Abstract
The risk of ventriculostomy-related hemorrhage among patients requiring antiplatelet therapy (AT) for the endovascular treatment of acutely ruptured intracranial aneurysms needed further investigation. The authors performed a systematic review and meta-analysis of the literature examining the EVD-related hemorrhage rate among patients with and without AT (controls). According to PRISMA guidelines, a comprehensive review of studies published between January 1990 and April 2018 was carried out. The authors identified series with > 5 patients reporting the EVD-associated hemorrhage rate among the AT group and the control group. Variables influencing outcomes were analyzed using a random-effects meta-analysis model. We included 13 studies evaluating 516 (with AT) and 647 (without AT) patients requiring ventriculostomy. EVD-related hemorrhage rates were higher among the AT group (125/516 = 20.9%, 95% CI = 11.9–30%, I2 = 90% vs 57/647 = 9%, 95% CI = 5.5–12.5%, I2 = 45.8%) (p < 0.0001). Major EVD-associated hemorrhage rates were low in both the AT and control group (25/480 = 4.4%, 95% CI = 1.7–7.7%, I2 = 53.9% vs 6/647 = 0.7%, 95% CI = 0.03–1.7%, I2 = 0%) (p < 0.0001). Ventriculostomy before embolization and intraprocedural AT were associated with lower rates of EVD-related bleeding (32/230 = 9.6%, 95% CI = 2.1–17.1%, I2 = 75.4% vs 6/24 = 25.1%, 95% CI = 8.8–41%, I2 = 0%) (p < 0.02). The rate of major hemorrhage was higher after dual AT (CP + ASA) compared to single AT (ASA or CP) used as an intraprocedural loading dose (13/173 = 7%, 95% CI = 3.3–10.7%, I2 = 0% vs 6/210 = 1.7%, 95% CI = 0.1–3.4%, I2 = 0%) (p < 0.009). AT during endovascular treatment of acutely ruptured intracranial aneurysms increases the risk of EVD-related hemorrhages, although most of them are small and asymptomatic. When ventriculostomy is performed before endovascular procedures requiring antiplatelet administration, the hemorrhagic risk is minimized. A single antiplatelet therapy is associated with a lower rate of major bleeding than a dual therapy.

Similar content being viewed by others
References
Amenta PS, Dalyai RT, Kung D, Toporowski A, Chandela S, Hasan D, Gonzalez LF, Dumont AS, Tjoumakaris SI, Rosenwasser RH, Maltenfort MG, Jabbour PM (2012) Stent-assisted coiling of wide-necked aneurysms in the setting of acute subarachnoid hemorrhage: experience in 65 patients. Neurosurgery 70:1415–1429 discussion 1429
Bodily KD, Cloft HJ, Lanzino G, Fiorella DJ, White PM, Kallmes DF (2011) Stent-assisted coiling in acutely ruptured intracranial aneurysms: a qualitative, systematic review of the literature. AJNR Am J Neuroradiol 32:1232–1236
Bruder M, Schuss P, Konczalla J, El-Fiki A, Lescher S, Vatter H, Seifert V, Guresir E (2015) Ventriculostomy-related hemorrhage after treatment of acutely ruptured aneurysms: the influence of anticoagulation and antiplatelet treatment. World Neurosurg 84:1653–1659
Cagnazzo F, Gambacciani C, Morganti R, Perrini P (2017) Aneurysm rebleeding after placement of external ventricular drainage: a systematic review and meta-analysis. Acta Neurochir 159:695–704
Chalouhi N, Zanaty M, Whiting A, Tjoumakaris S, Hasan D, Ajiboye N, Hann S, Rosenwasser RH, Jabbour P (2015) Treatment of ruptured intracranial aneurysms with the pipeline embolization device. Neurosurgery 76:165–172 discussion 172
Chung J, Lim YC, Suh SH, Shim YS, Kim YB, Joo JY, Kim BS, Shin YS (2014) Stent-assisted coil embolization of ruptured wide-necked aneurysms in the acute period: incidence of and risk factors for periprocedural complications. J Neurosurg 121:4–11
Edwards NJ, Jones WH, Sanzgiri A, Corona J, Dannenbaum M, Chen PR (2017) Antiplatelet therapy for the prevention of peri-coiling thromboembolism in high-risk patients with ruptured intracranial aneurysms. J Neurosurg 127:1326–1332
Fifi JT, Brockington C, Narang J, Leesch W, Ewing SL, Bennet H, Berenstein A, Chong J (2013) Clopidogrel resistance is associated with thromboembolic complications in patients undergoing neurovascular stenting. AJNR Am J Neuroradiol 34:716–720
Jankowitz B, Thomas AJ, Vora N, Gupta R, Levy E, Yamamoto J, Kassam A, Gologorsky Y, Panapitiya N, Sandhu E, Crago E, Hricik A, Lee K, Gallek M, Jovin T, Horowitz M (2008) Risk of hemorrhage in combined neuroform stenting and coil embolization of acutely ruptured intracranial aneurysms. Interv Neuroradiol 14:385–396
Hudson JS, Yasunori Nagahama BSP, Nakagawa D, Guerrero WR, Zanaty M, Chalouhi N, Jabbour P, Dandapat S, Allan L, Ortega-Gutierrez S, Samaniego EA, Hasan D (2018) External ventricular drain and hemorrhage in aneurysmal subarachnoid hemorrhage patients on dual antiplatelet therapy: a retrospective cohort study. Neurosurgery 0:1–6
Kim DJ, Suh SH, Kim BM, Kim DI, Huh SK, Lee JW (2010) Hemorrhagic complications related to the stent-remodeled coil embolization of intracranial aneurysms. Neurosurgery 67:73–78 discussion 78-79
Leschke JM, Lozen A, Kaushal M, Oni-Orisan A, Noufal M, Zaidat O, Pollock GA, Mueller WM (2017) Hemorrhagic complications associated with ventriculostomy in patients undergoing endovascular treatment for intracranial aneurysms: a single-center experience. Neurocrit Care 27:11–16
Lin N, Brouillard AM, Keigher KM, Lopes DK, Binning MJ, Liebman KM, Veznedaroglu E, Magarik JA, Mocco J, Duckworth EA, Arthur AS, Ringer AJ, Snyder KV, Levy EI, Siddiqui AH (2015) Utilization of pipeline embolization device for treatment of ruptured intracranial aneurysms: US multicenter experience. J Neurointerv Surg 7:808–815
Lozupone E, Piano M, Valvassori L, Quilici L, Pero G, Visconti E, Boccardi E (2017) Flow diverter devices in ruptured intracranial aneurysms: a single-center experience. J Neurosurg 1–7
Madaelil TP, Moran CJ, Cross DT 3rd, Kansagra AP (2017) Flow diversion in ruptured intracranial aneurysms: a meta-analysis. AJNR Am J Neuroradiol 38:590–595
Maus V, Mpotsaris A, Dorn F, Mohlenbruch M, Borggrefe J, Stavrinou P, Abdullayev N, Barnikol UB, Liebig T, Kabbasch C (2018) The use of flow diverter in ruptured, dissecting intracranial aneurysms of the posterior circulation. World Neurosurg 111:e424–e433
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2010) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Int J Surg 8:336–341
Pandey AS, Koebbe C, Rosenwasser RH, Veznedaroglu E (2007) Endovascular coil embolization of ruptured and unruptured posterior circulation aneurysms: review of a 10-year experience. Neurosurgery 60:626–636 discussion 636-627
Pierot L, Cognard C, Anxionnat R, Ricolfi F, Investigators C (2010) Ruptured intracranial aneurysms: factors affecting the rate and outcome of endovascular treatment complications in a series of 782 patients (CLARITY study). Radiology 256:916–923
Ryu CW, Park S, Shin HS, Koh JS (2015) Complications in stent-assisted endovascular therapy of ruptured intracranial aneurysms and relevance to antiplatelet administration: a systematic review. AJNR Am J Neuroradiol 36:1682–1688
Scheller C, Strauss C, Prell J, Simmermacher S, Brandt S (2018) Increased rate of ventriculostomy-related hemorrhage following endovascular treatment of ruptured aneurysms compared to clipping. Acta Neurochir 160:545–550
Taylor RA, Callison RC, Martin CO, Hayakawa M, Chaloupka JC (2010) Acutely ruptured intracranial saccular aneurysms treated with stent assisted coiling: complications and outcomes in 42 consecutive patients. J Neurointerv Surg 2:23–30
Tumialan LM, Zhang YJ, Cawley CM, Dion JE, Tong FC, Barrow DL (2008) Intracranial hemorrhage associated with stent-assisted coil embolization of cerebral aneurysms: a cautionary report. J Neurosurg 108:1122–1129
van Gijn J, Hijdra A, Wijdicks EF, Vermeulen M, van Crevel H (1985) Acute hydrocephalus after aneurysmal subarachnoid hemorrhage. J Neurosurg 63:355–362
Wells GSB, O’Connell D (2011) The Newcastle-Ottawa Scale (NOS) for assessing the quality of nonradomized studies in meta-analyses. Ottawa Hosp Res Inst 1–4. https://doi.org/10.2307/632432
Acknowledgements
We thank Professor Beth De Felici for the English revision.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This work was performed ethically and complies with the ethical standards of our Institutional Review Board.
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
The nature of this article did not require informed consent.
Electronic supplementary material
Supplemental Figure 1
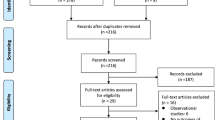
PRISMA diagram detailing the specifics of the systematic literature review and meta-analysis (PNG 381 kb)
Supplemental Figure 2
(A, B, C). Forest plot demonstrating the overall rate of EVD-related hemorrhage among patients with AT (Fig. A). Meta-regression showed a non-significant variation of the effect size during the analyzed period among the AT group (Fig. B). The funnel plot followed by Egger’s linear regression test excludes publication bias among the AT group (Fig. C). (PNG 197 kb)
Supplemental Figure 3
(A, B, C). Forest plot demonstrating the overall rate of EVD-related hemorrhage among patients without AT (control group) (Fig. A). Meta-regression showed a non-significant variation of the effect size during the analyzed period among the control group (Fig. B). The funnel plot followed by Egger’s linear regression test excludes publication bias among the control group (Fig. C). (PNG 84 kb)
ESM 1
(DOC 66 kb)
Supplemental Table 1
(DOCX 11 kb)
Supplemental Table 2
(DOCX 15 kb)
Rights and permissions
About this article
Cite this article
Cagnazzo, F., Di Carlo, D.T., Petrella, G. et al. Ventriculostomy-related hemorrhage in patients on antiplatelet therapy for endovascular treatment of acutely ruptured intracranial aneurysms. A meta-analysis. Neurosurg Rev 43, 397–406 (2020). https://doi.org/10.1007/s10143-018-0999-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-018-0999-0