl 1):A80–A82
Author information
Authors and Affiliations
Corresponding author
Additional information
Comments
Ben Brown and Anil Nanda, Shreveport, USA
Hashimoto et al. present an interesting study investigating the relationship between histopathologic features of CEA plaques and corresponding CBF and CVR. The implication of this work is that we may be able to refine our indications for CEA based not only on degree of stenosis and symptomatology but by plaque composition as well. Their findings assert higher amounts of IPH correlated with a decrease in CBF. Furthermore, they found the amount of calcification within the plaque was inversely correlated with CVR. These results are a good step in furthering our knowledge of how plaque composition affects a patient’s overall risk for stroke. Currently, the guidelines proposed by multicenter trials, such as NASCET and ECST are the most proven and reliable criteria for patient selection, and more work needs to be done in this area before guidelines can be made based on plaque histopathology.
Dorothea Miller and Ulrich Sure, Essen, Germany
The presented study analyzes the effect of IPH and calcification in carotid arterial plaques on CBF and CVR. The results are interesting and show a trend of a higher risk for ischemic stroke for patients with IPH and absence of intraplaque calcification. Such finding might have an impact on future more aggressive treatment strategies of patients suffering from such plaques. However, before a stratified treatment can be recommended, further prospective studies are needed, since more than half of the patients had to be excluded in the present trial.
Rights and permissions
About this article
Cite this article
Hashimoto, N., Hama, S., Yamane, K. et al. Carotid arterial intraplaque hemorrhage and calcification influences cerebral hemodynamics. Neurosurg Rev 36, 421–427 (2013). https://doi.org/10.1007/s10143-012-0445-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-012-0445-7