Abstract
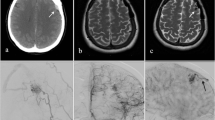
Brain vascular malformations are dynamic disorders. Although mostly considered to be of congenital origin, the improvement of clinical imaging and vasculogenesis knowledge has shown that they might also result from a biological dysfunction of the remodeling process after birth. Venous occlusive disease and ishemia may represent powerful revealing triggers and support the capillary venous origin of some vascular malformations. We report a unique case of the development of multiple de novo vascular malformations (transverse sinus dural fistula and posterior fossa cavernomas) following acoustic neuroma surgery.





Similar content being viewed by others
References
Chaudhary MY, Sachdev VP, Cho SH, Weitzner I, Jr., Puljic S, Huang YP (1982) Dural arteriovenous malformation of the major venous sinuses: an acquired lesion. AJNR Am J Neuroradiol 3:13–19
Houser OW, Campbell JK, Campbell RJ, Sundt TM, Jr. (1979) Arteriovenous malformation affecting the transverse dural venous sinus—an acquired lesion. Mayo Clin Proc 54:651–661
Ishikawa T, Houkin K, Tokuda K, Kawaguchi S, Kashiwaba T (1997) Development of anterior cranial fossa dural arteriovenous malformation following head trauma. Case report. J Neurosurg 86:291–293
Ozawa T, Miyasaka Y, Tanaka R, Kurata A, Fujii K (1998) Dural-pial arteriovenous malformation after sinus thrombosis. Stroke 29:1721–1724
Zabramski JM, Wascher TM, Spetzler RF, Johnson B, Golfinos J, Drayer BP, Brown B, Rigamonti D, Brown G (1994) The natural history of familial cavernous malformations: results of an ongoing study. J Neurosurg 80:422–432
Brunereau L, Levy C, Laberge S, Houtteville J, Labauge P (2000) De novo lesions in familial form of cerebral cavernous malformations: clinical and MR features in 29 non-Hispanic families. Surg Neurol 53:475–482
Porter PJ, Willinsky RA, Harper W, Wallace MC (1997) Cerebral cavernous malformations: natural history and prognosis after clinical deterioration with or without hemorrhage. J Neurosurg 2:190–197
Labauge P, Brunereau L, Coubes P, Clanet M, Tannier C, Laberge S, Levy C (2001) Appearance of new lesions in two nonfamilial cerebral cavernoma patients. Eur Neurol 45:83–88
Massa-Micon B, Luparello V, Bergui M, Pagni CA (2000) De novo cavernoma case report and review of literature. Surg Neurol 53:484–487
Houtteville JP (1997) Brain cavernoma: a dynamic lesion. Surg Neurol 48:610–614
Labauge P, Laberge S, Brunereau L, Levy C, Tournier-Lasserve E (1998) Hereditary cerebral cavernous angiomas: clinical and genetic features in 57 French families. Societe Francaise de Neurochirurgie. Lancet 352:1892–1897
Pozzati E, Acciarri N, Tognetti F, Marliani F, Giangaspero F (1996) Growth, subsequent bleeding, and de novo appearance of cerebral cavernous angiomas. Neurosurgery 38:662–669
Zouaoui A, Maillard JC, Ganthier V, Chedid G, Dangeard S (1995) Modern imaging in cerebral vein angioma. J Neuroradiol 22:86–102
Kupersmith MJ, Kalish H, Epstein F, Yu G, Berenstein A, Woo H, Jafar J, Mandel G, De Lara F (2001) Natural history of brainstem cavernous malformations. Neurosurgery 48:47–53
Lasjaunias P (1997) A revised concept of the congenital nature of cerebral arteriovenous malformations. Intervent Neuroradiol 3:275–281
Itoyama Y, Kitano I, Fujioka S, Takagi S, Morioka M, Yano T, Kai Y, Ushio Y (1994) Mixed angioma of the brain: report of two cases. No Shinkei Geka 22:465–469
Awad IA, Robinson JR, Mohanty S, Estes ML (1993) Mixed vascular malformations of the brain: Clinical and pathogenetic considerations. Neurosurgery:179–188
Janz C, Meisel J, Brock P, Lasjaunias P (2002) De novo appearance of three cavernomas in an infant with dural AV shunts. Intervent Neuroradiol:85–90
Acknowledgements
The authors are grateful to Drs. MC Wallace, R. Willinsky, P.J. Porter and to the Toronto Brain Vascular Malformations Study Group for their support.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Desal, H.A., Lee, S.K., Kim, B.S. et al. Multiple de novo vascular malformations in relation to diffuse venous occlusive disease: a case report. Neuroradiology 47, 38–42 (2005). https://doi.org/10.1007/s00234-003-0971-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-003-0971-7