Neuroangiography is a safe and effective technique for evaluating various intracranial and extracranial disorders. The diagnostic information obtained by neuroangiography, combined with other clinical and noninvasive imaging findings, can be used to plan or evaluate results of treatment.
Participation by the angiographer in preprocedural selection, intraprocedural monitoring, and postprocedural follow-up and management of the patient is an integral part of neuroangiography and will increase the success rate of the procedure.
These guidelines have been written for use in institution-wide quality improvement programs to assess the practice of neuroangiography. The most important processes of care are 1) patient selection, preparation, and education; 2) procedural performance; and 3) patient monitoring. The outcome measures or indicators for these processes are indications, success rates, and complication rates. Outcome measures are assigned threshold levels.
Definition and Procedural Overview (1–3)
Neuroangiography is a process by which the intracranial and extracranial head and neck circulation is evaluated. (Spinal and selective intracranial angiography will be addressed in a separate document.) It consists of selective catheter placement into extracranial cervical vessels by using imaging guidance, followed by contrast material injection, to delineate anatomy. The catheter is usually inserted via a common femoral arterial access site, but other access sites (eg, axillary, brachial) may be used in selected cases. Aortic arch flush injections may be performed to delineate the origins and/or tortuosity of the extracranial cervical vessels prior to selective catheterization. However, unless severe occlusive disease prohibits safe selective catheterization, a selective study should be performed. Selective catheter placement optimally shows the extracranial and intracranial circulation and better defines occlusive morphology, tandem occlusive lesions, and coincident or contributory pathology. Evaluation of the intracranial circulation is an essential component of the angiographic study of occlusive extracranial cerebrovascular disease. The injection of contrast media must be at a rate and volume that safely and adequately opacifies the vascular territory of interest. Optimal positioning, magnification, and filming rates are necessary to provide sufficient information regarding the disease and vascular territory being studied. Several projections may be necessary to show the targeted area, but a minimum of two orthogonal projections is essential. Findings are acquired and stored either on conventional film or digitally on computerized storage media. Imaging and image recording must be consistent with the As Low As Reasonably Achievable (ALARA) radiation safety guidelines (2). Image-based diagnosis and treatment planning require integrating the angiographic findings within the context of the patient's history, physical findings, and prior imaging studies. Therefore, the neuroangiographer must be clinically informed and understand the specific questions to be answered by neuroangiography prior to the procedure in order to plan and perform the procedure safely and effectively.
The physician performing the neuroangiogram must fully appreciate the benefits, alternatives, and risks of the procedure. S/he must have a thorough understanding of extracranial and intracranial vascular anatomy (including congenital and developmental variants and common collateral pathways), the angiographic equipment, radiation safety considerations, physiologic monitoring equipment, and have access to an adequate supply of catheters, guidewires, and personnel to perform the procedure safely. The physician must understand the principles of prevention of thromboembolic phenomena with anticoagulation and catheter flushing, the need for adequate hydration, puncture-site hemostasis, and management of neuroangiographic complications. Furthermore, the performing physician must be able to detect and understand the clinical significance of unsuspected findings.
Although practicing physicians should strive to achieve perfect outcomes (eg, 100% success, 0% complications), in practice, all physicians will fall short of this ideal to a variable extent. Thus, indicator thresholds may be used to assess the efficacy of ongoing quality improvement programs. For the purpose of these guidelines, a threshold is a specific level of an indicator that should prompt a review. “Procedure thresholds” or “overall thresholds” reference a group of indicators for a procedure, such as major complications for selective neuroangiography. Individual complications may also be associated with complication-specific thresholds. When measures such as indications or success rates fall below a (minimum) threshold, or when complication rates exceed a (maximum) threshold, a review should be performed to determine causes and to implement changes, if necessary.
Thresholds may vary from those listed herein; for example, patient referral patterns and selection factors may dictate a different threshold value for a particular indicator at a particular institution. Thus, setting universal thresholds is very difficult and each institution is urged to alter the thresholds as needed to higher or lower values, to meet its own quality improvement program needs. The threshold for the following indications is 99%. When fewer than 99% of procedures are performed for these indications, the institution will review the process of patient selection.
Indications (3–10)
1) Define presence/extent of vascular occlusive disease and thromboembolic phenomena.
2) Define etiology of hemorrhage (subarachnoid, intraventricular, parenchymal, and craniofacial).
3) Define presence, location, and anatomy of intracranial aneurysms and vascular malformations.
4) Evaluate vasospasm related to subarachnoid hemorrhage.
5) Define presence/extent of trauma to cervicocerebral vessels (eg, dissection and pseudoaneurysm).
6) Define vascular supply to tumors.
7) Define presence/extent of vasculitis (infectious, inflammatory, and drug-induced).
8) Diagnose and/or define congenital or anatomic anomaly (eg, vein of Galen fistula).
9) Define presence of venous occlusive disease (eg, dural sinus, cortical, and deep).
10) Outline vascular anatomy for planning and determining the effect of therapeutic measures.
11) Perform physiologic testing of brain function (eg, Wada's test).
There are no absolute contraindications to adult diagnostic neuroangiography. Relative contraindications include iodinated contrast media allergy, hypotension, severe hypertension, coagulopathy, renal insufficiency, and congestive heart failure. Patient management should address these relative contraindications prior to the procedure. Patients with diabetes who are taking metformin (Glucophage) should discontinue its use at the time of angiography and for the following 48 hours until renal function has been assessed as adequate.
Success Rate (11–13)
A successful examination is defined as sufficient selective neuroangiographic technical evaluation and image interpretation to establish or exclude pathology of the extracranial and intracranial circulation. Successful neuroangiography for the evaluation of atherosclerotic disease is performed in one sitting but, rarely, repeated neuroangiography may be necessary owing to limitation of vascular access, contrast media dose limit, patient intolerance, inadequate anesthesia, or comorbid illness such as congestive heart failure, which obviates prolonged supine positioning. Evaluation of certain conditions, such as intracranial hemorrhage, may require multiple studies to define or exclude pathology. Success rate for neuroangiography is as follows: 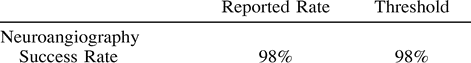 The rate of success is related to the patient's age, severity of atherosclerosis, and the presence of hypertensive disease.
The rate of success is related to the patient's age, severity of atherosclerosis, and the presence of hypertensive disease.
Complications (14–71)
The risks of neuroangiography are generally higher among patients of advanced age with severe atherosclerosis, pre-existing symptomatic cerebrovascular disease, acute subarachnoid hemorrhage, certain vascular dysplasias such as Ehlers-Danlos Syndrome, and possibly a history of migraine headache. The risks are related to the length of the procedure, number of catheter exchanges, catheter size, extent of catheter manipulation, and amount of contrast media used. Femoral introduction of the diagnostic catheter is considered safer than retrograde axillobrachial catheterization and direct carotid/vertebral puncture. Nonionic low-osmolarity contrast media are generally safer than ionic, high-osmolarity contrast media among patients with a previous history of contrast media hypersensitivity or nephropathy. The risk of contrast media–induced nephropathy is greater for patients with pre-existing acute or chronic azotemia, particularly in association with diabetes.
Neurologic
Neurologic complications that occur within 24 hours of the angiogram are, by definition, attributed to the angiogram and are defined by the duration and severity of the neurologic deficit (Table 1). A deficit lasting fewer than 24 hours is a transient ischemic attack (TIA). Deficits lasting longer than 24 hours are considered strokes. Strokes may be divided, based on reversibility, into reversible and permanent strokes. A deficit that resolves within 7 days is defined as a reversible stroke, and one lasting longer than 7 days is defined as a permanent stroke. Permanent strokes range in severity from trivial to life-threatening. In order to evaluate the outcome of patients after cerebral angiography, an objective measure of stroke severity should be made. The Modified Rankin Disability Score (Table 2) is easily performed and allows stratification of stroke severity that can be compared with patient status prior to angiography.
Neurologic complications
Modified Rankin Disability Scores
Non-neurologic
Non-neurologic complications can be stratified on the basis of outcome. Major complications result in admission to a hospital for therapy (for outpatient procedures), an unplanned increase in the level of care, resulting in prolonged hospitalization, permanent adverse sequelae, or death (Table 3). Minor complications result in no sequelae; they may require nominal therapy or a short hospital stay for observation (generally overnight) (Appendix A). The complication rates and thresholds below refer to major complications. Any death for which the onset of cause is within 24 hours of the procedure or a puncture-site infection should be reviewed as part of the institution-wide quality improvement program.
Major complications (non-neurologic)
Published rates for individual types of complications are highly dependent on patient selection and are based on series comprising several hundred patients, which is a volume larger than most individual practitioners are likely to treat. It is also recognized that a single complication can cause a rate to cross above a complication-specific threshold when, for example, the complication occurs in a small volume of patients early in a quality improvement program. In this situation, the overall procedure threshold is more appropriate for use in a quality improvement program.
Overall Procedure Threshold
All major complications resulting from Adult Diagnostic Neuroangiography … 2%.
This threshold refers to any complication that requires additional therapy, prolonged hospitalization, or causes permanent adverse sequelae, as defined in Appendix A.
Disclaimer
The clinical practice guidelines of the Society of Cardiovascular and Interventional Radiology, the American Society of Interventional and Therapeutic Neuroradiology, and the American Society of Neuroradiology attempt to define practice principles that generally should assist in producing high-quality medical care. These guidelines are voluntary and not intended to be rules. A physician may deviate from these guidelines, as necessitated by the individual patient and available resources. These practice guidelines should not be deemed inclusive of all proper methods of care or exclusive of other methods of care that are reasonably directed toward the same result. Other sources of information may be used in conjunction with these principles to produce a process leading to high-quality medical care. The ultimate judgment regarding the conduct of any specific procedure or course of management must be made by the physician, who should consider all circumstances relevant to the individual clinical situation. Adherence to the Quality Improvement Program will not assure a successful outcome in every situation. It is prudent to document the rationale for any deviation from the suggested practice guidelines in the departmental policies and procedural manual or in the patient's medical record.
Society of Cardiovascular & Interventional Radiology Standards of Practice Committee Classification of Complications by Outcome
Minor Complications
A. No therapy, no consequence.
B. Nominal therapy, no consequence; includes overnight admission for observation only.
Major Complications
C. Require therapy, minor hospitalization (<48 hours).
D. Require major therapy, unplanned increase in level of care, prolonged hospitalization (>48 hours).
E. Permanent adverse sequelae.
F. Death.
Reported complication-specific rates in some cases reflect the aggregate of major and minor complications. thresholds are derived from critical evaluation of the literature, evaluation of empirical data from standards of practice committee member practices, and, when available, the HI-IQ™ system national database.
Consensus on statements in this document was obtained utilizing a modified Delphi technique. (72, 73)
Footnotes
↵1 Technical documents specifying the exact consensus and literature review methodologies are available upon request from the Society of Cardiovascular & Interventional Radiology, 10201 Lee Highway Suite 500, Fairfax, VA 22030.
↵2 * Robert C. Wallace, MD, Co-Chair, ASITN and ASNR; Steven J. Citron, MD, Co-chair, SCVIR.
Curtis A. Lewis, MD; Robert C. Dawson, MD; Jacques E. Dion, MD; Allan J. Fox, MD; James V. Manzione, MD; Cynthia S. Payne, MD; Frank J. Rivera, MD; Eric J. Russell, MD; David Sacks, MD; Wayne F. Yakes, MD; Curtis W. Bakal, MD, MPH, participated on behalf of the Joint Standards of Practice Task Force of the Society of Cardiovascular and Interventional Radiology, the American Society of Interventional and Therapeutic Neuroradiology, and the American Society of Neuroradiology.
3 Address reprint requests to the American Journal of Neuroradiology, 2210 Midwest Rd, Oak Brook, IL 60521.
References
- Copyright © American Society of Neuroradiology






