Abstract
BACKGROUND AND PURPOSE: Prediction of survival in patients with glioblastomas is important for individualized treatment planning. This study aimed to assess the prognostic utility of presurgical dynamic susceptibility contrast and diffusion-weighted imaging for overall survival in patients with glioblastoma.
MATERIALS AND METHODS: MR imaging data from pathologically proved glioblastomas between June 2006 to December 2013 in 58 patients (mean age, 62.7 years; age range, 22–89 years) were included in this retrospective study. Patients were divided into long survival (≥15 months) and short survival (<15 months) groups, depending on overall survival time. Patients underwent dynamic susceptibility contrast perfusion and DWI before surgery and were treated with chemotherapy and radiation therapy. The maximum relative cerebral blood volume and minimum mean diffusivity values were measured from the enhancing part of the tumor.
RESULTS: Maximum relative cerebral blood volume values in patients with short survival were significantly higher compared with those who demonstrated long survival (P < .05). No significant difference was observed in the minimum mean diffusivity between short and long survivors. Receiver operator curve analysis demonstrated that a maximum relative cerebral blood volume cutoff value of 5.79 differentiated patients with low and high survival with an area under the curve of 0.93, sensitivity of 0.89, and specificity of 0.90 (P < .001), while a minimum mean diffusivity cutoff value of 8.35 × 10−4mm2/s had an area under the curve of 0.55, sensitivity of 0.71, and specificity of 0.47 (P > .05) in separating the 2 groups.
CONCLUSIONS: Maximum relative cerebral blood volume may be used as a prognostic marker of overall survival in patients with glioblastomas.
ABBREVIATIONS:
- EGFR
- epidermal growth factor receptor
- GBM
- glioblastoma
- MD
- mean diffusivity
- MDmin
- minimum mean diffusivity
- rCBV
- relative cerebral blood volume
- rCBVmax
- maximum relative cerebral blood volume
Glioblastomas (GBMs) are the most common malignant tumors of the central nervous system in adults, representing 50% of all gliomas and 20% of all intracranial solid lesions.1 The prognosis of GBM is poor, and median overall survival is <1 year.2 Even in optimal conditions (young patients treated by radical surgery, radiation therapy, and chemotherapy), death usually occurs within 2 years.3,4 Several factors, both clinical (age, performance status) and therapeutic (extent of surgery, radiation therapy, chemotherapy), as well as specific tumor characteristics such as location and nature (de novo or secondary from a low-grade glioma)5,6 have been studied as potential prognostic markers of overall survival with variable degrees of sensitivity and specificity. Recently, tumor genetics is also being investigated as a prognostic index.7,8
Conventional MR imaging is widely used as the technique of choice for GBM diagnosis and also has an important role in monitoring disease progression and response to therapy for patients with GBM. Additional advanced imaging techniques, such as relative cerebral blood volume (rCBV) obtained from dynamic susceptibility contrast perfusion imaging, have been used to predict glioma grade9⇓–11 and assess treatment response.12 A recent report10 indicated that maximum relative cerebral blood volume (rCBVmax) can be used as a predictive marker of progression-free survival in patients with gliomas, regardless of the tumor grade.
Similar to perfusion imaging, diffusion-weighted imaging has also been used for diagnosis of tumors. Tumors with high cellularity demonstrate restricted diffusion and thus low mean diffusivity (MD) or apparent diffusion coefficient, which inversely correlates with tumor cellularity.13,14 Areas with minimum mean diffusivity (MDmin) reflect the sites of highest cellularity, and tumors with a low MD tend to have a poor prognosis.15⇓⇓–18
Radiation therapy and chemotherapy with temozolomide have become the standard of care in the treatment of GBM and have demonstrated increased survival benefits in patients with newly diagnosed GBM.19 However, several clinical trials, including blocking the tyrosine kinase activity of epidermal growth factor receptor (EGFR),20,21 using competitive and noncompetitive kinase inhibitors in combination with radiation and temozolomide,20,21 and using monoclonal antibodies,20 are also investigating the treatment of GBMs. The exact value of each of these therapeutic strategies remains investigative though. The overall survival of patients with glioblastomas varies significantly,17,18 and it is imperative to know which patients will do better or worse, preferably before initiation of treatment, by using a noninvasive imaging method, so as to tailor fit the therapy for the best management and hopefully increased survival. We have evaluated the role of DSC-MR imaging and DWI as potential prognostic imaging markers in patients with GBM with an eventual goal of using these parameters in the selection of the optimal treatment option for these patients.
Materials and Methods
MR Imaging
This retrospective study was approved by the institutional review board and was compliant with the Health Insurance Portability and Accountability Act. A total of 564 treatment-naïve patients diagnosed with GBM at the University of Pennsylvania from June 2006 to December 2013 were retrospectively reviewed. Because we were interested in evaluating the role of perfusion-weighted imaging and diffusion-weighted imaging, we excluded the cases in which the PWI or DWI scans were not available. In addition, we analyzed the pretreatment MR imaging scans of only those patients who had gross total resection of their tumors so that the extent of surgery was not a confounder in the analysis. Furthermore, we also excluded all GBMs with oligodendroglial features. Of the 564 cases reviewed, 58 patients (32 men and 26 women; mean age, 62.71 ± 13.2 years; age range, 22–89 years) with a pathologically proved GBM met our inclusion criteria and were included in the study. After surgery, all the patients were treated with chemotherapy and radiation therapy.
We used a 15-month overall survival as the cutoff to evaluate rCBVmax and MDmin as predictive markers because several previous studies have reported a median overall survival time of 12–15 months for patients with GBM.2,18,19 Thus, the 58 patients in our study were divided into 2 groups: patients having long survival (n = 30, patients who had an overall survival of ≥15 months) and short survival (n = 28, patients who had an overall survival of <15 months). The survival time was calculated as the time (in months) from the initial date of diagnosis until the date of death. The clinical symptoms, survival duration, Karnofsky score, and lesion diameter of the patients demonstrating short and long survival are reported in On-line Tables 1 and 2. The MR images acquired before surgery (<1 week) were evaluated in this study.
All MR images were obtained on a 3T clinical MR imaging system (Tim Trio; Siemens, Erlangen, Germany), equipped with a 12-channel phased array head coil. The imaging protocol included a 3-plane scout localizer, axial 3D T1-weighted magnetization-prepared rapid acquisition of gradient-echo images by using the following parameters: TR, 1760 ms; TE, 3.1 ms; TI, 950 ms; matrix size, 192 × 256; FOV, 25 × 25 cm2; and 1-mm section thickness; and FLAIR images with TR, 9420 ms; TE, 141 ms; TI, 2500 ms; matrix size, 192 × 256; and 3-mm thick contiguous sections with no gap. DWI data were acquired by using a single-shot spin-echo echo-planar imaging sequence with parallel imaging by using a generalized autocalibrating partially parallel acquisition and an acceleration factor of 2. Other sequence parameters were as follows: FOV = 22 × 22 cm2; b=0, 1000 s/mm2; section thickness, 3 mm; number of sections, 40; acquisition time, 8 minutes.
For dynamic susceptibility contrast imaging, a bolus of gadobenate dimeglumine (MultiHance; Bracco Diagnostics, Princeton, New Jersey) was injected as the preloading dose of 0.07 mmol/kg. The preloading dose was administered to reduce the effect of contrast agent leakage on CBV measurements. A DSC T2*-weighted gradient-echo, echo-planar sequence was obtained during the second 0.07-mmol/kg bolus of intravenous contrast agent. The injection rate was 5 mL/s for all patients and was immediately followed by a bolus injection of saline (total of 20 mL at the same rate). DSC sequence parameters included the following: TR/TE, 2000/45 ms; FOV, 22 × 22 cm2; in-plane resolution, 1.72 × 1.72 × 3 mm3; slab of 20 sections covering the tumor region; and acquisition time of 1 minute 38 seconds. A long TR and a low flip angle were used to reduce the effect of changes in T1 relaxation from contrast agent leakage.22 Post-contrast-enhanced T1-weighted MPRAGE images were acquired after completion of the DSC sequence.
Image Processing
The rCBV was calculated from PWI data by using the intravascular indicator dilution algorithms described previously.23⇓–25 Data processing was performed by using PWI Task Card (Massachusetts General Hospital, Boston, Massachusetts) on a Leonardo workstation (Siemens). MD maps were automatically generated by using the software tools available on the scanner by using a monoexponential fit to the multiple b-value images. Measurements were obtained by 2 radiologists (G.Ç. and F.K., with >4 years of experience reading brain MR imaging). We meticulously chose multiple ROIs from the enhancing part of the tumor, avoiding areas of cerebral blood vessels, calcifications, hemorrhage, and CSF-filled sulci to measure a reliable CBV value as proposed earlier.26–27 The ROIs were drawn and chosen in agreement by the 2 readers, thereby reducing any interobserver variability. The commonly used rCBVmax parameter28 was computed by calculating the mean CBV values from 3 circular ROIs measuring 30–50 mm2 from areas of visually high CBV as reported previously.26–27 For normalization, 3 circular ROIs of the same size were drawn in the contralateral normal-appearing white matter. A similar analysis method was used to investigate the minimum mean diffusivity. Three circular ROIs measuring 30–50 mm2 from the visually lowest MD values were used to compute MDmin, representing high cellularity as reported previously.13,17
Statistical Analysis
The long and short survival patient groups were compared by using a Student t test. A P value < .05 was considered significant. A receiver operating characteristic analysis was performed to evaluate the predictive power of rCBVmax and MDmin for overall survival. Areas under the curve were computed. A cutoff value for each parameter was determined by maximizing the sum of sensitivity and specificity. Kaplan-Meier survival curves were used to characterize and compare the groups with high-versus-low rCBVmax and high-versus-low MDmin in terms of overall survival. All statistical analyses were conducted by using PASW Statistics, Version 18 (IBM, Armonk, New York).
Results
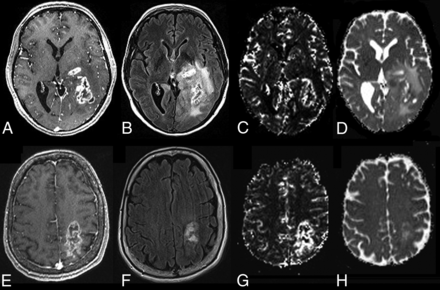
Representative images of patients with GBM with long and short survival are shown in Fig 1. The contrast-enhanced T1-weighted images and FLAIR images from these patients look similar, showing heterogeneous peripheral enhancement and extensive surrounding FLAIR signal abnormality. All tumors showed prominent enhancement after IV contrast administration. The patient with short survival demonstrated higher rCBVmax compared with the patient who exhibited long survival.
Representative MR images and parametric maps from patients with GBM. The top row (A–D) shows images from a 66-year-old woman with GBM who survived for >58 months after gross total resection of her GBM in the left temporo-occipital lobe. Representative MR images from a 75-year-old man with a GBM in the left parietal lobe with only a 5-month survival are shown (E–H). Images of both patients demonstrate heterogeneous peripheral enhancement (A and E) and extensive surrounding FLAIR signal abnormality (B and F) on axial contrast-enhanced T1-weighted and FLAIR images, respectively. The patient with short survival has a higher CBV (G) (rCBVmax = 12.22) in comparison with the patient with long survival (C) (rCBVmax = 3.57). The MD maps from these patients (D and H) do not show any difference (6.50 × 10−4 mm2/s versus 6.80 × 10−4 mm2/s).
The rCBVmax values of patients with short survival (9.90 ± 4.01) were significantly higher compared with those of long survival (4.78 ± 1.30, P < .05). There was no significant difference in the MDmin values between the 2 groups: 0.80 ± 0.17 versus 0.75 ± 0.15 × 10−3mm2/s (Table).
Average ± SD, sensitivity, specificity, PPV, and NPV of pretreatment rCBVmax and MDmin in patients with GBM demonstrating long (≥15 mo) survival and short (<15 mo) survival
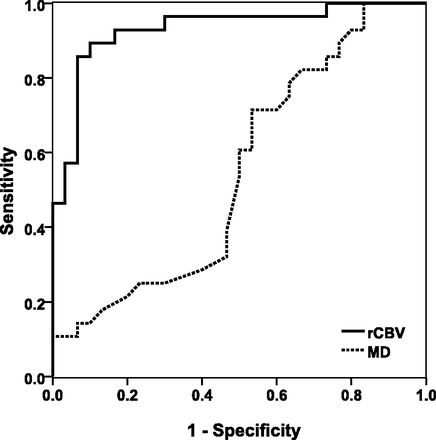
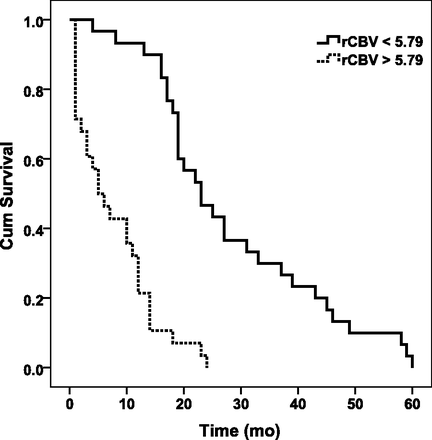
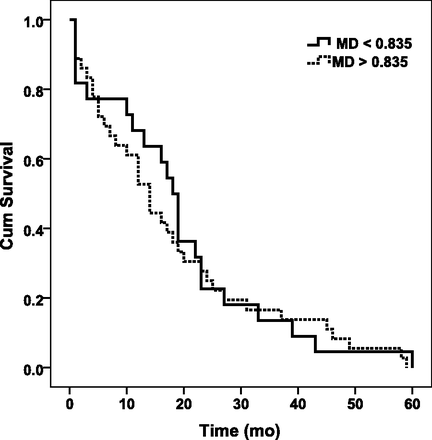
Receiver operating characteristic analysis indicated that a rCBVmax cutoff value of 5.79 was the best parameter for predicting overall survival with an area under the curve of 0.93, sensitivity of 0.89, specificity of 0.90, positive predictive value of 0.89, and negative predictive value of 0.90 (Fig 2 and Table). The MDmin cutoff value of 8.35 × 10−4mm2/s, on the other hand, showed only a modest area under the curve of 0.55, sensitivity of 0.71, specificity of 0.47, positive predictive value of 0.56, and negative predictive value of 0.64 (Fig 2 and Table). A combination of rCBVmax and MDmin did not improve the prediction capability and had an area under the curve (0.93) similar to that of rCBVmax. Kaplan-Meier survival curves demonstrated that GBMs with low rCBVmax (<5.79) had a median survival time of 23 ± 3.4 months, whereas GBMs with high rCBVmax (≥5.79) had a median survival time of 5 ± 1.9 months (Fig 3). There was a significant difference in patients with high rCBVmax and low rCBVmax (P < .001). For the DWI measurements, GBMs with low MDmin (<8.35 × 10−4mm2/s) had a median survival time of 14 ± 2.0 months, whereas GBMs with high MDmin (>8.35 × 10−4mm2/s) had a median survival time of 18 ± 1.4 months, and there was no significant difference between the 2 groups (P > .05) (Fig 4).
Receiver operative characteristic curves of rCBVmax (solid line) by using a rCBVmax cutoff value of 5.79. The area under the curve was 0.93. The receiver operating curve of MDmin (dotted line) by using a cutoff value of 8.35 × 10−4mm2/s demonstrated only a modest area under the curve of 0.55.
Kaplan-Meier curves for patients with low (<5.79, solid line) and high (≥5.79, dotted line) rCBVmax. GBMs with low rCBVmax had a median survival time of 23 ± 3.4 months, whereas GBMs with high rCBVmax had a median survival time of 5 ± 1.9 months (P < .001). Cum indicates cumulative.
Kaplan-Meier curves for patients with GBM with low (<0.835 × 10−3mm2/s, solid line) and high (≥0.835 × 10−3mm2/s, dotted line) MDmin. GBMs with a low MDmin have a median survival time of 14 ± 2.0 months, whereas GBMs with a high MDmin have a median survival time of 18 ± 1.4 months. There is no significant difference between the 2 groups (P > .05). Cum indicates cumulative.
Discussion
Our study suggests that pretreatment rCBVmax can be used as a prognostic marker for overall survival in patients with GBM. In particular, patients with high pretreatment rCBVmax demonstrated lower survival in comparison with patients with low pretreatment rCBVmax, who exhibited longer survival of >15 months. These results could have a potential clinical benefit and in the future may aid in individualized treatment planning because patients with high pretreatment rCBVmax can be offered upfront alternative treatment strategies, including bevacizumab, immunotherapy, or other therapies targeted toward increased survival.
Conventional imaging characteristics of GBM, including location, size, and degree of enhancement; necrosis; and extent of edema, have been studied for prediction of survival.9⇓–11,29⇓⇓⇓⇓⇓⇓–36 Although contrast enhancement is generally used to estimate the extent of the tumor, it is clear from the literature that conventional radiologic findings, such as the absence of contrast enhancement, are not only poor predictors of tumor grade but may or may not be prognostic factors for either survival or progression-free survival.12,37 PWI is increasingly being used to assess microvascular changes associated with the tumor grade, and it is widely used to assess tumor angiogenesis and microvasculature.34,35,38 Law et al30 suggested that rCBV measurements in low-grade gliomas correlated more accurately with time to progression than the initial histopathologic grading of the tumor. Although Oh et al18 suggested that rCBV had no predictive value with respect to the prognosis in GBM, they evaluated GBM tumors after surgical resection; thus, it is unclear whether the extent of surgery played a role in determining the prognostic value in their study.18 Bisdas et al11 reported that there was no correlation among CBV, World Health Organization grade, and progression-free survival in a mixed population of gliomas. Similar to ours, findings of Mangla et al32 were that rCBV was useful for predicting progression-free survival in anaplastic astrocytomas, but not for grade III tumors with oligodendroglial components.
We observed that an rCBVmax threshold value of 5.79 was the best predictor for overall survival with a very high sensitivity and specificity. In other words, this threshold was evaluated as a prognostic index of survival in GBM and not for predicting tumor grade, for which a much lower rCBV threshold was reported by Bisdas et al11 (4.2), Lev et al29 (1.5), Law et al31 (1.75), and Mangla et al32 (2.55).
High-grade brain tumors are usually associated with high cellularity and therefore exhibit low MD values.15⇓–17 Previous studies15,16,39 reported that MDmin was a sensitive marker for prognosis and survival. The cutoff MD values used in these studies were 0.74 × 10−3 mm2/s, 0.90 × 10−3 mm2/s, 0.93 × 10−3 mm2/s, and 1.00 × 10−3 mm2/s, respectively.15⇓⇓–18 Higano et al16 studied 37 malignant astrocytic tumors, including 22 GBMs, and reported a significant negative correlation between MDmin and Ki-67, which may explain the poor prognosis of patients with lower MDmin. The authors of that study also reported that the MDmin (0.834 × 10−3mm2/s) of GBM was significantly lower than the MDmin (1.06 × 10−3mm2/s) of anaplastic astrocytomas. In another study, Murakami et al15 studied 79 malignant supratentorial astrocytic tumors, including 50 patients with GBMs, and observed that patients with an MDmin of >1.00 × 10−3mm2/s had better outcomes than patients with an MDmin of ≤1.00 × 10−3mm2/s. Yamasaki et al39 reported that MDmin also predicted overall survival in patients with GBMs who did not have a complete- or near-total resection of their tumors. We did not observe an MDmin cutoff value that could differentiate patients having short or long survival (Fig 4). However, in comparison with these previous studies, we studied a homogeneous population of patients with GBMs who had undergone gross total resection of their tumors, which may partially explain the difference in our results.
Because GBM is composed of prominent necrosis, nuclear atypia, cellular proliferation, and microvascular hyperplasia, the extent of necrosis and the amount of edema have been shown to negatively correlate with survival.5,40 Immunohistochemical staining for p53, Ki-67, and EGFR is generally used for differential diagnosis and grading of these tumors.41 Previous studies have shown that abnormal microvasculature may be associated with increased endothelial cellularity, proliferation, and tumor grade.42,43 Tumors with increased EGFR, Ki-67, and p53 staining are more invasive and exhibit a more malignant phenotype. A tumor-specific mutant of the EGFR, EGFRvIII, causes constitutive upregulation of the tyrosine kinase activity of the receptor and is frequently expressed in primary GBMs. EGFR signaling has, therefore, been the target for GBM therapy. It is also possible that rCBV measurements are revealing changes in microvascular attenuation that precede malignant transformation44 and may be indicative of poor prognosis as demonstrated in our study.
Previous survival analysis studies for patients with brain tumors have evaluated several factors: tumor grade, extent of resection, radiation dose, age, and Karnofsky score.5,6 Based on the results of some prospective clinical trials that evaluated patients with gliomas, the important prognostic factors for predicting outcome in gliomas are the extent of surgical resection, histologic results, and size of the lesion.12,45,46 Tumors not involving eloquent regions of the brain undergo gross total resection because it has been shown that maximal resection improves survival in patients with gliomas.12,45,46 Preoperative knowledge of the rCBVmax of a tumor may help to determine whether to biopsy or to resect, the aggressiveness of resection, the use of pre-/postoperative adjuvant radiation therapy and chemotherapy, and the frequency of follow-up examinations.
Although our study indicates the role of pretreatment rCBVmax as a potential imaging biomarker for predicting survival in GBM, the results should be interpreted in light of the limitations of the study. One was the use of hand-drawn ROIs for data analysis, which, though being simple and straightforward, tend to be subjective. Future studies involving semiautomated segmentation routines47,48 may be needed to analyze the data more objectively without any user bias. In addition, we did not evaluate other perfusion variables from the DSC data, such as cerebral blood flow and mean transit time values. Increasing the TR is only one of the methods to reduce the effects of T1, but it comes with a penalty of increased acquisition time. In addition to the simplistic measurements of MDmin, other parameters from diffusion imaging can be computed, such as fractional anisotropy and radial and axial diffusivity. It would be desirable to perform a multivariate analysis by using these varied imaging parameters to evaluate whether these additional parameters further increase the sensitivity and specificity in the overall prognosis of patients with GBM. The study was performed retrospectively, and the sample size for the Kaplan-Meier analysis was relatively small. The survival of patients with GBM can also be affected by other factors such as the location, tumor size, and Karnofsky score. A larger sample size would be necessary to perform a Kaplan-Meier analysis of the rCBVmax accounting for these confounding factors. We have limited the number of confounders, including selection of pure GBM (excluding patients with oligodendroglial features) and selection of patients with near-total resection of the mass, and restricted the analysis to tumors with a similar initial size in the 2 groups. A prospective study on a larger cohort of patients with GBM needs to be performed to further establish rCBV as a marker for overall survival in GBM.
Conclusions
Our results indicate that pretreatment rCBVmax may be a used as a sensitive prognostic marker for overall survival in patients with glioblastomas.
Footnotes
G. Çoban and S. Mohan contributed equally to this work.
Disclosures: Donald M. O'Rourke—UNRELATED: Medicolegal opinions, clinical neurosurgery only; Grants/Grants Pending: National Institutes of Health,* Comments: 1) RO1 and R21 applications on glioblastoma pathobiology and imaging; 2) Celldex Therapeutics sponsored imaging research, EGFRvIII and glioblastoma; Patents (planned, pending or issued): issued US patent,* Comments: EGFR/radiation treatment, issued December 1, 2009, US patent No. 7,625,558. Harish Poptani—UNRELATED: Consultancy: American College of Radiology, Image Metrix; Grants/Grants Pending: National Institutes of Health.* *Money paid to the institution.
REFERENCES
- Received August 29, 2014.
- Accepted after revision December 14, 2014.
- © 2015 by American Journal of Neuroradiology