Abstract
BACKGROUND AND PURPOSE: Magnetization transfer ratio histogram peak height (MTR-HPH) has been shown to correlate with macroscopic and microscopic brain disease in patients with multiple sclerosis (MS). We studied the changes in MTR-HPH and in Kurtzke's Expanded Disability Status Scale (EDSS) scores over time in a group of patients with relapsing-remitting MS.
METHODS: Twenty adult patients with relapsing-remitting MS (four men and 16 women) were followed up for a period of 334 to 1313 days. In all, 86 MR imaging studies of the brain were obtained, and MTR-HPH was calculated for each MR examination by using a semiautomated technique. Changes in MTR-HPH were compared between patients over the study's duration. A neurologist specialized in the care of MS patients assessed the EDSS score for each patient as a measure of clinical disability.
RESULTS: Serial MR data showed a subtle but significant decline in MTR-HPH with time. No significant changes in EDSS scores were noted over the same period.
CONCLUSION: Patients with relapsing-remitting MS have a significant progressive decline in normalized MTR-HPH, which is independent of EDSS score. MTR-HPH measurements can be used to monitor subclinical disease in patients with relapsing-remitting MS over a short time frame of 1 to 4 years. This parameter might be applied in future therapeutic trials to assess its usefulness.
Contrast-enhanced T1- and T2-weighted MR imaging has been the mainstay in the assessment of patients with multiple sclerosis (MS). Contrast-enhanced T1-weighted sequences have proved useful for detecting lesions with active inflammation (1). Nevertheless, measuring the long-term progression of MS is difficult with contrast-enhanced T1-weighted sequences because lesion enhancement is transient. Several investigators have used T2-weighted sequences to demonstrate that, over time, MS patients incur a great number and volume of white matter lesions as well as brain atrophy (2, 3). The interferon beta-1b (IFN-â) trial revealed that untreated patients with relapsing-remitting MS showed median increases of 6.7% and 30.2% in T2-weighted MR lesion volume over a period of 1 and 5 years, respectively (4). With treatment, the progression of MS brain disease as detected on MR images can be retarded. Patients treated with IFN-â showed a significantly lower rate of increase of T2-weighted lesion volume in comparison with placebo-treated control subjects over the 5-year duration of the study (4).
The normal-appearing white matter (NAWM) in MS patients contains microscopic pathologic abnormalities that are not detected by standard T2-weighted lesion volumetric measurements (5–7). Such MR-occult disease may contribute to clinical abnormalities in MS patients. Previous work using magnetization transfer (MT) and spectroscopy has shown that these techniques consistently depict abnormalities in the NAWM of patients with clinically definite MS (5, 6, 8–12). The MT ratio (MTR) of both NAWM and macroscopic T2-weighted lesions is significantly lower than that of white matter in healthy control subjects (5, 10, 13). These studies also have shown that the MTR of macroscopic lesions is lower than that of NAWM. The difference in MTR between macroscopic lesions and NAWM has been attributed to a variety of histopathologic changes. As such, MT imaging has been reported to be a sensitive indicator of both macroscopic and microscopic disease in MS patients (5, 9, 11). Specifically, MTR histogram peak height (MTR-HPH) is a robust parameter for assessing global brain disease in these patients (14). Van Buchem and colleagues (11, 14) believe that MTR-HPH reflects a residual amount of normal brain tissue in MS patients. This method retains the sensitivity of MT imaging to macroscopic and microscopic MS brain disease, and has interobserver and intraobserver correlations greater than 99%. The above characteristics of MTR-HPH would make it an optimal parameter with which to follow up macroscopic and microscopic brain disease in MS patients. To our knowledge, however, changes in MTR-HPH have been not been investigated for more than a year. Our study was designed to examine any trend in MTR-HPH changes in patients with relapsing-remitting MS.
Even though the aforementioned MR techniques are strongly reproducible in the putative assessment of lesion burden, clinical assessment of disability can be difficult to quantitate. Disability in MS patients is commonly assessed by means of Kurtzke's Expanded Disability Status Scale (EDSS), which is used to monitor disease progression and assess therapeutic outcome (15). Nevertheless, the EDSS score has a high inter- and intrarater variability and employs a nonlinear scale (16–19). Therefore, more accurate clinical and paraclinical measures of disease progression are needed for monitoring the course of MS.
In this study, we tested the efficacy of MTR-HPH for following MS disease progression in patients with relapsing-remitting MS. Changes in EDSS score were examined over the same time period.
Methods
Patients with a diagnosis of MS as defined by Poser criteria (20) have been followed up with prospective MR imaging and neurologic examinations at our institution. All such patients with relapsing-remitting MS who had at least three serial MR examinations were included for analysis. Each MR examination was required to be of diagnostic quality and to include the MT imaging sequence. Twenty patients (four men and 16 women) ranging in age from 21 to 50 years (mean age, 37 years) were followed up for an average of 748 days (range, 334 to 1313 days) and underwent a total of 86 MR studies (range, three to seven MR examinations per patient). Eleven of these patients did not receive steroids or maintenance therapy for MS (ie, interferon) for the entire duration of the study. Steroid treatment was instituted in eight patients for acute clinical exacerbation, usually for a period of 1 month. Although we excluded patients on maintenance IFN-â therapy at the onset of the study, three patients received this medication after, on average, 60% (range, 55% to 66%) of the study period had been completed. Two of these patients had one MR examination and the third patient had two MR studies after beginning the medication.
All MR examinations were performed on the same 1.5-T magnet with a quadrature head coil. The MT imaging protocol has been described in prior publications (11, 14) and is described briefly herein. MT imaging was performed in the axial plane by using a modified 3D gradient-echo pulse sequence. The sequence was designed to minimize both T1 and T2 weighting (106/5 [TR/TE]; flip angle, 12°; section thickness, 5 mm; matrix, 256 × 128; field-of-view, 22 cm). A 19-millisecond single cycle, sinc-shaped saturation pulse at a frequency 2 kHz below water resonance with an amplitude of 3.7 × 10−6 T was applied approximately 1 millisecond before each excitation in order to provide selective partial saturation of macromolecular spins. The above sequence was repeated without the application of an off-resonance saturation pulse to obtain control data. The raw data for each study were transferred to a workstation via the departmental picture archiving and communications system.
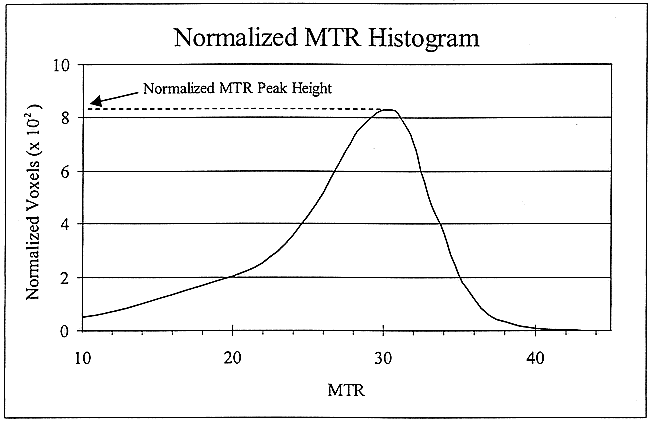
The analysis of MT images was performed as implemented by van Buchem et al (14), and is described briefly herein. A Sparc 20 workstation (Sun Microsystems, Palo Alto, CA) was used to analyze global brain tissue. A neuroradiologist identified CSF and brain parenchyma, specifying seed points by using regions of interest (ROIs). Each image then was segmented automatically to map the area of the brain parenchyma with the exclusion of bone, scalp, and CSF (21). When necessary, the segmented images were corrected manually by a trained neuroradiologist. The computer software (22) analyzed data in a 3D fashion using the concept of fuzzy connectedness (23). MTR was calculated for each brain voxel by using the equation MTR = [(MO − MS)/MO] × 100%, where MO and MS represent signal intensity of the voxel with MT saturation off and on, respectively. For each MR examination, MTR data from brain parenchymal voxels were sorted in increments of 1%. To correct for the variation in head size and positioning among patients, normalization was performed. The frequency of each MTR value was divided by the total number of voxels, yielding a normalized MTR value. From this, a normalized whole-brain MTR histogram was created, and the MTR-HPH was recorded from the normalized MTR histogram for each MR study (Fig 1). Normalized whole-brain MTR-HPH is the fraction of voxels representing the largest histogram frequency.
Normalized MTR histogram from a single MR examination. MTR-HPH measures 0.083.
A neurologist specialized in the care of MS patients examined each patient in conjunction with every MR examination visit. Functional disability in motor (pyramidal and cerebellar), sensory, brain stem, bowel/bladder, visual, and cerebral (mental) function was assessed (15). A numeric EDSS scale from zero to 10 (with 0.5 increments) was calculated using the findings of functional disability and the ability to ambulate. The EDSS score was recorded for each visit.
Median absolute deviation linear regression was used to assess trends in MTR-HPH over time for each subject. The single-sample Wilcoxon rank sum test was used to determine whether the median of the patients' slopes differed from zero, indicating a trend in MTR-HPH over time. Changes in EDSS scores over time were assessed using the same method. Statistical analysis was performed using S+ software (Mathsoft, Seattle, WA) for the IBM-compatible personal computer. The three patients who received IFN-â in mid-study did not constitute an adequate statistical sample for separate analysis.
Results
The average MTR-HPH was 0.083 ± 0.012 (mean ± SD). Fourteen patients had a negative slope of MTR-HPH over time, whereas five patients had a positive slope. One patient had a horizontal MTR-HPH slope over time. On average, patients with relapsing-remitting MS experienced a 5% decrease in MTR-HPH. The Wilcoxon rank sum test for comparison of MTR-HPH slopes among patients showed a significant negative slope over time (P < .05). The EDSS slopes did not demonstrate any significant changes over the same time period (P = NS) (Fig 2). A persistent increase in EDSS score of at least 1 point was seen in 25% of patients, whereas another 25% of patients showed a persistent decrease in EDSS score of at least 1 point. The remainder had no change in EDSS score.
Representative patient data show no significant change in EDSS score with time. Nevertheless, a significant decline in MTR-HPH is seen during the same period. Median absolute deviation linear regression was used to calculate slopes for changes in MTR-HPH and EDSS scores over time.
Discussion
Disease progression in patients with relapsing-remitting MS is typically assessed by MR lesion volume or EDSS score. In one study (4), 30% of placebo-treated MS patients had a cumulative increase in lesion volume on T2-weighted MR images over a period of 5 years. In the same study, disease progression was retarded in a dose-dependent manner using maintenance IFN-â therapy. The treated patients showed a significant dose-dependent benefit, with an increase in MR lesion volumes between 3.6% and 10.6% after 5 years. Our study found a statistically significant decline in MTR-HPH in patients with relapsing-remitting MS (Fig 3). Variability in MTR-HPH was observed for all patients over time, and for that reason, a best-fit line was obtained using median absolute deviation linear regression. On average, there was 5% decline in MTR-HPH per year for our group of patients with relapsing-remitting MS. Our study supports the findings of the IFN-â trial in demonstrating progression of global brain disease in patients with relapsing-remitting MS.
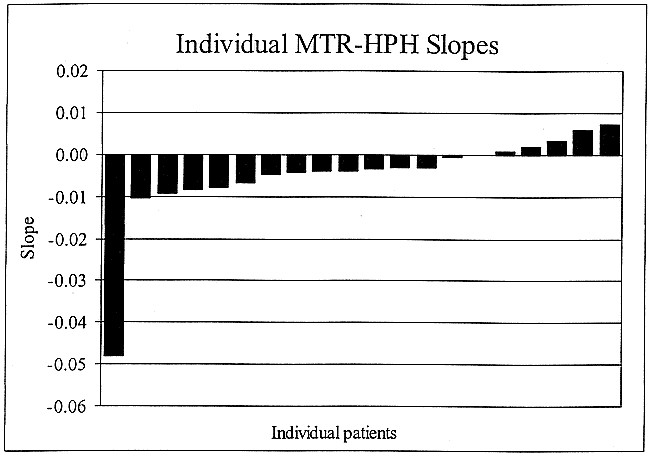
Graph shows distribution of MTR-HPH slope (change in MTR-HPH per year) for an individual patient. The average slope for the study group was −0.005. A statistically significant number of patients with relapsing-remitting MS show a decline in MTR-HPH with time.
Histopathologic examination shows microscopic brain disease in MS that is not typically detected on conventional T2-weighted MR images. These regions have been referred to as NAWM. The IFN-â trial used T2-weighted lesion volume as a measure of MS brain disease. Other MR parameters have been used to study MS disease progression, including brain volume, enhancing lesion volume, and T1 signal changes. These conventional MR parameters, however, have not been shown to be sensitive to disease in NAWM. Conversely, several studies have reported MTR analysis to be sensitive to disease in macroscopic lesions and to that in NAWM (5, 9, 11).
Calculation of the MTR provides a standardization of MT analysis and allows comparisons to be made between different regions of the brain. Although MTR analysis is a robust technique, Gass et al (24) report that selection of imaging sequence parameters can affect absolute MTR values. These authors found a lower MTR in the NAWM of MS patients as compared with the MTR in white matter of control subjects; however, this did not reach statistical significance. Although these authors attribute this difference to variations in the imaging parameters used, it may also be explained in part by the criteria used to select white matter ROIs. Focal areas of NAWM abnormalities have been seen that sometimes cover a width of only a few pixels (25). Filippi et al (10) have shown that, with decreasing distance to a macroscopic MS lesion, the white matter exhibits a progressive decrease in MTR values, making proper selection of the ROI an important variable when assessing NAWM.
Whole-brain MTR-HPH provides a global evaluation, and is resistant to variations caused by volume averaging and misregistration. Because whole-brain evaluation is performed with this method, ROI selection for MTR measurement is not needed. MTR histogram analysis can be used for objective and quantitative comparison between MR examinations obtained at different times or from different patients. The MTR histogram analysis is a robust technique, with intraobserver and interobserver correlations greater than 99% (14). These factors, in combination with the sensitivity of MT imaging to macroscopic and microscopic disease, make MTR-HPH a useful method for measuring the progression of global brain disease in MS patients. The clinical EDSS score did not show significant trends in our patient population, suggesting that MTR-HPH may be an independent measure of subclinical brain disease.
MTR histogram parameters other than MTR-HPH have been used to measure brain disease in MS patients. A recent study showed that an MTR histogram area divided by quartiles can be used to examine changes in white matter lesion burden (26). The same study showed an inverse correlation between MTR-HPH and white matter lesion load, but this did not reach statistical significance. The authors report that the shorter follow-up period (12 months) of their patients may be a possible explanation. Interestingly, this study showed variability in MTR-HPH over time that persisted even when there was an absence of new enhancing lesions. The control subjects did not show similar variability in MTR-HPH. Our patient group also displayed variability of MTR-HPH with time, and therefore we used median absolute linear regression to assess trends over time.
The IFN-â trial demonstrated a progression of disability by at least 1 EDSS point over 5 years in 46% of placebo-treated patients with relapsing-remitting MS (4). Comparatively, 35% of patients with relapsing-remitting MS treated with the higher dose of IFN-â showed a 1-point or greater change in EDSS score; however, this difference did not reach statistical significance. The EDSS score did not change significantly over time in our patient population. One fourth of the patients had a persistent decline of at least 1 EDSS point, whereas another quarter had a persistent increase of at least 1 EDSS point. The difference between our findings and those of the IFN-â trial may be the result of the shorter follow-up period in our study. Our data suggest that EDSS may be a relatively insensitive measure of disease progression in patients with relapsing-remitting MS over relatively short periods of time. Possible reasons for the low sensitivity of EDSS include the use of an arbitrary scale with limited and discrete levels of disability. EDSS also relies heavily on motor function evaluation and requires a subjective evaluation of disability using a parametric scale. Consistent with these potential limitations, EDSS has a high inter- and intrarater variability and employs a nonlinear scale (16–19). Intrarater reproducibility with modification of the EDSS is improved when scores between 1.0 and 3.5 are examined (26). The authors reported that a modified bowel and bladder disability scale, not the scoring of cerebral function or ambulatory disability, was the reason for the improvement in reproducibility. The absence of ambulatory assessment limits the EDSS evaluation to scores of 3.5 or less.
A drawback to the brain MTR-HPH method is the absence of evaluation of disease within the spinal cord. Nevertheless, because only a minority of MS patients have significant involvement of the spinal cord, this may represent only a minor limitation. Because the EDSS score relies considerably on motor function, it therefore provides a better assessment of spinal cord involvement in MS patients. Spinal evaluation using MTR-HPH would be conceivable if similar MT examinations of the spinal cord were performed. We have not attempted this at present.
Conclusion
MTR-HPH shows a subtle but significant decline in MTR-HPH in patients with relapsing-remitting MS. MTR-HPH may be useful in future therapeutic trials, because it is independent of clinical EDSS scoring and provides a measure of global macroscopic and microscopic brain changes.
Footnotes
1 Supported by grants R01 NS29029-01A1, R01 NS37172, R29-NS34353, and M01-RR00044 from the National Institutes of Health.
2 Address reprint requests to Robert I. Grossman, MD, Department of Radiology, Neuroradiology Section, Hospital of the University of Pennsylvania, 3400 Spruce St, Philadelphia, PA 19104.
References
- Received June 19, 1998.
- Accepted after revision February 26, 1999.
- Copyright © American Society of Neuroradiology