Abstract
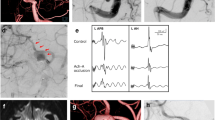
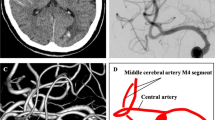
A prospective study was performed to evaluate the efficacy of neurophysiological monitoring (NPM) techniques in the detection of ischemic changes that may be seen during endovascular treatment of cerebral aneurysms. Sixty three patients underwent NPM during first-stage endovascular treatment of cerebral aneurysms. The endovascular procedures included coil embolization (26 patients), balloon-remodeling coiling (16 patients), stent-assisted coiling (ten patients), balloon-stent-assisted coiling (nine patients), and balloon test occlusion (two patients). NPM included electroencephalography, somatosensory evoked potentials, and brain stem auditory evoked potentials, depending on the location of the aneurysm and its associated vascular territory. NPM changes were seen in three patients (4.8%), and the procedures were altered immediately. No neurological changes were found postendovascularly. Ten patients demonstrated abnormal angiographic findings without concurrent NPM changes, of which five patients developed visual disturbance or hemiparesis. It is concluded that NPM is a valuable monitoring tool for endovascular treatment of cerebral aneurysms.



Similar content being viewed by others
References
Anderson LC, Hemler DE, Luethke JM, Latchaw RE (1994) Transcranial magnetic evoked potentials used to monitor the spinal cord during neuroradiologic angiography of the spine. Spine 19:613–616
Berenstein A, Young W, Ransohoff J, Benjamin V, Merkin H (1984) Somatosensory evoked potentials during spinal angiography and therapeutic transvascular embolization. J Neurosurg 60(4):777–785
Branston NM, Ladds A, Symon L, Wang AD (1984) Comparison of the effects of ischaemia on early components of the somatosensory evoked potential in brainstem, thalamus, and cerebral cortex. J Cereb Blood Flow Metab 4:68–81
Cedzich C, Schramm J, Mengedoht CF, Fahlbusch R (1988) Factors that limit the use of flash visual evoked potentials for surgical monitoring. Electroencephalogr Clin Neurophysiol 71(2):142–145
Cloughesy TF, Nuwer MR, Hoch D, Viñuela F, Duckwiler G, Martin N (1993) Monitoring carotid test occlusions with continuous EEG and clinical examination. J Clin Neurophysiol 10:363–369
Debatisse D, Pralong E, Dehdashti AR, Regli L (2005) Simultaneous multilobar electrocorticography (mEcoG) and scalp electroencephalography (scalp EEG) during intracranial vascular surgery: a new approach in neuromonitoring. Clin Neurophysiol 116:2734–2740
Deletis V, Sala F (2008) Intraoperative neurophysiological monitoring of the spinal cord during spinal cord and spine surgery: a review focus on the corticospinal tracts. Clin Neurophysiol 119(2):248–264
Ferbert A, Buchner H, Bruckmann H, Zeumer H, Hacke W (1988) Evoked potentials in basilar artery thrombosis: correlation with clinical and angiographic findings. Electroencephalogr Clin Neurophysiol 69:136–147
Florence G, Guerit JM, Gueguen B (2004) Electroencephalography (EEG) and somatosensory evoked potentials (SEP) to prevent cerebral ischaemia in the operating room. Neurophysiol Clin 34:17–32
Hargadine JR, Branston NM, Symon L (1980) Central conduction time in primate brain ischemia: a study in baboons. Stroke 11:637–642
Huotari AM, Koskinen M, Suominen K, Alahuhta S, Remes R, Hartikainen KM, Jantti V (2004) Evoked EEG patterns during burst suppression with propofol. Br J Anaesth 92:18–24
Hyun SJ, Rhim SC (2009) Combined motor and somatosensory evoked potential monitoring for intramedullary spinal cord tumor surgery: correlation of clinical and neurophysiological data in 17 consecutive procedures. Br J Neurosurg 23(4):393–400
John ER, Chabot RJ, Prichep LS, Ransohoff J, Epstein F, Berenstein A (1989) Real-time intraoperative monitoring during neurosurgical and neuroradiological procedures. J Clin Neurophysiol 6(2):125–158
Jones TH, Morawetz RB, Crowell RM (1981) Thresholds of focal cerebral ischemia in awake monkeys. J Neurosurg 54:773–782
Kothbauer KF (2007) Intraoperative neurophysiologic monitoring for intramedullary spinal-cord tumor surgery. Neurophysiol Clin 37(6):407–414
Krieger D, Adams HP, Albert DIMF, Haken MV, Hacke W (1992) Pure motor hemiparesis with stable somatosensory evoked potential monitoring during aneurysm surgery: case report. Neurosurgery 31:145–150
Lesnick JE, Michele JJ, Simeone FA, DeFeo S, Welsh FA (1984) Alteration of somatosensory evoked potentials in response to global ischemia. J Neurosurg 60:490–494
Little JR, Lesser RP, Luders H (1987) Electrophysiological monitoring during basilar aneurysm operation. Neurosurgery 20(3):421–427
Lopez JR, Chang SD, Steinberg GK (1999) The use of electrophysiological monitoring in the intraoperative management of intracranial aneurysms. J Neurol Neurosurg Psychiatry 66:189–196
Martin CJ, Sinson G, Patterson T, Zager EL, Strecker MM (2002) Sensitivity of scalp EEG, cortical EEG, and somatosensory evoked responses during surgery for intracranial aneurysms. Surg Neurol 58:317–320
Min KT, Kim JH, Shin YS, Kwon SY, Nam YT (2001) The monitoring of somatosensory evoked potentials and neurologic complications in aneurysm surgery. Yonsei Med J 42(2):227–232
Mizoi K, Yoshimoto T (1993) Permissible temporary occlusion time in aneurysm surgery as evaluated by evoked potential monitoring. Neurosurgery 33:434–440
Niimi Y, Sala F, Deletis V, Setton A, de Camargo AB, Berenstein A (2004) Neurophysiologic monitoring and pharmacologic provocative testing for embolization of spinal cord arteriovenous malformations. AJNR Am J Neuroradiol 25(7):1131–1138
Paiva T, Campos J, Baeta E, Gomes LB, Martins IP, Parreira E (1995) EEG monitoring during endovascular embolization of cerebral arteriovenous malformations. Electroencephalogr Clin Neurophysiol l95:3–13
Paulsen RD, Steinberg GK, Norbash AM, Marcellus ML, Lopez JR, Marks MP (1999) Embolization of rolandic cortex arteriovenous malformations. Neurosurgery 44:479–486
Paulsen RD, Steinberg GK, Norbash AM, Marcellus ML, Marks MP (1999) Embolization of basal ganglia and thalamic arteriovenous malformations. Neurosurgery 44:991–997
Sala F, Beltramello A, Gerosa M (2007) Neuroprotective role of neurophysiological monitoring during endovascular procedures in the brain and spinal cord. Neurophysiol Clin 37(6):415–421
Sala F, Bricolo A, Faccioli F, Lanteri P, Gerosa M (2007) Surgery for intramedullary spinal cord tumors: the role of intraoperative (neurophysiological) monitoring. Eur Spine J 16(Suppl 2):S130–S139
Sala F, Niimi Y, Berenstein A, Deletis V (2001) Neuroprotective role of neurophysiological monitoring during endovascular procedures in the spinal cord. Ann NY Acad Sci 939:126–136
Sala F, Niimi Y, Krzan MJ, Berenstein A, Deletis V (1999) Embolization of a spinal arteriovenous malformation: correlation between motor evoked potentials and angiographic findings: technical case report. Neurosurgery 45(4):932–937
Sundt TM Jr, Sharbrough FW, Piepgras DG, Kearns TP, Messick JM Jr, O’Fallon WM (1981) Correlation of cerebral blood flow and electroencephalographic changes during carotid endarterectomy: with results of surgery and hemodynamics of cerebral ischemia. Mayo Clin Proc 56:533–543
Zentner J, Schumacher M, Bien S (1988) Motor evoked potentials during interventional neuroradiology. Neuroradiology 30:252–255
Acknowledgment
This study was kindly cooperated with Drs. C.G. McDougall, F.C. Albuquerque, and R.F. Spetzler, Barrow Neurological Institute, Phoenix, AZ, USA. Part of the funding was supported by the State Administration of Foreign Experts Affairs of China. There is no conflict of interests.
Author information
Authors and Affiliations
Corresponding author
Additional information
Comments
Johannes Sarnthein, Zurich, Switzerland
The present paper is one of few in the literature that report neurophysiological monitoring during endovascular procedures for cerebral aneurysms. In three patients, changes in evoked potentials were observed, which indicated risk of procedure-related morbidity. Consequently, treatment strategy was adapted, and no new postoperative deficits occurred. However, it will of course never be known whether neurological deficits would have actually occurred without adapting treatment strategy. In other patients, infarctions occurred in areas not covered by neuromonitoring and resulted in neurological deficits. Thus, as always, one has to (1) carefully select the potentials to be monitored and (2) define the conclusions that can be drawn from changes in potentials.
Gerasimos Baltsavias, Anton Valavanis, Zurich, Switzerland
Chen et al in their prospective study of 63 cases of neurophysiologic monitoring (NPM) during endovascular treatment of cerebral aneurysms aimed to assess the effectiveness and efficacy of NPM in detecting significant ischemia during such operations. In their report, it is not clear whether this population comprises of a consecutive series of patients or some inclusion–exclusion criteria were applied. Also, it is not mentioned the reason why MEPs were not employed.
NMP changes were seen in three patients during balloon remodeling, which led to immediate balloon deflation without postoperative clinical neurological deficit. On the other hand, in ten cases of abnormal angiographic findings, no NPM changes were detected. In eight of these cases, it is not clear whether no NPM changes were to be expected as the authors mentioned, whereas in the two other cases with severe angiographic complications, no NPM changes were detected as well. In total, five out of ten patients with angiographic complications developed clinical neurological deficit. None of them was detected in NPM.
Based on the above-described results, one should conclude that the NPM setup that the authors applied failed in 100% of cases to detect angiographically and clinically (confirmed by CT, MR) proved ischemia during endovascular therapy of aneurysms, whereas it is not clear if the three cases with NPM changes did not represent a false positive finding.
In conclusion and regardless of potential real benefit of NPM during neuroendovascular operations, we would say that evaluation of its efficacy should not be the goal of such a study. Otherwise, the effectiveness of the above-described setup was demonstrated very poor. Therefore it should be emphasized that according to the present study the decision-making during endovascular procedures cannot be based on NPM changes, but rather on the real-time and proper evaluation of the angiographic findings. Moreover, none intraoperative monitoring technique can substitute or reduce the value of the individualized approach and indication for treatment, combined with a non-aggressive technique and appropriate interpretation of the angiographic findings.
Rights and permissions
About this article
Cite this article
Chen, L., Spetzler, R.F., McDougall, C.G. et al. Detection of ischemia in endovascular therapy of cerebral aneurysms: a perspective in the era of neurophysiological monitoring. Neurosurg Rev 34, 69–75 (2011). https://doi.org/10.1007/s10143-010-0276-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-010-0276-3