Pituitary tumors present because of either mass effect or functional abnormalities or, increasingly, as incidental findings on MR imaging. Although most infundibular masses are benign, the differential diagnosis includes germ cell tumors, CNS lymphoma, and cerebral inflammatory lesions, including neurosarcoidosis and histiocytosis (1–3). Invasive biopsy, with its associated risks, is required for definitive diagnosis of infundibular lesions. A patient with an infundibular mass associated with pituitary hormonal deficiency—both of which spontaneously regressed, enabling conservative management—is described in this letter.
A 17-year old male patient was referred to the endocrine clinic with a 7-week history of thirst, polydipsia, and polyuria. He was otherwise well, with no significant medical history, and diabetes had been excluded. The initial differential diagnosis lay between psychogenic polydipsia and diabetes insipidus. Initial investigations demonstrated normal serum osmolality (293 mosmol/kg) yet dilute urine (89 mosmol/kg), while other pituitary function tests were unremarkable. Consequently, a water deprivation test was performed, which confirmed a diagnosis of cranial diabetes insipidus. Oral desmopressin was commenced, with immediate symptomatic improvement.
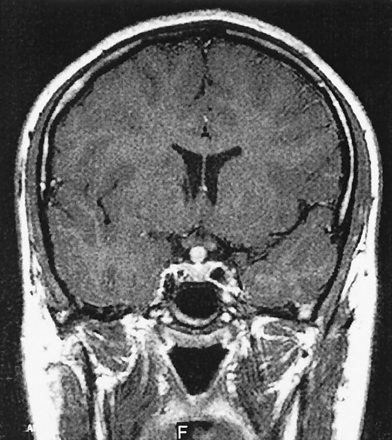
MR imaging of his pituitary gland demonstrated loss of high signal intensity within the posterior pituitary gland and an associated 6-mm focal enhancing infundibular mass following contrast (Fig 1). The radiologic appearance of the anterior pituitary was unremarkable, and there was no involvement of the optic chiasm. Further examination of the MR images revealed no meningeal enhancement, whereas a chest radiograph, autoimmune profile, anti-neutrophil cytoplasmic antibody, c-reactive protein, erythrocyte sedimentation rate, beta human chorionic gonadotrophin, and alpha fetoprotein did not suggest sarcoidosis or inflammatory or malignant disease. Invasive biopsy was deferred because visual fields were normal, and the patient was studying for examinations.
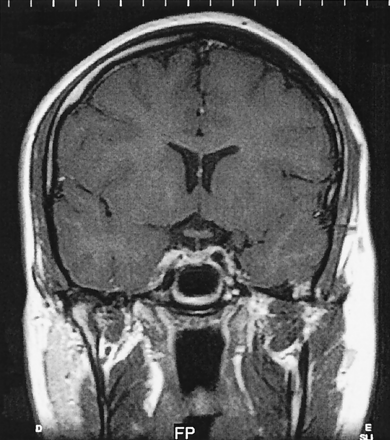
In the 3 months following the initial endocrine assessment, repeat hormone testing revealed progressively rising prolactin (656 mU/L, 1366 mU/L) and diminishing testosterone (5.5 nmol/L, 0.6 nmol/L), consistent with an evolving pituitary stalk lesion (Table). He was commenced on testosterone replacement therapy. A second MR imaging performed 3 months following the initial imaging demonstrated the infundibular mass to be fractionally smaller. Subsequent MR images confirmed shrinkage of the infundibular lesion until it completely resolved a year after initial imaging (Fig 2); however, the loss of high signal intensity in the posterior pituitary seen on initial imaging remained unaltered. Further endocrine tests reflected the radiologic regression of the pituitary lesion with prolactin and gonadotrophin levels normalizing (Table). Testosterone replacement therapy was successfully withdrawn a year after initiation. Gonadotrophin and prolactin levels have remained within the normal range for 4 years, and the radiologic improvement has been sustained over this period. In keeping with the persistent loss of the normal high signal intensity seen in the posterior pituitary, however, repeated attempts to wean him from desmopressin acetate replacement have failed, which has resulted in an immediate return of polyuria.
Regression of pituitary region tumors following administration of steroids is well recognized in germ cell tumors, lymphomas, and neurosarcoidosis (1–3). Similar regression of a pituitary mass due to lymphocytic adenohypophysitis has been reported, but only during the postpartum period (4). We are unaware of other cases with spontaneous radiologic and hormonal recovery of an infundibular mass outside of the postpartum period. Furthermore, we can demonstrate the acute deterioration of pituitary function followed by functional recovery mirrored by the disappearance of the pituitary mass on MR imaging. Although Rathke cleft cysts have been reported to regress spontaneously, MR imaging appearances in these patients have been of a cystic mass with ring enhancement.
The explanation for regression of the infundibular mass is unclear. Lymphocytic infundibuloneurohypophytis can cause transient abnormalities of pituitary function, yet the radiologic appearances are of thickened pituitary stalk as opposed to the discrete mass seen in this case. Our findings challenge the necessity for tissue diagnosis in small infundibular masses, and in similar circumstances a “wait-and-see” policy of close clinical and radiologic surveillance may negate the potential hazards of pituitary biopsy. We are curious whether others have seen this type of apparent spontaneous mass regression.
Coronal T1-weighted image following intravenous gadolinium, showing discrete enhancing infundibular mass at presentation.
Coronal T1-weighted image following intravenous gadolinium 2 years after presentation, showing normal appearances of the pituitary gland, infundibulum, and suprasella cistern.
Summary of hormonal and radiologic results
- Copyright © American Society of Neuroradiology