Abstract
BACKGROUND AND PURPOSE: Postdural puncture headache, a known complication of lumbar puncture, typically resolves with conservative management. Symptoms persist in a minority of patients, necessitating an epidural blood patch. One method of decreasing rates of postdural puncture headache is using atraumatic, pencil-point needles rather than bevel-tip needles. To the best of our knowledge, this is the first study comparing epidural blood patch rates between pencil- and bevel-tip needles with a subgroup analysis based on body mass index.
MATERIALS AND METHODS: This single-institution retrospective study identified 4435 patients with a recorded body mass index who underwent a lumbar puncture with a 22-ga pencil-tip Whitacre needle, a 20-ga bevel-tip Quincke needle, or a 22-ga Quincke needle. The groups were stratified by body mass index. We compared epidural blood patch rates between 22-ga pencil-tip Whitacre needles versus 22-ga Quincke needles and 22-ga Quincke needles versus 20-ga bevel-tip Quincke needles using the Fischer exact test and χ2 test.
RESULTS: Postdural puncture headache necessitating an epidural blood patch was statistically more likely using a 22-ga Quincke needle in all patients (P < .001) and overweight (P = .03) and obese (P < .001) populations compared with using a 22-ga pencil-tip Whitacre needle. In the normal body mass index population, there was no statistically significant difference in epidural blood patch rates when using a 22-ga pencil-tip Whitacre needle compared with a 22-ga Quincke needle (P = .12). There was no significant difference in epidural blood patch rates when comparing a 22-ga Quincke needle versus a 20-ga bevel-tip Quincke needle in healthy (P = .70), overweight (P = .69), or obese populations (P = .44).
CONCLUSIONS: Using a 22-ga pencil-tip Whitacre needle resulted in lower epidural blood patch rates compared with a 22-ga Quincke needle in all patients. Subgroup analysis demonstrated a statistically significant difference in epidural blood patch rates in overweight and obese populations, but not in patients with a normal body mass index.
ABBREVIATIONS:
- BMI
- body mass index
- EBP
- epidural blood patch
- LP
- lumbar puncture
- PDPH
- postdural puncture headache
- 20Q
- 20-ga bevel-tip Quincke needle
- 22Q
- 22-ga bevel-tip Quincke needle
- 22W
- 22-ga pencil-tip Whitacre needle
The lumbar puncture (LP), first introduced in the late 1800s, is a common and critically important minimally invasive procedure performed across varied medical specialties. Most commonly performed as a diagnostic procedure to obtain CSF for laboratory testing, LPs are also performed for myelography and various therapeutic applications.1 The risk of severe complications associated with LP is low; however, minor complications are frequently encountered in clinical practice, the most common being a postdural puncture headache (PDPH).2,3 Characteristics of PDPH commonly include positional exacerbation in the upright position. Patients may also experience neck stiffness, nausea, vomiting, hearing loss, tinnitus, vertigo, visual disturbances, and paresthesia. In severe cases, symptoms can include cranial nerve palsies and seizures.1
The cause of PDPH is believed to be secondary to leakage of CSF from the dural defect created by the needle during the LP.1,4,5 There are several accepted noninvasive strategies and treatments to alleviate PDPH; however, the most common invasive treatment is the epidural blood patch (EBP).6,7 An EBP requires the patient to undergo another procedure during which a sterile blood draw is performed and subsequently injected into the patient’s epidural space to mitigate the leakage of CSF from the dural defect. No current consensus exists for the optimal amount of autologous blood to introduce into the epidural space, with the maximum volume dependent on the patient’s tolerance. This supplementary procedure for treating PDPH not only carries additional risks of complications, including temporary worsening of headache, infection, low back pain, and radicular pain, but also results in increased cost to the patient and institution.1
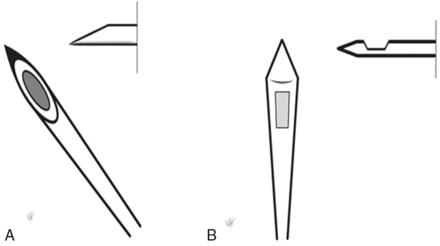
Numerous studies have been conducted to identify the factors related to the increased incidence of PDPH.5,8⇓-10 Needles with pencil-point atraumatic tips have been shown to decrease the rates of PDPH compared with conventional needles with a sharp bevel tip (Figure).1,5,8⇓-10 Additional identified predisposing factors for PDPH include female sex, prior PDPH, and needle size.4,9,11 The impact that body mass index (BMI) has on rates of PDPH is unclear, with prior studies providing evidence that a higher BMI may be protective.9,12
A, A conventional needle with a sharp bevel tip has a cutting tip with the needle orifice incorporated within the tip. B, A pencil-point atraumatic tip has a blunt tip. The orifice is not directly continuous with the tip but rather adjacent to it.
This study highlights our experience with >4400 patients and, to our knowledge, is the first study that compares the incidence of EBP with needle type when stratified for BMI. The objective of this study was to compare EBP rates between pencil- and bevel-tip needles with a subgroup analysis based on BMI.
MATERIALS AND METHODS
Patients and Clinical Data
A single-institution retrospective review was conducted as a quality-improvement project. A Montage (Montage Healthcare Solutions) search for fluoroscopy-guided LP within the radiology department between January 2009 and January 2017 yielded 4854 patients, including inpatient, outpatient, and emergency department referrals. Among these patients, 146 patients were excluded secondary to different needle types or sizes, 110 patients were excluded secondary to unknown needle type or size, and 163 patients were excluded secondary to lack of an available BMI. The total number of patients meeting the inclusion criteria that required EBP within 10 days of the LP was 127.
As per AdventHealth institutional policy, radiologists performed all lumbar punctures under fluoroscopic guidance. No formal criteria existed to determine the use of a Whitacre or Quincke needle, and the needle use was determined by the radiologist’s preference. After the procedure, before discharge, all patients were placed on 1- to 2-hour bed rest with the head of the bed flat. Patients were instructed to drink fluids and refrain from strenuous activity for 24 hours. If patients developed intractable headaches that persisted longer than 48 hours, they were encouraged to call the department for EBP evaluation, at which time the procedure, risks, and benefits would be discussed in detail.
Patients were first stratified on the basis of the needle type used for the procedure, which included the pencil-point tip 22-ga Whitacre (22W) needle (Becton Dickinson Medical) and the sharp bevel-tip 22-ga Quincke (22Q) and 20-ga Quincke (20Q) needles (Becton Dickinson Medical). Further stratification among each group was conducted on the basis of BMI, including normal (BMI ≤ 25), overweight (BMI, 25 to ≤30), and obese (BMI >30). The rates of EBP were determined for each group and compared for 22W versus 22Q, and 22Q versus 20Q.
Statistical Analysis
Numeric variables were summarized as mean (SD). Categoric variables were summarized as frequency (%). A Wilcoxon Mann-Whitney test was used to compare the EBP for numeric variables (BMI) in Table 1. The Kruskal-Wallis test was used to test the BMI among needle type/size groups in Table 2. Multiple logistic regression was used to predict EBP with BMI and needle type/size controlled in Table 3. The χ2 test was used to compare the EBP for the normal BMI categoric variables in Table 4. The Fisher exact test was used to compare the EBP for the overweight/obese categoric variables in Table 4. All analyses were performed at a significance level of 5% using SAS 9.4 (SAS Institute).
Characteristics of study cohorta
Association of LP needle type and patient’s BMI
Multiple logistic regression to predict EBP (n = 4435)
EBP numeric value outcome of each needle type with respect to the BMI subgroup
RESULTS
Characteristics of Study Cohort
Table 1 lists the characteristics of patients in our study cohort with regard to EBP use/lack of EBP use. There was no difference in EBP rates when factoring for BMI alone. Needle type impacted the rate of EBP and was lower in the 22W versus 22Q (P < .001) and 22W versus 20Q (P < .001).
Association of LP Needle Type and Patient’s BMI
Table 2 reports an association with the patient’s BMI and needle type, with the average BMI of patients in the 22W lower than that in the 22Q/20Q groups (P < .001); thus, there was a propensity in this study to use Quincke needles in larger patients.
Comparison of Needle Type EBP Rates with BMI Controlled
Table 3 indicates the rates of EBP for each needle type when the BMI was controlled. Results show that there was an association of increased rates of EBP when using the 22Q compared with the 22W. The odds ratio of the EBP rate for the 22W compared with the 22Q was 0.34 (95% CI, 0.20−0.58; P < .001), indicating that the use of the Whitacre needle was associated with lower rates of EBP compared with the use of a Quincke needle. The odds ratio of the EBP rate for the 20Q compared with the 22Q was 1.21 (P < .001) (95% CI, 0.77−1.9), indicating no association of higher rates of EBP between 20- versus 22-ga Quincke needles.
Comparison of Needle Type EBP Rates Based on BMI Subgroup
The 22W resulted in lower rates of EBP compared with 22Q in the overweight (BMI, 25 to ≤30) and obese (BMI > 30) populations (P = .03 and P < .001, respectively). There was no statistically significant difference among patients with normal BMIs (P = .12). No difference existed in the rates of EBP within each subgroup between the 22Q and 20Q.
DISCUSSION
While multiple studies have shown the superiority of pencil-point needles in reducing the incidence of PDPH,1,5,8⇓-10 the rates of EBP between needle type and BMI stratification have not been evaluated. The results of this study show that the use of a pencil-point needle reduces the rates of EBP despite the perceived technical difficulties in the overweight and obese populations. When controlling for BMI, the rates of EBP were lower when using the 22W compared with the 22Q, a finding consistent with that of Hatfield et al.13 Although there was a trend toward lower EBP rates among patients with normal BMIs using the 22W compared with the 22Q, there was no statistically significant difference. This could be an area of future study.
At our institution, needle selection was determined on the basis of the radiologist’s preference, resulting in increased Quincke use in the obese population. One reason may be due to the physician’s preference because the Quincke needle is more maneuverable, making it advantageous in the technically challenging heavier patient populations. However, the most likely explanation is that our institution supplied the Whitacre needle in only the 3.5-inch size, and the longer sizes were not available at the time of this study. This inherent preference resulted in a relatively larger number of Quincke needles used in the overweight/obese population, and a relatively smaller number, in normal-weight patients. Since performing this study, our radiology group has stocked the longer Whitacre needle sizes.
Several studies reported predisposing factors that lead to PDPH, including a history of PDPH and female sex.4,9,11 Other potential predisposing factors are a difficult LP, which may result in multiple dural punctures and increased fluoroscopy times. The limitations of this study are that these factors were not analyzed to determine whether a difference occurred between our subgroups and whether possible confounding variables could have occurred.
This study showed no difference in the rates of EBP between the 20Q and 22Q when the BMI was not controlled or within the BMI subgroups. This finding differed from the study performed by Hatfield et al,13 which showed that the use of a 20Q resulted in overall increased rates of EBP. The cause of this discrepancy is unclear, but generally, larger needles result in greater rates of PDPH,11,14,15 which is believed to be secondary to larger defects in the thecal sac; thus, we recommend the use of smaller-bore needles. The greatest limitation of this study was the retrospective design. Additionally, the lumbar punctures were performed by both board-certified radiologists and radiology residents under direct supervision.
CONCLUSIONS
Our study supports prior evidence that pencil-tip atraumatic needles reduce the rate of PDPH necessitating treatment with an EBP compared with sharp bevel-tip spinal needles. A subgroup analysis suggests that pencil-tip atraumatic needles should be used in overweight and obese populations despite their potentially inherent technical disadvantages. In patients with normal BMIs, there was an observed trend toward lower EBP rates using pencil-tip atraumatic needles, though this was not statistically significant.
Acknowledgment
We would like to thank the biostatisticians Jiajing Wang and Yuan Du for their help with the statistical analysis.
References
- Received October 16, 2020.
- Accepted after revision November 10, 2021.
- © 2022 by American Journal of Neuroradiology