Abstract
Introduction
To assess the management of immunocompetent patients with primary central nervous system lymphomas (PCNSL) in Spain.
Methods
Retrospective analysis of 327 immunocompetent patients with histologically confirmed PCNSL diagnosed between 2005 and 2014 in 27 Spanish hospitals.
Results
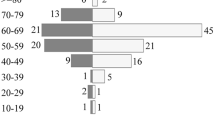
Median age was 64 years (range: 19–84; 33% ≥ 70 years), 54% were men, and 59% had a performance status (PS) ≥ 2 at diagnosis. Median delay to diagnosis was 47 days (IQR 24–81). Diagnostic delay > 47 days was associated with PS ≥ 2 (OR 1.99; 95% CI 1.13–3.50; p = 0.016) and treatment with corticosteroids (OR 2.47; 95% CI 1.14–5.40; p = 0.023), and it did not improve over the years. Patients treated with corticosteroids (62%) had a higher risk of additional biopsies (11.7% vs 4.0%, p = 0.04) but corticosteroids withdrawal before surgery did not reduce this risk and increased the diagnostic delay (64 vs 40 days, p = 0.04). Median overall survival (OS) was 8.9 months [95% CI 5.9–11.7] for the whole series, including 52 (16%) patients that were not treated, and 14.1 months (95%CI 7.7–20.5) for the 240 (73.4%) patients that received high-dose methotrexate (HD-MTX)-based chemotherapy. Median OS was shorter in patients ≥ 70 years (4.1 vs. 13.4 months; p < 0.0001). Multivariate analysis identified age ≥ 65 years, PS ≥ 2, no treatment, and cognitive/psychiatric symptoms at diagnosis as independent predictors of short survival.
Conclusions
Corticosteroids withdrawal before surgery does not decrease the risk of a negative biopsy but delays diagnosis. In this community-based study, only 73.4% of patients could receive HD-MTX-based chemotherapy and OS remains poor, particularly in elderly patients ≥ 70 years.


Similar content being viewed by others
References
Mendez JS et al (2018) The elderly left behind-changes in survival trends of primary central nervous system lymphoma over the past 4 decades. Neuro Oncol 20(5):687–694
Hoffman S, Propp JM, McCarthy BJ (2006) Temporal trends in incidence of primary brain tumors in the United States, 1985–1999. Neuro Oncol 8(1):27–37
Grommes C, DeAngelis LM (2017) Primary CNS lymphoma. J Clin Oncol 35(21):2410–2418
DeAngelis LM (1999) Primary central nervous system lymphoma [editorial]. J Neurol Neurosurg Psychiatry 66(6):699–701
Houillier C et al (2019) Radiotherapy or autologous stem-cell transplantation for primary CNS lymphoma in patients 60 years of age and younger: results of the intergroup ANOCEF-GOELAMS randomized phase II PRECIS study. J Clin Oncol 37(10):823–833
Kasenda B et al (2015) First-line treatment and outcome of elderly patients with primary central nervous system lymphoma (PCNSL)–a systematic review and individual patient data meta-analysis. Ann Oncol 26(7):1305–1313
Abrey LE, DeAngelis LM, Yahalom J (1998) Long-term survival in primary CNS lymphoma. J Clin Oncol 16(3):859–863
Chang SM et al (2005) Patterns of care for adults with newly diagnosed malignant glioma. JAMA 293(5):557–564
Fabbro-Peray P et al (2019) Association of patterns of care, prognostic factors, and use of radiotherapy-temozolomide therapy with survival in patients with newly diagnosed glioblastoma: a French national population-based study. J Neurooncol 142(1):91–101
Houillier C et al (2020) Management and outcome of primary CNS lymphoma in the modern era: an LOC network study. Neurology 94:e1027
Hoang-Xuan K et al (2015) Diagnosis and treatment of primary CNS lymphoma in immunocompetent patients: guidelines from the European association for neuro-oncology. Lancet Oncol 16(7):e322–e332
Porter AB et al (2008) Primary central nervous system lymphoma can be histologically diagnosed after previous corticosteroid use: a pilot study to determine whether corticosteroids prevent the diagnosis of primary central nervous system lymphoma. Ann Neurol 63(5):662–667
Binnahil M et al (2016) The influence of corticosteroids on diagnostic accuracy of biopsy for primary central nervous system lymphoma. Can J Neurol Sci 43(5):721–725
Haldorsen IS et al (2007) Increasing incidence and continued dismal outcome of primary central nervous system lymphoma in Norway 1989–2003: time trends in a 15-year national survey. Cancer 110(8):1803–1814
Enblad G et al (2017) Population-based experience on primary central nervous system lymphoma 2000–2012: the incidence is increasing. Acta Oncol 56(4):599–607
Eloranta S et al (2018) Increasing incidence of primary central nervous system lymphoma but no improvement in survival in Sweden 2000–2013. Eur J Haematol 100(1):61–68
Hart A et al (2014) Outcome of patients with primary central nervous system lymphoma treated outside clinical trials. Neth J Med 72(4):218–223
Fallah J, Qunaj L, Olszewski AJ (2016) Therapy and outcomes of primary central nervous system lymphoma in the United States: analysis of the National Cancer Database. Blood Adv 1(2):112–121
Shan Y, Hu Y (2018) Prognostic factors and survival in primary central nervous system lymphoma: a population-based study. Dis Markers 2018:7860494
van der Meulen M et al (2017) Improved survival in primary central nervous system lymphoma up to age 70 only: a population-based study on incidence, primary treatment and survival in the Netherlands, 1989–2015. Leukemia 31(8):1822–1825
Campo E et al (2011) The 2008 WHO classification of lymphoid neoplasms and beyond: evolving concepts and practical applications. Blood 117(19):5019–5032
Bessell EM et al (1996) Primary non-Hodgkin's lymphoma of the CNS treated with BVAM or CHOD/BVAM chemotherapy before radiotherapy. J Clin Oncol 14(3):945–954
Kuker W et al (2005) Primary central nervous system lymphomas (PCNSL): MRI features at presentation in 100 patients. J Neurooncol 72(2):169–177
Buhring U et al (2001) MRI features of primary central nervous system lymphomas at presentation. Neurology 57(3):393–396
Haldorsen IS et al (2009) CT and MR imaging features of primary central nervous system lymphoma in Norway, 1989–2003. AJNR Am J Neuroradiol 30(4):744–751
Izquierdo C et al (2016) Lymphomatosis cerebri: a rare form of primary central nervous system lymphoma. Analysis of 7 cases and systematic review of the literature. Neuro Oncol 18(5):707–715
Weller M (1999) Glucocorticoid treatment of primary CNS lymphoma. J Neurooncol 43(3):237–239
Haldorsen IS et al (2005) Diagnostic delay in primary central nervous system lymphoma. Acta Oncol 44(7):728–734
Bruck W et al (2013) Differential diagnosis of lymphoid infiltrates in the central nervous system: experience of the network lymphomas and lymphomatoid lesions in the nervous system. Pathologe 34(3):186–197
Cerqua R et al (2016) Diagnostic delay and prognosis in primary central nervous system lymphoma compared with glioblastoma multiforme. Neurol Sci 37(1):23–29
Burton EC et al (2017) A regional multicenter retrospective analysis of patients with primary central nervous system lymphoma diagnosed from 2000–2012: treatment patterns and clinical outcomes. Cureus 9(7):e1512
Abrey LE et al (2006) Primary central nervous system lymphoma: the memorial Sloan-Kettering cancer center prognostic model. J Clin Oncol 24(36):5711–5715
Ferreri AJ et al (2003) Prognostic scoring system for primary CNS lymphomas: the international extranodal lymphoma study group experience. J Clin Oncol 21(2):266–272
Xie H, Ahluwalia MS, Peereboom DM (2015) The Cleveland Clinic experience with primary central nervous system lymphoma. Am J Clin Oncol 38(2):140–146
Kiewe P et al (2008) Primary central nervous system lymphoma: monocenter, long-term, intent-to-treat analysis. Cancer 112(8):1812–1820
Graus F et al (2013) Patterns of care and outcome for patients with glioblastoma diagnosed during 2008–2010 in Spain. Neuro Oncol 15(6):797–805
Siegal T, Bairey O (2019) Primary CNS lymphoma in the elderly: the challenge. Acta Haematol 141(3):138–145
Ferreri AJM et al (2017) Whole-brain radiotherapy or autologous stem-cell transplantation as consolidation strategies after high-dose methotrexate-based chemoimmunotherapy in patients with primary CNS lymphoma: results of the second randomisation of the international extranodal lymphoma study group-32 phase 2 trial. Lancet Haematol 4(11):e510–e523
Correa DD et al (2019) Longitudinal cognitive assessment in patients with primary CNS lymphoma treated with induction chemotherapy followed by reduced-dose whole-brain radiotherapy or autologous stem cell transplantation. J Neurooncol 144:553
van der Meulen M et al (2018) Cognitive functioning and health-related quality of life in patients with newly diagnosed primary CNS lymphoma: a systematic review. Lancet Oncol 19(8):e407–e418
Acknowledgements
We thank all the institutions that made possible the review of the medical records. We thank CERCA Programme/Generalitat de Catalunya for institutional support.
GELTAMO (Grupo para el Estudio de Linfomas y Trasplante Autólogo de Médula Ósea): Department of Hematology. Catalan Institute of Oncologia-Hospital Duran i Reynals. IDIBELL Universitat de Barcelona. L’Hospitalet de Llobregat, Barcelona (Eva González-Barca), Department of Pathology, Hospital Universitari de Bellvitge, IDIBELL, L´Hospitalet, Barcelona (Fina Climent), Department of Oncology, Hospital Universitario y Politécnico La Fe, Valencia, Spain (Gemma Bruixola), Department of Hematology. Hospital Universitari Vall d’Hebron. Barcelona (Pau Abrisqueta), Department of Hematology. Hospital Universitario de Salamanca, Salamanca, Spain (Alejandro Martin García-Sancho; Míriam Lopez Parra), Department of Hematology. ICO-Hospital Universitari de Tarragona Joan XXIII. Universitat Rovira I Virgili, Tarragona, Spain. (Lourdes Escoda), Department of Hematology. ICO-Hospital Germans Trias i Pujol. Badalona (Marc Sorigué). GENOSEN (Grupo de Estudio de Neurooncología de la Sociedad Española de Neurología): Department of Neurology, Hospital Universitario La Fe, Valencia (Luis Bataller), Department of Neurology, Fundación Jimenez Diaz, Madrid (Raúl Córdoba), Department of Neurology, Hospital Universitario Miguel Servet, Zaragoza (Miguel González Sánchez), Department of Neurosurgery, Hospital Universitario Marqués de Valdecilla, Santander (Juan Martino), Department of Neurology, Hospital Rey Juan Carlos, Madrid (Javier Pardo-Moreno)
Funding
This work was partially supported by Grant PI1501303 from ISCIII and Fondo Europeo de Desarrollo Regional (FEDER).
Author information
Authors and Affiliations
Consortia
Contributions
RV, SM, NV, JB conceived and designed the analysis. RV,SM, NV, FG, MA, AM, IB, MJIJ, LB, SB, PA, RC, EG, PM, PC, AM, JM, JMS, IC, TLL, EE, LG, AS, AC, MS, JG, NH, JE, MB, NB, JP, RC, LE, ED, EGB, ID collected the data. RV, SM, JB, and ME performed the analysis. RV, SM, and FG wrote the paper.
Corresponding author
Ethics declarations
Conflict of interest
R.V. discloses membership on speaker bureau for Gilead and Novartis. A.S. discloses research funding and membership on advisory committees or speakers bureau for Roche, Celgene, Gilead or Janssen. F.G. holds a patent licensed to Euroimmun for the use of IgLON5 in an autoantibody test, for which he receives royalties, and receives honoraria from MedLink Neurology. The other authors declare no conflict of interest.
Ethical approval
The study was approved by the Institutional Ethical Committee of the coordinating center and, subsequently, by each participating center.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The members of the study GELTAMO and GENOSEN group are listed in acknowledgement section.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Velasco, R., Mercadal, S., Vidal, N. et al. Diagnostic delay and outcome in immunocompetent patients with primary central nervous system lymphoma in Spain: a multicentric study. J Neurooncol 148, 545–554 (2020). https://doi.org/10.1007/s11060-020-03547-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-020-03547-z