Abstract
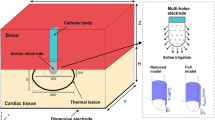
A novel three-dimensional finite element model for the study of radiofrequency ablation is presented. The model was used to perform an analysis of the temperature distribution in a tissue block heated by RF energy and cooled by blood (fluid) flow. This work extends earlier models by including true flow in place of a convective boundary condition to simulate realistic experimental conditions and to improve the prediction of blood temperatures. The effect of fluid flow on the temperature distribution, the lesion dimensions, and the ablation efficiency was studied. Three flow velocities were simulated: (i) 30, (ii) 55, and (iii) 85 mm/s. The modeling results were validated qualitatively and quantitatively with in vitro data. The correlation coefficients between the modeling and the experimental temperature measurements were 0.98, 0.97, and 0.95 for flows (i)–(iii), respectively. The slopes were 0.89, 0.95, and 1.06, and the mean root mean square differences between modeling and experimental temperature measurements were 17.3%±11.6%, 15.8% ± 13.4%, and 18.8% ± 14.9% for flows (i)–(iii), respectively. A comparison of temperature distribution obtained with a convective boundary versus inclusion of fluid motion showed that the convective boundary resulted in a similar tissue temperature distribution, but overestimated fluid temperatures and lacked the flow asymmetry seen in the true flow model. © 2000 Biomedical Engineering Society.
PAC00: 8754Br, 8719Pp, 8719Uv, 8750Jk, 0270Dh
Similar content being viewed by others
REFERENCES
Avital, B., K. Mughal, and J. Hare. The effects of thoracic electrode-tissuecontact on radiofrequency lesion generation. Pacing Clin. Electrophys.20:2899–2910, 1997.
Bejan, A. Convection Heat Transfer. New York: Wiley, 1995.
Bennet, C. O., andJ. E. Myers. Momentum, Heat and Mass Transfer. New York: McGraw-Hill, 1962.
Bowman, H. F. Heat transfer and thermal dosimetry. J. Microwave Power 16:121–133,1981.
Chato, J. C. Thermal Properties of Tissues. In: Handbook of Bioengineering, edited byR. Skalak and S. Chien. New York: McGraw-Hill, 1987.
Duck, F. A. Physical Propertiesof Tissue: A Comprehensive Reference Book. San Diego: Academic, 1990.
Foster, K. R., andH. P. Schwan. Dielectric properties of tissues and biological materials: A critical review. Crit. Rev. Biomed. Eng.17:25–104, 1989.
Geddes, L. A., and L. E. Baker. The specificresistance of biological material-a compendium of data for the biomedical engineer and physiologist. Med. Biol. Eng.5:271–293, 1967.
Haines, D. E. The biophysics of radiofrequency catheter ablation inthe heart: The importance of temperature monitoring. Pacing Clin. Electrophys.16:586–591, 1993.
Haines, D. E., and D. D. Whatson. Tissue heating during radiofrequency catheter ablation: Athermodynamic model and observations in isolated perfused and superfused canine right and left ventricular free wall. Pacing Clin. Electrophys. 12:962–976, 1989.
Hoyt, R. H., S. K. Huang, F. I. Marcus, and R. S. Odell. Factors influencing trans-catheter radiofrequency ablation of the myocardium. J. Appl. Cardiol.1:469–86, 1986.
Incropera, F. P., and D. P. DeWitt. Fundamentals ofHeat Transfer. New York: Wiley, 1981.
Jain, R. K. Bioheat transfer: Mathematical models ofthermal systems. In: Hyperthermia in Cancer Therapy, edited by F. K. Storm. Boston, MA.: Hall Medical, 1983, pp. 9–46.
Jain, M. K., and P. D. Wolf. Finite Element Analysis PredictsDose-Response Relationship for Constant Power and Temperature Controlled Radiofrequency Ablation. Proc. of the 19th Ann. Int. Conf. of the IEEE Eng. in Med. and Biol. Soc.:165–169, 1997.
Jain, M. K.,and P. D. Wolf. In vitro temperature map of cardiac tissue demonstrates the effect of flow on lesion development. Ann. Biomed. Eng.28:1066–1074, 2000.
Jain, M. K., and P. D. Wolf. Temperature controlled and constant power radiofrequency ablation: What affects lesion growth? IEEE Trans. Biomed. Eng.46:1405–1412, 1999.
Jain, M. K., P. D. Wolf, and C. S. Henriquez. Chilled-tip electrode radiofrequency ablation of the endocardium: a finite element study. Proc. of the 17th Ann. Intl. Conf. of IEEEEMBS: 273–274, 1995.
Jain, M. K., G. Tomassoni, R. E. Riley, and P. D. Wolf. Effect of skin electrode location on radiofrequency ablation lesions: An in vivo and a three dimensional finite element study. J. Cardiovasc. Electrophys.9:1225–1235, 1998.
Labonte', S. Numerical Model for Radio-Frequency Ablation of the Endocardium and its ExperimentalValidation. IEEE Trans. Biomed. Eng.41:108–115, 1994.
Mechling, J. A., and J. W. Strohbehn. A theoretical comparison of the temperature distributions produced by three interstitial hyperthermia systems. Int. J. Radiat. Oncol., Biol., Phys.12:2137–2149, 1986.
Nakagawa, H., W. S. Yamanashi, J. V. Pitha, M. Arruda, X. Wang, K. Otomo, K. J. Beckman, J. H. McClelland, R. Lazzara, and W. M. Jackman. Comparison of in vivo tissue temperature profile and lesion geometry for radiofrequency ablation with a saline-irrigated electrode versus temperature control in a canine thigh muscle preparation. Circulation91:2264–2273, 1991.
Panescu, D., J. G. Whayne, S. D. Fleischman, M.S. Mirotznik, D. K. Swanson, and J. G. Webster. Threedimensional finite element analysis of current density and temperature distributions during radio-frequency ablation. IEEE Trans. Biomed. Eng.42:879–890, 1995.
Pennes, H. H. Analysis of tissue and arterial blood temperatures in resting forearm. J.Appl. Physiol.1:93–122, 1948.
Roth, B. J., F. L. H. Gielen, and J. P. Wikswo, Jr.Spatial and temporal frequency-dependent conductivities in volumeconduction for skeletal muscle. Math. Biosci.88:159–189, 1988.
Shahidi, A. V., and P. Savard. A finite element model forradiofrequency ablation of the myocardium. IEEE Trans. Biomed. Eng.41:963–968, 1994.
Stuchly, M. A., and S. S. Stuchly. Dielectric properties of biological substances: Tabulated. J.Microwave Power15:19–26, 1980.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Jain, M.K., Wolf, P.D. A Three-Dimensional Finite Element Model of Radiofrequency Ablation with Blood Flow and its Experimental Validation. Annals of Biomedical Engineering 28, 1075–1084 (2000). https://doi.org/10.1114/1.1310219
Issue Date:
DOI: https://doi.org/10.1114/1.1310219