Abstract
SUMMARY: Hemophagocytic lymphohistiocytosis (HLH) is a rare disorder of the immune system that is associated with frequent involvement of the central nervous system (CNS). The MR imaging and CT findings of the CNS infiltration have been reported in the past; however, the diffusion-weighted imaging (DWI) findings have not been previously described. We present MR imaging findings in a case of secondary HLH with CNS involvement, with an emphasis on the DWI findings.
Hemophagocytic lymphohistiocytosis (HLH), also called hemophagocytic syndrome (HPS), is a multisystem disorder characterized with aggressive proliferation of activated macrophages and histiocytes, frequently affecting the central nervous system (CNS).1 Its neuroimaging findings may mimic other disease entities and can become a diagnostic challenge, especially in immunocompromised patients. To the best of our knowledge, this is the first report to describe the diffusion-weighted MR imaging (DWI) findings of the CNS infiltration in HPS.
Case Report
A 13-year-old girl who had recently completed her induction chemotherapy for acute T-cell lymphoblastic leukemia was admitted to the hospital with nausea, projectile vomiting, and high-grade fever occurring for the past few days. She had developed diplopia during the past few hours. She was previously discharged from the hospital after receiving the first dose of her chemotherapy 3 weeks earlier. Her complete blood count revealed pancytopenia. An emergency cranial CT revealed several hypoattenuated lesions in the bilateral cerebral hemispheres, right cerebellum, and the vermis (Fig 1A). Postcontrast images additionally disclosed multiple nodular leptomeningeal enhancements adjacent to the hypoattenuated lesions (Fig 1B). The results of the CSF examination did not indicate any findings suggestive of infection or leukemic infiltration, though hemophagocytic macrophages were observed. Cranial MR imaging revealed a large midline vermian with surrounding edema showing ring enhancement and restricted diffusion (Fig 2A–D). There were also multiple small lesions in the cerebral hemispheres (mostly cortical with some deeply seated), right cerebellum, and right cerebral peduncle that were hyperintense on T2-weighted turbo spin-echo (TSE) (Fig 3A). The lesions were hypointense on T1-weighted spin-echo (SE) studies and showed ring enhancement following gadolinium injection (Fig 3 B). There was also diffuse leptomeningeal enhancement (Fig 2B, 3B). DWI demonstrated restricted diffusion in all lesions and revealed additional lesions, undetected in other pulse sequences (Fig 3C, -D). The bone marrow aspiration, which was subsequently performed, revealed numerous histiocytes with hemophagocytosis consistent with HLH. The child underwent HLH 2004 protocol but died during treatment.
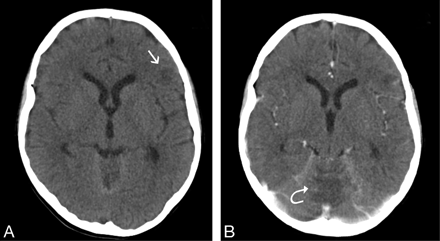
A, Noncontrast axial CT demonstrates low-attenuation lesion in the left frontal subcortical region (arrow).
B, Contrast-enhanced axial CT from the same level shows peripheral nodular enhancement at the left frontal lesion and low attenuation within the vermis (curved arrow).
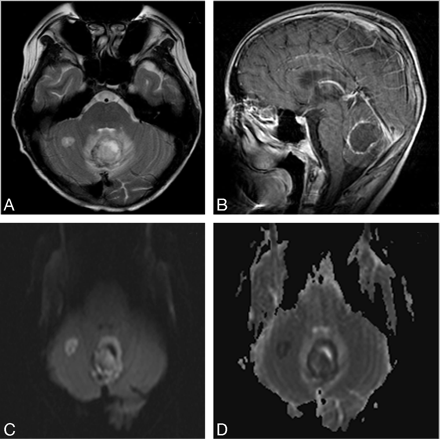
A, Axial T2-weighted TSE (4000/99 [TR/TE]) image shows a large vermian mass with a complete hemorrhagic ring and surrounding edema. A small right cerebellar hyperintense lesion is also seen.
B, Postcontrast sagittal T1-weighted SE (550/15) image demonstrates ring enhancement of the vermian lesion.
C and D, DWI (2800/78; b of 0, 500, 1000 seconds/mm2 in 3 axes; 256 × 256 matrix; 230 mm FOV; C) and ADC (D) images show decreased diffusion at the center of the vermian lesion as well as at the right cerebellar lesion.
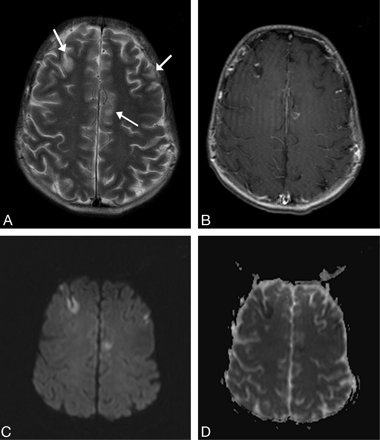
A, Axial T2-weighted TSE (4000/99) image shows cortical hyperintense lesions (arrows).
B, Postcontrast axial T1-weighted SE (550/15) image reveals peripheral enhancement of the lesions. C and D, DWI (2800/78; b of 0, 500, 1000 seconds/mm2 in 3 axes; 256 × 256 matrix; 230 mm FOV; C) and ADC (D) images show restricted diffusion of the lesions (note that the lesions are much more conspicuous on this sequence).
Discussion
HLH is included within the histiocytic disorder spectrum and may either present as a primary disease or occur as a secondary, reactive disease.1 The primary form (familial or sporadic) results from a defect of the immune system, occurs in young infants, and is fatal if untreated. The secondary form (as in our case) occurs as a reactive process in response to infective agents (such as bacteria, viruses, and parasites) as well as to malignancies2 and tends to occur in immunocompromised individuals. When it is secondary to a viral infection, it can also be called “virus-associated HPS.”3 This form is usually self-limiting but may require treatment with chemotherapy and/or immunosuppressive agents. The disorder is characterized by benign proliferation of tissue histiocytes showing hemophagocytosis with an up-regulation of the inflammatory cytokines.4 The diagnostic criteria include fever, splenomegaly, cytopenia that affect more than 2 cell lines, hypertriglyceridemia, hyperferritinemia and/or low fibrinogen level, and hemophagocytosis in the reticuloendothelial system.1
The CNS is involved in 10%–73% of the patients with variable neurologic symptoms, including irritability, cranial nerve findings, convulsions, and coma.4,5 The histopathologic process starts as a leptomeningeal process, progressing to perivascular infiltration with astrocytic proliferation affecting mainly the white matter, followed by areas of necrosis and focal demyelination.4 The small series and case reports in the literature reviewing the neuroimaging findings disclose the same pattern. Reported CT findings include atrophy, focal hypodensities, occasional hyperattenuated areas due to calcification and parenchymal hemorrhage, extra-axial hemorrhages mimicking child abuse, and enhancing leptomeningeal and/or parenchymal lesions.4-7 Our case had similar findings, with low attenuating focal lesions in the hemispheric white matter, some showing peripheral nodular enhancement following contrast. The previously described MR imaging findings are fairly consistent. The most commonly seen findings are parenchymal volume loss with focal necrosis and white matter abnormalities. Diffuse leptomeningeal and perivascular enhancement is also frequently seen, corresponding to the meningeal and perivascular infiltration of the histiocytes and lymphocytes,4,8 and it has been suggested that HPS should be considered in the differential diagnosis of leptomeningeal and perivascular space enhancement with diffuse white matter lesions.8 Multiple enhancing lesions with T2 prolongation have also been described.5,6,8 The imaging findings in our case were consistent with the above-mentioned findings.
The imaging findings of our case and those in other reports are nevertheless nonspecific. As demonstrated by the findings of our case and those in other reports, the fact that both the CT and MR findings of the HPS are nonspecific may cause significant diagnostic challenge and may delay the specific treatment, especially in an immunocompromised patient. The DWI and apparent diffusion coefficient (ADC) maps evaluate the diffusion properties of water molecules in tissue. This particular imaging technique gives important diagnostic information for the characterization of rim-enhancing parenchymal lesions and may also be of some help in the differential diagnosis of HLH. The most important differential to consider in that case is the CNS infections, especially in an immunocompromised patient. Although some pathogens have more specific imaging findings, many share common features, and DWI provides proved help in differential diagnosis of abscesses. The pyogenic brain abscess has restricted diffusion at its center, related to its high viscosity and cellularity.9 Similarly, fungal cerebral abscesses have been shown to cause decreased diffusion, likely due to the proteinaceous nature of their fluid content and cellular infiltration-infarction of the lesions.10 In contrast, toxoplasma abscesses do not exhibit restricted water diffusion.11 It has been reported that tuberculomas also have normal ADC values.12 Septic emboli with foci of cerebritis and fungal infection should then be included in the differential in this case, but the laboratory evaluation guides rule out these possibilities. The diffuse leptomeningeal enhancement in our case may raise the concern for leukemic infiltration of the CNS, but parenchymal leukemic masses are very uncommon. When present, these are contiguous with the meningeal surface and are almost always hyperattenuated on the CT.13 In addition, our patient was in remission and had no evidence of leukemic cells in the bone marrow or on CSF examination.
The exact cause of the diffusion restriction in the white matter lesions in our patient is unclear. The water diffusion in living tissue is influenced by many factors, including chemical (cell type and attenuation, macromolecule size and type) and physical properties of the tissue (viscosity and temperature) and perfusion. The diffusion restriction of hemophagocytic infiltration may be due to neuronal loss with cytotoxic edema in scattered small foci, which will then progress to areas of necrosis.4,5 Previous neuropathologic studies have also demonstrated that the hemophagocytic infiltration is associated with focal areas of demyelination.4,14 The acute demyelinating lesions were found to have reduced diffusivity due to either swelling of injured oligodendrocytes or ischemic cell damage.15 The reported findings may then also result from this alternate process. DWI appears to have a role in both suggesting and confirming the diagnosis of the potentially lethal HPS particularly in the appropriate clinical setting.
References
- Received July 10, 2005.
- Accepted after revision August 13, 2005.
- Copyright © American Society of Neuroradiology