Abstract
BACKGROUND AND PURPOSE: Fluoroscopic-guided lumbar puncture is an effective alternative to bedside lumbar puncture in challenging patients. However, no published guidelines are available for an acceptable range of fluoroscopic time for this procedure. The purpose of this study was to set department benchmark fluoroscopic times for lumbar puncture, accounting for body mass index in our patient population.
MATERIALS AND METHODS: We identified and reviewed all patients who underwent fluoroscopic-guided lumbar puncture at 4 hospitals during a 2-year period (July 2011 to June 2013). Data collection included patient information (demographics, body mass index, history of prior lumbar surgery and/or lumbar hardware, scoliosis); procedure details (fluoroscopic time, level of access, approach, needle gauge and length); level of operator experience; and hospital site. A generalized linear model was used to test whether body mass index influenced fluoroscopic time while controlling other factors.
RESULTS: Five hundred eighty-four patients (mean age, 47.8 ± 16.2 years; range, 16–92 years; 33% male) had successful fluoroscopic-guided lumbar puncture s. Mean body mass index and fluoroscopic time were higher in female patients (34.4 ± 9.9 kg/m2 and 1.07 minutes; 95% CI, 0.95–1.20) than in male patients (29.2 ± 7.3 kg/m2 and 0.91 minutes; 95% CI, 0.79–1.03). Body mass index (P = .001), hospital site (P < .001), and level of experience (P = .03) were factors significantly affecting fluoroscopic time on multivariate analysis. Benchmark fluoroscopic times in minutes were the following: 0.48 (95% CI, 0.40–0.56) for normal, 0.61 for overweight (95% CI, 0.52–0.71), 0.63(95% CI, 0.58–0.73) for obese, and 0.86 (95% CI, 0.74–1.01) in extremely obese body mass index categories.
CONCLUSIONS: In patients undergoing fluoroscopic-guided lumbar punctures, fluoroscopy time increased with body mass index We established benchmark fluoroscopic-guided lumbar puncture time ranges as related to body mass index in our patient population.
ABBREVIATIONS:
- ACR
- American College of Radiology
- BMI
- body mass index
- FGLP
- fluoroscopic-guided lumbar puncture
- IIH
- idiopathic intracranial hypertension
- LP
- lumbar puncture
Lumbar puncture (LP) is an invasive technique that accesses the restricted compartment of the subarachnoid space to sample CSF. This procedure involves the percutaneous introduction of a needle below the termination level of the spinal cord, passing through the dura mater of the spinal canal and entering the subarachnoid space. The diagnostic LP is typically performed at the bedside by using surface landmark guidance, as first described by Quincke in 1891.1 However, surface landmark identification of underlying structures has been shown to be accurate only 30% of the time and can be difficult in the obese patient.2
CSF analysis is a valuable diagnostic tool. The American College of Radiology (ACR) Appropriateness Criteria include LP as a recommended procedure in the setting of negative findings on CT head in the clinical scenario of thunderclap headache when subarachnoid hemorrhage is suspected.3 Valid indications for CSF sampling also include suspected CNS infection, demyelinating disease, and CNS malignancy. The LP technique is also used to access the CSF space to allow instillation of chemotherapeutic agents, antispasmodics, and contrast media.4
Fluoroscopic-guided lumbar puncture (FGLP) is an effective alternative to bedside LP in patients with challenging body habitus. LP performed under fluoroscopic guidance can be less traumatic, therefore having a decreased likelihood of spurious false-positive results of hemorrhage and hence avoiding subsequent investigations such as CTA and conventional angiography.5 However patients are exposed to ionizing radiation during the procedure and obesity by itself is a predisposing factor for an increased procedure-associated radiation dose, as proved with interventional cardiology.6 Obesity is a growing epidemic with a specific increase in the obese and extremely obese body mass index (BMI) categories during the past 50 years.7,8 Increasing reliance by the clinicians on radiology to perform FGLPs may be a reflection of this epidemic. Both the American Board of Radiology and the Accreditation Council for Graduate Medical Education have recognized FGLP as a core competency in radiology residency and neuroradiology fellowship training.9⇓–11
In 2011, The Joint Commission released a sentinel alert expressing concern about the American population exposure to ionizing radiation and significant increase in the contribution of medical imaging to overall ionizing radiation. Medical radiation constitutes almost half (3.0 mSv) of the US population average annual radiation exposure (6.1 mSv) and 5 times the per capita effective dose of the global population from medical exposure (0.64 mSv).12 The Joint Commission advised physicians to review their practices to reduce radiation exposure to as low as reasonably achievable without compromising patient care.13
The ACR recommends documentation of actual fluoroscopy time for all procedures in the patient medical record.14,15 In addition, the ACR also recommends that the documented fluoroscopic times for various procedures should then be compared with benchmark figures.14 However, a thorough literature search revealed a lack of guideline or benchmark data for the FGLP procedure.
The purpose of this study was to establish baseline fluoroscopic time ranges for FGLP and to evaluate the variability of fluoroscopic time ranges relative to national BMI categories in our patient population. We tested the hypothesis that the fluoroscopic times for the LP increase with increases in BMI.
Materials and Methods
Patient Population
All patients who had FGLP at any of the 4 hospitals in our health care system (University Hospital, University Hospital Midtown, Orthopedic and Spine Center, and Memorial Hospital) during 24 consecutive months (July 1, 2011 to June 30, 2013) were identified for review. The radiology information system at these 4 hospitals was searched by using the department procedure codes “XR Spine LP” and “Fluoroscopic-guided spinal tap” to identify subjects. All successful FGLPs performed on a standard fluoroscopic table for which the fluoroscopic time and BMI were known were included in this study. On the basis of the standard policy for requesting FGLP by the radiology department, most of these patients had at least 2 failed attempts at bedside LP. Direct FGLP was available to patients with pre-existing challenging conditions such as marked obesity, severe scoliosis, and/or prior lumbar surgery with underlying scar tissue and/or spinal-fixation hardware. This study was reviewed and granted institutional review board exemption.
Procedure Technique
Following informed consent, all patients underwent the FGLP procedure in the prone or prone oblique position by using a standard fluoroscopic table in the radiology department. The procedure is performed by using sterile technique.4 The Centers for Disease Control and Prevention recommendations of using a facemask, aseptic technique, and following other safe injection practices for performing a spinal injection procedure to prevent the risk of bacterial meningitis16 are routinely applied.
Routine access was at the L3/4 level with few variations involving the L2/3, L4/5, and L5/S1 levels. Twenty-two-gauge needles were most commonly used and occasionally lower (14 ga, 16 ga, 18 ga, and 20 ga) or higher (23 ga and 25 ga) gauge needles were used. Intermittent-pulse fluoroscopy was used to identify the appropriate site for the LP and to monitor the course of the advancing needle during the procedure until the subarachnoid space was entered, confirmed by the reflux of clear CSF, marking the end point of the fluoroscope use. The radiology report routinely included the fluoroscopy time and any known immediate complications from the procedure. Board-certified, subspecialty-trained neuroradiologists and trainees (diagnostic radiology residents and neuroradiology fellows) performed the FGLPs during the study period. Faculty directly or indirectly supervised trainees. The level of experience of the operator was recorded.
Data Collection
The radiology information at the 4 hospitals was searched by using the department procedure codes “XR Spine LP” and “Fluoroscopic-guided spinal tap.” The procedure report and the stored images were reviewed (A.C., S.R.B., R.P.) by using electronic medical records and PACS, respectively. Age, sex, BMI, and hospital site parameters were obtained from the electronic medical records. The BMI was obtained from the electronic medical records directly or calculated on the basis of the height and weight documented in the records by using the formula: Weight (kg) / [Height (m)]2. Fluoroscopic screening time, clinical indication, approach, side, level of procedure, needle size and length, and experience of the operator were documented from the radiology report. A history of prior lumbar surgery, scoliosis, and spinal hardware were identified on image review and review of patient clinical notes.
Categorization of BMI, Clinical Indication, and Other Variables
Patients were grouped on the basis of their body mass index according to obesity guidelines of the National Heart, Lung, and Blood Institute17: underweight (BMI < 18.5), normal (BMI = 18.5–24.9), overweight (BMI = 25–29.9), obese (BMI = 30–39.9), and extremely obese (BMI ≥ 40). Patients were also categorized on the basis of the clinical indications provided by the referring clinicians, including the following: altered mental status, infection, inflammation, neoplasm, cognitive decline, CSF leak, intrathecal chemotherapy or baclofen, idiopathic intracranial hypertension (IIH), and suspected hemorrhage.
Patients were dichotomized for the presence or absence of lumbar surgery, scoliosis, and lumbar orthopedic hardware as noted from radiograph and chart review. The variable “approach” was categorized into “Media/Interspinal” and “Paramedian/Paraspinal” needle approach. Variable “Side” was documented for patients with “Paramedian/Paraspinal” approach as “Right” or “Left.” “Needle length” was categorized as “Standard (3.5 inches)” or “Longer” (5 or 7 inches) as related to the spinal needle length used. “Level of procedure” was categorized as “Upper” (L2/3 and L3/4) and “Lower” (L4/5 and L5/S1) to describe the level at which access to the subarachnoid space was achieved. “Needle size” was divided into 3 groups: “22 ga,” “<22 ga,” and “>22 ga.” Operator experience was grouped as “Junior Resident (R1/R2),” “Senior Resident (R3/R4),” “Fellow,” and “Attending.” Sixteen attending neuroradiologists and 32 trainees (radiology residents and neuroradiology fellows) performed the procedures. Trainees performed 94% of the procedures under the direct or indirect supervision of the attending physicians.
Statistical Analysis
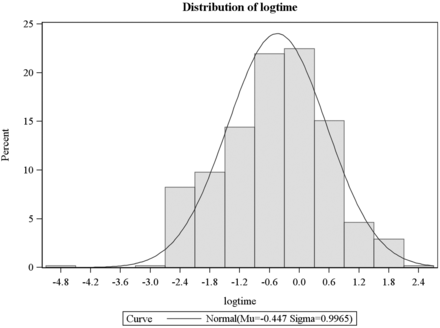
The outcome variable, fluoroscopic time, was considered as the continuous variable. BMI, sex, age, prior lumbar surgery, scoliosis, lumbar spine hardware, approach, indication, level, side, needle size, needle length, operator experience, and hospital site were all considered potential factors affecting the fluoroscopic time. The mean, median, SD, and 95% CI of the mean were calculated for the continuous variables. One-way ANOVA was used to test for any difference of BMI across the groups of the characteristics of patients. The Fisher exact test was used to test for any association between the characteristics of patients and categorized BMI. Generalized linear model regression was used for univariate and multivariate analyses on fluoroscopic time. Log transformation was applied for fluoroscopic time (Fig 1), to fit the model better because the distribution was highly skewed (Fig 2). The Akaike information criterion was used for model selection. The significance level for the analyses was .05. SAS 9.3 (SAS Institute, Cary, North Carolina) was used for data management and analyses.
The distribution of log-transformed fluoroscopic time versus patient population. Normal distribution of the fluoroscopic time following log transformation of the skewed raw data of the fluoroscopic time.
The distribution of fluoroscopic time versus patient population. Because the distribution of the fluoroscopic time is highly skewed, log transformation is applied to the fluoroscopic time to fit the model better.
Results
Patient Population
A total of 653 procedures were found in the radiology information system search. Following the exclusion criteria (Table 1), we excluded 69 patients. Five hundred eighty-four patients (389 men and 195 women) constituted the study population. The mean age was 47.8 ± 16.2 years, and the mean BMI of study population was 31.8 ± 8.6 kg/m2. The age of the obese (46.8 ± 14.9 years) and extremely obese (40 ± 12.8 years) patients was significantly lower (P < .001) than that in the patients with normal BMI (51.1 ± 16.7 years).
Exclusion criteria
Patient Characteristics Based on BMI and Clinical Indication
The mean BMI of the female patients (34.4 ± 9.9) was significantly higher (P < .001) than that of the male patients (29.2 ± 7.3). The mean BMI of the patients with prior lumbar spine surgery (30.4 ± 6.7) and scoliosis (25.8 ± 6.4) was significantly lower than that in patients without surgery (32.9 ± 9.6, P < .01) and without scoliosis (33.1 ± 9.4, P < .001).
The most common reasons for referral for FGLP were IIH closely followed by infection and inflammation (Table 2). The mean BMI of patients with IIH (40.5 ± 8.6) was significantly higher than any other clinical indications (P < .001). The mean BMI of patients who required a longer LP needle (5 or 7 inches) was 39.2 ± 7.7 and 46.9 ± 7.5, respectively, significantly higher (P < .001) than that in patients (27.6 ± 6.0) who had the procedure with a standard needle (3.5 inches). No significant variation in the patient BMI was noted between different operator levels of experience or different health care sites.
The association between categorized BMI and clinical indication of patients
Fluoroscopic Time Based on Clinical Indication
Patients with IIH had the maximum mean fluoroscopic time of 0.81 minutes (95% CI, 0.70–0.93 minutes) compared with all other clinical indications. Patients with suspected subarachnoid hemorrhage evaluation had the least fluoroscopic time of 0.41 minutes (95% CI, 0.22–0.74 minutes). The fluoroscopic time distribution based on the clinical indication is summarized in Table 3.
Fluoroscopic time in minutes based on the clinical indication of the patients
Fluoroscopic Time: Univariate Analysis
Approach (P = .01), clinical indication (P = .01), BMI (P < .001), level (P = .005), needle length (P < .001), operator experience (P < .001), and hospital site (P < .001) significantly affected the fluoroscopic time. Sex (P = .66), surgery (P = .88), scoliosis (P = .22), hardware (P = .61), side (P = .15) and needle size (P = .3) had no significant effect on fluoroscopic time. The fluoroscopic time of patients with normal BMI was significantly shorter than that of the patients in overweight (P < .05), obese (P = .02), and extremely obese (P < .001) BMI weight categories.
Fluoroscopic Time: Multivariate Analysis
BMI (P = .001), hospital site (P < .001), and experience of the operator (P = .03) were factors significantly affecting the fluoroscopic time. On the basis of operator experience, fluoroscopic time for the LPs performed by the “Fellows” was significantly lower (P = .03) compared with “Residents” and “Attendings.” Note that the “Attending” cases may have been completed after failed resident or fellow attempts. Approach and level variables had a marginally significant effect on fluoroscopic time. FGLP performed by using a paramedian approach had a shorter fluoroscopic time compared with a midline approach (P = .08). Fluoroscopic time for FGLP performed at lower levels (L4/5 and L5/S1) was marginally longer than procedures performed at higher levels (L2/3 and L3/4) (P = .07). BMI affected the fluoroscopic time significantly after controlling for approach, hospital site, level, and experience variables.
Fluoroscopic Time according to the BMI
The benchmark fluoroscopic times for the LP based on the BMI are summarized in Table 4. The mean fluoroscopic time for LP increased with an increase in the BMI compared with patients with normal BMI on both pre- and postlogarithmic conversion of the data. The fluoroscopic time of the patients with normal BMI was significantly shorter than that of the patients who are obese (P = .02) or extremely obese (P < .001), while controlling for other variables. The significantly shorter fluoroscopic time of the normal BMI compared with overweight BMI noted on univariate analysis (P < .05) was not confirmed in the multivariate analysis (P = .09).
Benchmark fluoroscopic time in minutes based on BMI categories17
Discussion
Our study demonstrated a longer fluoroscopic time with increasing BMI. Table 5 summarizes the differences in the patient distribution based on the BMI categories between the study population and age-adjusted American adults 20 years or older, based on the National Health and Nutrition Examination Survey 2009–2010 data.8 The percentage of the extremely obese patients in our study population was almost 4 times higher than the national average. The percentage of the extremely obese female patients was significantly higher (P < .001) in our study population compared with the age-adjusted prevalence in the US population. The normal BMI patient subgroup constituted only 21% of the study population, whereas the obese and extremely obese patients together constituted more than half (53%) of the study population. The prevalence of the obese and extremely obese BMI distribution in our study population was significantly higher (P < .001) in the female population (62%) compared with males (39%) and higher in the younger age group. This pattern of BMI distribution with obese and extremely obese patients among the young female patients was well above the national average. The authors hypothesize that this finding can be related to the number of patients with IIH in our study and note the correlation of that diagnosis and both female sex and obesity. In our study population, IIH was the single largest clinical indication, with 149 patients (26%), closely followed by infection. The mean BMI of the IIH group was significantly higher (P < .001) than the mean BMI of any other clinical indication.
Comparison of the percentage of overweight, obese, and extreme obesity distribution of patient population from the current study versus age-adjusted prevalence among US adults 20 years of age and older
There were 12 underweight (BMI < 18.5 kg/m2) patients in our study. Despite low BMI, these patients had paradoxically higher mean fluoroscopic time than any other BMI groups. The authors propose that this group, more so than the others, had very challenging patients, including individuals with cerebral palsy (n = 3), HIV encephalopathy (n = 5), terminally ill malignancy (n = 3), and CNS vaculities (n = 1). Many of these patients were poorly oriented and had difficulty maintaining position and following the instructions. In addition, the small number of patients in this category contributing only 2% of the study population could explain the paradoxical trend in this group. This theory was substantiated by the wide confidence intervals and higher SD and standard error of this group compared with the other BMI groups.
Understandably, patients with IIH present a greater challenge to successful bedside LP due to associated high BMI and difficulty in palpating the bony landmarks. Laxity of adipose tissues and long needle lengths necessary in the obese patients can complicate the procedure and potentially increase the amount of fluoroscopic time. In our study group, patients in the IIH subgroup had the highest mean fluoroscopic time of 0.81 minutes (95% CI, 0.70–0.93 minutes) as well as a maximum mean BMI of 40.5 ± 8.8 kg/m2. Although clinical indication was a statistically significant variable on the univariate analysis, this variable was not chosen by the multivariate analysis.
The referrals of patients in the infection subgroup were not related to their BMI; mean BMI in this subgroup was 30.5 ± 8.6 kg/m2. These patients pose a challenge for the bedside LP related to increased agitation and inability to stay still for longer times, which was usually documented on clinical request or progress notes accessed from the electronic medical records. Increased referrals for FGLP in this subgroup were likely related to the potential of more rapid access to the subarachnoid space with fluoroscopic guidance, as reflected in our study with a mean fluoroscopic time of 0.61 minutes (95% CI, 0.53–0.74 minutes).
The health care facility is a significant variable affecting the fluoroscopic time. There is no significant variation in the BMI categories between the health care facilities to explain this variation. The authors hypothesize that this variation is related to the work flow variations such as technicians obtaining a localizer image before the start of a procedure by a radiologist and variability in the duration of hands-on for the trainees before faculty takeover for difficult cases. Also, IIH, the clinical indication with the maximum mean fluoroscopic time, constitutes 29% of Memorial Hospital study population. IIH represents 24% at University and 21% at University Midtown hospital site study population.
The level of operator experience is another significant variable affecting the fluoroscopic time. Fluoroscopic time for the LPs performed by “Fellows” is significantly lower (P = .03), compared with “Residents” and “Attendings.” The variation between “Resident” and “Fellow” fluoroscopic times is probably related to increased operator experience by/during fellowship. The variation between “Fellow” and “Attending” fluoroscopic times might reflect the fact that at our teaching institution, trainees typically perform the procedures (under supervision) to the point of completion or until the attending takes over in cases of difficulty. In rare instances of no resident or fellow on service or by patient request, the attending is the sole operator. In either of these instances, the cumulative fluoroscopic time is credited to the attending.
The authors realize that target time values are needed to assess the quality and safety of the current practice of FGLP at their institutions. The authors searched the current literature and were unable to identify targeted fluoroscopic time values for this procedure or for variation in the fluoroscopic time of LP as related to BMI.
Brook et al18 showed that both the CT and fluoroscopic-guided LP are a useful alternatives with low procedure times and radiation dose in obese patients with prior failed unguided attempts. However, the authors in that study measured the total procedure time but not the actual radiation screening time. While CT guidance is a viable alternative to FGLP, at our facilities, the greater availability of the fluoroscopy slots, workflow considerations, rapid room turnaround time, and patient physical characteristics as related to the geometry of the tube size and table limit are some of the reasons we do not routinely use CT for subarachnoid space access. Recently the Stanford Orthopedic Group published their experience of a 30% increase in the fluoroscopic time in overweight patients undergoing spine interventions. However subcategorization of the overweight BMI (>25 kg/m2) was not considered, and none of the patients had FGLP in this study.19
Given the lack of published guidelines, this study contributes to the literature by providing the baseline fluoroscopic time based on the BMI categories. We plan to use these data as a benchmark in the evaluation of the individual and department performance with an aim to keep the fluoroscopic time as low as reasonably achievable and specifically within the 2 SD range. Furthermore, these data can be used to identify the individual trends in the fluoroscopic times, provide feedback to operators about their performance, identify the outliers, and prompt targeted education and/or intervention for the outliers. Overall, these data can be a great resource toward improvement of patient care, radiation safety, and training.
Limitations
We acknowledge the limitations of the study, including but not limited to its retrospective nature and the regionally specific patient population of this single institution. This study was performed at an academic center and has inevitable patient-selection bias. Because most of the procedures are performed by the trainees, variable trainee confidence levels and the point of takeover by the attending in difficult cases were not documented; this lack of documentation can be an area of potential bias. In addition, we could not control for certain patient factors including anxiety, ability/willingness to cooperate, individual pain threshold, pre-existing degenerative changes or spinal stenosis, and postsurgical scar tissue or hardware. Those variables could certainly impact the time it takes to do the procedure.
Conclusions
BMI affects the fluoroscopic time significantly after controlling for other variables (approach, hospital site, level of access, and operator experience). The fluoroscopic time increases with increasing BMI. We were able to establish benchmark fluoroscopic time ranges for our patient population in relation to their BMI. Tracking fluoroscopy time and an ongoing quality assurance program with operators are essential to minimize radiation exposure for both patients and radiation heath workers.
Footnotes
Disclosures: Amanda Corey—UNRELATED: Other: Osler Institute, Comments: speaker at their ear, nose, and throat review course. Patricia A. Hudgins—UNRELATED: Royalties: Amirsys, Inc, Comments: medical education company. Kimberly E. Applegate—UNRELATED: Board Membership: Association of University Radiologists, ACR, Comments: Volunteer, Consultancy: American Imaging Management, Comments: Advisory Board on patient safety, Royalties: Springer Publishing, Comments: Coeditor of a textbook series on evidence-based imaging.
Paper previously presented at: Annual Meeting of the American Society of Neuroradiology, May 18–23, 2013; San Diego, California. (An additional year of data has been added in the article.)
Indicates open access to non-subscribers at www.ajnr.org
REFERENCES
- Received October 25, 2013.
- Accepted after revision December 23, 2013.
- © 2014 by American Journal of Neuroradiology