Abstract
BACKGROUND AND PURPOSE: The purpose of this study was to compare obtained packing densities of aneurysms treated with the newly introduced GDC 360° coils with packing densities of aneurysms treated with either complex Orbit/Trufill coils or helical GDC 10 coils.
PATIENTS AND METHODS: Twenty-two aneurysms in 20 patients were coiled with GDC 360° coils. For each of the 22 aneurysms coiled with GDC 360° coils, 2 volume-matched controls treated with either complex Orbit/Trufill coils or helical GDC coils were identified from our data base. The packing of these matched controls was compared with the calculated packing of the 22 aneurysms treated with GDC 360° coils.
RESULTS: There was no difference in mean aneurysm volume between aneurysms treated with any of the 3 types of coils (P = .9). Mean packing of 22.1% of aneurysms treated with GDC 360° coils was significantly lower than mean packing of 30.3% of aneurysms treated with complex Orbit/Trufill coils (P = .0015). Mean packing of 22.1% of aneurysms treated with GDC 360° coils was not different from mean packing of 21.6% of aneurysms treated with helical GDC 10 coils (P = .81).
CONCLUSION: The use of complex-shaped GDC 360° coils does not lead to increased packing in comparison with that of helical GDC 10 coils. The use of complex Orbit/Trufill coils results in significantly higher packing than that of both GDC 360° coils and helical GDC 10 coils.
Approximately 25% of intracranial aneurysms treated with platinum coils show reopening of the lumen with time.1–2 Compaction of coil mesh (decrease of interspaces between the loops of the coils leading to a smaller coil mesh) is the most important contributing factor. One of the ways to prevent compaction is increasing the packing attenuation, defined as a ratio of inserted coil volume and volume of the aneurysm.3 Higher aneurysm packing can be obtained by inserting a higher volume of coils. The volume of inserted coils is dependent on both coil thickness and inserted coil length. In a previous study, we showed that packing is significantly higher in aneurysms treated with predominantly complex-shaped coils of 0.012-inch wire thickness (Trufill coils; Cordis, Miami Lakes, Fla) than in aneurysms treated with predominantly helical coils of 0.010-inch wire thickness (Guglielmi detachable coil [GDC 10 coils]; Boston Scientific, Fremont, Calif)4 and that higher packing led to lower reopening and retreatment rates.5,6 Another study showed that complex-shaped Trufill coils allowed better aneurysm filling than helical Trufill coils of the same wire diameter.7
Recently, a modification of the helical GDC coil, the GDC 360° (Boston Scientific), was introduced. This new coil has a complex shape intended to increase the packing of aneurysms. In this study, we compared the obtained packing densities of this GDC 360° coil with packing densities of volume-matched aneurysm controls treated with either complex coils (Orbit; Cordis) or helical GDC 10 coils.
Patients and Methods
Description of Coils
GDC 360° Coils.
GDC 360° coils are shaped in a double omega configuration (Fig 1). The first 1.5 loops are 25% smaller than the stated coil diameter to reduce herniation of the first loops into the parent artery. The double omega configuration assumes a more-or-less spheric shape on deployment. According to the company, GDC 360° coils have been developed to increase packing attenuation by “better confirmation to irregular aneurysm shape, concentric layering of coils and reduced compartmentalization.” GDC 360° coils are available in 0.010-inch (GDC 360° 10 Regular and Soft) and 0.018-inch wire thickness (GDC 360° 18) in diameters ranging from 2–24 mm.
GDC 360° coil.
Orbit/Trufill Coils.
Orbit coils are the evolution of the Trufill Detachable Coil System (Cordis) with a reduced detachment system profile to allow compatibility with 0.014-inch microcatheters. Orbit complex coils are shaped in a complex 3D configuration (Fig 2) and have a wire thickness of 0.012 inches. The complex shape has been developed to increase packing attenuation in the same way that the GDC 360° does. According to the company, the complex shape assures “random coil loops and breaks that seek out the true periphery of the aneurysm.” Available size range is 2–20 mm. The detachment mechanism is hydraulic.
Complex Orbit coil.
GDC 10 Coils.
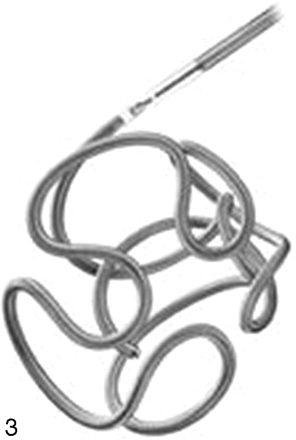
GDC 10 coils are helical coils with a wire thickness of 0.010 inches. GDC 10 coils are available in 3 softness grades (Regular, Soft, and Ultrasoft) in sizes ranging from 2–14 mm. GDC 10 coils are also available in a 3D shape (GDC 10 3D, Fig 3). According to the company, the GDC 3D coils are “intended to use as a first coil to obtain a framework bridging the neck of the aneurysm. Helical coils are subsequently inserted to fill the residual aneurysm lumen.”
GDC 10 3D coil.
Coiling Procedure
Coiling of aneurysms was performed by either of the 2 authors on a biplane angiographic unit (Integris BN 3000, Philips Medical Systems, Best, the Netherlands) with the use of general anesthesia and systemic administration of heparin. Intravenously or subcutaneously administered heparin was continued for 48 hours after the procedure, followed by 80 mg of aspirin daily for 3 months. The aim of coiling was to pack the aneurysm as densely as possible, until not 1 more coil could be placed.
Aneurysms Treated with GDC 360° Coils
Between November 2005 and January 2006, 22 aneurysms in 20 patients were coiled with GDC 360° coils. In 2 additional wide-necked aneurysms, a GDC 360° coil could not be delivered as a first coil, and both aneurysms were subsequently treated with complex Orbit coils.
There were 16 women and 4 men with a mean age of 53.3 years (median, 51.5 years; range, 37–77 years). Seventeen aneurysms had ruptured, 2 were in addition to another ruptured aneurysm, 2 were incidentally discovered, and 1 aneurysm presented with mass effect. The range of GDC 360° coils included GDC 10/360° for spiral diameters of 2–7 mm and GDC 18/360° for spiral diameters >7 mm. Seven aneurysms were coiled exclusively with GDC 360° coils. In the remaining 16 aneurysms, additional helical GDC 10 Soft and Ultrasoft coils were used. Overall, the proportion of inserted GDC 360° coil volume had a mean of 86% (median, 87%; range, 53%–100%). The volume of the 22 aneurysms was calculated from 3D angiographic datasets by using validated machine software.8 The volume of inserted coils was calculated with a spreadsheet containing volume per centimeter of coils for every coil type used. Packing of the aneurysms was calculated by dividing the volume of inserted coils by the volume of the aneurysm × 100%.
Matched Aneurysms Treated with Orbit/Trufill or GDC 10 Coils
For each of the 22 aneurysms coiled with GDC 360° coils, 2 volume-matched controls treated with either complex Orbit/Trufill coils or helical GDC 10 coils were identified from our data base containing 673 coiled aneurysms with known volumes and packings.4,5 Selection of the volume-matched controls was performed as follows: in case of a single exact volume match, this particular aneurysm was chosen. In case of more than 1 exact volume match, the aneurysm with the same location was selected. In case of 2 exact volume matches on the same location, the rupture status of the aneurysm was the decisive criterion. On the basis of these criteria, 22 pairs of aneurysms treated by either GDC 360° coils or Orbit/Trufill coils and 22 pairs of aneurysms treated by either GDC 360° coils or GDC 10 coils were identified. Of aneurysms treated with GDC 360° coils, 17 had ruptured; of aneurysms treated with Orbit/Trufill coils, 15 had ruptured; and of aneurysms treated with GDC 10 coils, 16 had ruptured.
With the use of GDC 10 coils, the first coil was generally a 3D coil followed by insertion of 1 or more helical coils. With the use of Cordis coils, all inserted coils were complex-shaped except for some 2- and 3-mm-diameter coils. In 1 of the aneurysms coiled with GDC 10 coils, a supporting balloon was used; in the remaining 65 procedures, no supporting device was used. The packing of the matched controls treated with GDC 10 coils and Orbit/Trufill coils was compared with the calculated packing of the 22 aneurysms treated with GDC 360° coils.
Statistical Analysis
Mean aneurysm volume and mean packing in the groups treated with GDC 360° coils, complex Orbit/Trufill coils, and GDC 10 helical coils were compared by using the t test. P values of <0.05 were considered statistically significant.
Results
Mean aneurysm volume of the 22 aneurysms treated with GDC 360° coils was 222.6 mm3 (median, 82.5 mm3; range, 13–1357 mm3). Mean aneurysm volume of the 22 aneurysms treated with Orbit/Trufill coils was 212.9 mm3 (median, 83 mm3; range, 13–1245 mm3). Mean aneurysm volume of the 22 aneurysms treated with GDC 10 helical coils was 225.9 mm3 (median, 81 mm3; range, 13–1377 mm3). There was no difference in mean aneurysm volume between any of the 3 groups (P > .9).
Mean packing of the aneurysms treated with GDC 360° coils, Orbit/Trufill coils, and GDC 10 helical coils was 22.1%, 30.3%, and 21.6%, respectively. SDs were 7.65, 8.33, and 5.65, respectively. The lower mean packing of GDC 360° coils versus Orbit/Trufill coils was statistically significant (P = .0015). The difference in mean packing between GDC 360° coils and GDC 10 helical coils was not significant (P = .81). The higher packing of Orbit/Trufill coils versus GDC 360° coils and GDC 10 helical coils was significant (P = .0015 and P = .0002, respectively).
Discussion
In this study, we found that the use of complex-shaped GDC 360° coils to treat intracranial aneurysms does not lead to increased packing in comparison with helical GDC 10 coils. The use of complex Orbit/Trufill coils results in significantly higher packing than that of both GDC 360° coils and GDC 10 helical coils. Although our study was not prospective and the number of patients was limited, the design of comparing packing of aneurysms treated with GDC 360° coils with that of matched controls of equal volumes provides meaningful results because aneurysm volume is the most important factor influencing packing.3
Apparently, for GDC coils, the modification from helical-to-complex shape does not lead to better aneurysm filling as was demonstrated for the modification from helical-to-complex shape for Cordis Orbit/Trufill coils.7 Although we cannot explain the lack of better performance of GDC 360° coils from small differences in complex-shape design with Orbit/Trufill coils, we have some possible explanations based on personal experience using the 3 types of coils. Using GDC 360° coils, we have the impression that loops of these coils have a tendency to move in a tumbling manner and more often herniate into the parent artery, that the tip of the microcatheter was more frequently pushed out of the aneurysm lumen, and that filling of the aneurysmal sac was less concentric than that with Orbit/Trufill coils. Re-entering the aneurysm with the microcatheter was frequently needed and sometimes difficult or impossible at a point where the aneurysm was not densely packed visually. With use of GDC 360° coils, we found the choice of size of the first coil to be more critical than that with Orbit/Trufill coils. Regularly, a GDC 360° coil with the same diameter as the aneurysmal sac could not be delivered, and consequently, this coil was wasted and replaced by a smaller diameter coil that sometimes did not cover the periphery and neck of the aneurysm. In contrast, Orbit/Trufill coils of equal or even larger diameter than that of the sac could generally be delivered easily with better peripheral aneurysm filling and neck coverage. In 2 of 24 aneurysms with attempted treatment with GDC 360° coils, it was impossible to place a 360° coil as a first coil because of repeated herniation of the coil into the parent artery and both aneurysms were treated with complex Orbit coils.
In conclusion, the use of complex-shaped GDC 360° coils does not lead to increased packing in comparison with helical GDC 10 coils. The use of complex Orbit/Trufill coils results in significantly higher packing than that of both GDC 360° coils and helical GDC 10 coils.
References
- Received February 24, 2006.
- Accepted after revision April 5, 2006.
- Copyright © American Society of Neuroradiology