Abstract
Summary: Xanthomas are associated with a spectrum of medical conditions, most commonly disorders of lipid storage and lipid metabolism. They occur primarily in the subcutaneous tissues, especially along the Achilles tendon and the extensor tendons of the hands. Intracranial xanthomas are extremely rare. We present a case of an extensive xanthoma of the temporal bone in a patient with hyperlipidemia.
Xanthomas are commonly characterized as granulomatous lesions (1) that usually occur among patients with hyperlipidemia, especially type II hyperlipidemia (2). They arise because of an excess of circulating serum lipids. Minor trauma plays an important role in the development of xanthomas. Therefore, they commonly occur along superficially exposed surfaces, such as the buttocks, elbows, eyelids, and hand creases (3). Xanthomas also frequently occur along the Achilles, patellar, and the hand extensor tendons (2). Small, yellow nodules representing lipid deposition in the eyelids (xanthelasma) and a hypopigmented circle of lipid deposition near the limbus of the cornea (corneal arcus) may develop (2). Although subcutaneous xanthomas are common, intracranial xanthomas have rarely been reported and are usually misdiagnosed. Although they are benign, intracranial xanthomas frequently progress and may cause cranial nerve deficits. We present the case of a patient with an extensive intracranial xanthoma associated with type II hyperlipidemia.
Case Report
A 31-year-old man presented in 1980 with right-sided facial pain and a watery discharge from his right nasal cavity and external auditory canal. A physical examination also revealed severe right-sided sensorineural hearing loss. The patient's medical history was remarkable for hyperlipidemia type II (serum cholesterol level above 500mg/dL), noninsulin-dependent diabetes mellitus, and coronary artery disease, for which the patient was being treated with lipid-lowering drugs and a cholesterol-restricted diet. A CT scan reportedly showed a large extra-axial mass in the right parietal region, which had been resected for biopsy, but the pathologic findings were inconclusive. No neoplasm was identified. The patient's nasal discharge resolved.
Five years later, the patient presented with right facial paresis. An unenhanced CT scan of the head showed an extra-axial right parietal and temporal bone mass that was hypodense to brain parenchyma. There was associated osseous remodeling of the parietal and temporal bones (Fig 1A–B). On MR images, the mass was heterogeneous in signal intensity and extended into the sphenoid sinus and nasopharynx (Fig 1C). The patient elected to have conservative management until 1992, when he again presented with recurrent symptoms leading to a second biopsy via a right canal wall up mastoidectomy. The pathologic findings, however, were again inconclusive.
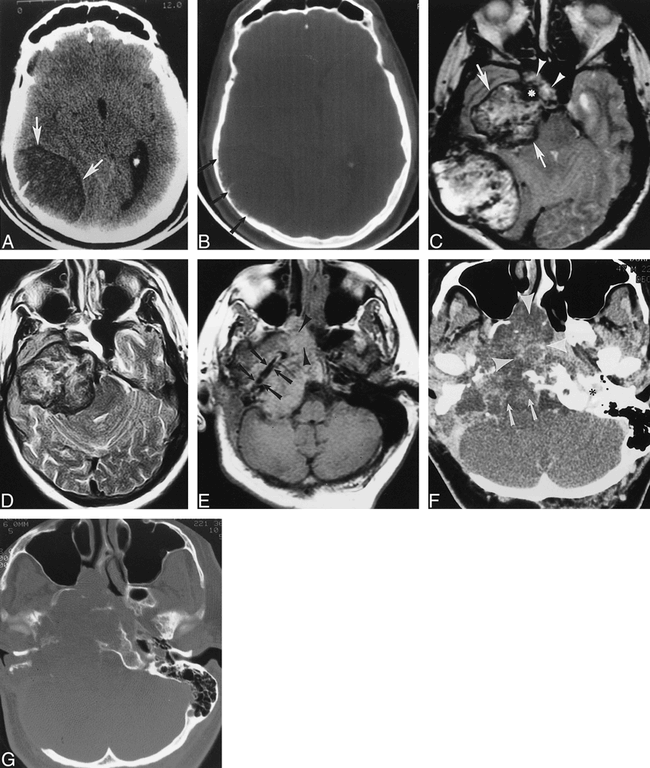
A–C, Axial unenhanced CT scan (A) shows hypodense extracerebral mass in right parietal region (arrows), and corresponding bone window (B) at the same axial level as A shows calvarial osseous remodeling and mild expansion (arrows). Axial T2-weighted (3500/85/2) MR image (C) shows extracerebral xanthoma with secondary bony expansion and remodeling. Mass is heterogeneous in signal intensity, with regions of hypointensity and involves petrous apex (arrows), extends into sphenoid sinus (arrowheads), and encases precavernous right internal carotid artery (ICA).
D–G, Images obtained 3 years after resection of extracerebral right parietal mass. Axial T2-weighted (3500/90/2) MR image (D) shows interval enlargement of lesion involving right temporal bone/petrous apex and extending from right petrous apex. Unenhanced axial T1-weighted (700/17/2) MR image (E) at skull base level shows encased right horizontal petrous ICA (arrows) and mass extending into sphenoid sinus and nasal cavity (arrowheads). Mass is hyperintense, consistent with its lipid content. Axial CT scan (F) at upper nasopharynx level shows mass' interval progression through skull base, involving clivus (arrows), jugular foramen (compare with uninvolved left side ;ob*;cb), and nasal choana and nasopharynx (arrowheads). Relative hypodensity of mass consistent with lipid content. Corresponding image (G) photographed for bone detail at level of F shows extensive bony destruction.
In 1993, the patient experienced progressive right facial and neck pain. A physical examination showed a right periauricular mass, xanthelasma, and incomplete right eyelid closure. Axial CT showed further progression of the mass. Occipital craniectomy and subtotal resection of the parietal portion of the mass were performed. Gross pathologic examination showed friable, yellow tissue. Histologic analysis revealed numerous lipid-laden macrophages and extracellular cholesterol clefts, suggesting the diagnosis of a xanthoma. The patient was stable postoperatively without progression of cranial nerve deficits. Follow-up MR imaging showed interval progression of the residual xanthoma (Fig 1D–G).
Discussion
Subcutaneous xanthomas typically occur in patients with heritable hyperlipidemia types I through V. Types I, IV, and V hyperlipidemia result from lipoprotein lipase deficiency as well as other glycoprotein abnormalities and are associated with hypertriglyceridemia and marked hypercholesterolemia. Types II and III hyperlipidemia are caused by biochemical abnormalities that result in excess circulating lipoproteins and moderately elevated serum cholesterol levels. Accelerated atherosclerosis frequently occurs, resulting in premature coronary artery disease and stroke. Existing hyperlipidemia may be exacerbated further by other conditions such as hypothyroidism and poorly controlled diabetes mellitus. Chronic uremia, nephrotic syndrome, and chronic alcoholism may increase plasma lipids (2). Abnormal lipid storage in the setting of normal serum lipids may occur in conditions such as histiocytosis X, leading to xanthoma formation (4).
Xanthomas develop because of lipid leakage from the vasculature into the surrounding tissues, where macrophages subsequently phagocytize these lipids. Because cholesterol is not degraded, it accumulates within these cells, creating “foamy” macrophages. The extracellular cholesterol crystallizes into clefts and induces an inflammatory reaction with giant cells and resultant fibrosis (1). Systemic xanthomas most commonly occur along the Achilles, patellar, and extensor tendons of the hands (2). They also occur along exposed surfaces, such as the buttocks, elbows, eyelids, and hand creases (3).
Intracranial xanthomas have been reported rarely among patients with hyperlipidemia, most commonly type II, which consists of several entities, such as polygenic hypercholesterolemia, combined familial hyperlipoproteinemia, and familial hypercholesterolemia. Family history, serum lipid profiles, and clinical findings may differentiate these disorders. Polygenic hypercholesterolemia is the most common and is thought to result from a combination of genetic and environmental factors. Familial hypercholesterolemias have a dominant inheritance pattern. Combined familial hyperlipoproteinemia occurs in 1% to 2% of the population and presents in the 3rd to 4th decade of life. It is usually not associated with xanthomas. Familial hypercholesterolemia arises from a reduced number of hepatic low-density lipoprotein receptors, leading to reduced low-density lipoprotein clearance from the blood. Subcutaneous and tendon xanthomas, xanthelasma, and corneal arcus are common manifestations (2).
Intracranial, extra-axial xanthomas have been described as occurring in the temporal bone (3–8), the skull base (clivus) (1, 8), and over the cerebral convexities. Most occur in middle-aged and elderly patients, although they have been reported in young patients (7, 9). Because of their slow progression, they tend to present late in life (3, 4, 6, 8). Clinical presentation depends on lesion location and extent. Symptoms may include severe headaches (1, 7, 9), otorrhea (6, 8), cranial nerve palsies, tinnitus (1–6, 8), otitis media, and otalgia (1).
Although the diagnosis of an intracranial xanthoma may be suggested by its imaging appearance, the diagnosis is usually not considered because of its rarity. Intracranial xanthomas are circumscribed, extra-axial masses that are hypodense to brain on unenhanced CT scans (1, 8). Nonetheless, isolated cases of xanthomas with heterogeneous density (6) or increased density with scattered calcifications (7) have been reported. Osseous abnormalities include bony destruction and remodeling (1, 3, 6, 8, 9). The MR imaging appearance of xanthomas is in part due to their high lipid content. On unenhanced T1-weighted images, most are hyperintense, with corresponding heterogeneous low signal intensity on T2-weighted images (1, 9), as in the current case (Fig 1). After the IV administration of contrast material, these lesions do not show significant enhancement (1, 10).
Although there is a spectrum of masses that may involve the temporal bone, more common lesions with an imaging appearance similar to that of xanthomas include epidermoids, cholesteatomas, and cholesterol granulomas. Epidermoids are epithelial inclusion cysts that may arise in the diploic space of the cranium, in the temporal bone, or as extra-dural masses. On CT scans, they are hypodense, expansile lesions with scalloped margins. On T1- and T2-weighted MR images, epidermoids follow the signal characteristics of CSF. On intermediate-weighted and fluid-attenuated inversion-recovery MR images, however, they are hyperintense to CSF. Histologically, epidermoids have keratin, which distinguish them from xanthomas (8).
Cholesteatomas are aggregations of keratin debris, resulting from an ingrowth of stratified squamous epithelium through a perforated tympanic membrane. Erosion of the middle ear ossicles and mastoid is common. These lesions are hypointense on T1-weighted images and are intermediate in signal intensity on T2-weighted images.
Cholesterol granulomas typically occur in a pneumatized petrous apex of the temporal bone among patients with a history of chronic otomastoiditis. A foreign-body reaction results in accumulation of giant cells, fibroblast proliferation, and cholesterol crystal deposition. On CT scans, these are expansile, lytic lesions. On MR images, hemorrhage-fluid levels may be present, and cholesterol granulomas are characterized by their marked hyperintensity on unenhanced T1-weighted images (11).
Although intracranial xanthomas are rare in the setting of familial hyperlipidemia, their identification is important, because successful control of serum lipid is required in their management (3). Pharmacologic agents used alone or in combination, as well as dietary limitation of saturated fats and cholesterol, are the basis of treatment of the underlying hyperlipidemia (3). Medical treatment includes bile resins, niacin, and statins that work indirectly to increase low-density lipoprotein receptors and reduce serum low-density lipoprotein levels (2, 3). Adequate dietary and medical management may cause the lesions to stabilize and, sometimes, to regress (3).
Conservative surgical resection is performed in most patients to debulk the lesion (1, 6–9). Surgery may offer relief or stabilization of symptoms, but the anatomic complexity of the region and the frequent occurrence of delayed diagnosis often complicate the procedures and prevent complete resection. Residual xanthoma may progress (6). Radiation therapy has rarely been used (4). The extensive involvement and the refractory nature of this lesion after both medical and surgical intervention emphasize the importance of the early diagnosis of this disorder. In our case, the patient's hyperlipidemia remained poorly controlled despite dietary and medical management. Postoperative imaging clearly shows xanthoma progression.
Footnotes
1 Supported by the RSNA Research and Education Fund Scholar Grant.
↵2 Address reprint requests to Laurie A. Loevner, MD, University of Pennsylvania Medical Center, Department of Radiology, 3400 Spruce Street, Philadelphia, PA 19104.
References
- Received June 9, 1999.
- Copyright © American Society of Neuroradiology