Abstract
Summary: The selection of patients with severe vertebrobasilar artery stenosis for angioplasty is based mainly on clinical experience rather than on controlled data. We present a patient with severe vertebral artery stenosis in whom we could document the positive effect of angioplasty on posterior circulation hemodynamics by using transcranial Doppler sonography.
Atheromatous disease of the intracranial vertebrobasilar system is usually treated medically either with platelet aggregation inhibitors or with oral anticoagulants. In selected patients, blood flow through the vertebral or basilar arteries is restored by angioplasty. Because of potentially deleterious complications in the posterior circulation, this procedure is applied principally to patients with severe vertebrobasilar ischemic symptoms. The selection of patients is based mainly on clinical experience and on the arteriographic appearance of the stenosis. There are few controlled data on which to base the decision to proceed with angioplasty of the intracranial vertebrobasilar arteries (1–5). In contrast, there is some experience concerning the embolic and hemodynamic risk of carotid disease (6, 7). A controlled study is underway to compare carotid endarterectomy with carotid angioplasty (8).
We present a patient with severe stenosis of the distal vertebral artery in whom we could document the hemodynamic effect of successful angioplasty by using transcranial Doppler sonography (TCD).
Case Report
A 70-year-old hypertensive man had recurrent vertigo for 2 weeks, precipitated by a right, locked head position, vomiting, right upper quadrantanopia, and slight dysarthria. MR tomography showed multiple bilateral cerebellar infarcts, an infarct in the upper brain stem, and an infarct in the territory of the left posterior cerebral artery (PCA). Four-vessel digital subtraction angiography revealed that the right PCA had a fetal origin from the right internal carotid artery; there was no right P1 segment. On the left side, the PCA arose from the basilar artery, there was no left posterior communicating artery. Therefore, the right PCA was supplied exclusively by the anterior circulation whereas the left PCA was supplied exclusively from the basilar artery. There was one left vertebral artery, the right vertebral artery was aplastic. The left vertebral artery had approximately 50% stenosis at the origin and a tight (>95%) stenosis of the distal segment at the level of the foramen magnum (Fig 1A).
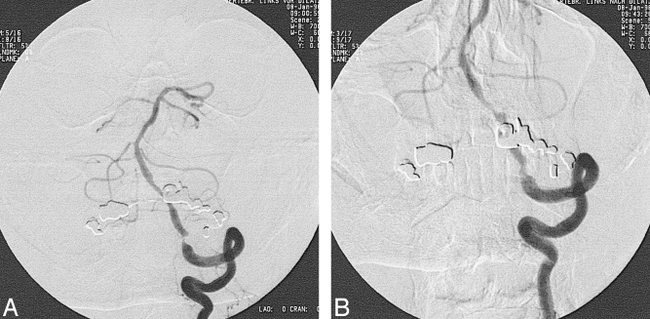
Digital subtraction angiography of the vertebrobasilar system.
A, Before angioplasty, there is a 95% stenosis of the distal segment at the level of the foramen magnum.
B, After angioplasty, there is a residual 50% stenosis.
Cerebrovascular reserve was assessed by TCD (9). Briefly, the percentage of change of mean blood flow velocity is measured during a sequence of breath-holding trials and is plotted over the time of breath-holding. Cerebrovascular reserve in the territory of the PCA was intact on the right side and lost on the left side (Fig 2A). The patient was off any antihypertensive medication. During the examination, his blood pressure was continuously around 220/100 mm Hg. Because there was no evidence of collateral flow in the posterior circulation angiographically, we proceeded with angioplasty to restore perfusion of the basilar artery and of the left PCA territory.
Cerebrovascular reserve, defined as percentage of change in mean blood flow velocity in the PCA over time of breath-holding.
A, Before angioplasty, there is marked impairment of cerebrovascular reserve on the left side as compared with the right.
B, After angioplasty, cerebrovascular reserve is equal on both sides.
Angioplasty was performed in two steps: first, with the use of a balloon catheter (Meditech, Westwood, MA), the proximal vertebral artery stenosis was approached and was slightly dilated up to a degree of 40%. We did not attempt to further dilate this proximal stenosis, because we considered this degree of stenosis hemodynamically irrelevant. In a second step, the distal stenosis was dilated using a Stealth balloon catheter (Target Therapeutics, Freemont, CA). The balloon was inflated twice for 10 seconds. During the procedure, the patient was awake and remained asymptomatic. The stenosis was dilated up to a degree of about 50% (Fig 1B).
Cerebrovascular reserve studies after angioplasty showed equal cerebrovascular reserve in both PCAs, the patient was still hypertensive with a blood pressure of 200/100 mm Hg (Fig 2B). During the course of a 6-month follow-up period, the patient did not experience further ischemic events. Repeated evaluation of the vertebral artery by TCD and repeated cerebrovascular reserve studies did not show recurrence of vertebral artery stenosis.
Discussion
This selected case illustrates that revascularization of a hemodynamically relevant vertebral artery stenosis can normalize abnormal cerebrovascular reserve in the posterior circulation assessed by TCD. Impaired cerebrovascular reserve in the middle cerebral artery territory shown by TCD has been found to be a risk for stroke in patients with unilateral carotid artery occlusion (10). Nonetheless, this has not yet been shown in the posterior circulation. Whether or not reversal of an abnormal cerebrovascular reserve shown by TCD reduces the risk of stroke is unknown, so we cannot comment on this. This case, however, demonstrates the use of cerebrovascular reserve in establishing marked impairment of perfusion pressure in the territory supplied by the vertebrobasilar system.
Conclusion
Cerebrovascular reserve studies may be helpful in the selection of patients for angioplasty in the vertebrobasilar system.
Footnotes
↵1 Address reprint requests to Georg Gahn, MD, Department of Neurology, Technical University of Dresden, Fetscher Str. 74, D-01307 Dresden, Germany.
References
- Received September 29, 1998.
- Accepted after revision January 12, 1999.
- Copyright © American Society of Neuroradiology