Abstract
Summary: Serial evaluation of diffusion tensor brain fiber tracking was performed in a 27-year-old female patient with diffuse axonal injury after a traffic accident. Although the result of brain fiber tracking was not necessarily parallel to her clinical symptoms, it may have predicted the neurologic prognosis.
Diffuse axonal injury (DAI) refers to damage to the white matter caused by unequal rotation or deceleration or acceleration forces acting at the interface of tissues that differ in density or rigidity (1–3). These forces stretch and injure the axons, causing edema and axoplasmic leakage (1). These lesions are caused by shear strain deformation and are thus known as shearing injuries. Diffusion tensor imaging (DTI) is reported to be useful in detecting white matter damage, which is not prominent on anatomic T1- and T2-weighted images (4). Recently, brain fiber tracking by using DTI data has been applied to visualize the white matter tract of the brain (5, 6). In this report, we performed the serial evaluation of brain fiber tracking in a patient with DAI after a traffic accident. The result of brain fiber tracking was not necessarily parallel to clinical symptoms, but it may have predicted the neurologic prognosis.
Case Report
A 27-year-old woman sustained severe closed head injury in a traffic accident. When she was brought to the emergency room, she had spontaneous respiration, although she was unconscious. No eye opening was seen by pain stimulus. On CT scans obtained on the day of the accident, there was a small intraparenchymal hematoma in the right temporal lobe and parietal lobe, and there was a small hemorrhage in her right lateral ventricle.
Four days later, initial MR imaging, including DTI, was performed. Axial and sagittal trace diffusion-weighted (DW) images were also obtained. At that time, she was still unconscious, but slight eye opening was seen by the pain stimulation. Still, no verbal response was seen. For the best motor response, flexion to pain stimulation was seen (Glascow coma score; E2V1M3 = GCS 6) (7). On the first MR image, bilateral intraventricular hematoma, right subdural effusion, axonal injury of corpus callosum, and the right parietal hematoma were seen (Fig 1).
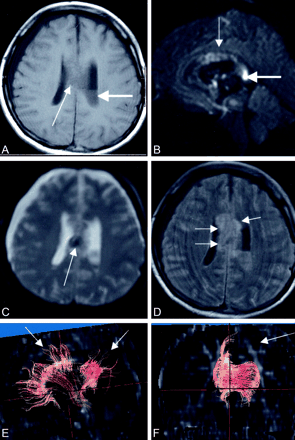
A 27-year-old woman 4 days after a traffic accident.
A, Axial T1-weighted image shows the intraventricular hemorrhage in left lateral ventricule (bold arrow) and right subdural effusion. A small hemorrhage in the corpus callosum is seen (thin arrow).
B, Sagittal trace DW image (b = 1000) shows areas of high signal intensity in corpus callosum (thin arrow), especially in the splenium (bold arrow).
C, Axial echo planar T2*-weighted image (b = 0 image from DTI sequence) shows a small hemorrhage in the corpus callosum as a low signal intensity area (arrow).
D, Axial FLAIR image shows high signal intensity area in the corpus callosum (arrows). No significant damage is seen in other white matter area.
E and F, Diffusion tensor fiber tracking from the seed area around the corpus callosum. Fibers are overlayed on FA map. The view from right side of the patient shows some fibers extending up to upper frontal and parietal white matter (E, arrows). On the frontal view, upward fibers in the left side are not seen (F, arrow).
Twenty-four days after the accident, she opened her eyes spontaneously, uttered incomprehensible sounds, and began to localize the pain stimulus (E4V2M5 = GCS 11). The second study of MR imaging, including DTI, was obtained. Again, axial and sagittal trace DW images were also obtained. Ventricular enlargement was prominent compared with the previous MR imaging study. The injury of corpus callosum was extended to a more frontal part compared with the previous study. Intraventricular hematoma was not seen at this time (Fig 2).
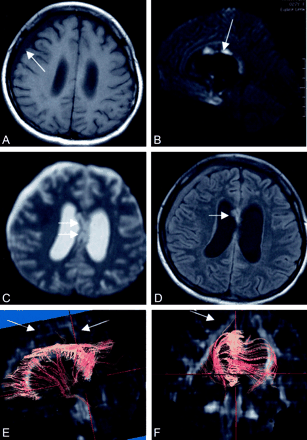
A 27-year-old woman 24 days after a traffic accident.
A, Axial T1-weighted image show slight enlargement of the lateral ventricules and right subdural bloody effusion (thin arrow).
B, Sagittal trace DW image (b = 1000) shows that the areas of strong high signal intensity in the corpus callosum have moved anteriorly compared with the first MR image (thin arrow).
C, Axial echo planar T2*-weighted image (b = 0 image from DTI sequence) shows no significant hemorrhage in the corpus callosum as a low signal intensity area (arrow).
D, Axial FLAIR image shows high signal intensity area in the anterior part of the corpus callosum (arrows). No significant damage is seen in other white matter areas.
E and F, Diffusion tensor fiber tracking from the seed area around the corpus callosum is shown. Fibers are overlayed on FA map. The view from right side of the patient shows almost no fibers extending up to the upper frontal and parietal white matter (arrows, E). On the frontal view, upward fibers in the right side have almost disappeared (arrow, F).
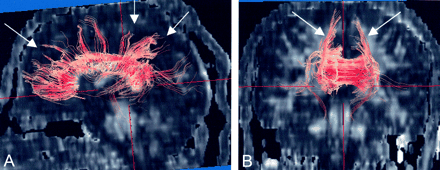
A 23-year-old male healthy volunteer for reference.
Diffusion tensor fiber tracking from the seed area around the corpus callosum. Fibers are overlayed on an FA map. The view from right side of the volunteer shows many fibers extending upward to frontal and parietal white matter from the corpus callosum (arrows, A). On the frontal view, upward fibers in the both side were visualized (arrows, B).
Two months after the injury, the third MR imaging study was performed. On anatomic scans, DW images, and diffusion tensor brain fiber tracking, no significant change was seen compared with the second MR imaging study. No significant improvement in her status was seen (E4V2M5 = GCS 11).
Diffusion tensor brain fiber tracking was performed for all DTI data. The seed area was set as the high signal intensity area of corpus callosum on midsagittal image of the sagittally reformatted fractional anisotropy (FA) map. On the first DTI data set, some fibers extending to right frontoparietal white matter were spared (Fig 1). On the second DTI data set, however, those fibers disappeared and no fiber extending to upper frontal and parietal white matter was seen (for reference, diffusion tensor brain fiber tracking data from 33-year-old male healthy volunteer is shown) (Fig 2). These data were obtained with the identical sequence parameters as the patient’s.
Imaging Parameters
All imaging was performed on a 1.5-T MR system (Symphony; Siemens AG, Erlangen, Germany) having a maximum gradient amplitude of 30 mT/m and slew rate of 125 mT/m/ms by using the eight-channel phased array head coils for signal intensity reception.
DTI was obtained by using the following parameters: Stejskal-Tanner sequence with single-shot spin-echo type echo-planar imaging, repetition time of 4000 ms, flip angle of 90°, echo time of 80 ms with b factor of 700 s/mm2. The echo spacing was 0.86 ms; bandwidth, 1158 Hz/ pixel; field of view, 23-cm; matrix, 128 × 128; and axial sections were 25–5 mm with a 1-mm intersection gap to cover the whole brain. The motion-probing gradient (MPG) in six orientations were applied following the acquisition of b = 0 images. The MPG orientation was defined as (x, y, z) = (1, 0, 1), (−1, 0, 1), (0, 1, 1), (0, 1, −1), (1, 1, 0), and (−1, 1, 0) for six directions. Imaging time was 3 minutes 16 seconds. The 128 × 128 data were zero-fill interpolated to a 256 × 256 matrix. The 128 × 64 points were recorded by using parallel imaging technique, generalized autocalibrating partially parallel acquisitions (GRAPPA) (8), which is an extension of the simultaneous acquisition of spatial harmonics (SMASH) technique (9). Although focal distortions near frontal sinus and temporal bone due to magnetic field inhomogeneity were seen, the eddy current-related image misregistrations between the images by each MPG direction were not prominent, so no distortion correction postprocessing was applied. Six signal averages of DT-MR imaging data were obtained with magnitude averaging.
Postprocessing for Fiber Tracking
DT-MR imaging data were transferred to an off-line windows PC with a Pentium 4 processor (2.8G Hz) and 1 GB of memory. Brain fiber tracking was performed by using the free software dTV (version 1.5) (University of Tokyo Hospital, Tokyo, Japan) for DT-MR imaging analysis.
The seed area was set as the region of interest drawn around the corpus callosum on the midsagittal image of the sagittally reformatted FA map. The target area was not set. Fiber tracking was stopped if the FA value was <0.18. Semiautomatic region definition is possible for corpus callosum by using the dTV software to apply the threshold on the FA map.
Evaluation of Fiber Tracking and Diffusion Tensor Data
For evaluation of callosal fiber visualization, the number of voxels in the seed area giving rise to a fiber track was calculated as a percentage of the total number of voxels in the seed area (%reached). Average FA values and apparent diffusion coefficient (ADC) values were measured for corpus callosum and the right and left frontal white matter 10-mm circular region of interest in the patient and volunteer data. The regions of interest in the bilateral frontal white matter were manually set on the section that is 12 mm cranial to the upper edge of corpus callosum. FA and ADC (mm2/s) values and %reached of the corpus callosum were as follows; 0.38, 1.08 × 10−3, and 84% on the first MR imaging examination of the patient; 0.35, 0.98 × 10−3, and 78% on the second MR imaging examination of the patient; and 0.52, 1.23 × 10−3, and 98% on the MR imaging examination of the volunteer subject. FA and ADC values of the right and left frontal white matter regions of interest were as follows; 0.34 (FA, right), 0.32 (FA, left), 0.92 × 10−3 (ADC, right), 0.96 × 10−3 (ADC, left) on the first MR imaging examination of the patient; 0.33 (FA, right), 0.32 (FA, left), 0.90 × 10−3 (ADC, right), 0.91 × 10−3 (ADC, left) on the second MR imaging examination of the patient; and 0.47 (FA, right), 0.46 (FA, left), 0.76 × 10−3 (ADC, right), 0.77 × 10−3 (ADC, left) on the MR imaging examination of the volunteer subject.
Discussion
Lesions of diffuse axonal injury are typically located at the gray matter-white matter interface or along or within fiber tracts, such as the centrum semiovale, internal capsule, corpus callosum, and the dorsal aspect of brain stem (1, 4). DAI is pathologically characterized by multifocal lesions, scattered in white matter, that are occasionally associated with petechial hemorrhage (1). Disruption of the cytoskeltal network and axonal membranes characterizes DAI in the first few hours after traumatic brain injury (4). White matter regions with reduced anisotropy are detected in the first 24 hours after traumatic brain injury by using diffusion tensor imaging. This reduction is often less evident 1 month after injury (4), although severity of brain fiber tracking findings increased 24 days after injury in this patient. DW images are reported to provide the additional information to T2-weighted and fluid-attenuated inversion recovery (FLAIR) images by detecting additional lesions (3, 10). In addition, DW images can differentiate degree of tissue injury extent and can potentially predict the injury reversibility, final outcome, and prognosis (2). In this particular patient, lesions in corpus callosum showed high signal intensity on DW images, and we could monitor the locational change of the lesion between the first and the second MR imaging examination.
In the present study, the corpus callosum was selected for the evaluation of diffusion tensor brain fiber tracking in the patient with diffuse axonal injury, although the corpus callosum is not the only tract damaged in the accident (2). The reasons we chose corpus callosum were as follows: 1) The corpus callosum can easily be extracted semiautomatically on sagitally reformatted FA map by using dTV software. This semiautomatic extraction can warrant high reproducibility, which is important for serial evaluation as performed in this study. 2) Fibers passing through the corpus callosum connect between the broad area of bilateral cerebral hemispheres. 3) The corpus callosum is one of the most frequently damaged fibers in DAIs. 4) Other tracts, except the corticospinal tract, are difficult to extract, especially with high reproducibility.
In the volunteer subject imaged in this report, many upward fibers from corpus callosum were extracted. These fibers were not seen on the second MR imaging examination of the patients. By the quantitative analysis, FA values of the corpus callosum were 0.52 and %reached was 98%, whereas those of the patient in the second examination were 0.35 and 84%. We cannot conclude this difference is significant from the results of only one patient and one volunteer subject, although quantitative analysis of diffusion tensor fiber tracking might be possible by using these parameters in the future.
Damage in the corpus callosum causes a variety of neurologic symptoms, such as hemialexia, unilateral agraphia, impaired dichotic listening performance, and unilateral apraxia (11–13). In this patient, even 4 months after the injury her consciousness level remains low. Thus, her callosal symptoms cannot be assessed.
Diffusion tensor brain fiber tracking is one method to visualize various tracts (5). Clinically, most reported results are limited to the corticospinal tract. The relation of the corticospinal tract and brain tumor or infarction is the first target of the research with fiber tracking (6). To the best of our knowledge, the report of brain fiber tracking in DAI is not seen.
In this patient, high signal intensity in the corpus callosum on DW images was seen even on the second MR imaging examination (24 days after injury). Usually, high signal intensity on DW images resolves within several days of the injury; however, the ADC reduction in this patient continued and high signal intensity area moved anteriorly. The reason for this is unknown, but late vascular occlusion might have happened because of hydrocephalus, resulting in new ischemic damage in the anterior part of the corpus callosum.
Conclusion
In this patient, findings of brain fiber tracking worsened during follow-up, although the patient’s symptoms gradually improved by the time point of the second MR image (24 days after injury). Three months after the second MR imaging examination, no significant recovery of her neurologic condition had been noted, compared with that at the second MR imaging examination. Thus, brain fiber tracking results might have showed some potential to predict the neurologic prognosis of this patient, although further study with a larger number of DAI patients is necessary to evaluate the predictive value of brain fiber tracking.
References
- Received November 10, 2003.
- Accepted after revision January 21, 2004.
- Copyright © American Society of Neuroradiology