Abstract
Summary: Persistent primitive lateral vertebrobasilar (PPLVB) anastomosis is a rare remnant of early fetal development whose occurrence, to our knowledge, has been reported only once. We now report a new variant in which the basilar artery was fed primarily by a PPLVB anastomosis because on one side the vertebrobasilar junction was incompletely developed and on the other it was aplastic. Aneurysmal rupture in this case may be attributable to excessive hemodynamic stress.
Fenestration and duplication are the unusual variations and configurations of previously reported intracranial vertebrobasilar systems (1–8). Remnants of a primitive vertebrobasilar anastomosis can result in rare duplications of the vertebrobasilar junction (2, 3, 5, 7, 8). The long tract of this rare anomalously persistent vessel was named persistent primitive lateral vertebrobasilar (PPLVB) anastomosis by De Caro et al (3). We now report a new variant in which the basilar artery (BA) was fed primarily by a PPLVB anastomosis.
Case Report
This 62-year-old man was admitted with sudden and transient loss of consciousness. He had undergone percutaneous transluminal coronary angioplasty for myocardiosclerosis 10 years earlier. On admission, he was alert but suffered severe headache and recurrent vomiting. Neurologic examination disclosed no deficits.
A CT scan revealed subarachnoid hemorrhage (SAH), and the patient underwent emergent four-vessel angiography. Bilateral carotid angiograms disclosed no anomalies. The left vertebral artery (VA) terminated at the posterior inferior cerebellar artery (PICA) (Fig 1) and the basilar artery (BA) was fed via an anomalous artery, recognized as a PPLVB anastomosis arising from the right VA. It passed laterally in parallel with the basilar trunk and connected vertically with the middle of the trunk at the level of the origin of the left anterior inferior cerebellar artery (AICA) (Fig 2). The BA was fed from the caudal and the cranial direction from the basilar-PPLVB anastomosis juncture; the flow was antegrade in the upper trunk and retrograde in the lower trunk. No normal junctions of the right VA and BA were demonstrated. There was a saccular aneurysm at the left basilar AICA contralateral to the basilar-PPLVB anastomosis jointure.
Left vertebral angiogram, lateral view. The left VA terminates at the PICA.
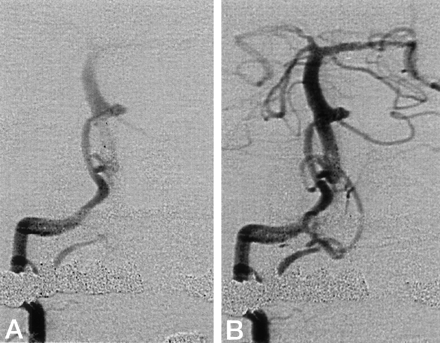
Right vertebral angiogram.
A, Early arterial phase.
B, Late arterial phase.
No normal vertebrobasilar junction is visualized. The BA is fed only via the PPLVB anastomosis. Flow is into the upper and lower BA via the BA-PPLVB anastomosis jointure. Note the saccular aneurysm at the left basilar anterior inferior cerebellar artery.
The patient underwent successful endovascular embolization of the aneurysm via the PPLVB anastomosis. He was discharged without any neurologic deficit.
Follow-up angiograms, obtained approximately 4 months later, again confirmed complete obliteration of the aneurysm. While the BA was primarily fed through the PPLVB anastomosis, 3D angiograms confirmed flow from the right VA to the BA (Fig 3). Some flow was delivered via anomalous, thin, meandering vessels that were duplicated at the level of the lower BA (Fig 4).
Schematic representation of the vertebrobasilar system. The arrows indicate the anomalous flow. The PPLVB anastomosis supplies most of the basilar artery flow with some flow delivered by anomalous, thin, hypoplastic arteries (asterisk).
Right vertebral angiogram depicting the vertebrobasilar system.
A, Digital subtraction angiogram in the anteroposterior view.
B, Three-dimensional angiograms in the left posterolateral oblique and posteroanterior view. Note the two indirect connections between the BA and the left VA, one through the PPLVB anastomosis, and the other through thin, serpentine arteries.
Discussion
Fenestration and duplication are documented vertebrobasilar system anomalies (2, 3, 5, 8) with some types of fenestration or duplication occurring at the vertebrobasilar junction (Fig 5). They derive from different fetal origins between the BA and the VA or the vertebobasilar junction.
Schema of fenestration or duplication in intracranial vertebrobasilar systems.
A, Basilar fenestration.
B, Duplication of the VA.
C, Premedullary duplication of the VA.
D, PPLVB anastomosis.
As shown in Figure 5A, the BA develops from the fusion of the primitive longitudinal neural artery. Incomplete fusion results in BA fenestration (1, 2, 4, 8) and a pathologic structural defect. Muscular gaps have been documented in the tunica media of the medial walls at the two ends of the fenestration (1, 4). These gaps and increased hemodynamic stress have been suggested as factors in the high incidence of aneurysms at the proximal end (1, 2, 4, 8).
According to Padget (9), the VA are formed during the 32nd–40th day of gestation: seven primitive cervical segmental arteries connect with each other and to the longitudinal neural arteries via bilateral channels that parallel the longitudinal neural arteries on each side to form the primitive VA. At this stage of development, there is a transient primitive vertebrobasilar anastomosis between the longitudinal neural artery and the first segmental arteries. It has been suggested that remnants of these anastomotic vessels result in intracranial VA or vertebrobasilar artery duplication (2, 7, 8).
On the basis of their angiographic studies, Lasjaunias et al (5, 10) presented schemas of 14 types of variation of the vertebrobasilar system. One type is the result of duplication of only the VA (Fig 5B), and another consists of duplication of the VA and the lower BA where a short segment of the persistent primitive vertebrobasilar anastomosis remains (Fig 5C). The latter is called premedullary duplication of the VA. De Caro et al (3) were the first to report another duplication formed with the remnant of the primitive long tract anastomosis between the right VA and the middle BA and named it PPLVB anastomosis (Fig 5D). To our knowledge, ours is only the second report of a PPLBV anastomosis.
In our case, both vertebrobasilar junctions were aplastic or hypoplastic, and the BA was primarily fed via the PPLVB anastomosis. The junction ipsilateral with the anastomosis manifested a thin, serpentine, anomalous, and duplicated artery, a variation that has not been reported elsewhere. We posit that in our patient vertebrobasilar connections failed to develop and primitive anastomotic arteries involuted during the 32nd–40th days of gestation.
An aneurysm developed at the site involved with this particular variation of the vertebrobasilar system. Although VA duplication results in a relatively high incidence of anomalies, including aneurysms (6, 7), we posit that our patient’s aneurysm development was related to the presence of a PPLVB anastomosis. The increased hemodynamic stress from the PPLVB anastomosis may have induced aneurysm formation and subsequent rupture, because the anastomosis supplied most of the blood flow to the BA and connected to it vertically.
The authors report the new vertebrobasilar variant accompanied with a ruptured aneurysm.
- Received June 23, 2003.
- Accepted after revision August 23, 2003.
- Copyright © American Society of Neuroradiology