Abstract
Summary: We report the unusual case of pulsatile tinnitus caused by muscular branches of the occipital artery, which developed to supply the distal vertebral artery after subclavian artery occlusion. Anatomical findings and options of endovascular treatment are discussed. To our knowledge, subclavian artery occlusion causing an objective tinnitus has not been reported.
Pulsatile tinnitus is a rare but potentially disabling symptom, which can be caused by both vascular and nonvascular abnormalities (1, 2). Subclavian steal syndrome is a systemic entity that is well documented in the medical literature. It occurs when the subclavian artery becomes stenosed or occluded and blood flow is reversed in the ipsilateral vertebral artery that supplies the ipsilateral arm (3). Anastomoses between muscular branches of the occipital artery and vertebral artery can develop when one of their supplying territories is insufficient (4). These anastomoses run close to the occipital bone, and their pulse can be transmitted to the ear. Percutaneous angioplasty and stent placement of a complete occlusion of the subclavian artery resulted in resolution of the symptoms.
Case Report
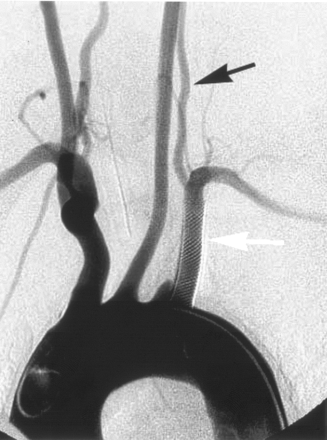
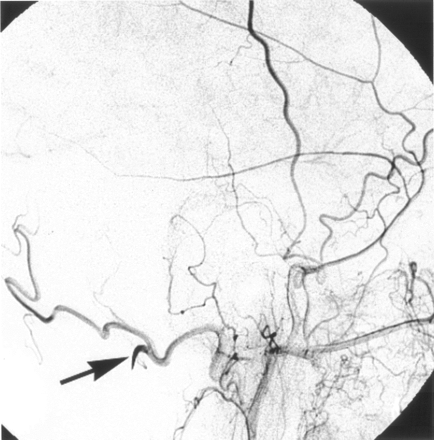
A 65-year-old woman had a pulsatile tinnitus on the left side, which had started 1 year earlier. The patient had a left subclavian artery occlusion diagnosed 3 years earlier when moving the left arm started causing vertigo. Aspirin therapy, 160 mg daily, was then initiated. The auscultation revealed a murmur in the left retroauricular region, which did not change during head rotation but disappeared when the left common carotid artery was compressed. MR imaging did not show any brain abnormality. To exclude a dural arteriovenous fistula on the left lateral sinus, we obtained a cerebral angiogram with the patient under general anesthesia. Both common carotid arteries and the right subclavian artery were selectively injected. The left subclavian artery was occluded above the left vertebral artery origin. The right subclavian artery injection showed a high-grade stenosis at the level of the vertebral artery origin and a delayed and reversed filling of the left vertebral and subclavian arteries. (Fig 1). Selective injection of the left external carotid and occipital arteries showed a filling of the proatlantal I and II anastomoses, providing reversed flow to the left vertebral and deep cervical arteries that supply the left arm arterial vasculature (Fig 2). Because of the clinical findings and especially because of the fact that the tinnitus disappeared when the left common carotid artery was compressed, the enlarged suboccipital anastomoses were considered the cause of the patient’s symptoms.
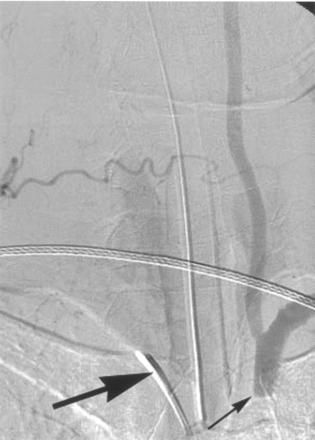
Selective arteriogram of the right subclavian artery (large arrow, catheter placed in this vessel), anteroposterior view, late phase, shows reversed flow in the left vertebral artery and the occluded proximal left subclavian artery (small arrow) as well as antegrade filling of the distal left subclavian artery.
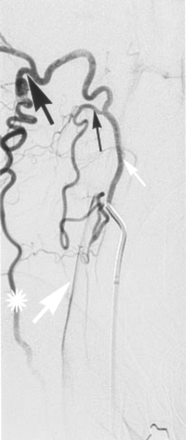
Selective arteriogram of the left occipital artery (small white arrow), lateral view after catheterization, shows the proatlantal I (small black arrow) and II (large black arrow) anastomoses providing retrograde flow to the left vertebral (large white arrow) and the left deep cervical (*) arteries.
Percutaneous transluminal angioplasty of the left subclavian artery occlusion was performed with the patient under general anesthesia and full anticoagulation (an initial bolus of 5000 IU of heparin followed by a continuous infusion of 2500–3000 IU/hour to maintain an activated clotting time between 200 and 300 seconds). A 250-mg bolus of aspirin was also administered intravenously. The left brachial artery was punctured, and a 6F sheath was introduced. A 5F catheter was navigated close to the subclavian artery occlusion (Fig 3). The occlusion was passed using a 0.035-inch guidewire (150 cm in length, Terumo Corporation, Tokyo, Japan), and the 5F catheter tip was pushed over the wire in the descending aorta. Then the guidewire was replaced by a longer one (260 cm in length, Terumo Corporation). Then, 2 percutaneous transluminal angioplasty Fox balloon catheters (6 × 15 mm and 8 × 20 mm) (Abbott Laboratories, Abbott Park, IL) were successfully navigated and inflated at the left subclavian artery origin (Fig 4).
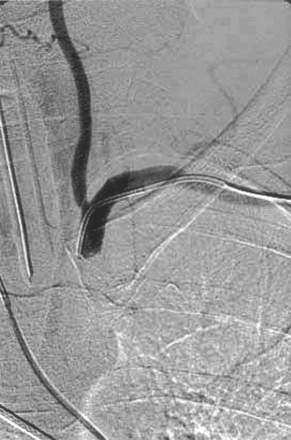
Selective arteriogram of the right subclavian artery, anteroposterior view, late phase, shows the 5F catheter navigated in the left subclavian artery after left transbrachial approach.
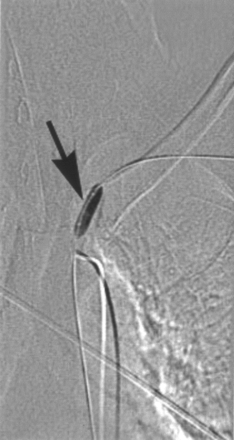
A blank road rap, anteroposterior view, shows the inflated percutaneous transluminal angioplasty balloon after passing the occlusion with a 0.0035-inch guidewire.
A self-expandable stent (Wallstent, 8/28 mm, Boston Scientific, Natick, MA) was then deployed proximal to the left vertebral artery origin. During the same procedure, using the femoral approach, we treated the right vertebral artery origin stenosis by placing a balloon-expandable stent (Liberte, 2.75 × 8 mm, Boston Scientific).
The final aortic arch angiogram showed patency of the left subclavian artery and both vertebral arteries (Fig 5). A left selective external carotid arteriogram showed complete disappearance of the previously enlarged skull base anastomoses (Fig 6). Postprocedurally, the pulsatile tinnitus resolved completely, and blood pressure was equal in both arms.
Arteriogram of the aortic arch after stent placement (white arrow) shows the recanalized left subclavian artery and the antegrade flow in the left vertebral artery (black arrow).
Postoperative left external carotid arteriogram, lateral view, shows that there is no longer filling of the skull base anastomoses. Note the contrast stagnation at the origin of the proatlantal II artery (arrow).
Discussion
Pulsatile tinnitus, also called vibratory tinnitus, manifests as an intracranial murmur, synchronous with the heartbeat. It can become significantly disturbing for a patient, and in some cases, it may be the only diagnostic clue to a potentially devastating or life-threatening disease, such as a dural arteriovenous fistula with cortical venous drainage. A tinnitus is classified as objective when the murmur is heard by the examiner or subjective when only the patient hears it. A vascular disorder causing pulsatile tinnitus can be either arterial (ie, internal carotid stenosis or dissection) or venous (ie, flow turbulences due to an arteriovenous shunt surgery lesion or a vascular tumor) (5–9). Among arteriovenous shunts, dural arteriovenous fistulas or carotid-cavernous sinus fistulas are most commonly found (1).
The suboccipital carrefour or “knot” refers to a network of anastomoses interconnecting the cervical, vertebral, occipital, and carotid arteries that has been well described in humans (3, 10). When a stenosis of the common carotid artery is present, the suboccipital carrefour may enlarge to provide collateral blood flow from subclavian to external carotid territories (11). In case of a subclavian artery origin occlusion proximal to the vertebral artery origin, a subclavian steal phenomenon may develop, caused by a flow reversal within the left vertebral artery that supplies the ipsilateral arm. Clinically, this is more frequently associated with a simple arm claudication (55%) than with a vertebrobasilar insufficiency (15%), both of which are present in 30% of patients (12).
In our report, tinnitus was objectively heard by the examiner and disappeared when the ipsilateral carotid artery was compressed, indicating a vascular disorder. On the initial angiogram, the left subclavian artery was occluded, and the contralateral vertebral artery origin was stenosed. Because of the flow reduction, anastomoses between the left occipital artery, the left vertebral artery, and the left deep cervical artery (proatlantal arteries I and II) progressively enlarged to maintain blood supply to the left arm. Because of a widely patent right posterior communicating artery, there was no vertebrobasilar insufficiency. The proatlantal arteries run close to the petrous bone, and their arterial pulsation can be transmitted to the ear.
The endovascular treatment was performed with antiplatelet therapy and full heparinization, while the reversed flow in the left vertebral artery protected the vertebrobasilar system from thromboembolic complication. At the end of the procedure, the left subclavian artery was fully recanalized and the anastomoses completely disappeared. The fact that the tinnitus disappeared after the procedure confirmed the causality between these anastomoses and the disturbing murmur. The patient no longer heard the bruit, and the blood pressure became equal on both arms.
References
- Received November 19, 2004.
- Accepted after revision November 28, 2004.
- Copyright © American Society of Neuroradiology