Abstract
SUMMARY: In a prospective study among patients in the THRombectomie des Artères Cerebrales trial, we analyzed the diagnostic accuracy of 2 imaging biomarkers, the 2-layered susceptibility vessel sign and a high overestimation ratio, obtained on pretreatment brain T2* sequences, to identify cardioembolic stroke etiology (107/260 patients). In combination, these 2 biomarkers, on 1.5T or 3T systems (159 and 101 patients, respectively), demonstrated high specificity (0.77 at 1.5T and 1 at 3T) and their simultaneous presence is highly associated with cardioembolism.
ABBREVIATIONS:
- CES
- cardioembolic stroke
- HOR
- high overestimation ratio
- NPV
- negative predictive value
- overR
- overestimation ratio
- PPV
- positive predictive value
- SVS
- susceptibility vessel sign
- THRACE
- THRombectomie des Artères Cerebrales
- TL-SVS
- 2-layered susceptibility vessel sign
Unraveling the etiology in acute ischemic stroke caused by large-vessel occlusion is important for secondary stroke prevention strategies. However, in many patients, risk factors for both large-artery atherosclerotic and cardioembolic stroke (CES) etiology are present. The composition of thrombus in obstructed arteries varies depending on whether the embolic source is cardioembolism or large-artery atherosclerosis.1,2 On admission brain MR imaging, the susceptibility vessel sign (SVS), defined as a hypointense signal exceeding the diameter of the contralateral artery at the thrombus site,3 may be seen on T2*-weighted images. The SVS was reported to be associated with cardioembolism, but with conflicting results and low specificity.4⇓⇓⇓–8 Recently, 2 characteristics of the SVS, overestimation ratio (overR), a quantitative evaluation of the SVS, and the 2-layered susceptibility vessel sign (TL-SVS), were reported to predict CES.7,8 Indeed, both the TL-SVS and high overR (HOR) were described as exhibiting almost perfect specificity for CES.7,8 However, these studies were retrospective, monocentric, and used time-consuming susceptibility-weighted imaging or 3T systems, and the TL-SVS and HOR were not both evaluated in individual patients. With >200 patients included with a gradient-echo sequence at either 1.5T or 3T, the multicenter THRombectomie des Artères Cerebrales (THRACE) trial9 offers an opportunity to analyze the diagnostic accuracy of these 2 imaging biomarkers for the prediction of CES.
Materials and Methods
THRACE was a randomized controlled trial conducted in 26 centers in France. Study design and protocol are detailed elsewhere.10 Patients with acute ischemic stroke were eligible for inclusion if they were 18–80 years of age, had an NIHSS score of 10–25, had an occlusion of the intracranial ICA or the M1 segment of the MCA on MRA, could be administered intravenous thrombolysis within 4 hours of symptom onset, and could undergo thrombectomy within 5 hours of symptom onset. Patients with cervical ICA occlusion or subocclusive stenosis were excluded. Written informed consent was obtained from all patients or their legal representatives. The study protocol was approved by the Comité de Protection des Personnes III Nord Est Ethics Committee and the research boards of the participating centers.
For the present study, we included patients screened with an MR imaging gradient-echo sequence for whom analysis of the SVS was available. We excluded patients with severe motion artifacts on gradient-echo sequences when the presence or absence of SVS could not be reliably determined. We also excluded 5 patients screened with susceptibility-weighted imaging instead of a gradient-echo sequence. MR imaging acquisition parameters of the sequence were left to the discretion of the recruitment centers according to their routine practice and were therefore not standardized.
Readers searched for the TL-SVS, defined as an inhomogeneous SVS with a linear low-intensity signal core surrounded by a peripheral higher intensity signal.8 The overR was manually measured according to the method previously described (ie, overR = Width of SVS / Width of Large Artery).7 The ipsilateral large-artery width proximal to the occlusion was used to calculate the overR. Note that absence of the SVS was considered as an overR = 1 (Figure).
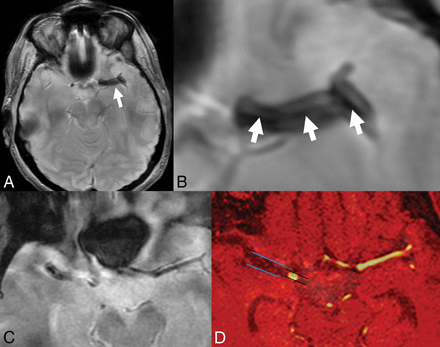
A and B, Two-layered susceptibility vessel sign. A 62-year-old man with left middle cerebral artery occlusion because of cardioembolism. 1.5T T2*-weighted gradient recalled-echo imaging (white arrow) shows a 2-layered SVS with a low-intensity signal core (arrowheads) surrounded by a higher intensity signal. C and D, Susceptibility vessel sign and overestimation ratio of SVS. A 69-year-old man with right middle cerebral artery occlusion. Overestimation ratio of SVS was 2.21 and the etiological work-up concluded to a cardiogenic embolism. The sequences of MR imaging from C, T2*-weighted gradient-echo images. D, The coregistered images of TOF-MRA and T2*-gradient-echo.
Stroke etiology was determined at the end of a complete etiologic work-up by a stroke neurologist, according to the Trial of Org 10172 in Acute Stroke Treatment classification.11 In the THRACE trial, the recommended general work-up, according to the European Stroke Organisation Guidelines,10 included physiologic parameters and routine blood tests, a 12-lead electrocardiogram, and continuous electrocardiography. In addition, 24-hour Holter electrocardiography monitoring was performed when arrhythmias were suspected and no other causes of stroke were found. The echocardiography was recommended when electrocardiographic abnormalities or evidence of cardiac disease on history was reported or when no other identifiable causes of stroke were found.
For details of the statistical analysis, see the On-line Appendix.
Results
Two hundred sixty patients, including 107 (41%) patients with CES (31/101 patients with 3T MR imaging and 76/159 patients with 1.5T MR imaging), were identified. Furthermore, the etiologic work-up found large-artery atherosclerosis in 40 (15%) patients, “other determined cause of stroke” in 16 (6%) patients, and “undetermined cause of stroke” in 97 (37%) patients.
Overall, the median overR was 1.59 (range, 1.0–2.9; interquartile range. 0.29). The median overR was 1.54 (range, 1.0–2.9; interquartile range, 0.36) and 1.60 (range, 1.0–2.7; interquartile range, 0.54) at 3T and 1.5T, respectively.
The TL-SVS was present in 94 (36%) patients (overall 43/101 patients screened at 3T and 43/80 patients with the SVS screened at 3T; overall 51/159 patients screened at 1.5T and 51/136 patients with the SVS screened at 1.5T).
At 1.5T, the association of the TL-SVS and HOR yielded a specificity of 0.77 and a positive predictive value of 0.60.
At 3T, the association of the TL-SVS and HOR yielded a specificity of 1, a negative predictive value of 0.74, and a positive predictive value of 1 (Tables 1⇓–3).
Diagnostic performance of the high overestimation ratio for the prediction of a cardioembolic etiology of stroke
Diagnostic performance of the 2-layered susceptibility vessel sign for the prediction of a cardioembolic etiology of stroke
Diagnostic performance of the combined 2-layered susceptibility vessel sign and the high overestimation ratio for the prediction of a cardioembolic etiology of stroke
Discussion
In the present study, using 3T systems, the simultaneous presence of the TL-SVS and HOR offered perfect specificity and a positive predictive value for CES. Using 1.5T systems, we also showed that the simultaneous presence of the TL-SVS and HOR had 77% specificity for CES.
Because exact stroke etiology cannot be determined with a high degree of reliability in >30% of strokes,12 a direct relationship between imaging characteristics and stroke etiology would be useful. We demonstrated that in real world conditions (ie, brain MR imaging performed in 26 different centers on either a 1.5 or a 3T MR imaging unit, using a gradient-echo sequence of <1 minute), the TL-SVS and HOR can have practical implications for determining stroke etiology at the acute phase.
Recently, from the THRACE trial, qualitative visual binary grading of the SVS offered a high sensitivity of the SVS to predict a stroke of cardioembolic origin (0.89; 95% CI, 0.83–0.95), but specificity was very low (0.21; 95% CI, 0.14–0.27).13 In the present study, we demonstrate that adding a more precise analysis of SVS characteristics (ie, TL-SVS and overR), increased specificity. This was achieved at the expense of lowering the sensitivity, as usually occurs when using a combination of biomarkers rather than a single sign. However, the combined analysis of the TL-SVS and HOR with cutoff values specific to the MR imaging system field strength increased specificity values.
Two recent retrospective studies using 3T systems analyzed separately the diagnostic accuracy of the TL-SVS and HOR for CES prediction. The authors found specificities of 97%8 and 91%,7 respectively, for the TL-SVS and overR of >2.01 to predict a CES.7 In our study, by means of a gradient-echo sequence rather than susceptibility-weighted imaging, the specificity of the TL-SVS and HOR both appeared lower on 1.5T and 3T systems.
The present prospective study is the largest to date that has evaluated the TL-SVS and overR in the context of stroke etiology. Our study has several limitations. First, THRACE was not a trial designed to specifically investigate stroke etiology. However, work-ups were performed in referral comprehensive stroke centers that ensure high quality and extensive etiologic work-ups in accordance with the current guidelines.10 Second, no information was registered on the anticoagulation regimen, the use of antiplatelet agents, or the platelet count before imaging, all factors that may have influenced the SVS. Third, the diagnostic accuracy of the SVS to predict thrombus composition varies according the MR imaging machines,14 and there was no standardization of gradient-echo sequence parameters among the 26 participating centers in the THRACE trial. In our opinion, this limitation enhances the generalizability of our findings.
Conclusions
The presence of both the TL-SVS and HOR offers a high specificity for CES etiology on both 1.5 and 3T systems. When a patient with stroke has both of these imaging biomarkers, a cardioembolic source is highly likely.
Acknowledgments
We thank Marc Soudant from the Institut National de la Santé CIC 1433 Epidémiologie Clinique for conducting the statistical analysis and Nick Barton for language editing.
Footnotes
Catherine Oppenheim and Olivier Naggara contributed equally to this work.
References
- Received June 7, 2018.
- Accepted after revision September 5, 2018.
- © 2019 by American Journal of Neuroradiology