Abstract
Objective
To describe the accuracy of the Bayley Scales of Infant Development-Second Edition (BSID-II) Mental Development Index (MDI) at 2 years of age for prediction of cognitive function at school age of children born extremely preterm.
Design
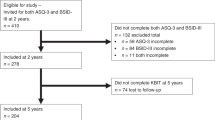
Study participants were enrolled in the Extremely Low Gestational Age Newborn Study between 2002 and 2004. Two-thirds of surviving children (n = 795) were assessed at 2 years with the BSID-II and at 10 years with an intelligence quotient (IQ) test. We computed test characteristics for a low MDI (<70), including predictive value positive.
Results
Almost two-thirds of children with a low MDI had a normal IQ (≥ 70) at 10 years. Concordance between MDI and IQ was highest among children with major motor and/or sensory impairment, and when MDI was adjusted for gestational age.
Conclusion
Most children born extremely preterm with low BSID-II MDI at 2 years have normal intelligence at school age.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
O’Shea TM, Allred EN, Dammann O, Hirtz D, Kuban KCK, Paneth N, et al. The ELGAN study of the brain and related disorders in extremely low gestational age newborns. Early Hum Dev. 2009;85:719–25.
Serenius F, Kallen K, Blennow M, Ewald U, Fellman V, Holmstrom G, et al. Neurodevelopmental outcome in extremely preterm infants at 2.5 years after active perinatal care in Sweden. J Am Med Assoc. 2013;309:1810–20.
Johnson S, Fawke J, Hennessy E, Rowell V, Thomas S, Wolke D, et al. Neurodevelopmental disability through 11 years of age in children born before 26 weeks of gestation. Pediatrics. 2009;124:E249–57.
Helderman JB, O’Shea TM, Kuban KCK, Allred EN, Hecht JL, Dammann O, et al. Antenatal antecedents of cognitive impairment at 24 months in extremely low gestational age newborns. Pediatrics. 2012;129:494–502.
Tyson JE, Parikh NA, Langer J, Green C, Higgins RD, National Institute of Child H. Intensive care for extreme prematurity–moving beyond gestational age. N Engl J Med. 2008;358:1672–81.
Marrs CC, Pedroza C, Mendez-Figueroa H, Chauhan SP, Tyson JE. Infant outcomes after periviable birth: external validation of the neonatal research network estimator with the BEAM trial. Am J Perinatol. 2015;33:569–76.
Marlow N. Measuring neurodevelopmental outcome in neonatal trials: a continuing and increasing challenge. Arch Dis Child Fetal Neonatal Ed. 2013;98:F554–8.
Morris BH, Oh W, Tyson JE, Stevenson DK, Phelps DL, O’Shea TM, et al. Aggressive vs. conservative phototherapy for infants with extremely low birth weight. New Engl J Med. 2008;359:1885–96.
Schmidt B, Davis P, Moddemann D, Ohlsson A, Roberts RS, Saigal S, et al. Long-term effects of indomethacin prophylaxis in extremely-low-birth-weight infants. N Engl J Med. 2001;344:1966–72.
Schmidt B, Roberts R, Davis P, Doyle L, Barrington K, Ohlsson A, et al. Long-term effects of caffeine therapy for apnea of prematurity. N Engl J Med. 2007;357:1893–902.
Kilbride HW, Aylward GP, Doyle LW, Singer LT, Lantos J. Prognostic neurodevelopmental testing of preterm infants: do we need to change the paradigm? J Perinatol. 2017;37:475–9.
Munck P, Niemi P, Lapinleimu H, Lehtonen L, Haataja L, Group PS. Stability of cognitive outcome from 2 to 5 years of age in very low birth weight children. Pediatrics. 2012;129:503–8.
Ross G, Lipper EG, Auld PA. Consistency and change in the development of premature infants weighing less than 1,501 grams at birth. Pediatrics. 1985;76:885–91.
Bode MM, D’Eugenio DB, Mettelman BB, Gross SJ. Predictive validity of the Bayley, Third Edition at 2 years for intelligence quotient at 4 years in preterm infants. J Dev Behav Pediatr. 2014;35:570–5.
Spencer-Smith MM, Spittle AJ, Lee KJ, Doyle LW, Anderson PJ. Bayley-III cognitive and language scales in preterm children. Pediatrics. 2015;135:e1258–65.
dos Santos E, de Kieviet J, Konigs M, van Elburg R, Oosterlaan J. Predictive value of the Bayley scales of infant development on development of very preterm/very low birth weight children: a meta-analysis. Early Hum Dev. 2013;89:487–96.
Hack M, Taylor HG, Drotar D, Schluchter M, Cartar L, Wilson-Costello D, et al. Poor predictive validity of the Bayley scales of infant development for cognitive function of extremely low birth weight children at school age. Pediatrics. 2005;116:333–41.
Yudkin PL, Aboualfa M, Eyre JA, Redman CWG, Wilkinson AR. New birth-weight and head circumference centiles for gestational ages 24 to 42 weeks. Early Hum Dev. 1987;15:45–52.
Teele R, Share J. Ultrasonography of Infants and Children. Philadelphia: Saunders; 1991.
Kuban K, Adler I, Allred EN, Batton D, Bezinque S, Betz BW, et al. Observer variability assessing US scans of the preterm brain: the ELGAN study. Pediatr Radiol. 2007;37:1201–8.
San Antonio TX, Elliott CD. Differential Ability Scales. 2nd ed. San Antonio, TX: The Psychological Corporation; 2007.
Korkman M, Kirk U, Kemp SL. NEPSY-II: Clinical and Interpretive Manual. 2nd ed. Pearson Education, Inc: London, UK; 2007.
Heeren T, Joseph RM, Allred EN, O’Shea TM, Leviton A, Kuban KCK. Cognitive functioning at age 10 years among children born extremely preterm: a latent profile approach. Pediatr Res. 2017;82:1201–16.
Fowlie PW. Towards safer diagnosis in clinical practice–understanding and using diagnostic tests in the neonatal unit more appropriately. Semin Fetal Neonatal Med. 2005;10:83–90.
Palisano R, Rosenbaum P, Walter S, Russell D, Wood E, Galuppi B. Development and reliability of a system to classify gross motor function in children with cerebral palsy. Dev Med Child Neurol. 1997;39:214–23.
Glas AS, Lijmer JG, Prins MH, Bonsel GJ, Bossuyt PM. The diagnostic odds ratio: a single indicator of test performance. J Clin Epidemiol. 2003;56:1129–35.
Bradley-Johnson S. Cognitive assessment for the youngest children: a critical review of tests. J Psychoeduc Assess. 2001;19:19–44.
Goldstein D, Folgle E, Weiber J, O’Shea T. Comparison of the Bayley scales of infant development 2nd ed. Bayley Scales Infant Dev premature Infants J Psychoed Assess. 1995;13:391–6.
Lowe JR, Erickson SJ, Schrader R, Duncan AF. Comparison of the Bayley II mental developmental index and the Bayley III cognitive scale: are we measuring the same thing? Acta Paediatr. 2012;101:E55–E8.
Black MM, K Matula. Essentials of Bayley Scales of Infant Development l-II Assessment. John Wiley & Sons, Inc.: New York, NY; 2000.
Orchinik LJ, Taylor HG, Espy KA, Minich N, Klein N, Sheffield T, et al. Cognitive outcomes for extremely preterm/extremely low birth weight children in kindergarten. J Int Neuropsychol Soc. 2011;17:1067–79.
Pugh SJ, Richardson GA, Hutcheon JA, Himes KP, Brooks MM, Day NL, et al. Maternal obesity and excessive gestational weight gain are associated with components of child cognition. J Nutr. 2015;145:2562–9.
Kuban KJ, R M, O’Shea TM, Allred EN, Heeren T, Douglass L, Stafstrom CE, Jara H, Frazier JA, Hirtz D, Leviton A. Extremely low gestational age newborn (ELGAN) study investigators girls and boys born before 28 weeks gestation: risks of cognitive, behavioral, and neurological outcomes at age 10 years. J Pediatr. 2016;173:69–75.e1.
Roberts G, Anderson PJ, Doyle LW. The stability of the diagnosis of developmental disability between ages 2 and 8 in a geographic cohort of very preterm children born in 1997. Arch Dis Child. 2010;95:786–90.
Kuban KC, Joseph RM, O’Shea TM, Allred EN, Heeren T, Douglass L, et al. Girls and boys born before 28 weeks gestation: risks of cognitive, behavioral, and neurologic outcomes at age 10 years. J Pediatr. 2016;173:69–75 e1.
Stevenson DK, Verter J, Fanaroff AA, Oh W, Ehrenkranz RA, Shankaran S, et al. Sex differences in outcomes of very low birthweight infants: the newborn male disadvantage. Arch Dis Child Fetal Neonatal Ed. 2000;83:F182–5.
Streimish IG, Ehrenkranz RA, Allred EN, O’Shea TM, Kuban KCK, Paneth N, et al. Birth weight- and fetal weight-growth restriction: Impact on neurodevelopment. Early Hum Dev. 2012;88:765–71.
O’Shea TM, Kuban KCK, Allred EN, Paneth N, Pagano M, Dammann O, et al. Neonatal cranial ultrasound lesions and developmental delays at 2 years of age among extremely low gestational age children. Pediatrics. 2008;122:E662–9.
Whitaker AH, Feldman JF, Lorenz JM, Shen S, McNicholas F, Nieto M, et al. Motor and cognitive outcomes in nondisabled low-birth-weight adolescents - Early determinants. Arch Pediatr Adolesc Med. 2006;160:1040–6.
van der Burg JW, Allred EN, Kuban K, O’Shea TM, Dammann O, Leviton A. Maternal obesity and development of the preterm newborn at 2 years. Acta Paediatr. 2015;104:900–3.
Watkins S, Jonsson-Funk M, Brookhart MA, Rosenberg SA, O’Shea TM, Daniels J. Preschool motor skills following physical and occupational therapy services among non-disabled very low birth weight children. Matern Child Health J. 2014;18:821–8.
Juul SE, Mayock DE, Comstock BA, Heagerty PJ. Neuroprotective potential of erythropoietin in neonates; design of a randomized trial. Matern Health Neonatol Perinatol. 2015;1:27.
Ballard RA, Keller RL, Black DM, Ballard PL, Merrill JD, Eichenwald EC, et al. Randomized trial of late surfactant treatment in ventilated preterm infants receiving inhaled nitric oxide. J Pediatr. 2016;168:23–9 e4.
Vaucher YE, Peralta-Carcelen M, Finer NN, Carlo WA, Gantz MG, Walsh MC, et al. Neurodevelopmental outcomes in the early CPAP and pulse oximetry trial. N Engl J Med. 2012;367:2495–504.
Silveira RC, Filipouski G, Goldstein D, O’Shea T, Procianoy R. Agreement between Bayley scales second and third edition assessments of very low birth weight infants. Arch Pediatr Adolesc Med. 2012;166:1075–6.
Anderson PJ, De Luca CR, Hutchinson E, Roberts G, Doyle LW. Underestimation of developmental delay by the new Bayley-III scale. Arch Pediatr Adolesc Med. 2010;164:352–6.
Johnson S, Moore T, Marlow N. Using the Bayley-III to assess neurodevelopmental delay: which cut-off should be used? Pediatr Res. 2014;75:670–4.
Aylward GP. Continuing issues with the Bayley-III: where to go from here. J Dev Behav Pediatr. 2013;34:697–701.
Schmidt B, Anderson PJ, Doyle LW, Dewey D, Grunau RE, Asztalos EV, et al. Survival without disability to age 5 years after neonatal caffeine therapy for apnea of prematurity. J Am Med Assoc. 2012;307:275–82.
Acknowledgements
This study was supported by the National Institute of Neurological Disorders and Stroke (Grant Nos. 5U01NS040069-05 and 2R01NS040069-09) and the Office of the Director of the National Institutes of Health (1UG3OD023348-01). We also gratefully acknowledge the contributions of their subjects, and their subjects’ families, as well as those of their colleagues listed below. This study was supported by from the Office of the Director, National Institutes of Health (1UG3OD023348-01), the National Institute of Neurological Disorders and Stroke (5U01NS040069-05 and 2R01NS040069-09), and the National Institute of Child Health and Human Development (5P30HD018655-28). Dr. Frazier has the following disclosures: serving on the data safety monitoring board for Forest Pharmaceuticals and receiving research support from Alcobra, Janssen Pharmaceuticals, Neuren, and SyneuRX International.
ELGAN Study Investigators
Bhahvesh Shah, Rachana Singh, Linda Van Marter, Camilla Martin, Janice Ware, Cynthia Cole, Ellen Perrin, Frank Bednarek, Jean Frazier, Richard Ehrenkranz, Jennifer Benjamin, T. Michael O’Shea, Carl Bose, Diane Warner, Steve Engelke, Mariel Poortenga, Steve Pastyrnak, Padu Karna, Nigel Paneth, Madeleine Lenski, Michael Schreiber, Scott Hunter, Michael Msall, Danny Batton, Judith Klarr, Karen Christianson, Deborah Klein, Maureen Pimental, Collen Hallisey, Taryn Coster, Ellen Nylen, Emily Neger, Kathryn Mattern, Lauren Venuti, Beth Powers, Ann Foley, Joanne Williams, Elaine Romano, Debbie Hiatt, Nancy Peters, Patricia Brown, Emily Ansusinha, Gennie Bose, Janice Wereszczak, Janice Bernhardt, Joan Adams, Donna Wilson, Nancy Darden-Saad, Dinah Sutton, Julie Rathbun, Karen Miras, Deborah Weiland, Grace Yoon, Rugile Ramoskaite, Suzanne Wiggins, Krissy Washington, Ryan Martin, Barbara Prendergast, Beth Kring, Anne Smith, Susan McQuiston, Samantha Butler, Rachel Wilson, Kirsten McGhee, Patricia Lee, Aimee Asgarian, Anjali Sadhwani, Brandi Henson, Cecelia Keller, Jenifer Walkowiak, Susan Barron, Alice Miller, Brian Dessureau, Molly Wood, Jill Damon-Minow, Elaine Romano, Linda Mayes, Kathy Tsatsanis, Katarzyna Chawarska, Sophy Kim, Susan Dieterich, Karen Bearrs, Ellen Waldrep, Jackie Friedman, Gail Hounshell, Debbie Allred, Rebecca Helms, Lynn Whitley, Gary Stainback, Lisa Bostic, Amanda Jacobson, Joni McKeeman, Echo Meyer, Steve Pastyrnak, Joan Price, Megan Lloyd, Susan Plesha-Troyke, Megan Scott, KatherineM. Solomon, Kara Brooklier, Kelly Vogt.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
O’Shea, T.M., Joseph, R.M., Allred, E.N. et al. Accuracy of the Bayley-II mental development index at 2 years as a predictor of cognitive impairment at school age among children born extremely preterm. J Perinatol 38, 908–916 (2018). https://doi.org/10.1038/s41372-017-0020-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-017-0020-8
This article is cited by
-
Understanding the multidimensional neurodevelopmental outcomes in children after congenital Zika virus exposure
Pediatric Research (2024)
-
Bayley trajectories predict school readiness better than single assessments in formerly very preterm preschoolers
Pediatric Research (2023)
-
Early visuospatial attention and processing and related neurodevelopmental outcome at 2 years in children born very preterm
Pediatric Research (2021)
-
Placental programming, perinatal inflammation, and neurodevelopment impairment among those born extremely preterm
Pediatric Research (2021)