Abstract
Background
Human papillomavirus (HPV) is the major predictor of outcome in oropharyngeal squamous cell carcinoma (OSCC) but the disease is heterogeneous and there is limited understanding of the prognostic significance of other molecular markers in relation to HPV. This multi-institutional, retrospective study examined the prognostic significance of Ki67 expression in association with HPV status in OSCC.
Methods
The 105 patients recruited had a median follow-up of 70 months. Tumor HPV status was determined by HPV E6-targeted multiplex real-time polymerase chain reaction/p16 semiquantitative immunohistochemistry and Ki67 expression by semiquantitative immunohistochemistry. Determinants of recurrence and mortality hazards were modelled using Cox regression with censoring at dates of last follow-up.
Results
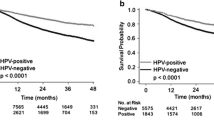
HPV and Ki67 positivity rates were 46 and 44 %, respectively. HPV-positive cancers were more likely to be Ki67-positive. On multivariate analysis, both HPV and Ki67 were predictors of outcome. Ki67-positive cancers were associated with a 3.13-fold increased risk of disease-related death compared with Ki67-negative cancers. Among HPV-negative patients, Ki67-positive disease was associated with 5.6-fold increased risk of oropharyngeal cancer-related death (p = 0.002), 5.5-fold increased risk of death from any cause (p = 0.001), and 2.9-fold increased risk of any event (p = 0.013). The risk of locoregional failure was lowest in patients with HPV-positive/Ki67-positive cancers.
Conclusions
Ki67 predicts disease-related death in oropharyngeal cancer independent of HPV status. A combination of Ki67 and HPV status provides improved prognostic information relative to HPV status alone. Our data suggest, for the first time, that Ki67 status has prognostic value, particularly in HPV-negative oropharyngeal cancer.

Similar content being viewed by others
REFERENCES
Hong AM, Dobbins TA, Lee CS, et al. Human papillomavirus predicts outcome in oropharyngeal cancer in patients treated primarily with surgery or radiation therapy. Br J Cancer. 2010;103(10):1510–1517.
Lassen P, Eriksen JG, Hamilton-Dutoit S, Tramm T, Alsner J, Overgaard J. Effect of HPV-associated p16INK4A expression on response to radiotherapy and survival in squamous cell carcinoma of the head and neck. J Clin Oncol. 2009;27(12):1992–1998.
Gillison ML. Human papillomavirus and prognosis of oropharyngeal squamous cell carcinoma: implications for clinical research in head and neck cancers. J Clin Oncol. 2006;24(36):5623–5625.
Gillison ML. Human papillomavirus-associated head and neck cancer is a distinct epidemiologic, clinical, and molecular entity. Semin Oncol. 2004;31(6):744–754.
Weinberger PM, Yu Z, Haffty BG, et al. Molecular classification identifies a subset of human papillomavirus–associated oropharyngeal cancers with favorable prognosis. J Clin Oncol. 2006;24(5):736–747.
Hong AM, Martin A, Chatfield M, et al. Human papillomavirus, smoking status and outcomes in tonsillar squamous cell carcinoma. Int J Cancer. 2013;132(12):2748–2754.
Rainsbury JW, Ahmed W, Williams HK, Roberts S, Paleri V, Mehanna H. Prognostic biomarkers of survival in oropharyngeal squamous cell carcinoma: systematic review and meta-analysis. Head Neck. 2013;35(7):1048–1055.
Schliephake H. Prognostic relevance of molecular markers of oral cancer: a review. Int J Oral Maxillofac Surg. 2003;32(3):233–245.
Brown DC, Gatter KC. Ki67 protein: the immaculate deception? Histopathology. 2002;40(1):2–11.
van Diest PJ, van der Wall E, Baak JP. Prognostic value of proliferation in invasive breast cancer: a review. J Clin Pathol. 2004;57(7):675–681.
Pich A, Chiusa L, Navone R. Prognostic significance of cell proliferation in head and neck tumors. Ann Oncol. 2004;15:1319–1329.
Ritta M, De Andrea M, Mondini M, et al. Cell cycle and viral and immunologic profiles of head and neck squamous cell carcinoma as predictable variables of tumor progression. Head Neck. 2009;31(3):318–327.
De Petrini M, Ritta M, Schena M, et al. Head and neck squamous cell carcinoma: role of the human papillomavirus in tumour progression. New Microbiol. 2006;29(1):25–33.
Grabenbauer GG, Muhlfriedel C, Rodel F, et al. Squamous cell carcinoma of the oropharynx: Ki-67 and p53 can identify patients at high risk for local recurrence after surgery and postoperative radiotherapy. Int J Radiat Oncol Biol Phys. 2000;48(4):1041–1050.
Klussmann JP, Gultekin E, Weissenborn SJ, et al. Expression of p16 protein identifies a distinct entity of tonsillar carcinomas associated with human papillomavirus. Am J Pathol. 2003;162(3):747–753.
Smeets SJ, Hesselink AT, Speel EJ, et al. A novel algorithm for reliable detection of human papillomavirus in paraffin embedded head and neck cancer specimen. Int J Cancer. 2007;121(11):2465–2472.
Stanley KK, Szewczuk E. Multiplexed tandem PCR: gene profiling from small amounts of RNA using SYBR Green detection. Nucleic Acids Res. 2005;33(20):e180.
Hong AM, Dobbins TA, Lee CS, et al. Use of cyclin D1 in conjunction with human papillomavirus status to predict outcome in oropharyngeal cancer. Int J Cancer. 2011;128(7):1532-1545.
Hong A, Jones D, Chatfield M, et al. HPV status of oropharyngeal cancer by combination HPV DNA/p16 testing: biological relevance of discordant results. Ann Surg Oncol. 2013;20 Suppl 3:S450-458.
Hong A, Jones D, Chatfield M, et al. HPV status of oropharyngeal cancer by combination HPV DNA/p16 testing: biological relevance of discordant results. Ann Surg Oncol. 2013;20 Suppl 3:450–458.
Homma A, Furuta Y, Oridate N, et al. Prognostic significance of clinical parameters and biological markers in patients with squamous cell carcinoma of the head and neck treated with concurrent chemoradiotherapy. Clin Cancer Res. 1999;5(4):801–806.
Lavertu P, Adelstein DJ, Myles J, Secic M. P53 and Ki-67 as outcome predictors for advanced squamous cell cancers of the head and neck treated with chemoradiotherapy. Laryngoscope. 2001;111(11 Pt 1):1878–1892.
Roland NJ, Caslin AW, Bowie GL, Jones AS. Has the cellular proliferation marker Ki67 any clinical relevance in squamous cell carcinoma of the head and neck? Clin Otolaryngol Allied Sci. 1994;19(1):13–18.
Barber BR, Biron VL, Klimowicz AC, Puttagunta L, Cote DW, Seikaly H. Molecular predictors of locoregional and distant metastases in oropharyngeal squamous cell carcinoma. J Otolaryngol Head Neck Surg. 2013;42(1):53.
ACKNOWLEDGMENT
The authors gratefully acknowledge the financial support of the Sydney Head and Neck Cancer Institute, Cure Cancer Australia, and Cancer Australia. We would also like to thank the clinicians at all the participating hospitals.
DISCLOSURE
The authors have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
10434_2014_4237_MOESM1_ESM.tif
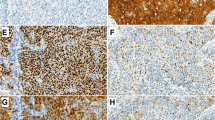
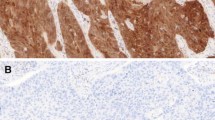
Supplementary material 1 (TIFF 2701 kb) Representative images of immunohistochemical expression of Ki67 fromhigh-expressing (Left; Ki67-positive) and low-expressing (Right; Ki67-negative) OSCC. Immunohistochemical staining shows positive cells in brown colour,counterstained with Harris’ hematoxylin
Rights and permissions
About this article
Cite this article
Liu, J., Zhang, M., Rose, B. et al. Ki67 Expression has Prognostic Significance in Relation to Human Papillomavirus Status in Oropharyngeal Squamous Cell Carcinoma. Ann Surg Oncol 22, 1893–1900 (2015). https://doi.org/10.1245/s10434-014-4237-x
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1245/s10434-014-4237-x