Abstract
BACKGROUND AND PURPOSE: Intra-arterial chemotherapy for retinoblastoma has dramatically altered the natural history of the disease. The remarkable outcomes associated with a high safety profile have pushed the envelope to offer treatment for patients weighing ≤10 kg. The purpose was to determine the efficacy and safety of IAC infusions performed in infants weighing ≤10 kg with intraocular retinoblastoma.
MATERIALS AND METHODS: A retrospective chart review was performed for patients diagnosed with retinoblastoma and managed with intra-arterial chemotherapy.
RESULTS: The total study cohort included 207 retinoblastoma tumors of 207 eyes in 196 consecutive patients who underwent 658 intra-arterial chemotherapy infusions overall. Of these, patient weights were ≤10 kg in 69 (35.2%) and >10 kg in 127 (64.8%) patients. Comparison (≤10 kg versus >10 kg) revealed that the total number of intra-arterial chemotherapy infusions was 222 versus 436. Periprocedural complications were not significantly different (2 [0.9%] versus 2 [0.5%]; P = .49). Cumulative radiation exposure per eye was significantly lower in infants weighing ≤10 kg (5.0 Gym2 versus 7.7 Gym2; P = .01). Patients weighing ≤10 kg had a greater frequency of complete tumor regression (82.6% versus 60.9%; P = .02). Mean fluoroscopy time was not significantly different (7.5 versus 7.2; P = .71). There was a significant difference in the frequency of enucleation (16 [21.6%] versus 52 [39.1%]; P = .01). Patients weighing ≤10 kg had greater number of aborted procedures (12 [5.4%] versus 7 [1.6%]; P = .01). On multivariate analysis, weight ≤10 kg was not an independent predictor of complications or procedure failure.
CONCLUSIONS: Intra-arterial chemotherapy in patients weighing ≤10 kg is a safe and effective treatment.
ABBREVIATIONS:
- IAC
- intra-arterial chemotherapy
- ICRB
- International Classification of Retinoblastoma
- OA
- ophthalmic artery
- Rb
- retinoblastoma
Intra-arterial chemotherapy (IAC) for retinoblastoma (Rb) has dramatically altered the natural history of the disease. Cure rates, globe salvage, and vision preservation have dramatically increased.1⇓⇓⇓⇓⇓⇓⇓⇓-10 Yamane et al11 in 1989 described an IAC delivery technique termed selective ophthalmic artery infusion using a catheter-based approach with an inflated balloon that occludes the supraclinoid internal carotid artery segment distal to the ostium of the ophthalmic artery (OA). Then Abramson et al12 in 2008 refined the Japanese technique in which the ophthalmic artery was superselectively catheterized. Since then several specialized centers have incorporated ophthalmic artery catheterization into the treatment paradigm with the advantage of delivering a high drug concentration to tumoral tissue while maintaining low systemic concentration, thereby avoiding systemic complications.12 Moreover, treatment can be delivered in 1 day, and 2–3 sessions can be sufficient for tumor control.4,13,14 We have previously reported our 5-year experience with IAC.7,15,16 The remarkable outcomes associated with an acceptable safety profile—despite the risks (retinal toxicity)—and advancement in catheter techniques have pushed the envelope to offer treatment for patients weighing ≤10 kg. Weight <10 kg or age younger than 3 months have previously been exclusion criteria because of the perceived risk of femoral artery access complications.8,12 However, a case report and a small series have reported successful IAC delivery for infants weighing ≤10 kg.17,18 We herein describe our efficacy and safety outcomes in a large series of IAC infusions performed in infants weighing ≤10 kg.
MATERIALS AND METHODS
Cohort Creation
The study subjects included patients with unilateral or bilateral intraocular Rb undergoing IAC from February 2008 to June 2016. The population was dichotomized according to weight, ≤10 kg or >10 kg. The study protocol was reviewed and approved by the institutional review board. Informed consent was waived because of the retrospective design of this study. Ocular exclusion criteria were vitreous hemorrhage, secondary glaucoma, and extension of tumor into the optic nerve, uvea, anterior segment, or extrascleral compartments. Systemic exclusion criteria were history of blood dyscrasia or thrombotic events.
The patient data were retrospectively reviewed for demographic data, including age (months), sex (male, female), race (white, African American, Hispanic, Asian, Arab), hereditary pattern (sporadic, familial), and laterality (unilateral, bilateral). The presenting symptoms and prior treatment details were recorded. Tumor features included the largest basal diameter, thickness, and location and the presence of subretinal seeds and vitreous seeds. The IAC was delivered either as primary therapy in patients who had no previous treatment or as secondary therapy after failure of previous other types of treatment. Treatment-naïve eyes were classified according to the International Classification of Retinoblastoma (ICRB) (Philadelphia) as group A, B, C, D, or E.
Treatment Protocol
Parents and patients were informed of the risks of ophthalmic artery cannulation, and procedure consents were obtained.
Each patient was examined initially in the office and then under anesthesia with large fundus drawings, photographic documentation, and fluorescein angiographic analysis of all tumors and features in each eye. The decision for IAC was made in consultation with members of the Ocular Oncology Service, the Department of Neurosurgery, and the Department of Pediatric Oncology. Family history and medical history, particularly for thrombotic events, were obtained. This information was used to assess the need for screening tests looking for an increased risk of thrombosis, including factor V Leiden mutation, methylenetetrahydrofolate reductase mutation, and prothrombin 20–21–0 mutation.
At each 4-week follow-up, a detailed ophthalmic examination was performed by the treating ocular oncologist with photographic, fluorescein angiographic, and ultrasonographic documentation. The planned protocol was to deliver 3 sessions of IAC and after that judge whether further sessions would be necessary. Per protocol, adjunctive therapy, including laser photocoagulation, cryotherapy, plaque radiation therapy, or external-beam radiation therapy, was not delivered. If there was documented tumor recurrence or resistance, then these methods were potentially used.
During follow-up, each eye was assessed for regression of the solid tumor, subretinal seeds, vitreous seeds, and subretinal fluid. Tumor recurrence was documented. Other subsequent ocular treatment modalities were recorded.
Technical Procedure
After a parent or legal guardian consent, the IAC catheterization procedure was performed in the interventional neuroradiology suite under general anesthesia and continuous electro-physiological monitoring as an outpatient procedure. Anticoagulation with intravenous heparin (75 IU/kg) was delivered. All surfaces in the interventional neuroradiology suite in contact with the patient and all catheters were covered with plastic wrap, avoiding the use of cotton fiber material, including linen towels and patient draping material. After careful preparation of the puncture site in the groin, a 4F micropuncture needle was inserted into the femoral artery, and heparin was administered with a target activated clotting time between 200 and 300 seconds. Under fluoroscopic guidance, a Marathon microcatheter (Medtronic) and a Synchro 10 microwire (Stryker) were navigated all the way up from the groin to the ostium of the OA. The tip of the microcatheter was allowed to hook the ostium of the OA, without the aid of the microwire. A superselective injection was subsequently performed to confirm the position of the microcatheter and ascertain the lack of reflux into the internal carotid artery. If the Marathon catheter did not track, then a Prowler-10 microcatheter (Codman & Shurtleff) was used. If the latter approach was unsuccessful or if the OA was occluded, catheterization of the OA was alternatively performed through the middle meningeal artery collateral to the OA or by using the balloon-assisted technique. The balloon-assisted technique described by Yamane et al11 was used when there was a stenosis at the ostium and no good middle meningeal collateral.
Chemotherapeutic medications included melphalan and topotecan. The melphalan dose was 3, 5, or 7.5 mg, increasing with patient age and tumor size, without dosing higher than dose limit, which is 0.5 mg/kg. The topotecan dose was 1 mg. All patients received melphalan, and those with more extensive disease, particularly with vitreous seeding, were given additional topotecan. The microcatheter was subsequently flushed with saline to avoid crystallization of the agent in the OA, and angiograms were obtained to rule out thromboembolic complications. Repeat angiography through the microcatheter was performed immediately after the procedure to ensure the patency of the vessels, and the microcatheter was removed. At the end of the procedure, the heparin was reversed with intravenous protamine, and hemostasis was achieved with manual compression of the femoral artery done only by the senior author. The child was monitored for 6 hours before discharge. Oral aspirin (40 mg) was advised for 2 weeks, and topical ophthalmic application of antibiotic-steroid ointment and cycloplegic eye drops was recommended for 2 weeks. Each session of IAC was planned at a 4-week interval. A blood hemogram was performed at 2 weeks and 4 weeks after the procedure.
Outcome Variables
The population was divided into ≤10-kg and >10-kg cohorts. The primary outcomes analyzed were the frequency of periprocedural complications related to the IAC, complete tumor regression, and globe enucleation. Secondary outcomes assessed were the duration of the procedure, fluoroscopy time, mean radiation exposure per eye, cumulative radiation exposure, and procedure termination frequency. Globe preservation was considered as a favorable outcome.
Statistical Analysis
Categoric variables were summarized as absolute and relative frequencies and compared with the χ-square test, and continuous variables were presented as means and standard deviations and compared with the t test. A multivariate logistic regression model was developed to assess whether the weight of ≤10 kg was a potential predictor of periprocedural complications and procedure failures. For all tests, a P value < .05 was considered statistically significant. All analyses were performed with STATA software (version 14.1; StataCorp).
RESULTS
The total study cohort included 207 Rb tumors of 207 eyes in 196 consecutive patients who underwent 658 intra-arterial chemotherapy infusions overall. Of these, patient weights were ≤10 kg in 69 (35.2%) and >10 kg in 127 (64.8%) patients. Of the 69 patients weighing ≤10 kg, 5 patients received IAC treatment for bilateral Rb, and of the 127 patients weighing >10 kg, 6 patients received IAC treatment for bilateral Rb. Thus, a total of 74 eyes of 69 patients weighing ≤10 kg were compared with 133 eyes of 127 patients weighing >10 kg.
Patient Demographics
Comparison (≤10 kg versus >10 kg) revealed a significant difference of age at presentation of 10 months (median 9, range 1–33) versus 32 months (median 23, range 4–387) (P = .01), age at first IAC treatment of 11 months (median 10, range 3–30) versus 35 months (median 25, range 4–387) (P = .01), and weight at first IAC treatment of 8.4 kg (median 8.9, range 3.1–10.4) versus 16.4 (median 13.3, range 10.3–209) (P = .01). There was no difference in the distribution of sex proportions between groups: 36 male patients (52.2%) and 33 female patients (47.8%) versus 68 male patients (53.5%) and 59 female patients (46.5%) (P = .85). Also, no significant difference in race distribution was observed: 37 (53.6%) versus 59 (46.5%) whites; 12 (17.4%) versus 26 (20.5%) Asians; 11 (16.0%) versus 21 (16.5%) African Americans; 9 (13.0%) versus 12 (9.4%) Hispanics; and 0 versus 9 (7.1%) others (P = .31). There was no difference in family history of Rb among both groups: 4 (5.8%) versus 8 (6.2%) (P = .88).
Comparison (≤10 kg versus >10 kg) revealed no significant difference in genetic mutations: 31 patients (44.9%) versus 51 patients (40.2%) with somatic mutations; 20 patients (28.9%) versus 38 patients (29.9%) with germline mutations; 2 patients (2.9%) versus 0 patients with 13q deletion syndrome; and 16 patients (23.2%) versus 38 patients (29.9) with unknown status (P = .29). There was no difference in disease laterality: 55 patients (79.7%) versus 91 patients (71.7%) with unilateral involvement; 14 patients (20.3%) versus 36 patients (28.3%) with bilateral involvement (P = .21) or right and left eye involvement; 31 (41.9%) versus 66 (49.6%) right eye involvement; and 43 (58.1%) versus 67 (50.4%) left eye involvement (P = .19) (Table 1).
Intra-arterial chemotherapy for retinoblastoma in infants weighing ≤10 kg (74 treated eyes with 222 IAC sessions)—patient demographics
Tumor Features
Comparison of tumor characteristics (≤10 kg versus >10 kg) revealed no difference in greatest basal diameter: 15.0 mm (median 16, range 3–24) versus 16.0 mm (median 16, range 4–24) (P = .25). Patients weighing ≤10 kg had lower tumor thickness: 7.2 mm (median 6.5, range 1–17) versus 8.4 mm (median 8, range 1–22) (P = .04) and shorter tumor distance to the foveola 0.7 mm (0, 0–11) versus 2.4 mm (0, 0–15) (P = .01) and optic disc 0.8 mm (0, 0–8) versus 2.0 mm (0, 0–18). There was no significant difference in subretinal seeding: 30 eyes (40.5%) versus 51 eyes (38.3) (P = .75). Patients weighing ≤10 kg had a lower frequency of vitreous seeding: 18 eyes (24.3%) versus 70 eyes (52.6%) (P = .01). There was no significant difference in anterior chamber seeding: 0 (0.0%) eyes versus 1 eye (0.7%) (P = .45). Patients weighing ≤10 kg presented with less advanced Rb ICRB stage: 12 (16.9%) versus 5 (4.2%) with stage B, 9 (12.7%) versus 6 (5.0%) with stage C, 34 (47.9%) versus 58 (48.3%) with stage D, and 16 (22.5%) versus 51 (42.5%) with stage E (P = .01) (On-line Table).
Treatment Features and Periprocedural Complications
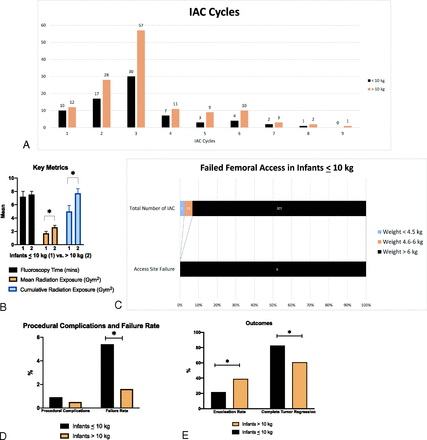
Comparison of treatment details (≤10 kg versus >10 kg) revealed that the total number of IAC infusions was 222 versus 436 (Fig 1A). There was no difference in primary, 38.0 eyes (51.3%) versus 66.0 eyes (49.6%), or secondary IAC treatment, 36.0 eyes (48.6%) versus 67.0 eyes (50.3%) (P = .85). There was no significant difference in number of IAC infusions per eye: 3.0 cycles (median 3, range 1–8) versus 3.3 cycles (median 3, range 1–9) (P = .26). There was no significant difference in the technique of IAC delivery by using selective OA catheterization: 206.0 (95.4%) versus 397.0 (92.9%) or an alternative approach such as balloon-assisted delivery: 6.0 (2.7%) versus 13.0 (3.0%) or middle meningeal artery 4.0 (1.9%) versus 17.0 (3.9%) (P = .65). There was a shorter procedure duration in infants weighing ≤10 kg: 47.5 minutes (median 42, range 6–156) versus 51.1 (median 48, range 7–200), but this was not statistically significant (P = .06). Mean radiation exposure per eye and cumulative radiation exposure per eye (Gym2) were both significantly lower in infants weighing ≤10 kg (1.7 ± 2.6, 95% CI 1.0–2.3 versus 2.6 ± 3.1, 95% CI 2.0–3.1; P = .02) and (5.0 ± 8.1, 95% CI 3.0–7.0 versus 7.7 ± 8.4, 95% CI 6.2–9.2; P = .01), respectively. Mean fluoroscopy time (in minutes) was not significantly different (7.5 ± 4.7, 95% CI 6.4–8.6 versus 7.2 ± 7.6, 95% CI 5.8–8.5; P = .71) (Fig 1B). Patients weighing ≤10 kg had a greater frequency of aborted procedures: 12 (5.4%) versus 7 (1.6%) (P = .01).
A, Bar graph showing the total number of IAC cycles per eye for infants weighing ≤10 kg and >10 kg. B, Bar graph showing the mean and standard error of fluoroscopy time (in minutes) and radiation exposure per eye (Gym2) of infants weighing ≤10 kg and >10 kg. Group 1: infants weighing ≤10 kg; group 2: infants weighing >10 kg. C, Bar graph showing the total number of IAC procedures and absolute value of failed femoral access in infants weighing ≤10 kg. Infants weighing <10 kg were subgrouped into 3 groups according to weight. D, Bar graph showing the percentage of periprocedural complications and failure rate of infants weighing ≤10 kg and >10 kg. E, Bar graph showing the enucleation rate and complete tumor regression of infants weighing ≤10 kg and >10 kg. Asterisks indicates significant difference.
Of aborted procedures in infants weighing ≤10 kg, 50% were because of inability to secure femoral artery access, but 70% of aborted cases in patients weighing >10 kg were because of a thrombosed OA. Infants weighing ≤10 kg were subgrouped into 3 groups according to weight: group 1, ≤4.5 kg; group 2, 4.6–6 kg; and group 3, >6 kg. The incidences of failed femoral access were 0 in the first 2 groups and 2.8% in the third group (P = .80) (Table 2 and Fig 1C). Of the 6 failed attempts, 5 had previous successful femoral access. The weight, age, and number of successful previous IAC attempts are presented in Table 3.
Intra-arterial chemotherapy for retinoblastoma in infants weighing ≤10 kg (74 treated eyes with 222 IAC sessions)—rate of femoral access failure in infants weighing ≤10 kg
Intra-arterial chemotherapy for retinoblastoma in infants weighing ≤10 kg (74 treated eyes with 222 IAC sessions—weight, age, and number of previous successful attempts for infants of failed femoral access
Periprocedural complications were not significantly different: 2 (0.9%) (vasospasm; 1 OA vasospasm after 5-cc infusion of the chemotherapy and 1 carotid vasospasm after straightening of a 360 carotid loop) versus 2 (0.5%) (1 incidence of ICA dissection by the microcatheter and 1 anaphylactic shock) (P = .49) (Fig 1D).
Outcomes
Comparison (≤10 kg versus >10 kg) revealed no difference in mean follow-up duration: 31.7 months (median 22.7, range 1.7–157.2) versus 30.0 (median 23.4, range 0.2–112.4) (P = .73). Patients weighing ≤10 kg had a greater frequency of complete tumor regression: 57 (82.6%) versus 81 (60.9%) (P = .02). Patients weighing ≤10 kg had lower frequency of enucleation: 16 (21.6%) versus 52 (39.1%) (P = .01) (Table 4 and Fig 1E).
Intra-arterial chemotherapy for retinoblastoma in infants weighing ≤10 kg (74 treated eyes with 222 IAC sessions)—clinical outcomes
Multivariate Analysis
By multivariate logistic analysis, weight ≤10 kg was not an independent predictor of procedural failure (OR: 1.24; 95% CI: 0.30–5.10, P = .75), nor an independent predictor of periprocedural complications (OR: 6.4; 95% CI: 0.63–65.6, P = .15).
DISCUSSION
Endovascular intra-arterial drug delivery is a promising field allowing for selective delivery of a high concentration of a therapeutic drug to selected targets. IAC for Rb stands as an inspiring example of the potential of selective drug delivery. IAC is a notable and established therapeutic option for Rb that has altered the natural history of the disease. Impressive cure rates have been reported, reaching 97%, with a dramatic drop in enucleation frequency (Fig 2).2,19-21 In a previous report of our 5-year experience with IAC, we found globe salvage rates of 100% for group B and C eyes,7 94% for group D eyes, and ≤73% for group E eyes with a combination of IAC and intravitreal chemotherapy.16 Most centers that use IAC for Rb have previously set treatment exclusion criteria for primary IAC of either weight ≤10 kg or age 3 months or younger, mainly because of the perceived risk of femoral artery complications in this group of patients. However, the importance of early treatment stems from data showing that younger and treatment-naïve patients may achieve better oncologic efficacy when they receive a minimal number of IAC cycles.6 Gobin et al22 showed that primary treatment with IAC was associated with an event-free survival rate of 81.7% after 2 years. Such a rate is much higher than 58.4% for eyes that had received intravenous chemotherapy or external-beam radiation in the pre-IAC era. Few reports exist in the literature on neuroendovascular approaches in infants and in particular on IAC treatment. Herein, we share our experience and report the safety and efficacy of IAC as a primary therapy for Rb in infants weighing ≤10 kg.
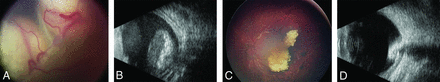
Retinoblastoma (A and B) before and (C and D) 9 months after treatment with intra-arterial chemotherapy (IAC). A, An infant presented with left eye leukocoria and unilateral group E retinoblastoma with no view of the optic nerve. B, B-scan ultrasonography demonstrated a calcified intraocular mass with overlying retinal detachment and no optic nerve involvement. C, After 4 IAC infusions using melphalan 5 mg and topotecan 1 mg, the tumor showed complete response with type III regression to a partially calcified mass in the macular region (D) confirmed by B-scan ultrasonography.
On review of our data (≤10 kg versus >10 kg), procedure duration (47.5 minutes versus 51.1 minutes, P = .06), fluoroscopy time (7.5 minutes versus 7.2 minutes, P = .71), cumulative radiation exposure per eye (5.0 Gym2 versus 7.7 Gym2; P = .01), percentage of aborted procedures (5.4% versus 1.6%, P = .01), percentage of periprocedural complications (0.9% versus 0.5%, P = .49), percentage of complete tumor regression (82.6% versus 60.9%, P = .02), and enucleation frequency (21.6% versus 39.1%, P = .01) speak to the safety and efficacy of IAC for infants ≤10 kg at a high-volume center. Vessel dissection was the only major complication that occurred in 1 patient weighing >10 kg. Multivariate analysis showed that weight ≤10 kg was not an independent predictor of complications or procedure termination. As expected, the frequency of failed procedures was significantly higher in infants weighing <10 kg, mainly because of inability to secure femoral artery access. Enucleation frequency in patients weighing <10 kg was significantly lower compared with those weighing >10 kg. Such outcomes highlight the fact that earlier treatment is associated with more favorable outcomes because of earlier stage of the cancer.
We previously reported a case of successful treatment of group D Rb with IAC in a subject weighing <6 kg. The subject received 2 cycles of IAC with 5 weeks in between and did well without adverse effects.18 Kim et al17 retrospectively analyzed outcomes of IAC for 11 Rb eyes in 6 patients whose average weight was 8.9 kg at the time of the first IAC. They reported excellent overall response to IAC with 100% globe salvage and minimal access site complications. They encountered 1 hospitalized case of severe neutropenia among 6 patients who developed chemotherapy-induced neutropenia. Chen et al23 retrospectively analyzed 10 patients who started IAC within their first 3 months of life, reporting that primary IAC was feasible for the treatment of Rb in that age group. Most (12/13) eyes were salvaged, and no signs of ischemia were reported. Interestingly, a recent animal model for Rb reported 100% success rate in rabbits that weighed 3.0–3.2 kg.24
IAC is a challenging procedure that requires an experienced neurointerventionalist competent in the cannulation of very small-caliber vessels in infants, an experienced anesthesia team, and well-prepared infrastructure. The procedure is not always straightforward because there are several technical, anatomic, and physiologic challenges. The minute caliber and fragility of access and target vessels is critical; therefore, sonography-guided femoral access is used for all procedures. In our series, we did not encounter any access site complications in either group. However, the small caliber of the femoral artery led to procedure termination in subjects weighing ≤10 kg at a frequency of 2.7% because of an inability to secure femoral access. However, it is paramount to know that femoral access is possible even in very young infants of 3 kg or age of 3 months. A low-profile 4F micropuncture kit may be used to gain access and used instead of a 4F pediatric sheath. In addition, a microcatheter may be used to complete the procedure without the use of a guide catheter. Sick infants in intensive care units receive a femoral line as a standard practice, and along the same line of thought, young infants eligible for IAC should not be denied the possibility based on weight or age alone. Eighty percent of the aborted IAC procedures due to failed arterial access had at least 1 successful attempt before. There was no incidence of procedure abortion in subjects weighing >10 kg because of vascular access. The main reason for procedure termination was OA thrombosis. On multivariate analysis, weight was not an independent predictor of procedure failure.
It is well established from the cardiac literature that larger sheath size relative to the femoral artery diameter is associated with higher rates of femoral artery complications (eg, vasospasm, thrombosis, and arterial disruption).25⇓-27 The 4F catheter has a diameter of 1.33 mm, which is larger than the size of the femoral artery in subjects weighing <10 kg. Reports of infants who underwent cardiac catheterization describe 8%–14% femoral artery injury leading to leg length discrepancy, with arterial thrombosis in one-third of cases.28⇓-30 Moreover, late arterial complications can occur because of catheter-induced endothelial damage. The senior author performs femoral artery compression at the end of the case for 20 minutes and monitors the arterial wave by using a pulse oximeter placed on the ipsilateral big toe. The philosophy is that too much compression may result in vessel damage, vasospasm, or limb ischemia, but poor compression may result in retroperitoneal hematoma, which may be disastrous in this age group. Also, the senior author has modified the IAC technique such that he no longer uses a guide catheter to avoid vessel dissection and to be able to downsize the groin sheath. Rather, catheterization is performed using a Marathon and a Synchro10 wire all the way from the femoral artery to the OA.
Limitations
Our study has the natural limitations of selection bias in a nonrandomized single-center study. Results have to be interpreted with caution, and conclusions should be validated in a larger population over a longer follow-up period. The strength of our study is a large number of procedures performed by the same group of neurointerventionalists in a single center.
CONCLUSIONS
IAC for Rb is a therapeutic approach that led to dramatic changes in the natural history of the disease. Cure rates, globe salvage, and vision preservation have significantly improved. The long, encouraging experience along with a high safety profile of IAC pushed the envelope to provide this patient population with such an alternative. Our results speak of the safety and efficacy of IAC in patients weighing ≤10 kg. Management should be tailored per patient, and variables such as age and weight should not be exclusion criteria to offer IAC.
Footnotes
Disclosures: Stavropoula Tjoumakaris—UNRELATED: Consultancy: Medtronic. Pascal Jabbour—UNRELATED: Consultancy: Microvention*; Grants/grants pending: Medtronic.* *Money paid to institution.
Data sharing statement: The relevant anonymized patient-level data are available on reasonable request from the authors.
References
- Received November 30, 2019.
- Accepted after revision April 14, 2020.
- © 2020 by American Journal of Neuroradiology