Abstract
Summary: We present a case of eclampsia complicated by alexia without agraphia. To our knowledge, this syndrome has never before been described in the literature.
The neuropathologic mechanisms for eclampsia are unclear. Cerebral vasospasm, hemorrhage, ischemia, edema, and encephalopathy have all been postulated (1). Cortical blindness and other disturbances of vision have been documented in cases of preeclampsia and eclampsia, and occipital lesions have been depicted by CT and MR imaging (1–4).
Case Report
A 33-year-old right-handed woman with factor V Leiden deficiency presented with the worst headache of her life. She was 6 days post partum following a vaginal delivery after prolonged labor. Low-molecular-weight heparin had been given throughout her pregnancy and was discontinued before induction of labor and then resumed after delivery. The immediate postpartum course was uncomplicated, and the patient was discharged home on warfarin and low-molecular-weight heparin. Headaches began 2 days post partum and gradually intensified.
On admission to the emergency room, the patient complained of a frontal throbbing headache. The blood pressure was 158/100 mm Hg. CT of the brain showed a faint right frontal cortical bleed with no midline shift or edema. Fresh frozen plasma was infused to reverse anticoagulation. The following morning, the patient complained of blurry vision. Neurologic examination revealed a mildly agitated, mildly encephalopathic woman. Her visual acuity and color vision were intact. There was a dense, right homonymous hemianopsia. The pupillary responses were normal, as were findings of the fundoscopic examination, which revealed flat optic discs bilaterally with no swelling and intact venous pulsations. The patient was unable to read most single letters and all words, but she was able to write words, which she was then unable to read. Ocular motility was full. The remainder of the neurologic examination revealed hyperreflexia and a right Babinski reflex.
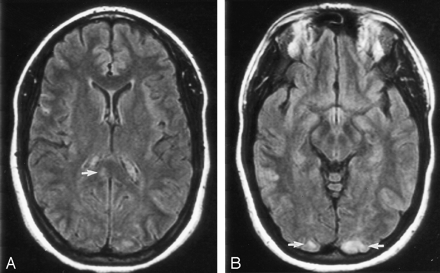
MR imaging performed at the time of the patient’s most profound visual deficits showed cortical hyperintensities on fluid-attenuated inversion recovery (FLAIR) images in the occipital cortex bilaterally, worse on the left, and also in the right side of the splenium of the corpus callosum, consistent with ischemia and petechial hemorrhage. (Fig 1) Similar lesions were observed scattered throughout both cerebral hemispheres, including the right frontal area seen on CT scan. Some of the lesions enhanced slightly. MR angiography and MR venography of the intracranial circulation were normal.
FLAIR images showing (A) lesion in the right side of the splenium of the corpus callosum and (B) bilateral occipital lesions.
The patient experienced vomiting and complained of worsening headache. Lumbar puncture performed on the same day revealed an opening pressure of 19 cm of water with a mild CSF pleocytosis of eight WBC (65% neutrophils, 35% lymphocytes). Findings of the remaining CSF studies were normal. Several hours later, the patient had a witnessed generalized seizure, and a magnesium infusion was started for a presumptive diagnosis of eclampsia.
Twelve hours later, the patient’s headache improved and she was able to read individual letters, but not words. Her visual field defect was moderately improved. Twenty-four hours later, her visual fields were full and she was able to read complete words easily. She admitted later to having vivid, unpleasant visual hallucinations of pillows puffing to enormous sizes, hairs growing out of the television, and “inverted letters” on signs hanging on walls. Magnesium sulfate was discontinued after 36 hours. A cerebral angiogram confirmed the normal cerebral vasculature without aneurysm or venous sinus thrombosis. Low-molecular-weight heparin was resumed, and the patient was discharged. On follow-up visit 2 weeks later, she reported that her vision was completely normal.
Discussion
Preeclampsia occurs in about 5% of deliveries, and of those cases, fewer than 10% develop eclampsia (2). The patient described here had many of the commonly recognized risk factors for eclampsia, including nulliparity, African-American ethnicity, and factor V Leiden syndrome, which has recently been linked to eclampsia and other complications of pregnancy (5, 6). Our patient demonstrated few of the laboratory findings typically associated with eclampsia, such as proteinuria and elevated liver enzymes; the relatively normal laboratory findings, while not necessarily unusual for eclampsia (3), contributed to some diagnostic uncertainty.
The visual complications of eclampsia and preeclampsia include blurred vision, papilledema, and cortical blindness (2). A Gerstmann syndrome was described in one patient (4). To our knowledge, the syndrome of alexia without agraphia has not been reported as a complication of eclampsia. This syndrome is typically due to an infarct in the left occipital lobe involving the splenium of the corpus callosum, thereby preventing the transfer of visual information from the intact left visual field across the corpus callosum to the angular gyrus in the left parieto-occipital cortex (7). The MR imaging findings in the case of our patient suggest that the syndrome was due to a combination of lesions in the occipital cortices and in the right side of the splenium of the corpus callosum. The presence of bilateral occipital lobe involvement suggests that the patient may have developed cortical blindness had her neurologic involvement from eclampsia progressed.
- Received March 28, 2003.
- Accepted after revision June 3, 2003.
- Copyright © American Society of Neuroradiology